Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Nutrición Hospitalaria
versión On-line ISSN 1699-5198versión impresa ISSN 0212-1611
Nutr. Hosp. vol.25 no.2 Madrid mar./abr. 2010
Standardisation of the Waist Circumference (WC) for each range of Body Mass Index (BMI) in adult outpatients attended to in Endocrinology and Nutrition Departments
Estandarización de la circunferencia de cintura (WC), para cada rango de índice de masa corporal (BMI) en pacientes adultos atendidos en un servicio de endocrinología y nutrición
M. López de la Torre1, D. Bellido2, A. Soto3, J. Carreira2 and A. Hernández Mijares3
1Endocrinology Department. Hospital Virgen de las Nieves (Granada).
2Endocrinology Department. Hospital Arquitecto Marcide. Ferrol. La Coruña.
3Endocrinology Department. Hospital Universitario de La Coruña. La Coruña.
4Endocrinology Department. Hospital Dr. Peset. Valencia. España.
ABSTRACT
By this study we seek the expectable range of waist circumference (WC) for every degree of body mass index (BMI), which will serve to studies targeting ascertaining the health risk. We studied 2,932 patients (39.6% men and 60.4% women, between 18 and 96 years ) of the same ethnic group who consecutively attended outpatient departments of our clinics between 2000 and 2004.. BMI correlated linearly with the WC (cc: 0.85; p < 0.001). The men, the obese, and diabetics were older (p < 0.001). BMI was greater in women and WC in men. The women had a greater WC if they had diabetes (p < 0.01), being equal to diabetic males. The men had greater WC when they had diabetes (p < 0.001). Waist at risk was detected (men > = 102 cm and women > = 88 cm) in 94.3% of the obese, in 32.3% of overweight patients, in 3.8% of patients with BMI < 25, in 84.3% of diabetics, and in 72.6% of patients without diabetes. We made graphic standardisation of WC with regard to BMI, and we calculated the percentiles 10, 25, 50, 75 and 90, grouping in ranges of 2 kg/m2 of BMI. The diabetic patients are grouped in ranges of 4 kg/m2. As conclusion we present a standardisation of the WC measurement of patients attended to in our Endocrinology and Nutrition practices distributed in percentiles as a clinically usable tool to define the ranges of WC for every BMI value.
Key words: Obesity. Diabetes mellitus. Waist circumference. Body mass index. Standardization.
RESUMEN
En este estudio hemos buscado el rango de circunferencia de cintura (WC) para cada grado de índice de masa corporal (BMI), que sirva para estudios que determinen riesgos de salud. Estudiamos 2.932 pacientes (39,6% varones y 60,4% mujeres, entre 18 y 96 años) del mismo grupo étnico que consecutivamente asistieron a consultas externas de nuestras clínicas entre 2000 and 2004. El BMI correlacionó linealmente con la WC (cc: 0,85; p < 0,001). Eran mayores los varones, los obesos y los diabéticos. El BMI era mayor en mujeres y la WC en varones. Las mujeres tenían mayor WC si eran diabéticas (p < 0,01), igualando a los hombres. Los varones tenían mayor WC si eran diabéticos (p < 0,001). La circunferencia de riesgo (varones > = 102 cm y mujeres > = 88 cm) la presentaban el 94,3% de los obesos, el 32,3% de los pacientes con sobrepeso y el 3,8% de pacientes con BMI < 25, el 84,3% de diabéticos y el 72,6% de pacientes sin diabetes. Elaboramos una estandarización gráfica de WC en relación con BMI y calculamos los precentiles 10, 25, 50, 75 y 90, agrupados en rangos de 2 kg/m2 de BMI. Como el número de diabeticos es menor, los agrupamos en rangos de 4 kg/m2. En conclusión presentamos una estandarización de la WC de pacientes atendidos en nuestra consulta de endocrinología y nutrición distribuidos en percentiles como herramienta utilizable clínicamente para definir rangos de WC para cada valor de BMI.
Palabras clave: Obesidad. Diabetes mellitus. Circunferencia de cintura. Índice de Masa Corporal. Estandarización.
