INTRODUCTION
Malnutrition describes a state where the human body does not obtain the adequate amount of macro and micronutrients in order to maintain healthy tissue and organ function 1. In developed countries, malnutrition affects 1-15% of the population, with a greater impact on hospitalized patients and on those living in nursing homes. The prevalence of undernutrition in a hospital setting may be greater than 50% and tends to increase with the length of hospital stay that ultimately leads to a worse clinical outcome 1,2,3.
The effect of acute disease is probably the most important factor that contributes to malnutrition in hospitalized patients. However, a deficiency in energy and protein ingestion may play an important role in different clinical scenarios. The use of several diagnostic and therapeutic medical interventions that require fasting or at least major changes in the type and amount of ingested food may have a negative impact on nutritional status, especially in patients who are already at nutritional risk 3,4.
Total colonoscopy is an invasive procedure widely used for screening, diagnostic and therapeutic purposes in both the ambulatory and hospital setting. Since diagnostic accuracy and therapeutic safety of colonoscopy depend on the quality of the colonic cleansing, bowel preparation is mandatory, involving a modification of the diet and laxative drugs, usually containing polyethylene glycol (PEG). Nevertheless, bowel preparation is still considered to be a very challenging and difficult task that is feared by many patients 5,6
Dietary regimens for patients undergoing total colonoscopy are not clearly established. The American Society for Gastrointestinal Endoscopy (ASGE) and the European Society for Gastrointestinal Endoscopy (ESGE) recommend a low-fiber diet on the day preceding the procedure. However, the current practice is to prescribe a diet of a duration of 2-3 days to improve the preparation quality and also take into account the population of most studies 7,8,9. A clear liquid diet is also advisable when PEG is prescribed, which should be stopped a few hours before the procedure when using deep sedation 10,11. The need for a low-residue diet 2-3 days before the examination, plus a clear liquid diet after starting PEG treatment, might be associated with a nutritional deficiency in terms of energy and protein ingestion due to the intrinsic characteristics of these diets 12. Bowel preparation may actually induce a semi-fasting state with a potential negative impact on fragile patients, particularly in older patients and cases with debilitating or life-threating conditions, who are already malnourished or with a high nutritional risk.
Nutritional deficiency during colonoscopy preparation remains unknown and this problem has not been addressed in previous studies and current guidelines 8,9. Furthermore, the impact of this deficiency on clinical outcome has not been determined, in particular, in hospitalized patients who are theoretically more easily assessable. The present study aimed to quantify nutritional deficiency during colonoscopy preparation, which has never been reported in the literature.
The primary aims of the present study were:
To study the energy and protein intake in patients undergoing bowel preparation.
To calculate the nutritional deficiency by comparing energy and protein intake with the patients' theoretical needs.
The secondary aims include:
To characterize the nutritional status of patients undergoing total colonoscopy according to anthropometric data.
To ascertain if the calculated nutritional deficiency is associated with the quality of bowel preparation.
To compare energy and protein deficiency during bowel preparation between ambulatory and hospitalized patients.
To compare nutritional deficiency during bowel preparation between elderly and young adults.
MATERIALS AND METHODS
Study design
This was a single center, observational and cross-sectional study performed in a large hospital. This study was approved by the Ethics Committee of the hospital.
Patients
A convenience sample was obtained via the recruitment of adults referred to the Endoscopy Unit of the Hospital Garcia de Orta during a three month period who underwent nutritional assessment by the Artificial Feeding Team (GENE) using clinical and anthropometric tools. Ambulatory and hospitalized adult patients (18 years old or older) who underwent a colonoscopy during the morning shift with a completed bowel preparation were included in the study. The exclusion criteria included: failure to accomplish a complete bowel preparation, examinations performed in an emergency setting, lack of reliable clinical data due to physical or cognitive impairment, and inability to provide informed consent. One or two patients were evaluated every morning.
The clinical indication for each procedure was collected from the written colonoscopy request protocol and bowel preparation quality was assessed by the endoscopist using the Boston Bowel Preparation Scale (BBPS) 13. The results of the intervention and all diagnostic and therapeutic procedures were also recorded for each patient.
Bowel preparation regimen
Patients underwent bowel preparation according to the center protocol, which included a 48h low-residue diet before the examination and the ingestion of four Klean-Prep(r) (Macrogol) sachets (diluted in one liter of water) during a four to six hour period. Only clear liquids were allowed after starting macrogol treatment and patients were nil by mouth six hours before the examination as deep sedation was used.
Anthropometric evaluation
Anthropometric evaluation was performed by a trained dietitian before the procedure, according to the ISAK manual of the International Society for the Advancement of Kinanthropometry 14. The average of three consecutive measurements were recorded in the patient file.
