Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Archivos Españoles de Urología (Ed. impresa)
versión impresa ISSN 0004-0614
Arch. Esp. Urol. vol.62 no.7 sep. 2009
Fournier's gangrene: Our experience in 5 years, bibliographic review and assessment of the Fournier's gangrene severity index
Gangrena de Fournier: Nuestra experiencia en 5 años, revisión de la literatura y valoración del índice de severidad de la Gangrena de Fournier
Alejandro García Morua, Juan Antonio Acuña López, Jesús Domingo Gutiérrez García, Rafael Martínez Montelongo and Lauro Salvador Gómez Guerra.
Department of Urology. Hospital Universitario Dr. José Eleuterio González. Monterrey. Nuevo León. México.
SUMMARY
Objectives: Fournier's gangrene is a devastating infection, which includes the genital, perineal and / or perianal regions. It is potentially fatal, and affects any age and gender. The severity index for Fournier's gangrene has been described; it is useful for evaluating the prognosis of these patients.
Our goal is to report our experience with this disease over the past 5 years and evaluate the index in retrospect.
Methods: We analyzed medical records of patients with Fournier gangrene over the last 5 years at the University Hospital "Dr. José E. González".
Results: We reviewed 50 cases, male gender was predominant (96%), mean age 47.5 years, diabetes mellitus was found in 80%, neurogenic bladder in 10%, 2% HIV positive. The most frequent sites of origin of infection were scrotum (52%) and perineum (38%), the most common pathogen E. coli and Enteroccocus faeca-lis (48 and 28% respectively). The death rate was 12%. The average severity index was 5.64.
Discussion: In our hospital, Fournier's gangrene is rare. Nevertheless, there is a rapid diagnosis protocol and therapeutic management is performed immediately. Until now, the immediate surgical treatment and early initiation of antibiotic therapy remains the best therapeutic option.
Conclusion: There is a relationship between the index of severity and patient survival, which may become a useful parameter in evaluating these patients.
Key words: Fournier's gangrene. Severity Index. Necrotizing fasciitis. Genital gangrene.
RESUMEN
Objetivo: La gangrena de Fournier es una infección fulminante, que abarca las regiones genital, perineal y/o perianal. Es potencialmente letal, afecta cualquier edad y género. Se ha descrito el índice de severidad de gangrena de Fournier, el cual es útil para evaluar el pronóstico de estos pacientes.
Nuestro objetivo es reportar nuestra experiencia con esta patología en los últimos 5 años y evaluar el índice de manera retrospectiva.
Métodos: Se analizaron los expedientes clínicos de los pacientes con gangrena de Fournier los últimos 5 años en el Hospital Universitario "Dr. José E. González".
Resultados: Se revisaron 50 expedientes, el género predominante fue el masculino (96%), la edad promedio 47.5 años, se encontró diabetes mellitus en un 80%, vejiga neurogénica 10%, HIV positivo 2%. Los sitios de origen más frecuente de infección fueron escroto (52%) y periné (38%), los agentes patógenos más frecuentes E. coli y Enteroccocus faecalis (48 y 28% respectivamente). El porcentaje de defunción fue del 12%, el índice de severidad promedio fue 5.64.
Discusión: En nuestro Hospital, la gangrena de Fournier es una patología poco frecuente; a pesar de esto, se cuenta con un diagnóstico rápido y a su vez un manejo inmediato. Hasta el momento la conducta quirúrgica inmediata y el pronto inicio de antibioticoterapia continúan siendo la mejor opción terapéutica.
Conclusión: Existe una relación entre el índice de severidad y la sobrevida de los pacientes, lo cual puede convertirlo en un parámetro útil en la evaluación de estos pacientes.
Palabras clave: Gangrena de Fournier. Índice de severidad. Fascitis necrotizante. Gangrena genital.
Introduction
Fournier's gangrene is a fulminant infection, including necrotizing fasciitis type regions genital, perineal and / or perianal. This infectious and necrotic skin lesion, although it was initially described by Bau-rienne in 1764 (1,3) is named after Jean Alfred Fournier, French dermatologist who in 1883 described a syndrome of unexplained gangrene in the penis and scrotum in 5 young men with no other pathology basis of sudden onset and rapid progresion (2).