Materials and methods
The study included a total of 2,932 patients (39.6% men and 60.4% women) who consecutively attended outpatient departments of the Endocrinology and Nutrition Services of the Spanish hospitals Virgen de las Nieves (Granada), Juan Canalejo (La Coruña) and Dr. Peset (Valencia) between 2000 and 2004. Patient age was comprised between 18 and 96 years, with no differences by sexes (45.9 ± 12.4 years men and 43.8 ± 14.3 years women).
BMI correlated linearly with the WC (cc: 0.85; p < 0.001), whereby the greater the BMI the greater the WC. The age, BMI and WC of the population studied and of the group of obese subjects are presented in table 1. The men were older than the women, the obese (obese 45.4 ± 13.8, non-obese 42.9 ± 13.1 years, p <0.001) and diabetics (p < 0.001).
BMI was greater in women and WC in men. The women had a greater WC if they had diabetes (p < 0.01), being equal in this parameter to diabetic males The men had greater WC when they had diabetes (p < 0.001). Waist at risk was detected (men > = 102 cm and women > = 88 cm) in 94.3% of the obese (men 91.8%, women 95.7%), in 32.3% of overweight patients (men 22.2%, women 43.9%), in 3.8% of patients with BMI < 25 (men 2%, women 5.3%), in 84.3% of diabetics (men 74.6%, women 94%), and in 72.6% of patients without diabetes (men 63.7%, women 78.2%).
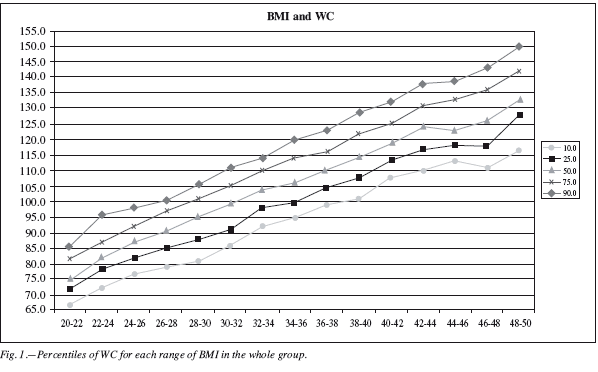
To obtain a graphic standardisation of WC with regard to BMI, we calculated the percentiles 10, 25, 50, 75 and 90, grouping in ranges of 2 kg/m2 of BMI (including patients that exceed a BMI value until the next one). We thus obtain the distribution from table 2 and figures 1, 2 and 3. Due to the difference found in BMI and WC between men and women, and between diabetic and non-diabetic patients, distribution is presented by sexes, and separately for diabetic patients. Since there were no significant differences in terms of WC between diabetic men and women, no different bysex graphics are provided for them. As the number of these patients is lower, they are grouped in ranges of 4 kg/m2.
Introduction
Obesity is the most frequent metabolic disease in the western world. Although prevalence data in Europe are variable (from 4% to 28% in males and from 6.2% to 36.5% in women), the prevalence in Spain and Italy is particularly high.1
The importance of obesity is derived fundamentally from its relationship with cardiovascular diseases and with type 2 diabetes mellitus, among others, with serious medical and economic consequences for public health, ranging from 0.09% to 0.61% of the gross domestic product of every country.2.
Obesity is defined by a Body Mass Index (BMI) value of 30 kg/m2 or greater, calculated as weight/height2 (BMI),3 and overweight by a value between 25 and 30 kg/m2. BMI has been chosen as a surrogate measurement of body fat content because it presents a good correlation with total body fat, and is an indicator of morbidity and mortality, even in the degree of overweight.4-7 In different works, the relationship with mortality describes a J curve, increasing progressively as of the degree of overweight.7,8
The risk entailed in obesity varies depending on the fat compartment considered, so that the visceral fat compartment is a better predictor of cardiometabolic risk and mortality than accumulated subcutaneous fat, whereby its determination is deserving of increasingly greater interest in clinical practice,8-17 and it may also be a better indicator of health expenditure than the BMI.18 The measurement of the waist circumference (WC) is a simple way of deducing a patient's level of visceral fat, and complements the information provided by the BMI.10,19,20 BMI, WC and the relationship of both of the latter with morbidity and mortality depend on multiple factors, which include age, gender and ethnic group.21,22.
