Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Nutrición Hospitalaria
versión On-line ISSN 1699-5198versión impresa ISSN 0212-1611
Nutr. Hosp. vol.22 no.5 Madrid sep./oct. 2007
Insufficient voluntary intake of nutrients and energy in hospitalized patients
Ingestión voluntariamente insuficiente de nutrientes y energía en pacientes hospitalizados
M. M. Tavares*,**, L. Matos*, # and T. F. Amaral*
*Faculdade de Ciências da Nutrição e Alimentação. Universidade do Porto. Portugal.
**Hospital Pedro Hispano - SA. Unidade de Saúde Local de Matosinhos. Portugal.
#Hospital Geral de Santo António - SA. Unidade de Nutrição. Porto. Portugal.
ABSTRACT
Aim: The aim of our study was to evaluate the inadequacy of voluntary energy and nutrient intake on the first day of hospital admission.
Patients and methods: A cross-sectional study was carried out in two terciary care hospitals, with a probabilistic sample of 50% of in-patients. Dietary intake was evaluated by a 24-hour dietary recall, and undernutrition was screened through the Nutritional Risk Screening 2002 tool. The overall frequency of inadequate energy and nutrient intake was estimated using Dietary Reference Intakes.
Results: Energy and nutrient intakes from 258 patients showed very low values for both men and women. No significant differences were found for energy and nutrient intakes across age groups (< 65 years and ≥ 65 years). When the proportion of study subjects with inadequate nutrient intakes was analysed, a high degree of inadequacy was found. The degree of inadequacy was higher for fibre, niacin, folate, vitamin B12, magnesium and zinc. No significant differences were found for energy and nutrients studied and for intakes below 1/3 of dietary recommendations from nutritionally-at-risk (n = 89) and well nourished (n = 169) patients.
Conclusion: Voluntary nutrient and energy intakes in the first 24 hour of hospital admission are highly inadequate. No differences were found between undernourished and well-nourished patients or patients < 65 years and ≥ 65 years.
Key words: Disease-related malnutrition. Inadequate nutrient intake. Estimated average requirements. Hospital food. Dietary reference intakes.
RESUMEN
Objetivo: El propósito de nuestro estudio fue evaluar la inadecuación de la ingestión voluntaria de energía y nutrientes durante el primer día de ingreso hospitalario.
Pacientes y métodos: Se realizó un estudio transversal en dos centros hospitalarios de atención terciaria con una muestra probabilística del 50% de pacientes ingresados. Se evaluó la ingestión alimenticia mediante un diario de 24 horas, y se hizo un cribado de desnutrición mediante la herramienta Nutritional Risk Screening 2002. Se estimó la falta de adecuación del consumo de energía y nutrientes mediante el Dietary Reference Intakes.
Resultados: El consumo de energía y nutrientes en 258 pacientes mostró niveles muy bajos tanto en hombre como en mujeres. No se hallaron diferencias significativas en el consumo de energía y nutrientes entre los distintos grupos de edad (< 65 años y ≥ 65 años). Cuando se analizó la proporción de sujetos del estudio con consumo inadecuado de nutrientes, se halló una alta proporción de inadecuación. El grado de inadecuación fue mayor para la fibra, niacina, folato, vitamina B12, magnesio y zinc. No se hallaron diferencias significativas en la energía y los nutrientes estudiados y los consumos inferiores a 1/3 de las recomendaciones dietéticas entre los pacientes con riesgo nutricional (n = 89) y aquellos bien nutridos (n = 169).
Conclusión: La ingestión voluntaria de nutrientes y energía durante las primeras 24 horas del ingreso hospitalario es muy inadecuada. No se hallaron diferencias entre los pacientes bien y mal nutridos, ni entre los mayores o menores de 65 años.
Palabras clave: Malnutrición relacionada con la enfermedad. Ingestión inadecuada de nutrientes. Requerimientos medios estimados. Comida hospitalaria. Ingestiones de referencia.
