Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Archivos Españoles de Urología (Ed. impresa)
versión impresa ISSN 0004-0614
Arch. Esp. Urol. vol.62 no.7 sep. 2009
Persistence of an infected urachus presenting as acute abdominal pain. Case report
Persistencia de uraco infectado como causa de abdomen agudo. A propósito de un caso
Diana Martín Hernandez1, Pablo Prieto Matos2, Juan Carlos Diez Hernández1, Jorge Liras Muñoz3 and Luis de Celis Villasana3
Radiodiagnosis Department1. Pediatric Department2. Pediatric Surgery Department3. Salamanca Universitary Hospital. Salamanca. Spain.
SUMMARY
Objectives: We report a case of urachal remnant disease and review the literature.
Methods/Results: We present the case of an urachal cyst in a 13-year-old patient who was admitted to the emergency department with acute abdominal pain. Differential diagnosis of his symptoms was made with other diseases such as appendicitis and inflammatory bowel disease.
Conclusions: Urachal remnant diseases are rare and they usually present during the neonatal period with fever and wet navel, lower abdominal pain around the middle line, palpable mass and urination symptoms with or without urinary infections. The presentation as acute abdominal pain in an older child is less common, and its differential diagnosis must be performed with other abdominal or pelvic acute diseases. The most appropriate imaging technique is an ultrasound exam.
Key words: Urachal remnant. Infection. Acute abdominal pain. Congenital anomalies.
RESUMEN
Objetivos: Revisar a propósito de un caso la literatura a cerca de las enfermedades del remanente uracal.
Método/Resultado: Presentamos el caso de un quiste de uraco infectado en un paciente de 13 años de edad que se acudió a urgencias con un dolor abdominal agudo, lo que obligó a hacer el diagnóstico diferencial de otras patologías como la apendicitis y la enfermedad inflamatoria intestinal.
Conclusiones: Las enfermedades del remanente uracal son poco frecuentes y suelen manifestarse en el periodo neonatal con fiebre y ombligo húmedo, dolor abdominal inferior alrededor de la línea media, masa palpable y clínica miccional con/sin infección urinaria. La presentación como abdomen agudo en un niño más mayor es infrecuente y obliga a hacer el diagnóstico diferencial con otras patologías abdominales o pélvicas. Las técnicas de imagen más adecuadas son la ecografía y el TAC.
Palabras clave: Remanente uracal. Infección. Abdomen agudo. Anomalías congénitas.
Introduction
The urachus or median umbilical ligament is a tubular structure located in the middle line. It spreads from the antero-superior part of the bladder to the navel. It is the embryological remnant of the cloaca and the allantois. Urachal remnant diseases are rare, and they present unspecific symptoms such as abdominal pain or urinary problems. Therefore, the differential diagnosis before surgery is not easy.
Case report
The patient is a 13-year-old boy with no relevant record, who is admitted as an emergency with severe abdominal pain in the suprapubic and infraumbilical regions of 12 hours of evolution. The patient reports urinary problems of 4 days of evolution, together with pain in that area which increased after the bladder emptying. He also presented a wet navel with no previous record.
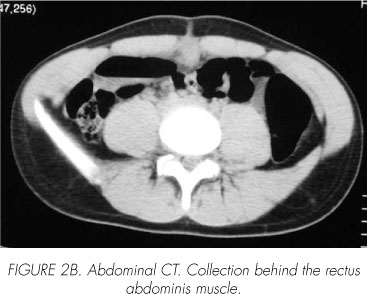
The patient shows intense pain on abdominal palpation in the suprapubic and abdominal regions, an increase of the acute-phase reactants and leukocytosis. An abdominal ultrasound and CT are performed, diagnosing an infected urachal remnant (Figure 1), together with a collection immediately below the navel (Figure 2A and 2B). The pH measurement of the umbilical liquid, which was between 5 and 6, confirmed that the collection was, in fact, urine.


A treatment with antibiotics and analgesics was started, and the purulent material was drained through an umbilical fistula. Two months later, the urachus was removed with laparoscopic surgery, and an urachal remnant of 3-4 cm was resected. The postoperative period did not present any complication.
Discussion
The urachus is the embryological remnant of the cloaca and the allantois. It spreads from the antero-superior part of the bladder to the navel. Between the fourth and the fifth months of gestational age, the bladder drops towards the pelvis, and the urachus prolongs and narrows until it turns into an epithelialized fibro-muscular cord. It extends between the transversalis fascia and the parietal peritoneum. The size of the urachus can range between 3-1 0 cm in length and 8-1 0 mm in diameter.
Urachal anomalies can be classified into congenital and acquired. Congenital anomalies consist of a defect in the obliteration of the urachus. There are four types of urachal congenital anomalies: persistent urachus, urachal cyst, vesicourachal diverticulum, and urachal sinus. Acquired anomalies are infections and malignant degeneration.
Persistent urachus is a full defect in the obliteration. It is the most common urachal congenital anomaly (50% of the cases). It is usually diagnosed during the neonatal period, because the urine can flow back from the bladder to the navel through the persistent urachus. In one third of the cases, this condition is associated with posterior urethral valves or urethral atresia. In other patients, the urachus can be asymptomatic.
In the urachal sinus, the apical segment of the urachus remains permeable, thus creating a communication with the navel. It represents 15% of all the congenital anomalies.