This condition is potentially fatal, affects any age and gender, has been reported even in neonates (4), is characterized by rapid progression of infection in soft tissue caused by the synergistic action of several agencies that extend along fascial planes, subfacial causing necrosis of these tissues and destruction (5). This necrosis is secondary to thrombosis of small vessels, which is due to endarteritis obliterans caused by the spread of microorganisms into the subcutaneous space (platelet aggregation stimulated by heparinasa produced by aerobic and anaerobic) (3), that in addition to generating local edema, hypoxia, difficulty by local blood supply, which favors the development of anaerobic bacteria, these microorganisms produce hydrogen and nitrogen that accumulate in tissues causing crepitation (5).
Among the most frequent concomitant diseases are diabetes mellitus (present between 32 - 66% of cases) (6), alcoholism and cancer, among other immunosuppressive diseases.
It is a situation that warrants urgent radical surgical treatment (debridement), in addition to the use of antibiotics apropiados (7). Mortality has been reported in different series, ranging from 3 - 67% in unas7 0 - 80% others (3).
Its clinical presentation is variable but often does so with edema, erythema, pain, fever and increased volume, the crepitus is present in 50-62% of cases (3). The time interval from onset of symptoms specific to the process until the request for medical care is from 2 to 7 days, on average. This time determines the extent of the necrotic area and a critical influence on the prognosis (1). Within the imaging studies of X-rays are useful in demonstrating the presence of gas in soft tissues, more useful is the ultrasound. who can demonstrate the presence of diffuse edema, thickness of the scrotal wall and possibly the penis and the presence of escrotal gas (3).
Has been described gangrene severity index of Fournier (5,8) (Table I), which is useful for evaluating the prognosis of these patients.
The management ranges from emergency surgery (debridement), managing topic (sodium hypochlorite, hydrogen superoxide and even honey), antibiotics, until hiperbaric oxygen (12,18).
Objective
The purpose of this paper is to report our experience over the past 5 years regarding this disease and to assess retrospectively the rate of severity and to assess whether our results are comparable to those published.
Material and methods
We analyzed medical records of patients admitted with a diagnosis of Fournier's gangrene in a period from June 2002 to June 2007, at the University Hospital "Dr. Joseph E. González".
The criteria used to establish the diagnosis were the anamnesis and physical examination of patient records were incomplete and excluded those who did not meet inclusion criteria.
All patients required early surgical debridement and administration of parenteral antibiotics for at least a double outline, this will change once the antibiograms obtained from samples sent to bacteriology.
We analyzed in retrospect the clinical records of these patients, assessing the age, gender, symptoms, physical examination, laboratory tests on admission, surgical procedures performed, transfusion, pathogen isolation, antibiotic administered and index of severity for this way to establish the criteria that could be very useful to evaluate these patients in the emergency department to predict what the prognosis for each.
Results
We obtained a total of 63 cases of patients with Fournier's gangrene in this period of 5 years, of whom 13 were excluded for not fulfilling the inclusion criteria. Of the 50 patients were reviewed, the male gender was predominant, with 48 men (96%) and 2 (4%) women, mean age was 47.5 years, ranging from 6 to 86 years (Figure 1) . Analyzing pathological antecedents, we find the presence of diabetes mellitus in most patients (80%) of whom 50% (25 patients) already had a diagnosis of DM2, with a diagnosis of DM1 (2%) and the diagnosis was performed in 14 patients (28%), at the time of admission to the emergency adult, other personal pathological significance neurogenic bladder were found in 5 patients (10%) and there was no history of importance in 6 patients (12%), only found one (2%) HIV positive. 48% had a history of smoking and alcohol positive.

The most common symptoms at the time of admission were attack the generally state (80%), scrotal volume increase (84%), fever (74%), perineal or genital pain (68%) (Figure 2), the average time of symptoms prior to referral to treatment was 6.87 days, ranging between 2 - 15 days.

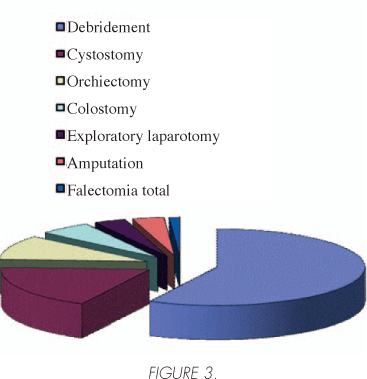
Within the surgery procedures, debridement was performed at 100% of patients, cystotomy to 32%, orchidectomy 18% and colostomy 10% (Figure 3) were performed on average 1.68 operations per patient (range 1-5) transoperative bleeding was evaluated and documented between 100 and 2000cc, with an average of 496cc, was evaluated as the time in the first surgical intervention being between 30 and 360 minutes with an average of 122.4 minutes.