Introduction
There has been a wide incidence of Disease-related Malnutrition (DRM) amongst hospitalized patients, with figures ranging between 10 and 60%.1 Studies have demonstrated that nutritional status deteriorates after hospital admission if nutritional support is absent.2, 3 Although the effect of underlying disease and inadequate food provision could be important contributors, reduced food intake is regarded as one of the most important components of a causal pathway leading to DRM and is the most important avoidable risk factor. Poor food intake results not only in an inadequate energy intake, but also in low intake of essential nutrients, which increases the risk of undernutrition. The measurement of daily energy and the full spectrum of nutrient intake at the beginning of hospital stay is an important part of the patient evaluation, because it helps to predict changes in nutritional status during hospitalization and provides nutritional support teams benchmarks to optimize subsequent nutritional care.
Although most hospital diets provide sufficient energy and nutrients, previous studies examining food consumption in hospitalized patients showed mean daily energy and protein intakes in general patients failing to meet the Estimated Average Requirements (EAR).4, 5 The assessment of energy and protein intakes in hospitalized elderly patients and specific disease groups showed similar results.6 However, only a small number of studies analysed dietary components other than energy and protein. Many of these studies were limited to evaluating the adequacy of nutrient intakes. The nutritional analysis that was performed, with a handful of nutrients, showed that hospitalized patients had inadequate nutrient intake.6
The amount of food consumed by each patient and food wastage is not usually monitored or of concern to hospital staff.3, 7 Patients with cognitive impairment or in poor health as well as those receiving artificial nutritional support are more likely to have their amount of feeding carefully monitored as opposed to patients on a hospital diet who do not need feeding assistance.
The aim of our study was to evaluate voluntary energy and nutrient intake inadequacy on the first day of admission to hospital.
Materials and methods
Study Design
This study was carried out as a cross-sectional study in two terciary care hospitals in Porto, Portugal: Hospital Geral Santo António, S. A., a teaching unit and Hospital Pedro Hispano S. A., a district unit. A probabilistic sample of 50% of in-patients was obtained by selecting the first of every two consecutively admitted patients, between 24 and 48 h from admission to each hospital. Patients were considered eligible if they were 18 or over and with a Length of Hospital Stay (LOS) longer than 24 hours. Exclusion criteria were nothing per os (NPO) prescription cognitive impairment, artificial nutritional support and pregnancy. Cognitive impairment was defined as a Folstein's mini-mental state examination test result < 24 points or < 20 in illiterate patients.8
Dietary intake was evaluated by a single 24-hour dietary recall performed in the first 48 hours of admission. Patients were asked, through a systematic repetition of open-ended questions, to recall and describe type and portion size of all food and drink consumed in the 24 hours prior to the interview.9 Food portion size was ascertained using the catering company's portion size book, patients described their food consumption as part of portion served (nothing; ¼;½;¾; all).
Functional status was evaluated using Katz index of the ability to be independent in the Activities of Daily Living (ADL's).10 Patients were scored depending on their performance in 6 categories of activities, from 0 if completely dependent in bathing, dressing, toileting, transfer, continence and feeding, to 6 if totally independent in all categories. Independence was defined as being able to perform the activity without the assistance of another person.
Weight was measured by a mechanical calibrated scale until 0.1 kg.11 Height was measured with individuals standing, until 0.1 cm. When patients could not stand, measurements were made with them lying on a bed.11 The Nutritional Risk Screening 2002 (NRS-2002) tool was used to screen undernutrition and to assess the risk of developing undernutrition in the hospital setting.12 NRS-2002 classifies patients' nutritional status based on Body Mass Index (BMI), percentage of recent weight loss and recent change in food intake and severity of disease in four categories: absent, mild, moderate and severe, which corresponds to a score between 0 and 3, respectively. The score obtained in each component is then added together and for patients older than 70 years or older an extra point is added to the total score. Any patient with a total score ≥ 3 is considered nutritionally-at-risk. This tool has a high predictive validity, a low inter-observer variation (k = 0.67), a high practicability12 and is recommended by the European Society of Clinical Nutrition & Metabolism (ESPEN) for hospital nutritional screening.13.
