Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO  Similares en Google
Similares en Google
Compartir
Revista Española de Enfermedades Digestivas
versión impresa ISSN 1130-0108
Rev. esp. enferm. dig. vol.97 no.5 Madrid may. 2005
| POINT OF VIEW |
Spigelian hernia in Spain. An analysis of 162 cases
L. Moles Morenilla, F. Docobo Durántez1, J. Mena Robles1 and R. de Quinta Frutos
Department of General Surgery. Hospital Vigil de Quiñones. 1Unit of Clinical Management (CMA).
Hospital Universitario Virgen del Rocío. Seville, Spain
Moles Morenilla L, Docobo Durántez F, Mena Robles J, de Quinta Frutos R. Spigelian hernia in Spain. An analysis of 162 cases. Rev Esp Enferm Dig 2005; 97: 338-347.
Recibido: 19-04-04.
Aceptado: 01-06-04.
Correspondencia: Luis Moles Morenilla. Avda. San Francisco Javier, 20-A, 3º-2. 41018 Sevilla
INTRODUCTION
Spigelian hernia is a rare defect of the abdominal wall. Incarceration and strangulation are frequent complications. Its diagnosis and treatment are still not standardized. The objective of this work is to review the Spanish bibliography up to 2003, and to bring this hernial pathology up to date. We analyze the number of total published cases, their series, etiopathogenesis, diagnostic procedures, differential diagnoses, and therapeutic alternatives, and the contributions of the video-endoscopic approach. The literature review included 37 papers from Spain with 162 cases, including the personal experience of the authors (16 plus 5 cases).
HISTORICAL BACKGROUND
The Flemish anatomist and surgeon Adrian van der Spiegel (1578-1625) published an anatomical description of the semilunar line (1). In 1764, J. T. Klinkosch described a spontaneous lateral ventral hernia specifically located in the semilunar line (Spigelian line) (2). Spigelian hernia (SH) is infrequently referred to in the worldwide literature. Spangen's review, in 1993, gathered a total of 979 published cases (3). In Spain, Gómez-Ferrer Bayo and Carbonell Antolí first published an article on this pathology in 1965 (4). Later, in 1970, the Barcelona Quirúrgica journal collected another reference to SH by Sueiras Fechtenburg (5). The review conducted by Martínez Díez, in 1975, gathered 9 personal cases and two contributions (6). Other authors have continued adding new cases, these being generally in short series (Table I).
The Spanish literature review and presentation of a 27-patient series by Moreno-Egea et al., in 2002, should be emphasized (5). Finally we quote a worldwide literature review by Moles and Marín in 2003 (17). In the present Spanish review, we studied 162 cases from the literature, included in 37 papers from 1965 to June 2003.
DEFINITIONS
Spigelian hernia is the protrusion of a peritoneal sac or organ, or of preperitoneal fat, through a congenital or acquired defect in Spiegel's aponeurosis (18). These hernias have been described with the names of spontaneous lateral ventral hernia, joint tendon hernia, semilunar line hernia, and ventral interstitial hernia (10,19). The semilunar line runs from the dorsal muscle transition to the aponeurosis in the transverse muscle of the abdomen; it has a lateral convexity between the eighth or ninth costal cartilages and the pubic spine (20). Spiegel's aponeurosis is located between the semilunar line and the external edge of the muscle (21), and SH protrudes through this potentially weak structure. There are two types of SH. Higher SHs are located above the inferior epigastric vessels. Lower SHs include hernias located caudally to these vessels (22). The latter are much rarer and they can be confused with ascending direct inguinal hernias, which protrude below the joint tendon.
ANATOMY
A fact to emphasize is that the fibers of the lesser oblique and transverse muscles in the supra-umbilical region intersect at right angles, making the formation of hernias difficult. Nevertheless, muscle fibers are infra-umbilically almost parallel, thus having less resistance and an increased herniation risk (16). Most hernial orifices occur in the Spigelian hernia belt of Spangen, which is a transverse strip at 0 to 6 cm over the interspinal line (23); in this zone Spiegel's aponeurosis is wider. Almost all SHs are located below the major oblique muscle, among the different muscular layers of the abdominal wall, and called interstitial and hidden hernias (4). In the superficial variety the hernial sac crosses the major oblique aponeurosis and becomes subcutaneous. We have found this subcutaneous location in 0.8% of reviewed cases (1 in 117). The deep variety is less frequent, with the single hernial sac crossing the aponeurosis of the transverse muscle and remaining below the smaller oblique muscle (15). A hernial sac is almost always present.
