Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Nutrición Hospitalaria
versión On-line ISSN 1699-5198versión impresa ISSN 0212-1611
Nutr. Hosp. vol.26 no.5 Madrid sep./oct. 2011
Impact of two low-calorie meals with and without bread on the sensation of hunger, satiety and amount of food consumed
Repercusión de dos comidas hipocalóricas con y sin pan sobre la sensación de hambre, saciedad y cantidad de comida consumida
V. Loria Kohen, C. Gómez Candela, C. Fernández Fernández, A. Pérez Torres, M. Villarino Sanz and L. M. Bermejo
Department of Nutrition. La Paz University Hospital. Health Research Institute. IdiPAZ. Madrid. Spain
This study was made possible thanks to a research project funded by the "Pan cada día" (Daily Bread) open call promoted by the Scientific Committee of Bread and by Incerhpan (Interprofessional Agrifoods of the Cereals-Flour-Bread Chain). The authors declare no conflict of interest.
ABSTRACT
Background: The aim was to compare the differences in feelings of hunger and satiety in a group of overweight/obese women after eating a test meal with or without bread.
Patients and methods: The study included 122 women (BMI ≥ 25 < 40 kg/m2) who were randomly assigned to consume one of the following test meals: NO BREAD meal (2.40 MJ, 46% carbohydrates, 26% protein, 28% fat; which included rice or pasta) and BREAD meal (2.39 MJ, with equal caloric distribution and the same foods except with bread instead of rice or pasta). A visual analogue scale (VAS) was used, with 5 questions to be answered at different times: 1) just before eating, 2) just after eating and exactly 3) 60 and 4) 90 minutes after eating the test meal. The test was performed at the start and after 16 weeks of following a lifestyle modification program based on a low-calorie diet (with or without bread).
Results: 104 women completed the study (48.4 ± 9.0 years) with a baseline BMI of 29.8 ± 3.5 kg/m2. At the start of the study there were no significant differences in any of the VAS parameters measured between the groups. After 16 weeks, BREAD group obtained higher scores in question 3 (referring to the sensation of satiety) that were significant at time 3 (7 versus 5; p < 0.05) and time 4 (8 versus 4; p < 0.01).
Conclusions: The inclusion of bread in a low-calorie meal may result in a greater sensation of satiety after eating. These results contradict the recommendation to exclude bread from a food plan aimed at weight loss.
Key words: Obesity. Overweight. Satiety. Bread. Glycemic index. Hunger.
RESUMEN
Objetivos: Analizar las diferencias en la sensación de hambre y saciedad en un grupo de mujeres con sobrepeso/obesidad en tratamiento tras el consumo de una comida prueba con o sin pan.
Pacientes y métodos: El estudio incluyó a 122 mujeres con IMC ≥ 25 < 40 kg/m2 que fueron randomizadas asignándolas a consumir una de las siguientes comidas prueba: comida NO PAN (2,40 MJ -575 kcal-, 46% hidratos de carbono, 26% proteínas, 28% grasas; que incluía arroz o pasta) y comida PAN (2,39 MJ -571 kcal-, con igual distribución calórica y los mismos alimentos pero con pan en lugar de arroz o pasta). Se empleó una escala analógica visual (Visual Analogue Scale: VAS) de 5 preguntas que debía completarse en diferentes tiempos 1) antes: -1 min; 2) inicio: 0 min; 3) después: 60 min y 4) después: 90 min después de la comida prueba. El test se realizó al inicio del tratamiento y después de 16 semanas de seguir una dieta hipocalórica (con o sin pan), educación nutricional y promoción de actividad física.
Resultados: Completaron el estudio 104 mujeres, edad media 48,4 ± 9 años e IMC basal 29,8 ± 3,5 kg/m2. Al inicio del estudio no existieron diferencias significativas en ninguno de los parámetros valorados por la VAS entre grupos. Al repetir el test tras la intervención el grupo comida PAN obtuvo una puntuación mayor en la pregunta 3 (referida a la sensación de saciedad) que fue significativa en los tiempos 3 (7 vs 5 p < 0,05) y 4 (8 vs 4 p < 0,01).
Conclusiones: La inclusión del pan en una comida hipocalórica podría favorecer una mayor sensación de saciedad tras la comida. Estos resultados entran en contradicción con la recomendación de excluir el pan en un plan de alimentación orientado a la pérdida de peso.
Palabras clave: Obesidad. Sobrepeso. Saciedad. Pan. Índice glucémico. Hambre.
Abbreviations
VAS: Visual Analogue Scale.
GI: Glycemic index.
BMI: Body Mass Index.
WC: Waist circumference.