Thresholds of WC that can be used as markers of morbidity and mortality have been sought with great interest, and a WC equal to or higher than 102 cm in men and 88 cm in women has been proposed as pathological, although the usefulness of these thresholds as predictors as a risk for health is still under debate.11,17,23.
The definition of a given threshold of WC may be of interest in individuals with a slightly high BMI, but this does not add further information when the BMI is frankly high, since the majority of obese patients have a WC above the risk threshold. It is therefore insufficient to consider a single threshold of WC for all individuals, 11,17 and the information provided by the combined determination of the WC must be associated with the BMI.
Our intention was to progress in this idea, seeking the expectable range of WC for every degree of BMI, which will serve to subsequently address studies targeting ascertaining the health risk. For this purpose we have chosen diabetic and non-diabetic patients that we see in endocrinology and nutrition clinics, which is where cardiometabolic diseases are concentrated. The population considered here is white people, of the same ethnic group, and the results are presented distinguished by gender and type 2 diabetes mellitus.
Materials and methods
The study included a total of 2,932 patients (39.6% men and 60.4% women) who consecutively attended outpatient departments of the Endocrinology and Nutrition Services of the Spanish hospitals Virgen de las Nieves (Granada), Juan Canalejo (La Coruña) and Dr. Peset (Valencia) between 2000 and 2004. Patient age was comprised between 18 and 96 years, with no differences by sexes (45.9 ± 12.4 years men and 43.8 ± 14.3 years women).
Diabetic condition was defined by the American Diabetes Association.24
The anthropometric parameters included weight, height, BMI, WC was measured using standard methods. Weight was measured in kilograms, and height was measured in centimetres using stadiometer, both measurements of the subject in light clothing and no shoes. BMI was calculated by dividing the weight in kilograms by the height in square meters. The WC in cm was measured with a tape measure at a point midway between the last rib and the iliac crest, with the patient standing and on expiration.
Statistical analysis: The data were pooled together and managed on an Excel spreadsheet. A descriptive analysis was performed of all the variables collected, and 95% confidence intervals were calculated. Mean and standard deviations summarized the continuous variables. The percentiles of 10, 25, 50, 75 and 90 were calculated for every range of BMI (with patients that exceeded one BMI value being grouped into each range until the next value).
A Student's t-test or a Mann-Whitney test was used to compare between-group numerical parameters, after checking normality with the Kolmogorov-Smirnov test. Values of p < 0.05 were considered significant. All the tests were two-sided.
Correlation and linear regression analyses by Pearson's correlation coefficient were performed to study the association of BMI with WC in diabetic and not diabetic patients.
The statistical analysis was carried out with SPSS 12.0 for Windows.
Results
BMI correlated linearly with the WC (cc: 0.85; p < 0.001), whereby the greater the BMI the greater the WC. The age, BMI and WC of the population studied and of the group of obese subjects are presented in table 1. The men were older than the women, the obese (obese 45.4 ± 13.8, non-obese 42.9 ± 13.1 years, p < 0.001) and diabetics (p < 0.001).
BMI was greater in women and WC in men. The women had a greater WC if they had diabetes (p < 0.01), being equal in this parameter to diabetic males The men had greater WC when they had diabetes (p < 0.001). Waist at risk was detected (men > = 102 cm and women > = 88 cm) in 94.3% of the obese (men 91.8%, women 95.7%), in 32.3% of overweight patients (men 22.2%, women 43.9%), in 3.8% of patients with BMI < 25 (men 2%, women 5.3%), in 84.3% of diabetics (men 74.6%, women 94%), and in 72.6% of patients without diabetes (men 63.7%, women 78.2%).