The most common site of origin of infection was 52% in the scrotum, followed by perianal in 38% (Figure 4), it is striking that in the patients who died perianal origin was the most frequent followed by urethral. The most frequent pathogens were E. coli and Enteroccocus faecalis (48 and 28% respectively) (Table III), 58% of patients had infections polibacte-rianas, 14% monobacterianas and 6% of cases the culture was negative in 22% was not found cultivation. The antibiotics scheme most commonly used was Ofloxacin 400mg IV every 12hrs plus clindamycin 600 mg IV every 6hrs, which was modified according to the antibiogram results. And if it changed was added a third-generation cephalosporin.



14 patients (28%) required intensive care unit stay there for an average of 7 days, the average hospital stay was 23.76 days (range 15 hrs to 95 days). The death rate was 12% (6 patients) (Table II), the severity index calculated ranged from 0 - 14 (average 5.64).
Discussion
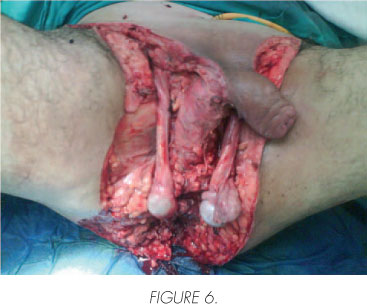
Fournier's gangrene is a necrotizing fasciitis of soft tissues of the scrotum and perineum of very rapid evolution can affect both men and women and usually patients have concomitant risk factors (2,14) (Figure 4 and 5). Therefore we must consider it as a urológica! emergency because if not treated quickly mortality of this condition is usually very high (11). In its early Fournier's gangrene was described as an idiopathic entity, but in most cases a perianal infection, urinary tract and local trauma or skin condition at that level can be identified (9), as noted in our review most of the patients had infection as the origin of the perianal area, scrotum, or urethra and others, there was none in which the origin could not be identified.

The average age was 47.5 years, in most published series from 40.9 to 61.7 years (20), we present a range of 6 to 86 years (the child of 6 years presented Fournier's gangrene following varicella infection involving the scrotum). It is important to emphasize these results because, as we see is a condition that is often present in patients of childbearing age in particular, decreasing at the extremes of life, for reasons that are not entirely clear but could be related with sexually active or simply with the activity of the patient.
With regard to gender, the male predominance in 96%, so the female was present in 4%, which is reported in the literature is often a male, 10 times the female (20), in our experience this ratio was 26 times higher.
At the onset of this pathology has been implicated in a number of factors, especially those that involve or interfere with the immune system, diabetes mellitus being the most frequently found co-morbid disease have been reported series where the frequency of this pathology in patients with Fournier's gangrene ranges from 55 to 70% (2,6) in the series that we present this figure is very similar in patients who were known diabetics (52%), but at the beginning we found that 28% were unaware they were diabetic and diagnosed so far, which shows the role of uncontrolled diabetes mellitus in the pathogenesis of this disease, as 100% of patients were known diabetics who were not wearing a proper control metabolism, the mean numbers of serum glucose of 268mg%. Of the 6 patients who died, 3 were known diabetics (one with figures of serum glucose to 784), 2 were not known diabetic and was diagnosed during their stay in the institution and not the one suffering.
Relationship was found between increased mortality and duration of symptoms before hospitalization, the percentage of area involved, and presence of serum BUN and creatinine hogh (15), we found that patients who died were on average 7.5 days of symptoms prior to their income compared with 6.8 days for those who survived, as well as BUN and serum creatinine higher in those who died compared with survivors (BUN 55.3 - 27.99 and Creatinine 2.7 - 1.5 respectively).
The most common sites are launched from the urethra (trauma, urolithiasis, catheterization, fistulas, stenosis, massage or prostate biopsy), anorectal (perianal abscesses, fissures, hemorrhoids, carcinoma, appendicitis, diverticulitis, and perforation by foreign body), skin infections (insertion of penile prosthesis, cauterization of warts, skin abscesses) and in women (Bartholin abscess, vulvar, vulvar or perineal wounds, episiotomy, hysterectomy, septic abortion, etc... ) (3,5).
No difference was found between the most common site of origin in our series compared with those reported in the literature, these being the scrotum, perianal and urethral like these more frequent and the perianal the worst prognosis (12).
