Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Nutrición Hospitalaria
versión On-line ISSN 1699-5198versión impresa ISSN 0212-1611
Nutr. Hosp. vol.24 no.4 Madrid jul./ago. 2009
Dietary habits associated with obesity among adolescents in Dubai, United Arab Emirates
Hábitos dietéticos asociados con la obesidad en los adolescentes de Dubai, Emiratos Árabes Unidos
A. A. bin Zaal1, A. O. Musaiger2 and R. D'Souza2
1Department of Preventive Medicine. Ministry of Health. Dubai. UAE.
2Bahrain Centre for Studies and Research. Kingdom of Bahrain. United Arab Emirates.
ABSTRACT
Aim: to study the association between the dietary habits and behavioural factors with the increased risk of obesity amongst adolescents in Dubai, United Arab Emirates (UAE).
Method: A cross-sectional study was carried out among 661 adolescents (324 boys and 337 girls) aged 12 to 17 years selected by means of a multistage stratified random sampling technique.
Results: The highest percentage of obesity was observed at 14 years of age in boys (30.5%) and at 13 years of age in girls (35.4%). There was a significant association between the frequency of eating breakfast (P =0.048), snacking between breakfast and lunch (P = 0.044), and obesity in girls but not in boys. A high risk of obesity was associated with eating breakfast at school in both boys (OR = 3.0; CI 1.1-8.3) and girls (OR = 3.4; CI 1.6-7.4). Fast foods showed a significant association with obesity in girls (P = 0.007), but not in boys (P = 0.745). The risk of obesity was higher in boys who ate fast foods at home (OR = 1.3; CI 0.5-3.2) but less in girls (OR = 0.2; CI 0.1-1.0).
Conclusion: Intervention programs focused on promoting changes in lifestyles, food habits and increasing physical activity need to be implemented at the earliest.
Key words: Adolescents. Diet. Lifestyle. Dubai.
RESUMEN
Objetivo: estudiar la asociación entre los hábitos dietéticos y los factores del comportamiento con el riesgo aumentado de obesidad en los adolescentes de Dubai, Emiratos Árabes Unidos (EAU.)
Método: Se realizó un estudio transversal en 661 adolescentes (324 chicos y 337 chicas) con edades entre 12 y 17 años seleccionados mediante una técnica de muestreo aleatoria estratificada de múltiples etapas.
Resultados: el mayor porcentaje de obesidad se observó en los chicos de 14 años de edad (30,5%) y en las chicas de 13 años (35,4%.) Hubo una asociación significativa entre la frecuencia de desayunar (P = 0,048), merendar entre el desayuno y la comida (P = 0,044) y la obesidad en las chicas pero no en los chicos. El riesgo elevado de obesidad se asoció con desayunar en el colegio tanto en los niños (OR = 3,0; IC 1,1-8,3) como en las niñas (OR = 3,4; IC 1,6-7,4.) La comida rápida mostró una asociación significativa con la obesidad en las niñas (P = 0,007), pero no en los niños (P = 0,745.) El riesgo de obesidad fue mayor en los chicos que comían comida rápida en casa (OR = 1,3; IC 0,5-3,2) pero menos en las niñas (OR = 0,2; IC 0,1-1,0.)
Conclusión: Se necesita implantar lo antes posible programas de intervención centrados en promocionar los cambios en el estilo de vida, los hábitos de alimentación y aumentar la actividad física.
Palabras clave: Adolescentes. Dieta. Estilo de vida. Dubai.
Introduction
A disturbing increase in the prevalence of overweight and obesity among children has taken place over the past twenty years in both the developingand developed countries.1,2 Specifically in the context of the Arabian Gulf countries and the United Arab Emirates in particular, it has been widely reported that obesity has become a major health problem in the past three decades as a result of the economic boom.3 Recent research in the United Arab Emirates (UAE) suggests that the prevalence of childhood obesity is increasing dramatically, already surpassing the high levels of obesity found amongst children and adolescents in the USA and Europe.4 In a similar study Al-haddad et al.,5reported that the frequency of obesity is two to three times greater than the recently published international standards in the UAE.