During surgery the sac was empty in 34.4% of cases (43 of 125). The most frequent hernial contents are the greater omentum (39.1%), small intestine (33.7%) and colon (13.5%). Other intra-saccular organs described include: gallbladder, stomach, Meckel's diverticulum, appendix, epiploic appendix, ovary, uterine leiomyoma, and saccular endometriosis. Also there are references to combined cases of small intestine and omentum, sigmoid and omentum, etc. The hernial orifice is usually small, less than 2 cm in 57% of the reviewed cases; it is oval or rounded in form with well-defined edges (24), which may facilitate hernial strangulation.
INCIDENCE
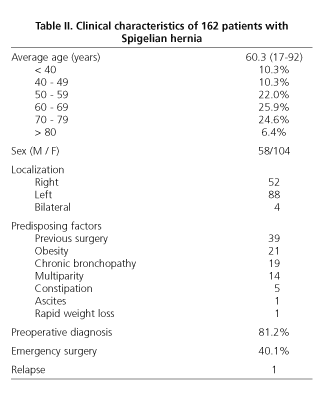
Spigelian hernia is rare, and represents 0.1-2% of all abdominal wall hernias (25). There is a certain predisposition in females. We found in our review 104 women and 58 men, with a female: male ratio of 1.7/1. Regarding the affected side, we compiled 52 right hernias, 88 left hernias and 4 bilateral hernias. The average age of the reviewed cases was 60.3 years, with a range of 17-92 years (Table II). In the worldwide literature we found thirty cases of children younger than 16 years operated on for Spigelian hernia (17). Scopinaro described for the first time (1935) a SH in a boy aged six days, who died from incarceration (26). Several cases of congenital SH associated with non-descended testicle have been described (24).
ETIOPATHOGENESIS
Vascular-nervous theory
Proposed by Astley Cooper, according to which the hernial sac emerges through increased-in-size orifices in Spiegel's aponeurosis by the penetration of the deep iliac artery, a branch of the inferior epigastric artery, or branches of the abdomino-genital nerves (12). However, neuro-vascular bundles have rarely been found in the vicinity of the hernia, which is why this theory is not satisfactory.
The musculo-aponeurotic fasciculation theory
Defended by Zimmerman et al., according to which the lesser oblique and transverse muscles have a fascicular disposition with fibro-adipose zones of reduced resistance. These defects or cracks are found in 6% of cases and provide sites for a possible herniation (27). Preperitoneal fat would infiltrate the deep musculature and weaken it, thus opening the way for the hernia and a stressing of the underlying peritoneum. This is the most accepted theory by authors worldwide.
Embryologic transition theory
The semilunar line, like the white line, has a zone of lower resistance between the anterior rectal muscles derived from the mid mesoderm, and the long muscles derived from the inferior thoracic and lumbar myotomes.
Theory of Watson and Iason
A weakness at the junction of Douglas' line with the semilunar line is the origin of these hernias (13). The concept of only one weak point from stress in the line is incompatible with the multiple sites where SH may appear (Table III).
PREDISPOSING FACTORS
Predisposing factors include those that produce an increase in intra-abdominal pressure: obesity, chronic bronchopathy, multiparity, constipation, ascites, and repeated muscular strain (3). Other implicated factors are peritoneal dialysis, rapid weight loss, and previous abdominal incisions (28). It is possible that the contraction of a scar next to a weak area in Spiegel's aponeurosis may increase the risk of hernia. Most SHs occur in the aged in association with the wearing down of connective tissue. Some neonatal cases have been related to congenital muscular defects (29).
CLINICAL DIAGNOSIS
Symptoms
Some SHs are asymptomatic and show up during an abdominal exploration or an operation. We found 4 well-documented asymptomatic cases among 148. The clinical picture is manifold and confusing, and depends on the saccular content. Delayed diagnosis is frequent. The most frequent symptoms are abdominal pain and a sensation of mass. Pain is nonspecific and increases with effort or strain, cough, and Valsalva's maneuver, whilst improving in selected positions (7). Pain was present in 89 of our 148 cases. The picture can be accompanied by a sensation of abdominal mass, which is sometimes reduced depending on the posture or pressure, located at the external edge of the rectal muscle. Of 148 cases reviewed, 85 patients had been thought to have a mass. Other symptoms include nausea, vomiting, local hyperesthesia, and altered intestinal rhythm (30). The rate of complications is high (31,32) due to delayed diagnosis and the small hernial orifice. In this review (162 cases) there were complications in 35.5% of cases, with the following distribution: incarceration 10.4%, strangulation 6.7%, intestinal obstruction 12.9%, and subocclusion 5.5%. Other potential complications include strangulated hernias of Richter's type and pyo-stercoral abscess by strangulation with perforation.
