Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Nutrición Hospitalaria
versión On-line ISSN 1699-5198versión impresa ISSN 0212-1611
Nutr. Hosp. vol.27 no.3 Madrid may./jun. 2012
https://dx.doi.org/10.3305/nh.2012.27.3.5730
Assessment of food consumption, energy and protein intake in the meals offered in four Spanish nursing homes
Evaluación del consumo de alimentos, ingesta de proteínas y energía en las comidas ofrecidas en cuatro residencias geriátricas españolas
R. Milà Villarroel1, R. Abellana Sangrà1, L. Padró Massaguer2 and A. Farran Codina2
1Departamento de Salud Pública. Facultad de Medicina. Universidad de Barcelona (UB). Barcelona. España.
2Departamento de Nutrición y Bromatología. Facultad de Farmacia. Universidad de Barcelona (UB). Barcelona. España.
This study was financed by Vegenat S.A. (Badajoz, Spain).
ABSTRACT
Background/objective: The elderly, and especially those attending nursing homes, are at great risk from certain nutritional deficiencies. The aim of this study was to examine the percentage of energy wasted, energy and protein intake and percentage consumed of meal offered by a group of healthy institutionalized elderly in four nursing homes in Spain.
Design and methods: This was a multicentre observational study of a sample of the institutionalized population over the age of 65. Our final sample comprised a total of 62 individuals. Dietary data were collected using double weight method for each meal during 21 days. We calculated the following consumption variables: percentage of food consumed (% food consumed) for each subject in each meal. We also calculated the energy intake (kcal/day), the wasted energy (kcal/day), the protein intake (g protein/ day) and the energy density (kcal/g meal) for each of the meals eaten. To analyse the overall differences we used analysis of variance test (ANOVA). The significance level used was 0.05 (p < 0.05).
Results: The largest meals were lunch (781 g/day [728.4, 833.6]) and dinner (653 g/day [612.1, 693.9]). The percentage of total consumption was 81.9% [79.3, 84.6]. The average energy consumption was 1,575.4 kcal/day [1,508.3, 1,642.6]. The percentage of caloric distribution varied depending on the center. The highest percentage of wasted food was found in the main meals. Forty four percent did not consume enough energy to meet the recommended intakes. Protein intake was 63.6 g protein / day [61.2, 66.1]. 12.5% of women and 4.55% of men did not consume the recommended intakes for the elderly. Breakfast and the bedtime snack had the highest energy density with 1.10 [0.9, 1.25] and 1.04 [0.9, 1.08] kcal/g food served respectively [Energy density].
Discusion/conclusions: The best strategy for increasing the energy intake of the institutionalized elderly without raising the amount of food that is rejected may be to provide higher energy density foods in the same serving sizes.
Key words: Nursing homes. Aged. Diet records. Nutritional requirements.
RESUMEN
Antecedentes/objetivos: Los ancianos, y especialmente los institucionalizados en residencias geriátricas, tiene un elevado riesgo de sufrir deficiencias nutricionales importantes. El objetivo de este estudio fue evaluar el porcentaje de comida consumida en cada ingesta así como la ingesta total energética y proteica en un grupo de ancianos sanos institucionalizados en cuatro residencias geriátricas de España.
Métodos: Se llevó a cabo un estudio observacional multicéntrico en una muestra de población anciana (edad > 65 años) institucionalizada. La muestra final incluyó un total de 62 individuos sanos. Los datos de consumo se evaluaron mediante el método de registro de doble pesada para cada comida durante un período de 21 días consecutivos. Se calcularon las variables: porcentaje de consumo de alimentos (% ración consumida) para cada individuo en cada comida. También se calculó el consumo de energía (kcal/día), la energía desperdiciada (kcal/día), la ingesta de proteínas y la densidad calórica de las comidas (kcal/g ingesta). Para analizar las diferencias se llevó a cabo un análisis de la varianza (ANOVA). El nivel de significación usado fue de 0,05 (p < 0,05).
Resultados: Las comidas más voluminosas fueron el almuerzo (781 g/día) [728,4-833,6] y la cena (653 g/día [612,1-693,9]. El porcentaje de consumo total fue del 81,9% [79,3-84,6]. El consumo de medio de energía fue de 1.575,4 kcal/día [1.508,3-1.642,6]. El porcentaje de distribución calórica varió en función de cada centro. El mayor porcentaje de desperdicio de alimentos fue en las comidas principales (almuerzo y cena). 44% de los ancianos no cubrían las recomendaciones energéticas establecidas. La ingesta de proteínas fue del 63,6 g proteína/día [61,266,1]. Un 12,5% de las mujeres y un 4,55 de los hombres no cubrieron las ingestas recomendadas de proteínas.