The aetiology of overweight and obesity is clearly multifactorial, but ultimately it is determined by the long-term balance between energy intake and expenditure. 6 Hence, one of the reasons for fuelling a worldwide increase in obesity in children and adolescents is the change in their food consumption and exercise patterns. 7 The recent changes in the nutrition environment, including greater reliance on convenience foods and fast foods, a lack of access to fruit and vegetables, and expanding portion sizes, are also widely believed to contribute to the epidemic of childhood obesity.8 In the Arabian Gulf, the traditional diet, characterized as a high-fibre content and low in fat, has changed to a more westernized diet with a high content of fat, free sugars, sodium and cholesterol.9 In addition, with the availability of cars, life has become more sedentary, and the pattern of exercise has diminished steeply.3 In particular, children today seem less likely to walk to school and travel more in cars than they did during the early 1970s, perhaps because of changes in the built environment.10 Additionally, children spend more time viewing television and using computers and their greater exposure to TV and videos may influence children's consumption of unhealthy foods.11 Studies among male university students in the UAE indicate that that social and lifestyle factors are important factors in the occurrence of obesity, and the risk of obesity was high among those who watched television for more than four hours a day (RR=1.31), were not engaged in sport (RR = 1.77) and had a car (RR = 1.23).12 Although, the rise of overweight and obesity in the UAE has been documented by researchers,13-15 studies regarding lifestyle factors associated with obesity among UAE adolescents are at most scanty. Hence, this study is an attempt to evaluate the association between some dietary and behavioural factors which lead to an increased risk of obesity in Dubai adolescents.
Methods
Subjects: The study population included U.A.E nationals, male and female students, aged 12 to 17 years. A representative sample of these adolescents (661 students, 324 boys and 337 girls) was selected from schools using a multistage stratified random sampling technique and stratified by sex and school type (preparatory and secondary). The sample was selected from between different educational grades and geographical areas of Dubai (within the preparatory and secondary school levels) to ensure that the appropriate age groups and different strata of the target population were represented. Only the national adolescents were included in the study. Ages and dates of birth were verified against school records, which in turn were based on the birth certificates. The study was approved by the Research Ethics Committee of the Ministry of Health, Dubai Medical District. All adolescents, parents and teachers were clearly informed about the purpose and content of the study and written consent was obtained from the parents.
Anthropometric measurements: Weight and height were measured using the standard procedure as described earlier.15 Weight was measured to the nearest 0.1 kg using an electronic portable scale (Seca). To ensure accuracy in measurement the scale was checked for a zero reading before each weighing and calibrated with a known weight on the morning of each data collection. Furthermore, both weight and height measurements were carried out by one person to avoid interpersonal error. The height of the student height was measured, in the standing position, to the nearest 0.1 cm using a portable stadiometer which was attached to the "Seca" weighing scale. The student was asked to stand without shoes and socks, back against the scale, heels together and head in the upright position. The movable headboard was lowered until it firmly touched the upper part of the subject's head and a direct reading of height was obtained.
The body mass index (BMI) (weight in kilograms divided by height in meters squared) was computed to determine overweight and obesity among adolescents using the cut-off values as recommended by the World Health Organization (WHO, 1995) as follows:
Underweight: < 5th percentile of BMI for age
Normal weight: 5th to < 85th percentile of BMI for age
Overweight: 85th to < 95th percentile of BMI for age
Obese : ≥ 95th percentile of BMI for age.
For the purpose of this paper the adolescents were divided into two categories: non-obese, which included underweight and normal weight adolescents (< 85th percentile of BMI for age), and obese: which included overweight and obese adolescents (> = 85th of BMI for age).
Dietary and behavioural habits assessment: Many of the questions used in the family study questionnaire were adapted from the Family Eating and Activity Habits Questionnaire, developed and validated by Golan and Weizman.16 The content validity of this questionnaire was determined by a group of 5 experts in the field of nutrition, epidemiology, and public health for clarity and appropriateness. The questionnaire was pre-tested twice, during the development stage and prior to data collection and was translated into Arabic and back into English. A language expert then checked the translation to ensure that the meaning of the questions was essentially the same in both the Arabic and English versions.