Physical examination
A soft, deep mass may be felt when the hernia is large. A gurgling sensation will be perceived when the hernia is manually reduced (33), and sometimes the hernial orifice may be felt. The hernia was palpable in 73 (80.2%) of 91 cases analyzed. If the hernial sac progresses in a caudo-lateral direction it may be felt outside the Spigelian zone, thus making the diagnosis difficult (23). When hernias are small they are not usually palpable, these being interstitial cases presenting in the obese. Sometimes when exploring a standing patient a sensation of resistance or a tender point is detected at the hernial orifice. Repeated explorations are necessary due to the difficulties of clinical diagnosis in these hernias.
DIAGNOSTIC PROCEDURES
Simple radiography
Authors, such as Ríos et al., remind us that a simple radiological study is a mandatory, although often inconclusive start point (9). This technique can demonstrate images of intestinal loops in an extra-abdominal location, with tangential views being very useful (34). Sometimes during orthostatism a hydro-air level may be observed (35). Simple abdominal radiology offers the radiological signs of intestinal obstruction (36) in strangulated hernias. Nevertheless this conventional examination is incapable of demonstrating epiploic content within the hernial sac (21).
Barium radiology
Studies with contrast material are of diagnostic utility when the hernial sac contains intestine, as occurred in the case of Cebollero et al. (37). Sometimes the pressure exerted by a contrast material can reduce the hernia. Oblique views are advisable to demonstrate these hernias (34), with an intestinal loop full of contrast material being observed outside the peritoneal cavity. Pérez Nevado et al. insist on the diagnostic value of an opaque enema, with radiological signs such as a greater impression of the proximal branch of the herniated loop, "peak signal", and the intermittent character of the radiological appearance of SH (27). Of 20 diagnostic barium studies (opaque enema and transintestinal) six cases were of positive diagnostic value.
Ultrasonography
The introduction of echography (ultrasounds) translated into important advances in the diagnosis of these hernias by demonstrating musculo-aponeurotic defects in the semilunar line (38). In 1989, Pérez Palma et al. published several cases diagnosed with ultrasounds (11). Because of its innocuity and simplicity it is recommended as a second technique after simple radiology in cases of suspected SH, mainly in emergencies (39). The hernial orifice is shown as an interruption in the line of echoes along Spiegel's aponeurosis (14). Valsalva's maneuver allows an appreciation of the sliding movement of sac contents through the hernial orifice. A typical "hour glass-like" image can be observed in intestinal loops when crossing the aponeurotic defect (39). Of 32 ultrasound studies reviewed in the Spanish literature a correct diagnosis was provided in 22 cases.
Computed tomography
In 1984, Carvajal et al. used computed tomography (CT) to diagnose a SH preoperatively (30). Since then most authors consider CT as the complementary test of choice when faced with the suspicion of SH, since it provides most demonstrative images of the parietal defect, the location and the contents of the sac (35). CT clearly delimits the different muscular layers of the abdominal wall, thus showing the hernia located between the anterior rectum and the transverse muscle of the abdomen (20). CT is the complementary exploration that provides really positive diagnoses. Of 26 reviewed tomographies of the abdominal wall, a correct diagnosis was arrived at in 23. Exact preoperative diagnosis facilitates a suitable approach and improves prognosis.
DIFFERENTIAL DIAGNOSIS
The differential diagnosis of SH must be made with the following pathological conditions: hemangiomas, fibromas, sarcomas, pseudo-hernia, myotendinitis, lipomas, Dercum's disease, metastases, other abdominal hernias, seromas, abscesses, desmoid tumors, and hematomas. It is also necessary to consider the following intra-abdominal diseases: diverticulitis, colonic tumors, peritoneal or epiploic tumor-like implants, pelvic neoplasm, ectopic pregnancy, ovarian cyst, intestinal obstruction, appendicitis, genito-urinary disorders, and cholecystitis (31,38). Abdominal ultrasonography and tomography are very useful in the ruling out of differential diagnoses.