To obtain a graphic standardisation of WC with regard to BMI, we calculated the percentiles 10, 25, 50, 75 and 90, grouping in ranges of 2 kg/m2 of BMI (including patients that exceed a BMI value until the next one). We thus obtain the distribution from table I and figures 1, 2 and 3. Due to the difference found in BMI and WC between men and women, and between diabetic and non-diabetic patients, distribution is presented by sexes, and separately for diabetic patients. Since there were no significant differences in terms of WC between diabetic men and women, no different by sex graphics are provided for them. As the number of these patients is lower, they are grouped in ranges of 4 kg/m2.
Discussion
The direct relationship between BMI and WC is well-known.25 The first is an indicator of the degree of corporality and the second of visceral fat. These parameters are measured in routine fashion in clinical practice as they are regarded as independent indicators of body fat content26 and predictors of cardiovascular risk.19,27,28 Moreover, both BMI and WC help to predict the risk of developing type 2 diabetes mellitus. BMI is a good predictor of the development of type 2 diabetes mellitus29 and of insulin resistance.12 Fat distribution can even predict progression to type 2 diabetes mellitus better than BMI.30 It is assumed that the accumulation of visceral fat plays an important role in the aetiology of this type of diabetes to subject the liver to an excess of free fatty acids, producing insulin resistance and hyperinsulinaemia.31,32 Our study verified the direct relationship between BMI and WC, both in diabetics and non-diabetics, as well as the relationship between age, BMI and WC and gender and the presence of diabetes mellitus. Our diabetic patients presented greater BMI, WC and age.
Levels of normality, overweight and obesity were established for BMI (BMI less than 25, between 25 and 30, and 30 or above, respectively).3 These thresholds have been maintained, whereby the different studies have defined a J curve where mortality increases progressively with the different degrees of overweight and obesity.
The interest in establishing these thresholds is derived from the need to detect cardiometabolic risk with their help. In this regard, the thresholds of WC make it possible to define "risk" groups for whom preventive activities can be indicated, even with normal or slightly increased BMI.
The thresholds of normality of WC are the most debated. A WC equal to or higher than 102 cm is regarded as pathological in men and 88 cm in women, as it corresponds to a BMI greater than or equal to 30 (kg/m2,33 although others have been proposed.34,35 In the IDEA study, this value was exceeded by 29% males and 48% women among the 182,970 patients aged between 18 and 80 years who attended primary care facilities in 63 countries.10 Similarly, in the overweight patients of our group, these thresholds have allowed us to select 32.3% with a greater cardiovascular risk. But the determination of WC is not sensitive enough to detect the risk in the group of obese patients.11,17,36 In our study, 94.3% of the obese exceeded these values. Had we applied the IDF criteria for European Caucasians (94 cm in men and 80 cm in women) these percentages would have been even greater.
We found a greater WC in men than in women, and in both sexes when they are diabetic. In women with diabetes, WC reaches values similar to diabetic males, whom they surpass in BMI. This relationship of WC with the male sex and with diabetes has been broadly confirmed in other transversal and prospective studies.4,30,37-40
These differences justify the definition of different risk thresholds for men and women in non-diabetic individuals (NCEP/ATPIII),41 but these thresholds could not be extrapolated to the population that is already diabetic, where we found no differences in WC between sexes, and where cardiovascular risk increases with the existence of diabetes. We have therefore offered an individualised standardisation for the diabetic population.
On the other hand, WC and BMI should be considered separately. In the observational studies, the J curve of the mortality study is progressive as BMI and WC increase, from degrees below those considered to be pathological.7,8,22
The greater or lesser importance attributed to BMI and WC depends on the approach taken by the studies, the population's circumstances, age, gender and degree of obesity.13,35,42 The true usefulness lies in combining both determinations, as was demonstrated in the Nurses Health Study,28 where the risk of coronary artery disease adjusted for age throughout an 8-year monitoring increases with WC for each tercile of BMI. In this study, the incidence of coronary artery disease was similar in women with lower BMI and greater WC compared to those who had a greater BMI and lower WC. The greater incidence was to be found in the greater levels of BMI and WC. The joint usefulness of BMI and WC in clinical practice was confirmed in subsequent studies. For both parameters, WC cut-off levels have been proposed in the different categories of BMI with regard to cardiovascular risk, with risk determined by the Framingham scale, which predicts the possibility of coronary events after 10 years. Optimal thresholds can be defined as 98, 109 and 124 in men and as of 92, 103 and 115 in women in the categories of overweight, degree 1 obesity and degree 2 obesity orhigher, respectively. With these thresholds, Ardern etal.43 improve sensitivity and specificity to detect patients at risk.