Data was collected using a structured questionnaire to record the following: social-demographic and clinical information, result of screening tool for nutritional risk, anthropometric data and dietary intake. Two nutritionists (one in each hospital) who were not involved in the patients' care carried out all the interviews and assessments. In order to improve between and intra-interviewer agreement, they trained together on the 24-hour recall and the anthropometric measurements procedures.
Despite the observational nature of the present research, the study was designed in accordance with the Declaration of Helsinki14 and was approved by Hospital Pedro Hispano S.A's Ethics Committee. Informed consent was obtained from all subjects and the protocol was approved by the institutional review board of the two hospitals.
Data analysis
Food intake was converted into nutrients for each patient using Microdiet® software version 1.1, 2000.15 This database was completed with traditional Portuguese food composition information.16-18
Results are presented for the entire sample, by sex and age. Mean values of energy and nutrient intake for the entire sample distribution and standard deviations were determined.
The overall frequency of inadequate energy and nutrient intake was estimated using Dietary Reference Intakes (DRI). The Estimated Energy Requirements (EER) from the Food and Nutrition Board (FNB) formulas were used for energy.19 The EAR, the nutrient quantity estimated to meet the requirement of half of all healthy people within a specific life stage and gender group, was used to evaluate the inadequacy of nutrient intake for vitamins C, B1, B2, niacin, B6, folate, B12, iron, magnesium and zinc. The minimal lipid recommendation was considered as 15% of EER for women and 20% of EER for men.20 Because the EAR's did not include a recommendation for fibre, Adequate Intakes (AI's), a category of DRI19 were used. Minimum protein needs were estimated using 0.8 g protein by each kg of body weight per day.21
Frequencies, mean values and standard deviations were calculated to describe the sample's most important characteristics. Mann-Whitney U and qui-square tests were used as appropriate to compare sample's characteristics between age and sex groups and nutrient intake between age, sex and nutritional risk groups. Statistical significance was set at p < 0.05. Data were analysed with SPSS statistical software version 13.0, 2004.22
Results
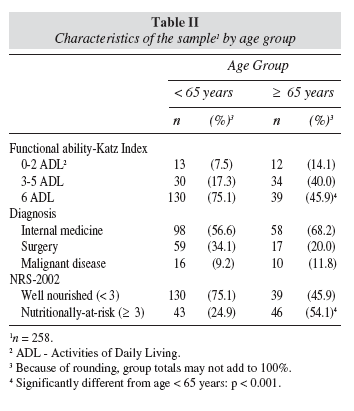
Compliance was excellent, with a response rate of 100%. The characteristics of the 258 patients are shown in table I, where sex-specific distributions of age, marital status, education level, smoking habits and BMI are described. Significant sex differences (p < 0.05) were observed for marital status, with a higher proportion of widows among women who also had lower levels of education and tended to be non-smokers. The distribution of the sample's functional ability, diagnosis and nutritional risk by age groups (< 65 years and ≥ 65 years) is presented in table II. As expected, older patients have lower functional ability, with a proportion of undernourished patients that roughly doubles that of the < 65 years (p < 0.001).
Energy and nutrient intakes stratified by sex and age group are described in table III, showing very low values for both men and women. No significant differences were found for energy and nutrient intakes across age groups (< 65 years and ≥ 65 years). When the group with inadequate nutrient intakes was analysed (table IV), a high degree of inadequacy was found, being highest for fibre, niacin, folate, vitamin B12, magnesium and zinc.
No significant differences were found for energy and nutrients in regards to proportions of high level of inadequacy, and intakes below 1/3 of dietary recommendations from nutritionally-at-risk (n = 89) and well nourished (n = 169) patients (table V).
Discussion
The inadequacy of voluntary energy and nutrient intakes at hospital admission was evaluated in a teaching and district hospital's probabilistic samples, representing a wide spectrum of pathologies and giving the opportunity to identify high risk groups for lower intakes. Voluntary nutritional intakes were found to be highly inadequate in the first 24-hours of hospital admission, as previously described3, 5, 23, 24 and no differences were found between studied age groups and nutritional status.