A preliminary version of the questionnaire was piloted prior to actual data collection. Questions that resulted in ambiguous answers on pilot testing were subsequently reworded to enhance clarity. A nutritionist then administered the final version of the questionnaire to both male and female adolescents to obtain information on the socio-demographic characteristics (age and sex) and dietary/behavioural habits (eating breakfast daily, snacking habits, eating meals with the family, eating meals while watching the television etc.).
A statistical analysis was performed using the SPSS (version 15) software package. Chi- square statistics were used to determine the presence of an association between the variables. Odds ratio (OR) and confidence intervals (CI) were used to quantify the strength of association between obesity risk and each of the other variables.
Results
The prevalence of overweight and obesity among Dubai male and female adolescents as assessed by the WHO (1995) reference data are seen in table I. The proportion of overweight (18.5%) and obese males (22.2%) was higher than that of overweight (13.1%) and obese (20.5%) females. Obesity was highest among boys at 12 years of age (32.4%) followed by 14 years (30.5%). A decline in obesity with age was observed, the lowest proportion of obese boys was at 17 years of age (12.5%). Overweight in boys was highest at 16 years of age (25.5%) though a decline was seen the following year (16.7%). In girls, the highest percentage of obesity was at 13 and 14 years of age (35.4% and 25.4% respectively). Overweight was the highest at 17 years of age (19.0%) and seemed to increase from the previous year (14.3%). About 66.5% of adolescent girls were in the normal weight group.
The crude association between dietary habits and obesity among Dubai adolescents is presented in table II. The risk of obesity decreased among girls who always (OR = 0.5; CI 0.2-1.0) and frequently (OR = 0.9; CI 0.5-1.7) ate breakfast, compared to those who never ate breakfast. The case was similar with boys who always (OR = 0.6; CI 0.3-1.4) and frequently (OR = 0.7; CI 0.3-1.5) ate breakfast. The association between obesity and frequency of breakfast intake was significant among girls (P = 0.048) but not in boys. A high risk of obesity was associated with eating breakfast at school in boys (OR = 3.0; CI 1.1-8.3) and in girls (OR = 3.4; CI 1.6-7.4). This is nearly three times more than the risk of eating breakfast at home for boys (OR = 1.4; CI 0.6-3.5) and girls (OR = 1.2; CI 0.6-2.6) respectively. There was a statistically significant difference between, snacking in between breakfast and lunch and obesity in girls (P = 0.044) but not in boys. Midnight snacking was significantly associated with obesity in boys (P = 0.050), but not in girls (P = 0.161). However, compared to the reference group, the obesity risk was higher in girls who always consumed midnight snacks (OR = 1.2; CI 0.6-2.2), but was not so in boys (OR =0.5; CI 0.2-1.0).
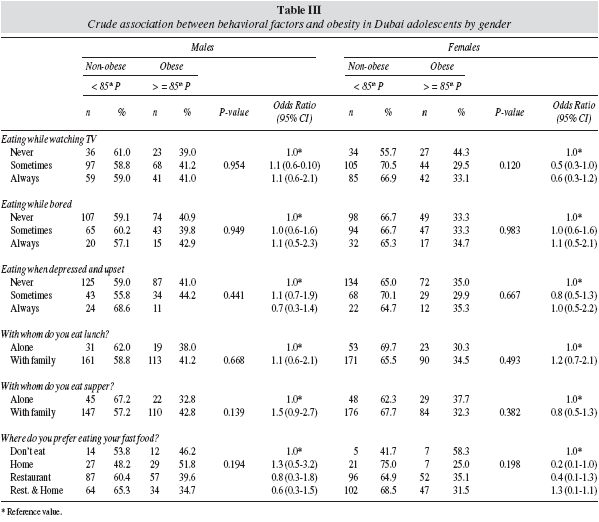
The crude association between behavioural habits and obesity in Dubai adolescent is presented in table III. The risk of obesity increased in boys who sometimes (OR = 1.1; CI 0.6-1.0) and always (OR = 1.1; CI 0.6-2.1) ate while watching TV, compared to those who never ate while watching TV. In contrast, there was a decrease in the risk of obesity in girls who sometimes (OR = 0.5; CI 0.3-1.0) and always (OR = 0.6; CI 0.3-1.2) ate while watching TV, compared to the reference group. The risk of obesity was higher in boys (OR = 1.1; CI 0.6-2.1) and girls (OR = 1.2; CI 0.7-2.1) who ate lunch with the family compared to those who ate alone. In the case of supper, the risk of obesity were higher in boys (OR = 1.5; CI 0.9-2.7) but lower in girls(OR = 0.8; CI 0.5-1.3). The location of the consumption of fast foods was not significantly associated with obesity, however the risk of obesity was higher in boys who ate fast foods at home (OR = 1.3; CI 0.5-3.2), but lower in girls (OR = 0.2; CI 0.1-1.0).