Our work seeks to further develop this idea, defining the expectable range of WC for every degree of BMI, which may serve for subsequent health risk studies. With this purpose in mind, we chose a group of patients with greater frequency of metabolic diseases, obesity and diabetes, who attend Endocrinology and Nutrition clinics, all of them Caucasian. This selection necessarily assumes a limitation, since the results might not be applicable to the general population.
In this study we offer the clinician the measurement of WC graphically by means of WC percentiles for each range of BMI (which may be translated to other dispersion values, such as the SDS). As WC depends on gender and on the patient's diabetic condition, the data must be displayed separately. But WC did not present differences between sexes in diabetics, and for this reason we do not provide a graphic differentiation in this case.
The percentiles of WC for each range of BMI inform the clinician as to patients whose abdominal fat (and therefore WC) is above or below the degree expected for their degree of corporality (BMI). The percentile that should be regarded as normal or pathological has yet to be defined, and would be the one that distinguished between patients whose health risks increase, and which will have to be determined in cross-sectional, prospective and predictive studies that may be performed by applying percentiles or other deviation parameters.
In conclusion, we present a standardisation of the WC measurement of patients attended to in our Endocrinology and Nutrition practices distributed in percentiles as a clinically usable tool to define the ranges of WC for every BMI value.
References
1. Berghöfer A, Pischon T, Reinhold T, Apovian CM, Sharma AM, Willich SN. Obesity prevalence from a European perspective: a systematic review. BMC Public Health 2008; 8: 200. [ Links ]
2. Müller-Riemenschneider F, Reinhold T, Berghofer A, Willich SN. Health-economic burden of obesity in Europe. Eur J Epidemiol 2008; 23: 499-509. [ Links ]
3. Salas-Salvado J, Rubio MA, Barbany M, Moreno B y Grupo Colaborativo de la SEEDO. Consenso SEEDO 2007 para la evaluación del sobrepeso y la obesidad y el establecimiento de criterios de intervención terapéutica. Med Clin (Barc) 2007; 128: 184-96. [ Links ]
4. Stevens J, Couper D, Pankow J et al. Sensitivity and specificity of anthropometrics for the prediction of diabetes in a biracial cohort. Obes Res 2001; 9: 696-705. [ Links ]
5. Jee SH, Sull JW, Park J et al. Body-mass index and mortality in Korean men and women. N Engl J Med 2006; 355: 779-87. [ Links ]
6. Flegal KM, Graubard BI, Williamson DF, Gail MH. Excess deaths associated with underweight, overweight, and obesity. JAMA 2005; 293: 1861-7. [ Links ]
7. Adams KF, Schatzkin A, Harris TB et al. Overweight, obesity, and mortality in a large prospective cohort of persons 50 to 71 years old.N Engl J Med 2006; 355: 763-78. [ Links ]
8. Pischon T, Boeing H, Hoffmann K et al. General and abdominal adiposity and risk of death in Europe. N Engl J Med 2008; 359: 2105-20. [ Links ]
9. Wang Y, Rimm EB, Stampfer MJ, Willett WC, Hu FB. Comparison of abdominal adiposity and overall obesity in predicting risk of type 2 diabetes among men. Am J Clin Nutr 2005; 81: 555-63. [ Links ]
10. Balkau B, Deanfield JE, Despres JP et al. International Day for the Evaluation of Abdominal Obesity (IDEA): a study of waist circumference, cardiovascular disease, and diabetes mellitus in 168,000 primary care patients in 63 countries. Circulation 2007; 116: 1942-51. [ Links ]