The institutional menus were developed to provide adequate micronutrients, enabling patients to achieve nutritional needs when the full diet of 2,400 kcal is consumed. Despite sufficient food provision, it is described that most of the patients did not achieve this goal, showing lower intakes of essential nutrients.25 This has lead to the present investigation, which can be regarded as an insight into the enormous problem of insufficient food intake by hospital inpatients. The 24-hour recall only provides estimates about the preceding day, which may not be representative of patient's usual intake, due to day-to-day variation, so these results could not be generalized to the entire hospitalization.
There were several reasons that led to the decision to opt for the 24-hour recall in evaluating diet intake. The high level of illiteracy in the sample made the use of food diaries impossible. In addition, the recall did not burden the patient with the additional task of a time-consuming interview -a requirement of food frequency questionnaires or diet history. The main disadvantage of the 24-hour recall is its heavy reliance on memory, and it can exhibit the "flat-slope" syndrome, i.e., subjects with low intakes tend to report higher than usual intakes, and those with high intakes tend to report lower than usual intakes,26 leading to misleading results. Nevertheless, all efforts, regarding previous training of interviewers and interview questions, were made in order to minimise recall bias. Furthermore, the present investigation was confined to patients with cognitive ability, as cognitive impaired patients were excluded, because they were more likely to have feeding assistance or dietary supplements.
Whilst interpreting the estimated proportions of energy and nutrient inadequacy, it is important to highlight the fact that DRIs are set to cover the requirements of 97.5% of the population.19 Consequently, intakes below this level do not necessarily indicate that patients are not meeting their nutritional requirements. Otherwise, these guidelines are set to meet nutritional needs of healthy people, which is not the case with hospitalized patients. Some of these patients could have increased metabolic requirements resulting from the disease that also widens the gap between requirements and intake and if so, the inadequacy of their intake should be higher than the estimated.
One implication of these findings is that all inpatients were likely to require energy, protein, full-spectrum vitamin and mineral supplements. As there are no substitutes for the adequate provision of "normal" food23 the second implication is that a number of strategies need to be urgently implemented, given the importance of nutrition screening and timely nutritional interventions to treat and prevent further deteriorations in nutrition status.
Sponsorship
Fundação Ilídio Pinho and Reitoria of the University of Porto - Programa Investigação Científica na Pré-graduação.
Acknowledgements
To Dr. Fernando Sollari Allegro (MD), Director of Hospital Geral de Santo António (SA) Porto, to Dr. Hermínio Loureiro (MD), Former Director of Hospital Pedro Hispano (ULS Matosinhos, SA) and to all other ward directors for facilitating the data collection. To our colleagues, Drª Dulce Senra e Dr. Fernando Piche, for the support given during the data collection.
References
1. Stratton RJ, Green CJ, Elia M. Prevalence of Disease-related Malnutrition. In: Disease-related Malnutrition: An Evidencebased Approach to Treatment. CABI Publishing. Wallingford, 2003: 35-92. [ Links ]
2. McWhirter JP, Pennington CR. Incidence and recognition of malnutrition in hospital. BMJ 1994; 308:945-8. [ Links ]
3. Beck AM, Balknas UN, Camilo ME Furst P, Gentile MG, Hasunen K et al. Practices in relation to nutritional care and support -Report from the Council of Europe. Clin Nutr 2002; 21:351-4. [ Links ]