Discusión/conclusiones: En vista de los resultados, probablemente una buena estrategia para mejorar el consumo de energía y nutrientes y reducir los porcentajes de comida desperdiciada entre los ancianos institucionalizados podría ser planificar comidas menos voluminosas y con una densidad energética y nutricional más elevada.
Palabras clave: Ancianos institucionalizados. Residencias geriátricas. Registros dietéticos. Requerimientos nutricionales.
Introduction
Population growth in the elderly population in recent years has resulted in increased institutionalization in nursing homes and day centers.12 Despite the importance of feeding for this group, the prevalence of malnutrition remains higher among institutionalized than non-institutionalized elderly.3,4 The elderly are a vulnerable group at great risk of certain nutritional deficiencies and even, in some instances, of severe malnutrition. Several studies have indicated that the institutional diet and pathological and emotional aspects are major risk factors of protein energy malnutrition in this population group.5-7 Some authors suggest that in many cases the energy and protein needs of the institutionalized elderly are not covered,8-12 increasing morbidity and mortality and decreasing quality of life.13-15
There are many reasons for the prevalence of protein energy malnutrition in geriatric homes and hospitals, including decreased appetite due to drug therapy or depressed emotional states with diverse clinical manifestations.16,17 However, certain studies have revealed other important factors such as poor planning of menus and/or high rates of food rejection due to this planning.18-23
One of the most worrying aspects for the institutionalized elderly in nursing homes is their adaptation to the meals that are served. Institutionalized elderly may refuse the food that they are served for several reasons: excessively large portions, fixed mealtimes, unfamiliar dishes, the organoleptic characteristics of the diet, or "therapeutic" diets (with no salt, modified texture or astringent taste).9,22 As a result, nursing homes must seek strategies to improve the nutritional status of the elderly, reduce the amount of food that is rejected, and avoid malnutrition among the residents.
Some of the strategies used to increase residents' energy and protein intake have not been successful. The best strategy for increasing consumption and reducing the amount of food waste has been found to be the use of smaller portions served with greater frequency. However, the catering services and kitchens in many homes cannot implement this strategy properly, due to a lack of resources and trained health personnel.23
However, studies in some nursing homes showed that splitting up the meals throughout the day, serving more frequent, less bulky meals and reducing the amount of food waste did not always increase energy intake, and in some cases even reduced it.24,25 The strategy of splitting meals was only effective if the energy density (ED) of the food portion was increased at the same time as its size was decreased. Several authors have noted the relationship between ED and portion size as a determinant of energy intake. Therefore, the best way to increase energy intake and reduce food waste in nursing homes appears to be to serve smaller portions with higher energy density.26-28
The aim of this study was to examine the percentage of energy wasted, energy and protein intake and percentage of meal consumed by a group of institutionalized elderly in four nursing homes in Spain (in Barcelona, Santa Coloma de Gramenet, Madrid and Bilbao). We also explored the relationship between the energy density of each meal and the total energy and protein consumed by each resident.
Study population and methodology
Study population
This was a multicenter observational study in a sample of institutionalized people over the age of 65. The sample was drawn from four nursing homes in Spain (Barcelona, Madrid, Bilbao and Santa Coloma de Gramanet). A random sample was selected at each nursing home. The maximum number of participants from each centre was fixed at 24, so as not to interfere greatly with mealtimes. The population selected to take part in the study was healthy. The inclusion criteria were as follows: individuals had to be over the age of 65, resident in the center for more than two weeks, capable of receiving food orally and able to feed independently. Elderly people suffering from insulin-dependent diabetes, chronic renal insufficiency, advanced stages of dementia or those taking anorectic drugs were excluded. Our final sample was comprised of a total of 62 healthy subjects (22 men and 40 women) aged between 68 and 96 years.