11. Bigaard J, Tjonneland A, Thomsen BL, Overvad K, Heitmann BL, Sorensen TI. Waist circumference, BMI, smoking, and mortality in middle-aged men and women. Obes Res 2003; 11: 895-903. [ Links ]
12. Farin HM, Abbasi F, Reaven GM. Comparison of body mass index versus waist circumference with the metabolic changes that increase the risk of cardiovascular disease in insulin-resistant individuals. Am J Cardiol 2006; 98: 1053-6. [ Links ]
13. Hoefle G, Saely CH, Aczel S et al. Impact of total and central obesity on vascular mortality in patients undergoing coronary angiography. Int J Obes (Lond) 2005; 29: 785-91. [ Links ]
14. Lakka HM, Lakka TA, Tuomilehto J, Salonen JT. Abdominal obesity is associated with increased risk of acute coronary events in men. Eur Heart J 2002; 23: 706-13. [ Links ]
15. Yusuf S, Hawken S, Ounpuu S et al. Effect of potentially modifiable risk factors associated with myocardial infarction in 52 countries (the INTERHEART study): case-control study. Lancet 2004; 364: 937-52. [ Links ]
16. Empana JP, Ducimetiere P, Charles MA, Jouven X. Sagittal abdominal diameter and risk of sudden death in asymptomatic middle-aged men: the Paris Prospective Study I. Circulation 2004; 110: 2781-5. [ Links ]
17. Janssen I, Katzmarzyk PT, Ross R. Waist circumference and not body mass index explains obesity-related health risk. Am J Clin Nutr 2004; 79: 379-84. [ Links ]
18. Cornier MA, Tate CW, Grunwald GK, Bessesen DH. Relationship between waist circumference, body mass index, and medical care costs. Obes Res 2002; 10: 1167-72. [ Links ]
19. Pouliot MC, Despres JP, Lemieux S et al. Waist circumference and abdominal sagital diameter: best simple anthropometric indexes of abdominal visceral adipose tissue accumulation and related cardiovascular risk in men and women. Am J Cardiol 1994; 73: 460-8. [ Links ]
20. Ross R, Leger L, Morris D, De GJ, Guardo R. Quantification of adipose tissue by MRI: relationship with anthropometric variables. J Appl Physiol 1992; 72: 787-95. [ Links ]
21. Ford ES, Mokdad AH, Giles WH. Trends in waist circumference among U.S. adults. Obes Res 2003; 11: 1223-31. [ Links ]
22. Stevens J, Cai J, Pamuk ER, Williamson DF, Thun MJ, Wood JL. The effect of age on the association between body-mass index and mortality. N Engl J Med 1998; 338: 1-7. [ Links ]
23. Misra A, Vikram NK, Gupta R, Pandey RM, Wasir JS, Gupta VP. Waist circumference cut-off points and action levels for Asian Indians for identification of abdominal obesity. Int J Obes (Lond) 2006; 30: 106-11. [ Links ]
24. American Diabetes Association. Diagnosis and classification of diabetes mellitus. Diabetes Care 2004; 27: S5-S10. [ Links ]
25. Iwao S, Iwao N, Muller DC, Elahi D, Shimokata H, Andres R. Does waist circumference add to the predictive power of the body mass index for coronary risk? Obes Res 2001; 9: 685-95. [ Links ]
26. Janssen I, Heymsfield SB, Allison DB, Kotler DP, Ross R. Body mass index and waist circumference independently contribute to the prediction of non-abdominal, abdominal subcutaneous, and visceral fat. Am J Clin Nutr 2002; 75: 683-8. [ Links ]
27. Janssen I, Katzmarzyk PT, Ross R. Body mass index, waist circumference, and health risk: evidence in support of current National Institutes of Health guidelines. Arch Intern Med 2002; 162: 2074-9. [ Links ]