4. Sandstrom B, Alhaug J, Einarsdottir K, Simpura EM, Isaksson B. Nutritional status, energy and protein intake in general medical patients in three Nordic hospitals. Hum Nutr Appl Nutr 1985; 39(2):87-94. [ Links ]
5. Barton AD, Beigg CL, MacDonald IA, Allison SP. High food wastage and low nutritional intakes in hospital patients. Clin Nutr 2000; 19(6):445-9. [ Links ]
6. Stratton RJ, Green CJ, Elia ME. Causes of Disease-related Malnutrition. In Disease Related Malnutrition: An Evidence-based Approach to Treatment. CABI Publishing. Wallingford, 2003: 93-112. [ Links ]
7. Allison SP. Malnutrition, disease, and outcome. Nutrition 2000; 18:590-3. [ Links ]
8. McDowell I, Newell C. The mini-mental state examination. In: Measuring Health. A Guide To Rating Scales and Questionnaires. Oxford University Press, New York 1996: 314-23. [ Links ]
9. Wiehl DG. Diets of a group of aircraft workers in Southern California. Millbank Memorial Fund Quarterly 1942; 20:329-66. [ Links ]
10. Katz S, Ford AB, Moskowitz RW, Jackson BA, Jaffe MW. Studies of illness in the aged. The Index of ADL: a standardized measure of biological and psychosocial Function. JAMA 1963; 185:914-9. [ Links ]
11. Lee RD, Nieman DC. Nutritional assessment of hospitalized patients. In: Nutritional Assessment. Mosby-Year Book Inc. St Louis (MO), 1996: 289-332. [ Links ]
12. Kondrup J, Rasmussen HH, Hamberg O. Nutritional Risk Screening (NRS-2002): a new method based on an analysis of controlled clinical trials. Clin Nutr 2003; 22:321-36. [ Links ]
13. Kondrup J, Allison SP, Elia M, Vellas B, Plauth M, Educational and Clinical Practice Committee, European Society of Parenteral and Enteral Nutrition. ESPEN Guidelines for Nutrition Screening 2002. Clin Nutr 2003; 22:415-21. [ Links ]
14. World Medical Association Declaration of Helsinki. Tokyo, 2004. http://www.wma.net/e/policy/b3.htm [ Links ]
15. Microdiet Plus for Windows. Copyright Downlee Limited. Version 1.1, 2000. [ Links ]
16. Ferreira FAG, Graça MES. Tabela da Composição dos Alimentos Portugueses. Instituto Nacional de Saúde Dr. Ricardo Jorge. Lisboa, 1985. [ Links ]
17. Mano ML, Meister MC, Fontes MR. Composição de sobremesas doces. Alguns produtos servidos em "snack bares". Rev Port Nutr 1989; 1:19-24. [ Links ]
18. Mano ML, Meister MC, Fontes MR, Lobo P. Composição de sobremesas doces. Rev Port Nutr 1992; 4:16-24. [ Links ]
19. Dietary Reference Intakes (DRIs): Recommended Intakes for Individuals, Macronutrients. Food and Nutrition Board, Institute of Medicine, National Academies 2002. [ Links ]
20. Torheim LE, Ouattara F, Diarra MM et al. Nutrient adequacy and dietary diversity in rural Mali: association and determinants. Eur J Clin Nutr 2004; 58:594-604. [ Links ]
21. Dupertuis YM, Kossovsky MP, Kyle UG et al. Food intake in 1,707 hospitalised patients: a prospective comprehensive hospital survey. Clin Nutr 2003; 22:115-23. [ Links ]
22. Statistical Package for Social Sciences for Windows. Copyright SPSS Inc., 1989-2004. Version 12.0, 2004. [ Links ]
23. Allison SP. Hospital food as treatment. Clin Nutr 2003; 22: 113-4. [ Links ]
24. Jeejeebhoy KN. Hospital malnutrition: is disease or lack of food? Clin Nutr 2003; 22:219-20. [ Links ]
25. Almdal T, Viggers L, Beck AM, Jensen K. Food production and wastage in relation to nutritional intake in a general district hospital -wastage is not reduced by training the staff. Clin Nutr 2003; 22(1):47-51. [ Links ]
26. Nelson M, Bingham SA. Assessment of food consumption and nutrient intake. In: Design Concepts in Nutritional Epidemiology. Oxford University Press. New York, 1997: 123-69. [ Links ]
![]() Correspondence:
Correspondence:
Dra. Teresa Amaral.
Faculdade de Ciências da Nutrição e Alimentação da
Universidade do Porto.
Rua Dr. Roberto Frias, 4200-465 Porto, Portugal.
E-mail: amaral.tf@gmail.com
Recibido: 26-VI-2006.
Aceptado: 30-XI-2006.