Body mass index (BMI) was obtained using the weight/height2 equation, which was measured in kilograms and meters. Each patient was classified according to age. Undernutrition was defined as a BMI < 18.5 kg/m2 or < 22 kg/m2; eutrophy, as a BMI 18.5-25 kg/m2 or 22-27 kg/m2; and overweight, as a BMI > 25 or > 27 kg/m2 for patients under 65 or over 65 years of age, respectively 15.
Mid upper arm circumference (MUAC) was measured in centimeters using a flexible measuring tape wrapped around the mid upper arm, halfway between the olecranon and the acromion process.
Triceps skinfold (TSF) was measured in millimeters using a skinfold caliper on the mid-line of the posterior surface of the arm, halfway between the olecranon and the acromion process. It is an indicator of fat mass.
Mid arm muscular circumference (MAMC) was estimated using MUAC and TSF according to the formula: MAMC (cm) = MUAC (cm) - [TSF (mm) x 0.314]. This is an indicator of fat-free mass.
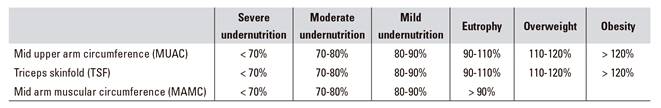
The anthropometric values of MUAC and TSF were compared for each patient with the NHANES National Health and Nutrition Examination Survey (NHANES) tables and the MAMC values, with Frisancho tables 16,17. The nutritional status was classified for each individual anthropometric parameter as eutrophic, overweight, obese or mild, moderate and severe undernutrition according to the criteria described by Blackburn and Thornton 16,18 (Table 1).
Nutritional deficiency calculation
Food ingestion was assessed in terms of energy and protein intake. Individual daily energy and protein needs were estimated using the formula 30 kcal x current weight (kg) and 1.25 g protein x current weight (kg), respectively. A recall of 48h before colonoscopy was performed to evaluate the proportion of food ingestion in each patient 19. The calculation of energy and protein intake was performed according to the Portuguese food composition table 20. The difference between energy/protein theoretical needs and energy/protein intake was considered as nutritional deficiency.
Statistical analysis
The statistical analysis was performed using the Statistical Package for Social Sciences (SPSS(r) Inc., Chicago, IL), version 21, and Microsoft Office Excel Professional 2013(r). The variables analyzed included: age, gender, patient provenience (ambulatory or hospitalized), clinical indication for colonoscopy, endoscopic findings, quality of bowel preparation, daily energy/protein needs, energy/protein ingestion within a 48h prior to the colonoscopy and energy/protein nutritional deficiency. The anthropometric variables considered were BMI, MUAC, TSF and MAMC.
A descriptive analysis of all the variables was performed and the Student's t-test for paired samples was used to ascertain the significance of energy and protein deficiency during the 48h prior to the examination. The Student's t-test for independent samples was also performed in order to assess the difference between energy and protein deficiency in ambulatory and hospitalized patients. The correlation between energy deficiency and the quality of the preparation was assessed using the Spearman's correlation test. A 5% level of statistical significance was considered for inferential tests.
RESULTS
Patients
One hundred and thirty-one patients were included (73 male and 58 female), ranging between 21 and 91 years of age (mean 63.6 ± 13.2 years). Seventy patients (53.4%) were 65 years of age or older; 111 patients underwent a colonoscopy as outpatients and 20 patients were hospitalized.
The main clinical indication for colonoscopy was the investigation of ferropenic anemia (n = 26, 19.8%), followed by post-polypectomy surveillance (n = 24, 17.6%), polypectomy (n = 21, 16%), suspicion of colorectal cancer (n = 14, 10.7%), haematochezia/rectal bleeding (n = 10, 7.6%), inflammatory bowel disease surveillance (n = 8, 6.1%) and post colorectal cancer resection surveillance (n = 6, 4.6%). Patient distribution according to the clinical indication for colonoscopy is shown in figure 1.

Fig. 1 Patient distribution according to the clinical indication for colonoscopy (CRC: colorectal cancer; IBD: inflammatory bowel disease; FOBT: fecal occult blood test).
The main endoscopic findings included colorectal polyps (n = 72, 55%), colonic diverticula (n = 8, 10.5%) and colorectal cancer (n = 7, 5.3%). Twenty-nine patients (22.1%) had no changes. Patient distribution according to the endoscopic findings are presented in figure 2. Baseline patient characteristics are shown in table 2.

Fig. 2 Patient distribution according to the endoscopic findings (CRC: colorectal cancer; UC: ulcerative colitis; CD: Crohn's disease).