Introduction
Obesity is one of the major public health problems of the 21st century, affecting more than a thousand million adults worldwide.1 Its prevalence has tripled in many European countries since 1980 and the number of those affected continues to rise. In Europe, the prevalence varies between countries, reaching higher values in eastern and central Europe, from 5% up to 23% in males and from 7% to 36% in women. Currently, obesity is responsible for around 8% of healthcare costs and 10-13% of deaths in various parts of Europe.1,2,3
In Spain, a study performed by the Spanish Society for the Study of Obesity (SEEDO: "by its spanish initials") in 20004 noted that obesity affected 14.5% of the adult population and 38.5% were overweight. According to the results of the DORICA study, the prevalence of obesity was estimated at 15.5% with a higher prevalence among women (17.5%) than men (13.2%).5
For a long time, the increase in bread consumption worldwide has been almost parallel to the growth in world population. However, since the 1960s, there has been a notable and progressive decrease in the consumption of bread worldwide, especially in Spain, placing bread at the tail end of food consumed in Europe.6 People wishing or needing to lose weight are among the lowest consumers of bread. This is because one of the most common mistakes and myths about nutrition is that bread should be limited in diets designed to control weight. Specifically, carbohydrates and foods that contain them are often considered "dangerous" and "caloric" and are often included in the list of forbidden and/or restricted foods by those trying to lose weight. Among these foods, one of the most feared tends to be bread, a food that is negatively rated below that of even sweets and fat, and is also considered by academics as being more dangerous than pastries, sausages, alcohol and fried foods.7,8
There is much controversy regarding the effect of bread on satiety.9,10,11,12 The controversy is based on the association between its effect on satiety and its glycemic index (GI). According to various studies, foods with high glycaemic indexes cause a rapid decline in blood glucose levels, causing the sensation of hunger to appear much sooner and are accompanied by a greater hyperinsulinaemic response.13 However, the satiety mechanism is very complex and other factors should be taken into account such as the time food spends in the stomach, digestibility, volume, degree of cooking, and consistency, just to name a few.
It is also important to note that a food's GI may vary depending on the milling of the grain, the most prominent type of starch (amylase or amylopectin), fibre content and the presence of other nutrients.14 In the case of bread, the glycaemic index varies according to the variety in question (French baguette: 95; gluten-free wheat bread: 90; white flour bread: 90; rye flour bread: 65; rye bread: 50 and oat bread: 47)15 and the manner in which it is prepared.16 This food is rarely consumed in isolation and is often accompanied by other foods, which may also determine its final glycaemic response along with other factors.13
In this study, we wanted to evaluate the evolution of the sensation of hunger, satiety, the desire to eat, wellbeing from eating and amount of food consumed after eating two standard low-calorie meals with bread versus other sources of carbohydrates. We studied these conditions in a group of overweight/obese patients both before and after weight loss treatment. This trial was registered at clinical trials.gov as NCT01223989.
Patients and methods
This was a controlled, prospective, randomised clinical trial in which 122 women older than 18 years and with a BMI greater than 25 and less than 39.9 kg/m2 were randomly placed into 2 groups: an intervention group (BREAD) and a control group (NO BREAD). Both groups received a diet that was lowcalorie (with or without bread) (6.27 MJ -1,500 kcal-), balanced (with a distribution of 55% carbohydrates, 21% proteins and 24% fat of the total caloric value) and based on the consumption of food groups recommended by the Spanish Society of Community Nutrition (SENC, by its Spanish initials)17 adapted for weight loss. The women also received nutrition education and physical activity guidelines, and monitoring continued monthly for 16 weeks.
Subjects were randomly assigned to consume one of the following test meals: NO BREAD meal (2.40 MJ -575 kcal-, 46% carbohydrates, 26% protein, 28% fat; which included grilled chicken, steamed vegetables with oil, rice or pasta and fruit) and BREAD meal (2.39 MJ -571 kcal-, with equal caloric distribution and the same foods except with bread instead of rice or pasta). This method aimed to eliminate the variable effect on satiety produced by other components of the diet or the food preparation methods. The test was carried out at home, and as a prerequisite the participants had to fast for at least 4 hours before the start to eat. Participants could have 500 ml of water along with the meal throughout the entire meal.
A visual analogue scale (VAS) was used to compare the evolution of the sensation of hunger, satiety, the desire to eat, well-being from eating and the amount of food consumed after the test meal assigned.18,19 VAS is composed of 5 questions: 1) how satiety do you feel?; 2) how hunger do you feel?; 3) how strong is your desire to eat?; 4) how pleasure from eating do you feel?; 5) How much food do you think you could eat?. Participants were asked to mark a point on a scale from 0 to 10 cm corresponding to the intensity of the sensation for each of the measured parameters (0 meant "not at all" and 10 meant "very much."). Quantification of the sensations perceived by each person was done by measuring the distance between 0 and the point marked. The questions were answered at different times: 1) just before eating, 2) just after eating and exactly 3) 60 and 4) 90 minutes after eating a test meal.