Methods
Each participant was interviewed to obtain information on their demographic characteristics, toxic habits, diseases and drug treatments. We also asked individuals whether they were given a texture modified diet or if they experienced any swallowing or chewing problems. During the interview, we measured the height and weight of all elderly subjects. Height was recorded using a stadiometer. The subjects stood barefoot in an upright position with their heads aligned in the Frankfort plane. The height of subjects who could not stand up was calculated from the knee-heel distance using the formula proposed by Cockram and Baumgartner.29 The patients were weighed barefoot and dressed in their underwear using medical scales accurate to ± 10 g. The body mass index (BMI) was then calculated from the anthropometric data (kg/m2). The BMI was calculated for each individual, apart from three cases in which calculations were not possible.
All the participants ate in their residences. They were served breakfast, lunch, an afternoon snack and dinner. All meals were taken in common dinning rooms at the time scheduled by each nursing home. Dietary data were collected for each meal during the day, including the food type, the quantity of food served and the amount of plate waste for each of the main meals served. The study was conducted over a three-week (21 day) period, which corresponded to a complete menu cycle at each of the nursing homes. The study carried out with the participation of all the centres and the approval of the protocol of study. All the participants accepted to take part in the study and signed the consent informed.
We used the double weighing method to calculate the size of the food portion that was actually consumed at each meal, as opposed to the size of the food portion served to each patient. This method took into account the amount of food that was edible and non-edible in each meal.30 The amount of food served to the patients on each dish was weighed before they began to eat. When they had finished eating, the plate waste was weighed again. Then, the non-edible portion of the food was weighed to estimate the true weight of the food consumed and served to each individual. The intake of each individual at each of the meals was determined by the following formula:
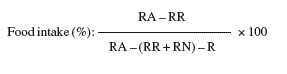
Where:
R: dish weight.
RA: dish weight + food portion served.
RR: dish weight + food portion not consumed.
RN: dish weight + food portion not consumed without non-edible portion.
The task of data collection was performed by a team of dieticians who were specifically trained to carry out the study. Three six-hour sessions were scheduled to outline the study tasks, provide training in the use of computer software and ensure standardized data collection. One dietician was responsible for the management and collection of information at each nursing home.
A computer application was created expressly for the project to record and process food intake data for each subject. To avoid data management errors, the application included a validation system that prevented the introduction of contradictory or obviously erroneous information. The application also incorporated algorithms for calculating the weight of food consumed and discarded by the participants and their respective energy and protein intake. To determine the energy and protein intake for each resident, we developed a computer application in Access Basic and SQL on Access 97 and used the food composition database designed by the Centre for Superior Studies in Nutrition and Dietetics at the University of Barcelona (CESNID).31,32
Energy and protein requirements
The estimated average requirements for energy and protein intake was estimated from the dietary recommendations for older people provided by the Spanish Nutrition Society (SEN).33 Energy requirements were estimated as 30 kcal/kg body weight (bw)/day on average and the protein needs were taken as 0.8 g protein/kg bw/day.
We calculated the following consumption variables: size of the food portion served (g food/day), size of the food portion consumed (g food/day) and the percentage of food consumed (% food consumed) for each subject in each meal. We also calculated the energy intake (kcal/day), the wasted energy (kcal/day), the protein intake (g protein/day) and the energy density (kcal/g food) for each of the meals eaten throughout the day (breakfast, lunch, afternoon tea, dinner and bedtime snack) at each centre. The values for each variable (amount of food consumed and discarded, energy intake and intake of protein) were obtained as the mean of the 21 day (menu cycle around 3 weeks).
Statistical analysis
The characteristics of the study population were compared by the Student's t-test and the 2 test. The variables of food intake, energy, energy density and protein intake had a normal distribution (Kolmogorov and Shapiro-Wilk test of normality was > 0.05) and the results were expressed as the mean and confidence interval 95% (Cl 95%). To make comparisons, the Student's t-test was used for the gender variable. Analysis of variance (ANOVA) was used for comparisons among centers. The significance level used was 0.05 (p < 0.05). The data were analyzed using SPSS v.16.0 (2008, SPSS, Inc, Chicago, IL).