TREATMENT
Treatment is surgical to prevent the frequent complications that may occur. Of 162 cases reviewed, 65 (40.1%) needed urgent surgery. The lateral approach route is most used (6), and is recommended for palpable hernias. The local approach route was used in 78 of 110 cases (Table IV). The major oblique is opened in the direction of its fibers. The sac is secured and dissected to its neck, thus avoiding the escape of hernial contents. The sac is opened and the vitality of viscera is noted, with later extirpation of the peritoneal sac and reconstruction of the wall by individual layers (29). Midline laparotomy is useful for strangulated hernias, since it allows an easy manipulation of hernial contents and a deep orifice (40). With this approach the abdominal cavity, the wall, and the opposite side can be explored. This route was used in 9 of 110 cases. Spangen proposed the preperitoneal route for non-palpable hernias. This approach, through a vertical incision, allows good visualization, a preperitoneal exploration, and the treatment of other associated hernias, and is appropriate for an exploratory laparotomy (22). The preperitoneal route is scarcely used in Spain.
Some authors have proposed a reinforcement of the wall by imbricating the external oblique aponeurosis in the Mayo fashion; a plastia of the rectal sheath or a fascia lata flap (41). Using a prosthesis of synthetic material when the aponeurosis is atrophic or defects are big, and in relapsed cases is often advisable (40). A mesh is placed between the peritoneum and the wide muscles, between two muscular sheets or in a plug form. Hernial recurrence is exceptional. In Spain, Daban et al. communicated one case (8).
Endoscopic surgical techniques
Since 1992, the endoscopic approach began to be used in the treatment of SH. In Spain, Salvador et al. published an intra-abdominal endoscopic repair in 1995 (42). Two varieties of endoscopic surgical treatment exist: transperitoneal and extraperitoneal. In the transperitoneal route, most authors close the defect by stapling prosthetic material to the abdominal wall, with or without previous suture of the hernial orifice (36). If a SH is incidentally discovered during an endoscopic exploration then repair by this route is advised in order to avoid the high risk of complications these hernias entail. The transperitoneal technique allows an exploration of the contralateral side and the abdominal cavity, and an excellent operative visualization (43). The endoscopic approach avoids the opening of the major oblique aponeurosis; it diminishes postoperative pain and the risk of dehiscence (42). Other advantages include a reduction of infection and earlier return to normal activity (44).
Moreno-Egea et al. introduced an extraperitoneal endoscopy technique in 1998 (45). This approach involves a balloon-mediated dissection, and does not require general anesthesia, thus allowing its performance on an outpatient basis and avoiding the potential morbidity of the intraabdominal route (46,47). In Spain, 23 procedures for Spigelian hernia using endoscopic techniques have been described in five different centers since 1995.
CONCLUSIONS
Being interstitial, the diagnosis of SH is difficult on many occasions. SH often has serious complications. There are few publications on this pathology among Spanish authors. These hernias are interesting and challenging for general practitioners, gastroenterologists, radiologists, and surgeons alike -those who may suspect the presence of SH when faced with atypical abdominal pain. Both sonography and CT are helpful diagnostic tools. Treatment is surgical, with excellent results. The videoendoscopic approach may contribute benefits with a reduction in hospital stay time, postoperative analgesia, and surgical wound infection.