The test was performed at the start of the low-calorie diet and was repeated at 16 weeks to assess any changes to the results after 16 weeks of monitoring.
With these data, we calculated the median score for each question and for each group (with or without bread) assessing the behaviour of the curves that represented each question on satiety, hunger, desire to eat, pleasure from eating and amount of food able to eat at each of the four times (before: -1 min; start: 0 min; after 60 min and after 90 min).
The study was approved by the Ethics Committee of La Paz University Hospital and conforms to the ethical standards of the Declaration of Helsinki. Written informed consent was obtained from all patients.
Statistical analysis of the data was performed by the Department of Biostatistics at La Paz University Hospital using the SPSS 9.0 (SPSS Inc Chicago, IL, USA) programme. The scale scores are presented as median and interquartile range (IQR: 25-75 percentile) due to being a short-range variable. The quantitative data between two groups are compared using the Student's t test and the U-Mann Whitney test, depending on the data distribution. Values of p < 0.05 were considered significant for all statistical tests.
Results
The total number of women who completed the study and for whom results were submitted was 104. The mean age was 48.4 ± 9.0 years with a mean baseline BMI of 29.8 ± 3.5 kg/m2 of which 56 belonged to the treatment group with BREAD and 48 belonged to the NO BREAD control group. After 16 weeks, both groups had significantly reduced their body weight, body fat, waist circumference and visceral fat and maintained their muscle mass (table I). There were no significant differences in the evolution of anthropometric markers between the groups.
The results for each question, group and time are shown in table II. In the first visit (pre-intervention baseline data), there were no significant differences between the group assigned to the BREAD meal and the group assigned to the NO BREAD meal in any of the VAS parameters at any of the given time points.
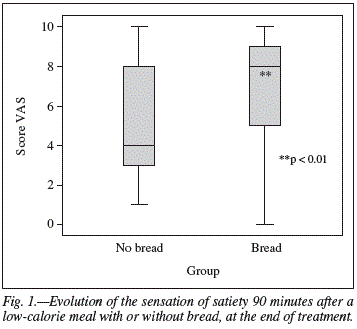
In the last visit, after repeating the test, there were differences in question 3 ("How satiated do you feel right now?"), which were t the limit of significance at time 2 (p = 0.052) and were significant at time 3 (p < 0.05) and at time 4 (p < 0.01). This means that the group that ate the menu with bread felt a greater sense of satiety immediately after eating and at 60 and 90 minutes after eating (fig. 1).
Discussion
The sensation of satiety felt by overweight or obese patients after eating a balanced low-calorie meal is not related to the presence of bread in the diet. There were no differences in the quantification of this sensation as measured by the VAS scale when the supply of carbohydrates came from bread or a different source (for example, rice and pasta) at the start of the study. This sensation was greater in the group that included bread after repeating the test at the end of the intervention.
Similar results were obtained in the study by Wolever et al. (2009) that measured the glycaemic response and the response on satiety following administration of white bread containing 25 or 50 g of carbohydrates. Although the glycaemic levels were observed to be higher for the portion with greater carbohydrate content, the effect on satiety was the same 2 hours after intake.20 This was not observed in the study by Jiménez Cruz et al. (2005), which investigated 4 breakfasts and found that the one containing white bread produced less satiety and greater caloric intake in the following meal. However, this study was conducted with an excessively small number of participants (8 women) and the breakfasts contained different levels of calories, macronutrients and fibre, which brings their methodology into serious question.10 Another study by the same team using patients with diabetes controlled the meals provided but only 10 volunteers participated.9
In the Arumugam et al. (2008) study, the results showed a greater sensation of hunger with greater GI, however, the test was conducted after identical meals with a drink added at breakfast time or with the meal divided into portions.21 The Warren et al study also showed greater hunger with greater GI, since after breakfasts with varying GI there was a greater intake of food at the following meal when the GI was greater. However, the authors recognised the study's limitation in not controlling different proportions of macronutrients and fibre in each of the breakfasts.11