Results
Population
We analyzed the food intake of 62 heathy residents (22 men and 40 women) over the age of 65 in four geriatric centers in Spain (Barcelona, Madrid, Bilbao and Santa Coloma de Gramanet). There were no significant differences between the BMI of men (27.2 kg/m2 [CI 95%:25.5, 29.0]) and women (27.3 kg/m2 [CI 95%:25.92, 28.61]). According to BMI values, 24,4% (n = 16) of elderly people was established underweight (BMI less than 21 kg/m2), 47,6% (n = 29) presented a correct weight (BMI between 21 and 27,9 kg/m2) and 28% (n = 17) were overweight (BMI > 27,9 kg/m2). Among the elderly with low weight, were detected 6 elders with a BMI less than 18,5 kg/m2. The most common diseases in the resident population were hypertension, with a prevalence of 40.2% (21.4% in men and 50% in women, χ2 p = 0.012) and hyperlipidemia with 23.2% prevalence (17.9% in men and 25.9% in women, χ2 p = 0.412).
Consumption variables: portions served and percentage of consumption
The data from this study showed that the largest meals were lunch (781 g/day [CI 95%:728.4, 833.6]) and dinner (653 g/day [CI 95%:612.1, 693.9]). Men and women were served very similar food portions, with no significant differences in any of the meals eaten throughout the day. There was wide variability between centers in the amount of food served. Subsequent statistical tests showed significant differences between all centers for all meals (data not show). One center (Madrid) served a bedtime snack, made up of an average of 198.8 g of food/day [CI 95%:187.5, 209.9].
The percentage of total consumption was 85.5% [CI 95%:83.6, 87.5], but there were significant differences between meals, as described below. The rate of consumption was 88.8% [CI 95%:85.7, 91.9] for men and 85.5% [CI 95%:83.3, 87.8] for women. There were no significant gender differences in consumption, except in lunch (83.8% [CI 95%:79.4, 88.3] for men vs. 76.8% for women [CI 95%:73.3, 80.3], F = 5.853, p = 0.018) and dinner (86.5% [CI 95%:82.9, 90.1] for men vs. 81.0% for women [CI 95%:77.6, 84.4], F = 4.272, p = 0.042), at which men consumed more of their portions. As can be seen in figure 1, the percentage of consumption varied at each meal of the day and also depended on the nursing home. The afternoon snack had the highest percentage consumption (91% [CI 95%:84.9, 97.1], F = 5.879, p < 0.001). The percentage consumption values for the other meals were: 89.5% [CI 95%:86.6, 92.5] (F = 16.904, p < 0.001) for breakfast, 82.9% [CI 95%:80.3, 85.4] (F = 4.468 p = 0.001) for dinner and 79.2% [CI 95%:76.4 and 82.1] (F = 15.026, p < 0.001) for lunch. The Bilbao center had the lowest consumption rate for all meals. Madrid center offered a bedtime snack, with consumption rates of 100% in all cases.
Energy consumption
The average energy consumption was 1,665 kcal/ day [CI 95%:1,595.4, 1,736.4]. By sex, the average consumption was 1,790 kcal/day [CI 95%: 1,659.8, 1,921.6] for men and 1,601 kcal/day [CI 95%: 1,520.8, 1,681.8] (t = 6.906, p = 0.010) for women. Residents of the Bilbao nursing home had the lowest energy intake (1,402 kcal/day [CI 95%: 1,298.6, 1,506.8]) and residents of the Madrid center had the highest energy intake (1,731.9 kcal/day [CI 95%: 1,647.8, 1,816.1]). The percentage of caloric distribution varied greatly depending on the center, although all centers provided the bulk of the energy at lunch and dinner. On average, lunch provided 591 kcal/day [CI 95%: 568.2, 621.9] and dinner contributed 512 kcal/day [CI 95%: 487.2, 537.3] (fig. 2). The highest percentage of wasted food, and consequently the greatest loss of energy, was found in the main meals. The average amount of energy that was wasted was 314 kcal/day [CI 95%: 268.5, 359.3] (fig. 3). There were no significant differences between men and women.
Forty-four per cent of subjects (55% of women and 32% of men) did not consume enough energy to meet the estimated energy requirement of 30 kcal/kg bw/day34 (fig. 4). In some cases, this percentage was higher. For example, in the Bilbao center, 81% of participants did not consume enough energy. There were significant differences between participants who met or not met the requirements; the average energy consumed by individuals who met the requirements was 1,851 kcal/day [CI 95%: 1,761.1, 1,942.7]; in other hand, participants who did not meet with the minimum requirement consumed 1,408.8 kcal/day [CI 95%: 1,346.9, 1,470.8] (t = 7.781, p < 0.001) on average. There were no significant differences between men and women in relation to the average energy consumed and whether or not the needs were met.