REFERENCES
1. Spiegel A. Opera quae extant omnia. Amsterdam: John Bloew, 1645: 103. [ Links ]
2. Klinkosch JT. Divisionem herniarum novamgue herniae ventralis speciem proponit. Dissertationum medicorum, 1764; 184. [ Links ]
3. Spangen L. Spigelian hernia. En: Nyhus LM, Condon RE, eds. Hernia. 4ª. ed. Philadelphia: JB Lippincott Co., 1995. p. 381-92. [ Links ]
4. Gómez-Ferrer F, Carbonell C. Hernia de Spiegel. Cir Ginecol Urol 1965; 19. p. 39-44. [ Links ]
5. Moreno-Egea A, Flores B, Aguayo JL, Canteras M. La hernia de Spiegel en España: revisión bibliográfica y presentación de una serie personal de 27 pacientes. Cir Esp 2002; 72: 18-22. [ Links ]
6. Martínez Díez M, González González M. A propósito de dos nuevos casos de hernia de la línea semilunar de Spiegel. Rev Esp Enferm Dig 1975; 46: 675-84. [ Links ]
7. Moles L, Fernández J, Ortiz C, de Quinta R, Díaz E, Ramos J. Hernia de Spiegel. A propósito de 16 casos. Cir Esp 2000; 67: 572-5. [ Links ]
8. Dabán F, Capitán JM, Jiménez J, Mezquita S, Nogales J, Cobo G. Hernia de Spiegel. Nuestra experiencia. Cir Esp 1992; 52: 45-8. [ Links ]
9. Ríos A, Rodríguez JM, González R, Ortiz S, Carrasco M, Parrilla P. Hernia de Spiegel: múltiples presentaciones de una hernia poco frecuente. Cir Esp 1999; 65: 123-6. [ Links ]
10. Novell F, Badía JM, Suñol J. Hernia de Spiegel. Rev Quir Esp 1987; 14: 205-8. [ Links ]
11. Pérez Palma J, Alarco A, Bordallo A, Pastor S, Hernández-Siverio N, Herrero A, et al. Hernia de Spiegel. A propósito de diez casos. Rev Esp Enferm Dig 1989; 76: 321-4. [ Links ]
12. Guirao J, Mansilla D, Pérez J, Vázquez J, Falomir G, Martín L, et al. Tratamiento de la hernia de Spiegel con mallas de polipropileno. Nuevo enfoque terapéutico. Cir Esp 2000; 67: 192-5. [ Links ]
13. Fernández L, Roig J, Monzón A, Gómez A, Pellicer JL, Tieso E, et al. Hernia de Spiegel: a propósito de siete casos. Rev Esp Enferm Dig 1989; 75: 267-70. [ Links ]
14. González-Uriarte J, Irazusta M, Gurruchaga JM, Álvarez J, Mendoza M, Almeida M, et al. Hernia de Spiegel. Diagnóstico y epidemiología. Cir Esp 2000; 68: 74-6. [ Links ]
15. Docobo F. Hernias de Spiegel. Revisión de una serie de 5 casos. Rev And Pat Digest 1997; 20: 80-2. [ Links ]
16. Lesaga J, Martínez C, Ramos R, García FJ, Suberviola E, Lucea C. Hernia de Spiegel. Cir Esp 1991; 50: 59-61. [ Links ]
17. Moles L, Marín J. Hernia de Spiegel. Estado actual. Cir May Amb 2003; 8: 69-78. [ Links ]
18. Skandalakis LJ, Gadacz TR, Mansberger AR Jr, Mitchell WE Jr, Colborn GL, Skandalakis JE. Spigelian (lateral ventral) hernia. En: Modern Hernia Repair. The embryological and anatomical basis of surgery. Carnforth: Parthenon Publishing Group, 1996. p. 71-4. [ Links ]
19. Weiss Y, Lernau OZ, Nissan S. Spigelian hernia. Ann Surg 1974; 180: 836-9. [ Links ]
20. Quiroga S, Romero I, Álvarez-Castells A, Sebastiá MC, Pallisa E, Tur C. Hernias abdominales externas y diafragmáticas. Hallazgos en la TC. Radiología 1997; 39: 677-83. [ Links ]
21. Pichi M, Pacífico G, Landi L, Corsi A, Rizzo DM, Senesi S, et al. L´ernia di Spigelio. Considerazioni anatomo-cliniche. Minerva Chir 1999; 54: 425-31. [ Links ]
22. Spangen L. Spigelian Hernia. World J Surg 1989; 13: 573-80. [ Links ]
23. Gómez Portilla A, Hernández Lizoaín JL, de Oca J, Zorzona G. Hernia de Spiegel. Aportación de tres nuevos casos. Rev Esp Enferm Dig 1987; 71: 247-9. [ Links ]
24. Silberstein PA, Kern IB, Shi ECP. Congenital Spigelian hernia with cryptorchidism. J Pediatr Surg 1996; 31: 1208-10. [ Links ]
25. Vara R, Rosell J, Guerrero JA, Ruiz A. Hernias externas simples y complicadas de la pared abdominal del adulto: 1635 casos. Cirugía Ibero-Americana 1993; 2: 58-64. [ Links ]