The vesicourachal diverticulum is less common (3-5% of the cases). It consists of the persistence of the distal part of the urachus, which creates a permeable communication with the bladder dome.
Finally, the urachal cyst represents 30% of the congenital anomalies of the urachus, and it consists of a persistence of the midline of the urachus, while the umbilical and vesical ends remain closed. It usually appears in the lower third of the urachal tract. They are generally small, although their size can vary considerably.
Any of these congenital anomalies can become overinfected. The infection route can be lymphatic, hematogenous or vesical. The clinical symptoms of an urachal infection are fever, abdominal pain in the lower region or around the middle line, urinary problems with or without infection and, sometimes, a suprapubic palpable mass.
The presentation as acute abdominal pain with abdominal guarding, an increase of the acute-phase reactants and leukocytosis in an older child is less common. In these cases, the differential diagnosis has to be performed with lots of inflammatory pathologies, mainly acute appendicitis, but also cystitis, inflammatory bowel disease, strangulated umbilical hernia, pelvic or intraabdominal abscess and Meckel's diverticulum.
Ultrasound and CT can be helpful in the differential diagnosis, and they can also detect other congenital anomalies that might be associated with these disorders.
The treatment approach is surgical, and it consists of a complete excision of the urachal remnant. If the remnant has become infected, an antibiotic treatment must be applied, and it can be associated to the draining of the cyst or the purulent collections, so that the lesion can be resected afterwards. The surgical treatment prevents the possibility of a malignant degeneration towards adenocarcinoma, sarcoma, or transitional cell carcinoma.
Conclusions
Urachal remnant diseases usually present themselves during the neonatal period with a wet navel. If they become overinfected, they cause fever, abdominal pain in the lower region or around the medial line, urinary problems with or without infection and, sometimes, a suprapubic palpable mass. Its presentation as acute abdominal pain in an older child is less common. In these cases, the differential diagnosis has to be performed with acute appendicitis and other inflammatory disorders.
 Correspondence:
Correspondence:
Diana Martin Hernandez
Calle Conde Vallellano,12, Bajo
37008 Salamanca. (Spain)
dianamh@gmail.com
Accepted for publication: January 29th, 2009.
References and recommended readings (*of special interest, **of outstanding interest)
**1. DiSantis DJ, Siegel MJ, Katz ME. Simplifed aproach to umbilical remnant abnormalities. Radigraphics. 1991; 11:59-66. [ Links ]
*2. Yu JS, Kim KW, Lee HJ, Lee YJ, Yoon CS, Kim MJ. Urachal remnant diseases: spectrum of CT and US findings. RadioGraphics 2001; 21:451-461. [ Links ]
3. Boothroyd AE, Cudmore RE. Ultrasound of the discharging umbilicus. Pediatr Radiol 1996;26:362-364. [ Links ]
4. Cilento BG Jr, Bauer SB, Retrik AB, Peters CA, Atala A. Urachal anomalies: difining the best diagnostic modality. Urology 1998; 52:120-122. [ Links ]
*5. Khati NJ, Enquist EG, Javitt MC. Imaging of the umbilicus and periumbilical region. RadioGraphics 1998:413-431. [ Links ]
*6. Gimeno Argente V, Domínguez Hinarejos C, Serrano Durbá A, Estornell Moragues F, Martinez Verduch M, Garcia Ibarra F. Quiste de uraco infectado en edad infantil. Actas Urol Esp 2006:30(10):1034-1037. [ Links ]
7. Allen JW, Song J, Velcek FT. Acute presentation of infected urachal cyst: case report and review of diagnosis and therapeutic interventions. Pediatr Emerg Care 2004;20(2)108-111. [ Links ]
8. Chauvin N, Domachowske JV. Infected urachal cyst presenting as fever of unkown origing. Clin Pediatr. 2005;44(1):85-87. [ Links ]
9. Donate Moreno MJ, Gimenez Bachs JM, Salinas Sánchez AS, Lorenzo Romero JG, Segura Martín M, Hernández Millán I et al. Patología del uraco: revision del conjunto y presentación de tres casos. Actas Urol Esp. 2005;29(3):332-336. [ Links ]
10. Luo CC, Huang CS, Wu WC, Chu SM, Chao HC. An unusual presentation of an infected urachal cyst: case report and review of the literatura. Eur J Pediatr 2004;163(4-5):268-269. [ Links ]
11. Mc Collum MO, MacNeily AE, Blair GK. Surgical implications of urachal remnants: presentation and management. J Pediatr Surg. 2003;38(5):798-803. [ Links ]
*12. Gómez Díaz ME, Tornero Ruiz JI, Caffaratti Sfulcini J, Barat Barredo JM. Quistes uracales en la infancia Arch Esp Urol. 2003;56(3):300-302. [ Links ]
**13. Gómez Parada J, Puyol Pallas JM. Quiste infectado de uraco: a propósito de un nuevo caso. Arch Esp Urol. 2001;54(7):722-725. [ Links ]
**14. Burgues Gasion JP, Domínguez Hinarejos C, Serrano Durbá A, Estornell Moragues F, Martinez Verduch M, García Ibarra F. Divertículos de uraco. Diagnóstico y tratamiento. Arch Esp Urol. 2002;55(3):285-291. [ Links ]











 texto en
texto en 