Protein intake
The average protein consumption among residents was 63.6 g protein/day [CI 95%: 61.2, 66.1]. The protein intake was statistically higher for men (68.8 g protein/day [CI 95%: 64.5, 73.1]) than for women (60.9 g protein/day [CI 95%: 58.2, 63.6], t = 3.287, p = 0.002). As in the case of energy intake, protein intake was highest at lunch and dinner. In the Barcelona center, the protein intake at breakfast was unusually high (21.4 g protein/breakfast [CI 95%: 18.1, 24.9]) in comparison with other centers. In relation to individual needs (EAR established as 0.8 g protein/kg bw/day), 12.5% of women and 4.55% of men did not consume the recommended amount for the elderly (fig. 4). The average protein consumption among individuals who met the protein requirements was 65.6 [CI 95%: 63.1, 68.1] g protein/day, compared to 52.7 [CI 95%: 46.7, 58.8] g of protein per day for those who did not meet the established minimum requirements (t = 3.914, p < 0.001). There were no significant differences between men and women in relation to whether or not their average protein intake was sufficient.
Energy density
Of all the meals, breakfast and the bedtime snack had the highest energy density with 1.10 [CI 95%: 0.9, 1.25] and 1.04 [CI 95%: 0.9, 1.08] kcal/g food served respectively. In general, the energy density of foods varied considerably according to the centers, and we found significant differences in all meals. At all centres the food groups with the highest energy density (i.e., fats and sauces and pastries and sweets) were those that contributed most energy to the total calorie count (data not shown).
Discussion
Few studies have used a double weighing method to analyze the amount of food rejected by residents in nursing homes, probably because this kind of research is labor-intensive and requires qualified personnel. However, it is very important to establish the amount of food that is consumed in homes, as it is a good indicator of how well menus are accepted and of the real consumption of energy and nutrients in a group that is particularly vulnerable to nutritional deficits. Although the menus in nursing homes are well planned, a high percentage of wasted food means that the established minimum recommendations are not likely to be met. In this study, the overall average food rejection rate was 13.8% (11.5% in men and 14.9% in women). These values are similar to that obtained in an Australian nursing home by Grieger et al.,35 but not to those recorded by Barton et al.,36 who found a rejection rate of 30 to 42%. It should be noted that these studies were carried out in hospitals where the health status of patients could be an important variable that influences the consumption of the menus, rather than the menus themselves. In our study, the amount of uneaten food accounted for a loss of 300 kcal/day/individual, which is close to the figure of 400 kcal/day/person found in a Finnish nursing home37 or that of 270 kcal/day/person in a residence in Sweden.28 However, these results differ significantly from the 600 kcal/day/individual observed in an Australian residence.35 This discrepancy in the results could be due to the fact that the study of the Australian residence only measured the amount of food refused in one day, while our study assessed the amount of food refused over 21 days, the Finnish study analyzed 14 days and the Swedish study 15 days.
The highest food rejection rates were found at lunch and dinner in all centers, with 20% and 15% of the total meals served being rejected. This represents approximately 240 kcal/day that were not consumed. In some cases, these percentages were much higher. For example in the Bilbao center, rejection rates at breakfast, lunch and the snack reached almost 30%. There was also particular concern over the lunch rejection rate at the Santa Coloma de Gramanet center (29.9%). Among the non-main meals (breakfast, afternoon snack and the bedtime snack), the rejection percentages were lower (12%, 9% and 0% respectively) and represented a total of 57 kcal/day. The low percentages of rejection of snacks match the values found by Grieger et al., although these authors recorded higher percentages of rejection at dinner.35 The results seem to confirm that large portions lead to greater rejection by nursing home residents, as noted by Cluskey et al.24,25
The average energy consumption was 1,665 kcal/ day. Suominem et al.37 and Gieger et al.35 found lower average consumption values of about 1,200 and 1,580 kcal/day. In the centers that participated in the study, the menus were planned to cover the energy needs of all residents.38 However, failure to consume all of the food or smaller servings than planned led to a lower energy intake that did not meet the recommended requirements. Most of the energy consumed came from the main meals: 32% (591 kcal/day) for lunch and 28% (512 kcal/day) for dinner. The rest of the energy was provided by breakfast (19.8%), snacks (7.4%) and the bedtime snack (12.4%) (fig. 2). Fifty-one per cent of individuals (39% of men and 57.4% of females) consumed less energy than required according to their age, body weight and physical activity level. These results indicate that greater attention should be paid to menu planning and to the use of the menus by the institutionalized elderly, as indicated in similar studies.20,24-35
Protein intake was 63.6 g/day. In this case, 86.2% of individuals (92.9% men and 82.7 for women) met the recommendations of 0.8 g protein/kg bw/day proposed by the SEN.34 Both men and women consumed, on average, about 1 g protein/kg bw/day, which is equivalent to a daily consumption of 68.8 and 60.9 g protein/ day, respectively. The values of protein intake in our study were close to those obtained in other studies of institutionalized elderly populations.27,35 However, the ratio of animal protein/ vegetable protein could be improved, since most of the protein in the diets was of animal origin (72% vs. 28% protein of vegetable origin), from sources such as meat and dairy products in particular, 39% and 21% of the total protein respectively (data not showed).