26. Scopinaro AJ. Hernia de la línea semilunar de Spiegel en un recién nacido. Semin Med 1935; 1: 284-9. [ Links ]
27. Pérez Nevado A, González N, Ramos SM, Torres G. Anatomía y radiología de las hernias de Spiegel. Aportación de un caso y revisión de la literatura. Radiología 1977; 19: 447-54. [ Links ]
28. Pardo L, Dávila D, Chamorro JJ. Hernia de Spiegel tras abdominoplastia. Cir Esp 1999; 65: 349-52. [ Links ]
29. Serrano P, Miras M, Sanz C. Hernia de Spiegel. Aportación de dos casos. Rev Esp Enferm Dig 1980; 57: 443-8. [ Links ]
30. Carvajal J, Climent V, Abellán J, García R, Capel A. Hernia de Spiegel. Valor de la tomografía axial computarizada. Radiología 1984; 26: 71-3. [ Links ]
31. Jerez B, Jerez RL, Mora G, Brusint B. Hernia de Spiegel en la consulta de Atención Primaria: a propósito de un caso. Medifam 2000; 10: 380-2. [ Links ]
32. García Pugés AM, Rovira JM, Gimeno F, Vilar J. Hernias de Spiegel. En: Gastroenterología y Hepatología. 1ª ed. Barcelona: Mosby 1982. p. 261-5. [ Links ]
33. Poza J, Barrera C, Amato E, Anasagasti I. Una causa poco frecuente de suboclusión intestinal. Rev Esp Enferm Dig 1989; 75: 216-7. [ Links ]
34. Gimeno F, Rovira JM. Diagnóstico casual de hernias de Spiegel por enema opaco. Rev Esp Enferm Dig 1996; 88: 643-4. [ Links ]
35. Apesteguía L, Lecumberri F, Bilbao JI, Aquerreta D, García F, Zornoza G. Tomografía axial computarizada en el diagnóstico de hernia de Spiegel. A propósito de un caso. Cir Esp 1985; 39: 1051-4. [ Links ]
36. Adell R, Salvador JL, Laguna M, Navarro J, Gibert J, Escrig J, et al. Hernia de Spiegel. Formas de presentación clínica y alternativas terapéuticas. Cir Esp 1996; 60: 14-6. [ Links ]
37. Cebollero MP, Escartín J, Blanco FJ. Intestinal occlusion and Spigelian Hernia. J Clin Gastroenterol 1999; 29: 213-4. [ Links ]
38. Zaragoza C, Villalba S, Castaño S, Trullenque R. Hernia de Spiegel. Cir Esp 1996; 59: 165-7. [ Links ]
39. Roig J, Olivet F, Bassaganyas R, Serres J, Farres R, Masvidal R. El valor de la ecografía y de la tomografía axial computarizada en el diagnóstico de las hernias abdominales altas. Cir Esp 1992; 51: 221-3. [ Links ]
40. Moles L, Ortiz C, Martín R, Fernández J, Sánchez M. Hernia de Spiegel conteniendo colon sigmoides con diverticulitis perforada. Med Mil (Esp) 1999; 55: 83-5. [ Links ]
41. Alexandre JH, Bouillot JL. Traitement chirurgical des hernies de Spieghel ou hernies ventrales latérales ou anterolatérales. En: Elsevier, ed. Encycl. Méd. Chir. Techiques chirurgicales. Paris: Appareil Digestif, 1994. p. 40-151. [ Links ]
42. Salvador JL, Laguna M, Adell R, García R, Gibert J. Reparación de hernia de Spiegel por vía laparoscópica. Rev Esp Enferm Dig 1995; 87: 759-60. [ Links ]
43. Novell F, Sánchez G, Sentís J, Visa J , Novell J, Novell F. Laparoscopic management of Spigelian hernia. Surg Endosc 2000; 14: 1189. [ Links ]
44. García Molina F, Ortegón B, Franco JD, Domínguez-Adame E, Gil FJ, Gutiérrez C, et al. Tratamiento laparoscópico de la hernia de Spiegel. Cir Esp 2002; 71: 207-9. [ Links ]
45. Moreno-Egea A, Torralba JA, Aguayo JL. Totally extraperitoneal laparoscopic repair of spigelian hernia. Eur J Coeliosurg 1999; 32: 83-4. [ Links ]
46. Moreno-Egea A, Girela E, Torralba JA, Aguayo JL. Descripción de la técnica laparoscópica totalmente extraperitoneal en el tratamiento de la hernia de Spiegel. Video-Review of Surg 2000; 2: 23-7. [ Links ]
47. Moreno-Egea A, Girela E, Torralba JA, Aguayo JL. Tratamiento laparoscópico ambulatorio de la hernia de Spiegel: presentación de 10 casos. Cir Esp 2002; 71: 221-3. [ Links ]











 texto en
texto en