A study by Flint et al. (2004) showed that the GI of a mixed meal calculated theoretically using a table does not predict the actual measured GI, and further showed that carbohydrates do not play an important role in determining the GI of a mixed meal.22 Another study found that after eating a breakfast that included bread, biscuits, cereals and oatmeal the insulin response was associated with postprandial satiety but not with the glycaemic response.23
The Aston et al. (2008) study investigated whether a diet with low GI affected appetite, dietary intake, weight and body composition in overweight and obese subjects. The study added foods rich in carbohydrates with low or high GI (bread, breakfast cereals, rice and pasta or potatoes) to their diets for 12 weeks while attempting to maintain the composition in terms of macronutrients, fibre and energy density. Their energy intake was assessed using a subjective hunger-satiety scale, which did not find any significant differences between both groups. This would show that there is no clear evidence of the positive effects of a low GI diet on satiety and energy intake.24 Alfenas et al. (2005) obtained the same results in a previous study using a similar design.25
A recent review of studies for and against the influence of the GI on appetite, satiety and body composition concluded that most studies that find a positive effect of the GI have a large number of methodological limitations, and that those that are well designed do not find clear benefits of the GI on those parameters. Therefore, GI would have limited application in clinical practice as a measure for improving satiety and reducing appetite.26
The differences observed between the results of the test performed at the start and the test performed after 16 weeks of intervention may be related to various factors. The first time they performed the test, the patients had just started the treatment in the assigned groups (BREAD/NO BREAD). The second time they performed the same test was between weeks 12 and 16, and during that time they followed the guidelines assigned to each group and therefore during that time the adaptation of those guidelines (with or without bread in their diet) may have been modified and reflected at the time of the test. In addition, when they completed the test the second time, both groups had undergone a change in weight and body composition, which is another factor that influences hunger and satiety, while at the start of the study their bodies were in a state of caloric balance. Throughout the intervention the group assigned bread was advised to choose whole wheat bread and the greater supply of fibre provided by this type of bread may have contributed to the greater satiety observed in this group. Finally, another factor that may have influenced the results was a better understanding of the test at the end of the intervention, since it was repeated.
One of the strengths of our study was to evaluate the effect of bread on satiety; in general most studies have had very few participants or have studied the effect using a glucose or insulin test or curve immediately after a meal or a long time afterwards (test are carried out after months of establishing a dietary guideline). In this case, both times were included because a meal was assessed at the start of the intervention, but when the test was repeated the patients had been following the guidelines of their assigned groups for between 12 and 16 weeks. A limitation of the study was that participants prepared their standard meals at home without proper supervision. Nevertheless, they were given very clear guidelines about the foods, their preparation methods, drinking, etc., in order to reduce the differences between the prepared meals as much as possible.
Conclusions
The effect on satiety assessed after eating a lowcalorie meal was no different if the supply of carbohydrates came from bread or any other source (for example, rice and pasta) at the start of the study and was even greater with bread after repeating the test at the end of the intervention. Therefore, the bread inclusion in a meal may result in increased sensation of satiety after eating and could help in the management of weight control.
These results contradict the recommendation to exclude foods such as bread from a food plan aimed at weight loss.
Acknowledgments
We thank the participants in the study and the staff of the Medical Clinical Nutrition and Dietetics Unit at La Paz University Hospital who contributed to its successful completion, and to the Biostatistics Unit of the Hospital La Paz for their assistance with the statistical evaluation of the study.
References
1. World Health Organization. Obesity and overweight. Geneva: 2008. Available at http://www.who.int/dietphysicalactivity/publications/facts/obesity/en [ Links ]
2. World Health Organization. The challenge of obesity in the WHO European Region and the strategies for response. Branca F, Nikogosian H. Lobstein T. ed. Copenague: WHO; 2007. Available at http://www.euro.who.int/_data/assets/pdf_file/0010/74746/E90711.pdf [ Links ]