The energy density of food (kcal/g food) is a relevant factor but has been little studied. The energy intake at each meal was closely related to its energy density. In most cases, we observed that a lower volume of food and a higher energy density not only increased energy intake, but also reduced the volume of food rejected. This may be due to the smaller volume of food offered, which is sometimes a limiting factor for consumption among the elderly.9,22 In addition, non-main meals (breakfast, afternoon snack and the bedtime snack) made a considerable contribution to the energy intake, as they provided 645.28 kcal/day,which is almost 40% of the total calories and 29% of the total food consumed. Experimental studies conducted in other nursing homes found that rich menus with smaller portion sizes were more readily accepted by residents, as were menus that increased the energy intake by 300 kcal/person/day26,27 and 500 kcal/person/day.28 It's is very interesting because this non-main meals can improve the ratio between energy consumed and % of food wasted.
Conclusions
The best strategy for increasing the energy intake of the institutionalized elderly without raising the amount of food that is rejected may be to provide higher energy density foods in the same serving sizes. In nursing home kitchens, meals could be enriched with high-energy foods (milk powder, egg yolk and grated cheese) without increasing the volume. This method can be easy to implement. It can be used for prolonged periods and with all kinds of food, at very little additional cost. In conclusion, increasing the energy density of foods and reducing the size of portions may decrease the amount of food that is rejected and improve the energy and protein intake of the institutionalized elderly.
Acknowledgement
The authors acknowledge the valuable assistance provided for data collection by Laura Álvarez, Maria Álvarez and Amaia Gereikz.
References
1. Abellán A, Fernández-Mayoralas G, Rodríguez V, Rojo F. Envejecer en España. Manual estadístico sobre el envejecimiento de la población. Madrid: Fundación Caja Madrid; 1996. [ Links ]
2. Ministerio de Trabajo y Asuntos Sociales ICEdlPM. II Congreso Estatal de Personas Mayores. Ministerio de Trabajo y Asuntos Sociales, Imserso, 2001. [ Links ]
3. Ramon JM, Subira C. Prevalence of malnutrition in the elderly Spanish population. Med Clin (Barc) 2001; 117 (20): 766-70. [ Links ]
4. Cuervo M, Garcia A, Ansorena D, Sanchez Villegas A, Martínez González M, Astiasaran I et al. Nutritional assessment interpretation on 22,007 Spanish community-dwelling elders throught the Mini Nutritional Assessement test. Pub Health Nutr 2009; 12: 82-90. [ Links ]
5. Ramos A, Luna R, González J, Hernando M, Kazemzadeh A, Martínez Cañavante MJ et al. Malnutrición en un servicio de medicina interna: influencia de los pacientes procedentes de residencias de ancianos. An Med Intern (Madrid) 2000; 17:347-50. [ Links ]
6. Esteban M, Fernández J, Salas J. Estado nutricional de la población anciana en función del régimen de institucionalización. Nutr Hosp 2000; 15 (2): 105-13. [ Links ]
7. Roberts SB, Rosenberg I. The anorexia of aging. Dig Dis 2007; 25: 129-137. [ Links ]
8. Lengyel CO, Whiting SJ, Zello GA. Nutrient adequacies among elderly residents of long term care facilities. Can J Diet Pract Res 2008; 69 (2): 82-8. [ Links ]
9. Bourdel-Marchasson I, Rolland C, Jutand MA, Egea C, Baratchart B, Barberger-Gateau P Undernutrition in geriatric institutions in South-West France: policies and risk factors. Nutrition 2009; 25 (2): 155-64. [ Links ]