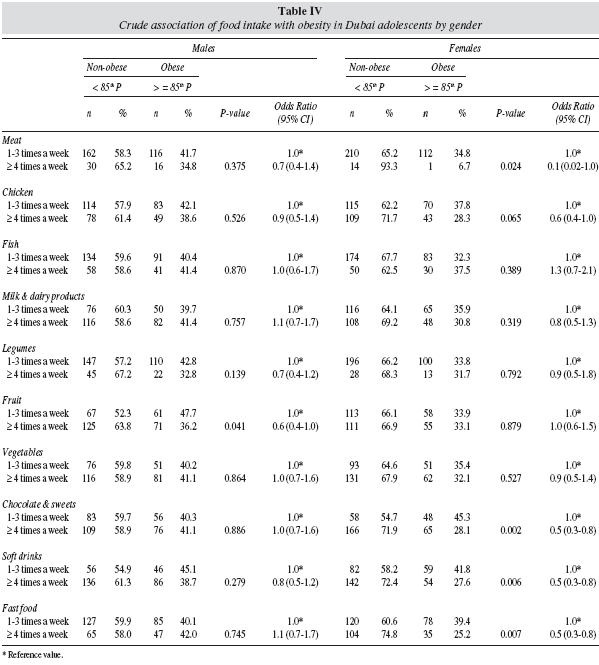
The crude association between necessary and nonnecessary food intake and obesity among Dubai adolescents is presented in Table IV. There was a statistically significant difference between the frequency of meat consumption and obesity in girls (P = 0.024) but not in boys. Boys who consumed meat more than 4 times a week had a higher risk of obesity (OR = 0.7; CI 0.4-1.4) compared to girls (OR = 0.1; CI 0.02-1.0). The risk of obesity with fish intake was higher in girls (OR = 1.3; CI 0.7-2.1) compared to boys (OR = 1.0; CI 0.6-1.7). Boys had a higher risk of obesity with consumption of dairy products (OR = 1.1; CI 0.7-1.7) compared to girls (OR = 0.8; CI 0.5-1.3). Consumption of fruits was significantly associated with obesity in boys (P = 0.041); though the risk of obesity decreased (OR = 0.6; CI 0.4-1.0). There was a significant association between the consumption of chocolates and sweets (P = 0.002), soft drinks (P = 0.006) and fast foods (P = 0.007) and obesity in girls but not in boys. However, the risk of obesity were double that for boys compared to girls: chocolates and sweets (OR = 1.0; CI 0.7-1.6 and OR = 0.5; CI 0.3-1.8 respectively), soft drinks (OR = 0.8; CI 0.5-1.2 and OR = 0.5; CI 0.3-0.8 respectively), fast foods (OR = 1.1; CI 0.7-1.7 and OR = 0.5; CI 0.3-0.8 respectively).
Discussion
The higher proportions of obesity observed amongst adolescents in Dubai the UAE are in concurrence with previous reports that showed that 22.9% girls and 20.2% boys in UAE were overweight and obese.14 The prevalence of obesity among girls in this study is higher than that reported for female students in Saudi Arabia where overweight and obesity were 20% and 11% respectively.17 The main reasons for the rising levels of obesity are the improved socio-economic status of many Middle East countries, which makes life more sedentary and is coupled with diminished patterns of exercise.3
The findings that missing breakfast was significantly related to the weight status of female adolescents are in accordance with observations made among adolescents in Brazil and in the Gulf region. 18,19 Skipping breakfast is a reflection of a dieting technique practiced by girls, and studies in the US indicated that 32% of female college students aged 18 to 24 years skip breakfast as means of weight control.20 It is reported that the emergence of dieting among girls is most prevalent at 13 and 14 years of age and remains prevalent throughout adulthood.21 It is also possible that girls who miss breakfast tend to consume greater amounts of food at lunch thereby gaining weight.