This entity represents a polymicrobial infection in most cases, so that both aerobic and anaerobic organisms may be present, although not all bacteria involved can be identified in cultures (23). Anaerobic bacteria are the least frequently isolated, and enterobacteria in turn are the most frequent and are usually found in particular E. coli, Bacteroides and streptococci, staphylococci, and Clostridium Peptoestreptococos have also been found.
The aerobic bacteria causing platelet aggregation and an acceleration of coagulation by complement fixation, while certain anaerobes promote the formation of clots in a different way to produce a heparinasa. These factors explain the characteristic obliterated endarteritis with vascular thrombosis observed in this necrotizing fasciitis which is responsible for the subcutaneous tissue necrosis and gangrene of the skin. Bacteroides inhibit the phagocytosis of aerobic bacteria destruction. In this way, it is a destructive infection of the combination of relatively non-pathogenic organisms and the immune status of the patient.
In our series, 58% of patients had polymicrobial infection, and within the most common pathogen E. coli, E. faecalis and Pseudomonas aeruginosa were the most frequent (48, 28 and 16% respectively), and it is also important to mention that 6% of patients with cultures of secretions were negative, most likely because it was not for cultivation or not anaerobic ask for fungi, although candida was found in 12% (6 patients) of crops, which was considered rare as described Kazuyoshi and colleagues in 2000 to publish the report of a case of Fournier's gangrene caused by Candida species as the primary microorganism (22), worth mentioning that 5 of these 6 patients (83.3%) were diabetic and one of them died.
Cutaneous manifestations begin with edema, erythema and local hardening of the tissue surface areas later appear as echymosis and necrosis that often accompanied by crepitation and end of drainage purulent material (2). Systemic manifestations are also quite varied and usually attack from the state, fever, to the presence of septic shock and usually these manifestations are related to the extent of necrosis. In our review there was no difference in the presence of these symptoms and necroting ulcer presented in 50% of patients, which is much higher than those reported in the literature that does not exceed 37.5% (2). With regard to laboratory findings showed leukocytosis and the majority as mentioned in the review that we do in presenting septic shock thrombocytopenia can occur as a decrease in clotting factors.
Regarding the management of these patients have been reported multiple behaviors, what is relevant is that in all situations is always recommended surgical management is more aggressive surgical debridement of the administration of broad-spectrum antibiotic therapy, at least one double schema, or possibly a triple scheme depending on the situation (19), and has even described the use of hyperbaric oxygen (23,24), in this situation with apparently good results, without forgetting the importance of healing prevalent in these patients, main recommendations the use of iodized solutions as it was in our review as this was the solution most frequently used have been described also the use of honey as a hyperosmolar solution that determines the destruction of the cell wall of microorganisms, which also promises high expectations, in our experience this behavior was used in 8 patients (16%), with very good results.
The diagnosis was based on clinical findings. Conventional radiology can be helpful in assessing some cases revealing the presence of gas in soft tissues. This is not pathognomonic but must warn of the possibility of necrotising subcutaneous infection. Ultrasound can be useful for distinguishing between Fournier's gangrene and other diseases that occur with scrotal pain, erythema and scrotal volume increase. CT and MRI can help us to delineate the extent of infection and location of outbreaks. These studies are essential for a correct diagnosis and offer appropriate treatment. In our series, no methods were used for imaging studies due to diagnostic certainty provided by the clinic as well as the lateness of the table at the beginning.
The basis of treatment is an early and aggressive radical action with surgical debridement (18), as has been documented that once it establishes this gas gangrene often advance to 1cm for hours (26), so that once the diagnosis is essential to the surgical debridement and as early as the Fournier's gangrene is dynamic sometimes you can not remove 100% of the necrotic tissue with the first debridament (17), for this to be very aggressive so it is not uncommon for patients requiring more a surgical debridement before being considered as resolved infection, as in this revision, as we reported a rate of 1.68 surgeries per patient with a range that varied from 1 to 5.
The leads from the urinary tract as a tract gastrointeestinal are sometimes necessary to ensure proper development of the wound and prevent contamination of the same, we find that cystostomy was performed to 32% of our patients and colostomy only 10% of these.
In our study, all patients received antimicrobial therapy of first instance with a double outline based Ofloxacin 400mg IV every 12hrs more Clindamycin 600mg IV every 6hrs, covering this way gramm negative, positive and anaerobic, this scheme was modified after it had the antibiogram and the culture of the abscess secretion, which never exceeded 7 days.