3. Elmadfa I, Freisling H. Nutritional status in Europe: methods and results. Nutr Rev 2009; 67(Suppl. 1): S130-4. [ Links ]
4. Spanish Society for the Study of Obesity. SEEDO. Consensus on the evaluation of overweight and obesity and establishment of criteria for therapeutic intervention. Med Clin (Barc) 2000; 115: 587-597. [ Links ]
5. Aranceta Bartrina J, Serra Majem LI, Foz Sala M, Moreno Esteban B. Prevalence of obesity in Spain. Med Clin (Barc) 2005; 125:460-466. [ Links ]
6. Serra Majem LI, Raido Quintana B. Bread consumption in the world and in Spain. In Gil Hernandez A, Serra Majem LI (ed). The white bread book; 2010:67-77. Madrid: Médica Panamericana. [ Links ]
7. López Sobaler AM, Ortega RM, Aparicio A, Bermejo LM, Rodríguez Rodríguez E. Concerns about body weight. National study on related mistakes and habits. In: Ortega RM, ed. Nutrition in the females population; 2007: 39-50. Madrid: Ergón. [ Links ]
8. Ortega RM, Requejo AM, Quintas ME, Andrés P, Redondo MR, López AM. Lack of knowledge of the relationship between diet and weight control in a group of university students. Nutr J 2006; 5:11-18. [ Links ]
9. Jiménez Cruz A, Gutiérrez González AN, Bacardi Gascón M. Low glycemic index lunch on satiety in overweight and obese people with type 2 diabetes. Nutr Hosp 2005; 20:348-350. [ Links ]
10. Jiménez Cruz A, Loustaunau López V, Bacardi Gascón M. The use of low glycemic and high satiety index food dishes in Mexico: a low cost approach to prevent and control obesity and diabetes. Nutr Hosp 2006; 21:353-356. [ Links ]
11. Warren JM, Henry CJ, Simonite V. Low glycemic index breakfasts and reduced food intake in preadolescent children. Pediatrics 2003, 112,e414. [ Links ]
12. Holt SH, Brand-Miller JC, Stitt PA. The effects of equal-energy portions of different breads on blood glucose levels, feelings of fullness and subsequent food intake. J Am Diet Assoc 2001; 101: 767-773. [ Links ]
13. Niwano Y, Adachi T, Kashimura J, Sakata T, Sasaki H, Sekine K et al. Is glycemic index of food a feasible predictor of appetite, hunger, and satiety? J Nutr Sci Vitaminol (Tokyo) 2009;55:201-207 [ Links ]
14. Arteaga Llona A. The glycemic index: a current controversy. Nutr Hosp 2006; 21 (Suppl. 2): 55-60. [ Links ]
15. Nutrinfo, the virtual community of Nutrition Professionals. Glycemic Index Tables. Year 2000 Current Version. Available at http://www.nutrinfo.com.ar (Accessed January 2010). [ Links ]
16. Burton P, Lightowler H. Influence of bread volume on glycaemic response and satiety. Br J Nutr 2006; 96: 877-882. [ Links ]
17. Spanish Society of Community Nutrition (SENC). Guide to sensible nutrition. Madrid: Spanish Society of Community Nutrition; 2004. (Available at http://www.aesan.msc.es/AESAN/docs/docs/come_seguro_y_saludable/guia_alimentacion2.pdf [ Links ]
18. Dohm FA, Striegel-Moore RH. The food amount rating scale: development, reliability, and validity. Obes Res 2002; 10: 1173-1179. [ Links ]
19. Parker BA, Sturm K, Macintosh CG, Feinle C, Horowitz M, Chapman IM. Relation between food intake and visual analogue scale ratings of appetite and other sensations in healthy older and young subjects. Eur J Clin Nutr 2004; 58:212-218. [ Links ]
20. Wolever TM, Leung J, Vuksan V, Jenkins AL. Day-to-day variation in glycemic response elicited by white bread is not related to variation in satiety in humans. Appetite 2008; 52:654-658. [ Links ]
21. Arumugam V, Lee JS, Nowak JK, Pohle RJ, Nyrop JE, Leddy JJ et al. A high-glycemic meal pattern elicited increased subjective appetite sensations in overweight and obese women. Appetite 2008;50:215-222. [ Links ]
22. Flint A, Møller BK, Raben A, Pedersen D, Tetens I, Hoist JJ et al. The use of glycaemic I meal. Brit J Nutr 2004; 91:979-989. [ Links ]
23. Flint A, Møller BK, Raben A, Sloth B, Pedersen D, Tetens I, et al. Glycemic and insulinemic responses as determinants of appetite in humans. Am J Clin Nutr 2006; 84:1365-1373. [ Links ]
24. Aston LM, Stokes CS, Jebb SA. No effect of a diet with a reduced glycaemic index on satiety, energy intake and body weight in overweight and obese women. Int J Ohes (Lond) 2008; 32: 160-165. [ Links ]
25. Alfenas RC, Mattes RD. Influence of glycemic index/load on glycemic response, appetite, and food intake in healthy humans. Diabetes Care 2005; 28:2123-2129. [ Links ]
26. Guttierres AP, Altenas Rde C. Effects of glycemic index on energy balance. Arq Bras Endocrinol Metabol 2007; 51: 382-388. [ Links ]
![]() Correspondence:
Correspondence:
Viviana Loria Kohen.
Department of Nutrition.
La Paz University Hospital.
Health Research Institute. IdiPAZ.
Paseo de la Castellana, 261.
28046 Madrid. Spain.
E-mail: vloria@hotmail.com
Recibido: 10-V-2011.
Aceptado: 13-V-2011.