The higher weight status resulting from eating breakfast at school as seen in this study could be due to the consumption of high density foods. Recently, a study by Musaiger et al.,23 found that foods such as thymes bread and the sausage sandwich commonly served in Bahraini school canteens have greater calorific values. In Bahrain, it was found that beef burgers, liver and egg sandwiches were consumed more by boys, while girls preferred carbonated beverages, cheese, uncarbonated canned drinks and broad beans as a morning snack.23 Frequent snacking is an important feature of adolescent food consumption, and since many snacks have a high caloric content, the direct relationship between the frequency of snacking and obesity observed in this study may be indicative of increased energy intake.24 Snacking may contribute to weight gain by both providing occasions for consumption of energy-dense foods in between meals, as well as by increasing the frequency of such intake.25 The observation that midnight snacking was linked to obesity in U.A.E. boys and not in girls, is not entirely unexpected and appears to be related to the social context in which snacking occurs, wherein the UAE adolescents have more opportunity to go out, especially at night.
The practice of consuming meals in front of the television has become very popular among UAE families in recent years and reports indicate that more than half of secondary school girls in the UAE frequently eat while watching television.23 This is contrary to reports that there exists a positive relationship between obesity and watching television, 26 this study indicates no such association between consuming meals while watching television and obesity in both boys and girls. This could be because, it was not the amount of food consumed during television viewing that was associated with the adolescent's BMI but, it was the fat content of the foods.27 This could explain the lack of association as seen in this study. It should, however, be noted that since the type of food consumed during TV viewing was not determined, it is not possible to draw any concrete conclusion with regard to the energy content. Another observation in this study was that eating when upset, angry or bored was not associated with an increase in body mass index and obesity in both the genders. It has been reported that that a stressed or depressed state in humans induces either increased comfort foodintake and body weight gain or decreased intake and body weightloss.28
Family food habits are a major factor influencing a child's energy intake, which includes not only food selection for meals but also the habit of eating meals together with parents and other family members.29 The results of this study indicated that eating meals together with the family or alone had no significant relation to obesity in boys and girls. A similar outcome has been reported among American adolescents wherein, it was suggested that although eating family dinner improved diet quality, prevention of overweight was not an additional benefit.30
Daily consumption of fruit and vegetables is an important indicator of a healthy diet and the beneficial effect of lowered BMI has been well documented.31
Contrary to expectations, the findings from this study indicate that fruit consumption revealed a significant association with obesity in boys. One plausible explanation could be the consumption of canned fruits packed in syrup in place of fresh fruit resulting in increased calorie consumption. A previous study of Bahraini adults showed that frequent consumption of vegetables was negatively related to obesity whereas, fruit consumption was positively related.23
The findings that the frequency of eating fast foods was significantly related to obesity in girls but not in boys may be related to a sedentary lifestyle amongst women. As reported by Kerkadi,32 the lack of physical activity due to social and religious norms precludes many UAE female students, especially obese and overweight ones, from engaging in public sports, thereby contributing to their higher weight status. It should also be noted that we found the risk of obesity due to consumption of sweets, soft drinks and fast foods was lower in girls than in boys. One reason could be due to a greater consumption of diet sodas by girls by using portion size control. This leads to the minimizing of overall energy consumption and existing data suggests that portion size influences energy intake.33 Studies in the Gulf region have reported in recent years that there is a preference for a smaller body size among Arab women.34,35 This could also explain the lower overweight and obesity status among girls versus boys as seen in this study. Furthermore, it has been reported that greater involvement in healthy dietary habits is associated with being female.36
The findings from this study suggest that although multiple factors can account for weight gain, the basic cause is an excess of energy intake over expenditure. An obvious reason is the consumption of food prepared outside the home in addition to unhealthy food selection practices thereby resulting in the higher weight status. Since snacks eaten between meals provide up to a quarter of the daily energy intake in some adolescent populations, limiting snacks or replacing them with healthy alternatives may be effective. Activity patterns have changed much in the past decade, making life more sedentary and the need to promote a healthy lifestyle and regular physical activity among adolescents has to become a top priority for health professionals. Understanding the contexts in which adolescents snack and skip meals may help parents and health professionals develop strategies to promote healthy food and lifestyle habits among adolescents.