Anthropometric evaluation
All patients included in the study underwent a full anthropometric evaluation using BMI, MUAC, TSF and MAMC before colonoscopy. Eleven patients (8.4%) had a low BMI and were considered as undernourished. Undernutrition was also observed in 48 (36.7%), 88 (67.2%) and 21 (16%) patients according to MUAC, TSF and MAMC, respectively. Patient distribution according to anthropometric evaluation is summarized in figure 2.
Bowel preparation
According to the Boston Bowel Preparation Scale (BBPS), the preparation quality score that reflects the sum of the different colon segments ranged between 1 and 9 points with a median of 6 points. Fifty-two patients had a BBPS < 6 points (40%), which was considered as an inadequate preparation, and only 13 patients (10%) had an optimal preparation (BBPS = 9 points).
Energy/protein intake and nutritional deficiency
Energy/protein individual needs and ingestion during the 48h before colonoscopy were evaluated. Mean patient energy and protein needs in our sample corresponded to 4,375 (sd 946) kcal and 182 (sd 39.4) g of protein, respectively. A 48h recall was performed in all patients and the mean total intake during this period was 1,795 (806.2) kcal, with a minimum of 171 kcal and a maximum of 4,242 kcal. Protein intake ranged between 0 g and 233 g, with a mean ingestion of 100 (sd 52.8) g.
The mean of energy ingestion was significantly lower than the mean of energetic requirements (t = 25.01, p < 0.01) via a paired-samples t-test, showing a calculated daily deficiency of approximately 59%. Energy/protein intake and nutritional deficiency are summarized in figure 3. Daily calorie intake was less than 50% of the individual needs in 88 patients (67%) and less than 25% in 29 patients (22%). Mean protein ingestion was also inferior to theoretical needs (t = 15.73, p < 0.01), reflecting a daily deficiency of 45%. There was no significant correlation between energy or protein deficiency and the quality of bowel preparation according to the Spearman's correlation test (p > 0.05).

Fig. 3 Mean total energy and protein intake during the 48 h before colonoscopy and nutritional deficiency calculation during the same period.
The mean energy deficiency of ambulatory patients was similar to hospitalized patients (2282 ± 1364 vs 2634 ± 1143.3 Kcal), via a Student´s t-test for independent samples as the small difference found did not reach statistical significance (t = 1.23; p = 0.22). Protein intake was also similar (82.6 ± 57.9 vs 82.2 ± 60.4 g) in both groups (t = -0.03, p = 0.98). Mean nutritional deficiency in the subgroup of hospitalized patients was 48% of energy and 42% of protein intake (t = -6.39, p < 0.01).
Splitting the sample according to age group as younger (age below 65 years) and older patients (65 years old or older), the mean daily energy deficiency (2,381 ± 1,264 vs 2,782 ± 1,088 kcal, t = -1.83, p = 0.07) and protein deficiency (71.3 ± 63.9 vs 92.8 ± 54.4 g, t = -1.95, p = 0.04) tended to be higher in older patients.
DISCUSSION
The importance of bowel preparation as a major determinant of the efficiency of colonoscopy examination is unquestionable and concerns about this issue have been debated by endoscopy and gastroenterology societies. The preparation should be sufficient to allow the detection of small polyps and ineffective bowel cleansing may result in missed precancerous lesions and increased costs due to repeat procedures. Preparation regimens have improved during recent years with the aim to optimize mucosa visualization and patient compliance 5,6,7,8,9. In fact, it is important that patients are educated and engaged in this process and different studies have shown that effective education significantly improves the quality of bowel preparation 21,22.
Malnutrition contributes to a poor outcome in different clinical scenarios, especially in the pre-operative setting, oncologic patients, intensive care units and elderly individuals. The prevalence of hospital malnutrition is a major health burden and efforts must be implemented in daily practice in order to correct and prevent this condition 2,3,4. Dietary recommendations for colonoscopy preparation remain unchanged in recent years and most are empirical due to the lack of clinical studies. Even though these diets are transient and are implemented over a 48h period, they can induce severe energy and protein deficiency. This may have no consequence in healthy and young patients, especially those undergoing colonoscopy for screening purposes. However, it can have detrimental effects on the nutritional status of older and fragile patients from several risk groups. The present study is innovative since it tried to quantify nutritional deficiency during bowel preparation, which had not been addressed by any other group or scientific society.
Our study was conducted in a hospital setting that included patients undergoing total colonoscopy, most of them in an ambulatory regimen. Although a convenience sample was used, it seems to be representative of our routine population, including patients of both genders, most in the sixth and seventh decade of life, who underwent the procedure according to the usual clinical indications.