28. Rexrode KM, Carey VJ, Hennekens CH et al. Abdominal adiposity and coronary heart disease in women. JAMA 1998; 280: 1843-8. [ Links ]
29. Wannamethee SG, Shaper AG. Weight change and duration of overweight and obesity in the incidence of type 2 diabetes. Diabetes Care 1999; 22: 1266-72. [ Links ]
30. Snijder MB, Dekker JM, Visser M et al. Associations of hip and thigh circumferences independent of waist circumference with the incidence of type 2 diabetes: the Hoorn study. Am J Clin Nutr 2003; 77: 1192-7. [ Links ]
31. Santi MJ, Carrozas MA, Barba A, Astola A, Jiménez A, Mangas A. Circunferencia de la cintura como predictor de resistencia insulínica en varones jóvenes. Med Clin (Barc) 2005; 125: 46-50. [ Links ]
32. Jensen MD. Adipose tissue as an endocrine organ: implications of its distribution on free fatty acid metabolism. Eur Heart J 2006; 8: B13-B19. [ Links ]
33. Lean ME, Han TS, Morrison CE. Waist circumference as a measure for indicating need for weight management. BMJ 1995; 311: 158-61. [ Links ]
34. International Diabetes Federation. The IDF Consensus Worldwide definition of the Metabolic Syndrome. IDF 2005. Available at: http://www.idf.org/home/index.cfm?node=1429 [ Links ]
35. Zhu S, Wang Z, Heshka S, Heo M, Faith MS, Heymsfield SB. Waist circumference and obesity-associated risk factors among whites in the third National Health and Nutrition Examination Survey: clinical action thresholds. Am J Clin Nutr 2002; 76: 743-9. [ Links ]
36. Klein S, Allison DB, Heymsfield SB et al. Waist circumference and cardiometabolic risk: a consensus statement from Shaping America's Health: Association for Weight Management and Obesity Prevention; NAASO, The Obesity Society; the American Society for Nutrition; and the American Diabetes Association.Am J Clin Nutr 2007; 85: 1197-202. [ Links ]
37. Carey VJ, Walters EE, Colditz GA et al. Body fat distribution and risk of non-insulin-dependent diabetes mellitus in women. The Nurses' Health Study. Am J Epidemiol 1997; 145: 614-9. [ Links ]
38. Lundgren H, Bengtsson C, Blohme G, Lapidus L, Sjostrom L. Adiposity and adipose tissue distribution in relation to incidence of diabetes in women: results from a prospective population study in Gothenburg, Sweden. Int J Obes 1989; 13: 413-23. [ Links ]
39. Chan JM, Rimm EB, Colditz GA, Stampfer MJ, Willett WC. Obesity, fat distribution, and weight gain as risk factors for clinical diabetes in men. Diabetes Care 1994; 17: 961-9. [ Links ]
40. Ohlson LO, Larsson B, Svardsudd K et al. The influence of body fat distribution on the incidence of diabetes mellitus, 13,5 years of follow-up of the participants of the study of men born in 1913. Diabetes 1985; 34: 1055-8. [ Links ]
41. National Institutes of Health, National Heart LaBI. ATP III Guidelines At-A-Glance. Quick Desk Reference. U.S. Department of Health and Human Services. Public Health Service. NIH Publication º 01-3305 2001. Available at: http://www.nhlbi.nih.gov/guidelines/cholesterol/atglance.pdf [ Links ]
42. Rexrode KM, Buring JE, Manson JE. Abdominal and total adiposity and risk of coronary heart disease in men. Int J Obes Relat Metab Disord2001; 25: 1047-56. [ Links ]
43. Ardern CI, Janssen I, Ross R, Katzmarzyk PT. Development of health-related waist circumference thresholds within BMI categories. Obes Res 2004; 12: 1094-103. [ Links ]
![]() Correspondence:
Correspondence:
Diego Bellido Guerrero.
Hospital Arquitecto Marcide.
Ferrol. La Coruña. Spain.
E-mail: diego_bellido@arrakis.es
Recibido: 20-IX-2009.
Aceptado: 26-X-2009.