References
1. De Onis M, Blössner M. Prevalence and trends of overweight among preschool children in developing countries. Am J Clin Nutr 2000; 72 (4): 1032-1039. [ Links ]
2. Samuelson G. Dietary habits and nutritional status in adolescents over Europe. An overview of current studies in the Nordic countries. Eur J Clin Nutr 2000; 54 (1S): S21-S28. [ Links ]
3. Musaiger AO. Overweight and obesity in the Eastern Mediterranean region: can we control it? East Mediterr Health J 2004; 10 (6): 789-793. [ Links ]
4. Westerbeek H, Smith A. Corporate social responsibility and community health in the UAE: The case of the Al Jazira sport and health foundation. Middle East Journal of Business 2005 1,1 Available at http://www.mejb.com/upgrade_flash/Vol1_Issue1/Corporate-Social-Responsibility.htm [ Links ]
5. Al-haddad FH, Bertis LB, Ghafar AGAM. Childhood obesity in United Arab Emirates schoolchildren: A national study. Ann Hum Biol 2005; 32 (1): 72-79. [ Links ]
6. Jebb SA, Moore MS. Contribution of a sedentary lifestyle and inactivity to the etiology of overweight and obesity: current evidence and research issues. Med Sci Sports Exerc 1999; 31 (11S): S534-S541. [ Links ]
7. Kiess W, Böttner A, Raile K et al. Type 2 diabetes mellitus in children and adolescents: a review from a European perspective. Horm Res 2003; 59(1S): 77S-84S. [ Links ]
8. Sallis JF, Glanz K. The role of built environments in physical activity, eating, and obesity in childhood. Future Child 2006; 16 (1): 89-108. [ Links ]
9. Musaiger AO. Diet and prevention of coronary heart disease in the Arab Middle East countries. Med Princ Pract 2002; 11 (2S): 9S-16S. [ Links ]
10. Anderson PM, Butcher KF. Childhood obesity: trends and potential causes of childhood obesity. Future Child 2006; 16 (1): 19-45. [ Links ]
11. Taveras EM, Sandora TJ, Shih MC, et al. The association of television and video viewing with fast food intake by preschool-age children. Obesity 2006; 14: 2034-2041. [ Links ]
12. Musaiger AO, Lloyd OL, Al-Neyadi SM, Bener AB. Lifestyle factors associated with obesity among male university students in the United Arab Emirates. Nutrition & Food Science 2003; 33 (4): 145-147. [ Links ]
13. Al-Hourani HM, Henry GJ, Lightowler HJ. Prevalence of overweight among adolescent girls in the United Arab Emirates. Am J Hum Biol 2003; 15: 758-764. [ Links ]
14. Malik M, Bakir A. Prevalence of overweight and obesity among children in the United Arab Emirates. Obes Rev 2007; 8 (1): 15-20. [ Links ]
15. Fidanza F. Anthropometric methodology. In Fidanza, F. (eds) Nutritional Assessment: a Manual for Population Studies. Chapman & Hall, London, pp. 1-43; 1991. [ Links ]
16. Golan M, Weizman A. Reliability and validity of the family eating and activity habits questionnaire. Eur J Clin Nutr 1998; 52 (10): 771-777. [ Links ]
17. Al-Saeed WY, Al-Dawood KM, Bukhari IA, Bahnassy A. Prevalence and socioeconomic risk factors of obesity among urban female students in Al-Khobar city, Eastern Saudi Arabia, 2003. Obes Rev 2007; 8 (2): 93-99. [ Links ]
18. Terres NG, Pinheiro RT, Horta BL, Pinheiro KAT, Horta LL. Prevalence and factors associated to overweight and obesity in adolescents. Rev Saude Publica 2006; 40 (4): 627-633. [ Links ]
19. Musaiger AO. Height, weight and menarcheal age of adolescent girls in Oman. Ann Hum Biol 1991; 18 (1): 71-74. [ Links ]