Anthropometric and nutritional evaluation
All patients underwent an extensive nutritional assessment using several anthropometric tools. According to our results, a high proportion of patients displayed anthropometric values pointing to some degree of malnutrition, ranging from almost 18% using MUAC and MAMC to 67% when TSF was applied. Most of the patients were overweight/obese according to the BMI value. However, when other parameters were analyzed, this proportion decreased to less than 20%, which reflects the poor accuracy of using BMI alone to assess nutritional status 23. Energy and protein deficiency during colonoscopy preparation may negatively influence muscle and fat mass in patients that present some signs of malnutrition.
Energy/protein intake and nutritional deficiency induced by colonoscopy preparation
Preparation was performed according to our institutional recommendations, which included a low residue diet during the 48 hours before the colonoscopy. A 48h recall was applied to quantify total energy and protein intake. This period included more than 24h under a low-residue diet and also the period after treatment with PEG solution, when ingestion markedly diminished. Energy and protein ingestion varied between practically any food intake (171 kcal and any protein intake) to low grade of restriction (4,242 kcal and 233 g of protein), which suggests that patients were not always sticking to the recommended diet. Nevertheless, most patients had a considerable deficiency with an ingestion level 50% or 25% below the theoretical needs. The deficiency of energy and protein intake was considerable and significant according to our results. Furthermore, the real nutritional deficiency might be higher than that calculated in the present study due to the potential interference caused by colonoscopy preparation in digestion and absorption mechanisms, which is not clearly addressed in the scientific literature.
Induced nutritional deficiency and quality of bowel preparation
A considerable number of patients had a deficient bowel preparation. However, the quality of preparation was not associated with energy and protein deficiency according to our data. In fact, this type of diet may be a more important determinant of bowel preparation rather than the amount of energy and protein intake by itself.
Induced nutritional deficiency in ambulatory and hospitalized patients
There was no significant difference in energy deficiency between ambulatory and hospitalized patients. This might be explained by the fact that nurses help to maintain some oral ingestion. On the other hand, ambulatory patients often tend to reduce further food intake due to the fear of not being well prepared.
Induced nutritional deficiency in young and aged patients
Energy and protein deficiency were more pronounced in patients aged 65 years or older according to our data. In fact, older individuals are particularly vulnerable to malnutrition due to the sensorial changes in smell and taste associated with aging; the inability to prepare meals, leading to a decrease in food intake; and cognitive impairment, which contributes to misunderstandings and a lack of compliance with diet recommendations. Some disorders that are more prevalent in older people also increase nutritional risk. Changes in body composition, in particular age-induced sarcopenia, accelerate with an energy and protein deficiency 24,25. Thus, nutritional deficiency induced by colonoscopy preparation may exacerbate the frailty of older patients and have a negative impact on their clinical outcome, which is a major concern in this age group.
Limitations of the study
There are some limitations of this study, such as the fact that a convenience sample was used. The quantification of energy and protein intake was dependent on what the patient reported, which may not be precise. In addition, the estimation of energy and protein needs was performed using a pre-established formula rather than applying tools such as indirect calorimetry. The clinical impact of nutritional deficiency induced by colonoscopy preparation on patient outcome was not assessed in the present study and further research is needed to clarify the consequences of this deficiency, especially in hospitalized and fragile patients. Analyses of the impact on prognostic variables such as length of hospital stay, perioperative mobility, incidence of infections and overall mortality are also additional valid and pertinent approaches in further studies.
Proposals and author's suggestions
The present study highlights the need to reformulate bowel preparation protocols to minimize nutritional deficiency and its potential negative consequences, especially in the risk group described above. The results obtained in this study prompted our department to modify the bowel preparation regimens used in our hospital. The new protocol includes a two-three day low-residue diet and the concomitant ingestion of hyper-caloric and protein-rich oral nutritional supplements (ONS) without residues, in order to minimize energy and protein deficiency during this period. The impact of this measure is uncertain and is not addressed in previous studies or current international recommendations. However, the simple implementation makes it a feasible option and is only limited by a slight increase in cost.
CONCLUSIONS
Current colonoscopy bowel preparation is efficient but is associated with a nutritional deficiency that reached 59% and 45% of the required energy and protein intake, respectively. Energy and protein deficiency tends to be more pronounced in older patients. The quality of bowel preparation is not directly associated with energy and protein deficiency during preparation. This deficiency might result from institutional regimens with severe restriction protocols and also from the misunderstanding of recommendations by the patients and caregivers. Thus, randomized controlled trials are needed to validate this nutritional deficiency and the real impact on patient nutritional status and clinical outcome. This study highlights the need for the reformulation of preparation regimens and/or for the inclusion of ONS without residues, especially in high-risk groups including older, oncologic and perioperative patients and patients at high nutritional risk or already malnourished.