On admission all patients received surgical and medical management as soon as possible in this way trying to avoid increased morbidity and complications death of the patient, and analyzing this situation we find that there are several attempts to predict the prognosis of patients with Fournier's gangrene, Laora et al. (8) in 1995 and designed the FGSIS (Fourniers's Gangrene Severity Index Score) which is a modification of the already known APACHE II (Acute Physiology and Chronic Health Evaluation II) in which they found that patients who survived were found in an average range of 6.9 ± 0.9 and those who survived had no values averaged 13.5 ± 1.5, finding statistical significance to these results, and more recently Ahmet et al. (9) and evaluating the same index values were very similar, an average of 11.56 ± 2.68 with no survivors and 5.11 ± 2.83 in those who survived. In our series, comparing the 6 patients who died with 44 other survivors are a FGSIS of 9.8 for those who died at an average of 5.64 for survivors, which is very close to those reported by them in their studies of 30 patients. It has been well documented usefulness of this index for predicting hospital stay and the number of debridement in patients who survived (8-11), which could not be demonstrated in our series.
Hospitalization for this disease is extremely long, refers to an average of 6 weeks (23) which is far above average that we found was 23.76 days (3.4 weeks) and mortality is often reported very variable from 0 to 80% (3,23) in our series is not as high as it turned out to be 12%, whereas the number of patients who are at significant compared with those found in other literatures.
Conclusion
Fournier's gangrene in our area is almost exclusively in males and frequently is associated with the presence of diabetes mellitus, even in some cases may be the initial manifestation of the disease.
There is a delay of almost a week between the onset of first symptoms and seeking medical care, which negatively affects the prognosis of the patient.
The debridement is the main form of surgical treatment of the disease and requires further surgical intervention in most patients.
The site of origin of the infection more common in our patients was the scrotum, however appears to have increased severity of the process and even higher mortality in cases that originated in the perianal region.
The etiologic agent in most cases was Escherichia coli, although in nearly 6 out of 10 cases the infection was polymicrobial, which requires the use of schemes with several antibiotics in initial form, with the subsequent modification of the scheme as findings in the cultures.
Despite appropriate treatment, mortality associated with the disease is high, thereby requiring a multidisciplinary and aggressive management, including many of requiring placement in intensive care. Mortality is directly associated with the index of severity of gangrene.
 Correspondence:
Correspondence:
Alejandro García Morua
Servicio de urología
Hospital Universitario José Eleuterio González
Avenida Francisco I Madero S/N
esquina Avenida Gonzalitos
Colonia: Mitras Centro
64460 Monterrey. Nuevo León. (México)
agmoura@hotmail.com
Accepted for publication: May 26th, 2008.
References and recomended readings (*of special interest, **of outstanding interest)
1. Rdz Alonso A, Pérez García D A, Núnez López A, Ojeda Calvo A, Alonso Rodrigo A, Rodríguez Iglesias B et al. Gangrena de Fournier: Aspectos Anátomo-clínicos en el adulto y en el niño. Actualización terapeutica. Actas Urol Esp. 2000; 24 (4): 294-306. [ Links ]
2. Planelles Gómez J, Vergés Prósper A, Rubio Tortosa I, Beltrán Armada J R, Carrascosa Lloret V y San Juan de Laorden C. Gangrena de Fournier". Arch. Esp. Urol. 2006; 59, (8) 767-771. [ Links ]
**3. Smith G L, Bunker G B and Dinneen M D. Fournier's gangrene. BJU 1998; 81: 347-355. [ Links ]
4. Adams JA, Culkin DJ, Mata JA, Bucchini JA, Venable DD. Fournier's gangrene in childrens. Urology 1990; 35: 339-41. [ Links ]