20. Malinauskas BM, Raedeke TD, Aeby VG, Smith JL, Dallas MB. Dieting practices, weight perceptions, and body composition: A comparison of normal weight, overweight, and obese college females. Nutr J 2006; 5:11 Available at http://www.nutritionj.com/content/5/1/11 [ Links ]
21. Huon G, Lim J. The emergence of dieting among female adolescents: age, body mass index, and seasonal effects. Int J Eat Disord 2000; 28 (2): 221-225. [ Links ]
22. Musaiger AO, Al-Jedah JH, D'Souza R. Nutrient composition of foods provided by school canteens in Bahrain. Nutrition & Food Science 2007; 37 (4): 246-253. [ Links ]
23. Musaiger AO, Gregory WB. Profile of body composition of school children (6-18Y) in Bahrain. Int J Obes Relat Metab Disord 2000; 24 (9): 1093-1096. [ Links ]
24. Forslund HB, Torgerson JS, Sjöström L, Lindroos AK. Snacking frequency in relation to energy intake and food choices in obese men and women compared to a reference population. Int J Obes 2005; 29 (6): 711-719. [ Links ]
25. Jahns L, Popkin BM. The increasing prevalence of snacking among US children from 1977 to 1996. Journal of Pediatrics 2001; 138 (4): 493-498. [ Links ]
26. Robinson TN. Television viewing and childhood obesity. Pediatr Clin North Am 2001; 48 (4): 1017-1025. [ Links ]
27. Matheson DM, Killen JD, Wang Y, Varady A, Robinson TN. Children's food consumption during television viewing. Am J Clin Nutr 2004; 79 (6): 1088-1094. [ Links ]
28. Dallman MF, Pecoraro N, Akana SF et al. Chronic stress and obesity: A new view of "comfort food". Proc Natl Acad Sci USA 2003; 100 (1): 11696-11701. [ Links ]
29. Birch LL, Davidson KK. Family environmental factors influencing the developing behavioural controls of food intake and childhood overweight. Pediatr Clin North Am 2001; 48 (4):893-907. [ Links ]
30. Taveras EM, Rifas-Shiman SL, Berkey CS, et al. Family dinner and adolescent overweight. Obes Res 2005; 13: 900-906. [ Links ]
31. Epstein LH, Gordy CC, Raynor HA, Beddome M, Kilanowski CK, Paluch R. Increasing fruit and vegetable intake and decreasing fat and sugar intake in families at risk for childhood obesity. Obes Res 2001; 9 (3): 171-178. [ Links ]
32. Kerkadi A. Evaluation of nutritional status of United Arab Emirates University female students. Emirates Journal of Agricultural Science 2003; 15; 42-50 http://www.cfs.uaeu.ac.ae/research/ejas.html [ Links ]
33. Ello-Martin JA, Ledikwe, JH, Rolls BJ. The influence of food portion size and energy density on energy intake: implications for weight management. Am J Clin Nutr 2005; 82 (1S): 236S-241S. [ Links ]
34. Rasheed P. Perception of body weight and self-reported eating and exercise behaviour among obesity and non-obese women in Saudi Arabia. Public Health 1998; 112 (6): 409-414. [ Links ]
35. Musaiger AO, Ajlan D, Al-Saad N et al. Dietary habits, lifestyle and chronic diseases among Bahraini adults. Bahrain Centre for Studies and Research, Bahrain; 2005. [ Links ]
36. Johnson F, Wardle J, Griffith J. The adolescent food habits checklist: reliability and validity of a measure of healthy eating behaviour in adolescents. Eur J Clin Nutr 2002; 56 (7): 644-649. [ Links ]
![]() Correspondence:
Correspondence:
Abdulrahman O. Musaiger.
Director of Nutritional Studies.
Bahrain Centre for Studies and Research.
P.O. Box 496, Manama-Kingdom of Bahrain
E-mail: amusaiger@bscr.gov.bh; amusaiger@gmail.com
Recibido: 25-VI-2008.
Aceptado: 14-VIII-2008.