5. Valagues Velasquéz C,Rodríguez García A, Arenas Ozuna J. Gangrena de Fournier en el hospital de infectología del centro médico nacional La Raza, análisis de 2 años. Educación e investigación clínica Vol. 2, No 1. Enero-Abril 2001: Pag 18-25. [ Links ]
6. Nisbet A A and Thompson I M. Impact of Diabetes Mellitus on the presentation and outcomes of Fournier's Gangrene. Urology 2002; 60: 775-79. [ Links ]
7. Corman J M, Moody J A and Aronzon W J. Fournie's Gangrene in a modern surgical setting: Improved Survival with aggressive management. BJU Int 1999; 84: 85-88. [ Links ]
8. Laor E, Palmer L S, Tolla B M, Reid R E and Winter H I. Outcome prediction in patients with Fournier's Gangrene. J. Urol. July 1995: 154: 89-92. [ Links ]
*9. Ersay A, Yilmaz G, Akgun Y and Celik Y. Factors affecting mortality of Fournier's Gangrene: Review of 70 patients. ANZ J. Surg. 2007; 77: 43-48. [ Links ]
*10. Cem Ozden Yeniyol, Tufan Suelozgen, Murat Arslan, and Ali Riza Ayder. Fournier's gangrene: experience with 25 patients and use of Fournier's gangrene severity index score. Urology, August 1, 2004; 64(2): 218-22. [ Links ]
*11. Tuncel A, Aydin O, Tekdogan U, Nalcacioglu V, Capar Y, and Atan A. Fournier's gangrene: Three years of experience with 20 patients and validaty of the Fournier's Gangrene Severity Index Score". Eur Urol, October 1, 2006; 50(4): 838-43. [ Links ]
12. Irazu J C, de Miceu S, Salas J, Katz O N, Eche-guren E S, Blundo O A. Gangrena de Fournier: Nuestra experiencia clínica, etiopatogenia y tratamiento. Actas Urol Esp. 1999; 23 (9): 778-783. [ Links ]
13. Ferreira PC, Reis JC, Amarante JM, Silva AC, Pinho CJ, Oliveira IC, da Silva PN. Fournier's gangrene: a review of 43 reconstructive cases. Plast Reconstr Surg. 2007 Jan;119(1):175-84 [ Links ]
14. Eke N. Fournier's gangrene: a review of 1726 cases. Br J Surg, June 1, 2000; 87(6): 718-28. [ Links ]
15. Jeong H J, Park S C, Seo I Y and Rim J S. Prognostic factors in Fournier gangrene. Int J Urol, December 1, 2005; 12(12): 1041-4. [ Links ]
16. Gürdal M, Yücebas E, Tekin A, Beysel M, Aslan R, Sengor F. Predisposing factors and treatment outcome in Fournier's gangrene. Analysis of 28 cases Urol Int, January 1, 2003; 70(4): 286-90. [ Links ]
17. Quatan N and Kirby R S. Improving outcomes in Fournier's gangrene BJU International 2004 (6), 691-692. [ Links ]
18. Chawla S N, Gallop C, Mydlo J H. Fournier's Gangrene: An Analysis of Repeated Surgical Desbridement. Eur Urol 2003. Vol 43: 572-575. [ Links ]
*19. Norton K S, Johnson L W, Perry T, Perry K H, Sehon J K, Zibari G. Management of Fournier's gangrene: An eleven year retrospective analysis of early recognition, diagnosis, and treatment. The am surg Aug 2002. Vol 68; 8, Pag 709. [ Links ]
20. López Samano V, Ixquiac-Pineda G, Maldona-do Alcaraz E, Montoya G, Serrano Brambila E, Peralta Alarcon J. Gangrena de Fournier: Experiencia en Hospital de Especialidades del CMN SXXI" Arch Esp Urol, 2007: 60 (5): 525-530. [ Links ]
21. Sánchez Mazzaferri F, Fadil Iturralde J, Provenzal O, Damiani H, Milman A, Bragagnolo A, Yunes J, Campodonico A. Gangrena de Fournier. Nuestra experiencia en los últimos 10 años. Revisión de la literatura. Arch Esp de Urol, 1999; 52 (7): 721-727. [ Links ]
22. Johnin K, Nakatoh M, Kadowaki T, Kushima M, Koizumi S and Okada Y. Fournier's Gangrene caused by Candida species as the primary organism. Urology, 2000; 56: 153xiii-153xv. [ Links ]
23. Mindrup SR, Kealey GP, Fallon B. Hyperbaric oxygen for the treatment of Fournier's gangrene. The J. Urol, 2005; 173: 1975-1977. [ Links ]
24. Shupak A, Shoshani O, Goldenberg I, Barzilai A, Moskuna R, Bursztein S. Necrotizing Fascitis: and indication of hyperbaric oxygenation therapy?. Surgery, 1995; 118: 873-876. [ Links ]
25. Laucks S S II. Fournier's gangrene. Surg. Clin. North Am, 1994; 74, 7339. [ Links ]











 texto en
texto en 