10. Akner G, Floistrup H. Individual assessment of intake of energy, nutrients and water in 54 elderly multidiseased nursing home residents. J Nutr Health Aging 2004; 7: 1-12. [ Links ]
11. Lammes E, Akner G. Repeated assessment of energy and nutrient intake in 52 nursing home residents. J Nutr Health Aging 2006; 10 (3): 222-30. [ Links ]
12. Portillo M, Guijarro J, Martín M, Rozas E, Abecia C. Estimación del aporte energético y nutritivo de las dietas en una residencia de ancianos del País Vasco. Nutrición Clínica 1996; XVI/71 (2): 29-38. [ Links ]
13. Sahyoun NR, Serdula MK, Galuska DA, Zhang XL, Pamuk ER. The epidemiology of recent involuntary weight loss in the United States population. J Nutr Health Aging 2004; 8: 510-7. [ Links ]
14. Sullivan DH. The role of nutrition in increased morbidity and mortality. Clin Geriatr Med 1995; 11: 6661-74. [ Links ]
15. Correia MI, Waitzberg DL. The impact of malnutrition on morbidity, mortality, length of hospital stay and costs evaluated through a multivariate model analysis. Clin Nutr 2003; 22: 235-9. [ Links ]
16. Nieuwenhuizen WF, Weenen H, Rigby P, Hetherington MM. Older adults and patients in need of nutritional support: Review of current treatment options and factors influencing nutritional intake. Clin Nutr 2010; 29 (2): 160-9. [ Links ]
17. Mowé M, Bohmer T. Reduced appetite. A predictor for under-nutrition in aged people. J Nutr Helath Aging 2002; 6: 81-3. [ Links ]
18. Portillo M, Guijarro J, Martín M, Rozas E, Abecia C. Estimación del aporte energético y nutritivo de las dietas en una residencia de ancianos del País Vasco. Nutrición Clínica 1996; XVI/71 (2): 29-38. [ Links ]
19. Pérez R, Moreno N, Tuells J. Estimación del aporte energético y nutritivo de los menús ofertados en las residencias de tercera edad existentes en el área del Baix Vinalopó (Elche). Nutrición Clínica 2000; XX/155 (4): 21-9. [ Links ]
20. Nowson CA, Sherwin AJ, McPhee JG, Wark JD, Flicker L. Energy, protein, calcium, vitamin D and fiber intakes from meals in residential care establishments in Australia. Asia Pac J Clin Nutr 12: 172-7. [ Links ]
21. Guillén N, Torrentó M, Alvadalejo R, Salas-Salvadó J. Evaluación de la aceptación de los menús servidos en el Hospital Universitari de Sant Joan de Reus. Nutr Hosp 2004; 19: 277-280. [ Links ]
22. Gimeno JA, Gracia M, Bosque P, Poned B, Arnal JA. Control de calidad de las dietas generales servidas en un hospital comarcal. Nutr Hosp 1998; 13: 312-315. [ Links ]
23. Sánchez-Campillo M, Torralba C, López MA, Zamora S, Pérez-Llamas F. Estrategias para mejorar el valor nutricional de los menús ofertados en residencias públicas para personas mayores. Nutr Hosp 2010; 25: 1014-1019. [ Links ]
24. Cluskey M, Kim YK. Use and perceived effectiveness of strategies for enhancing food and nutrient intakes among elderly persons in long-term care. J Am Diet Assoc 2001; 101 (1): 111-4. [ Links ]
25. Cluskey M, Dunton N. Serving meals of reduced portion size did not improve appetite among elderly in a personal-care section of a long-term-care community. J Am Diet Assoc 1999; 99 (6): 733-5. [ Links ]
26. Gall MJ, Grimble GK, Reeve NJ, Thomas SJ. Effect of providing fortified meals and between-meal snaks on energy and protein intake of hospital patients. Clin Nutr 1998; 17 (6): 259-264. [ Links ]
27. Barton AD, Beigg CL, Macdonald IA, Allison SP. A recipe for improving food intakes in elderly hospitalized patients. Clin Nutr 2000; 19 (6): 451-454. [ Links ]
28. Ödlund Olin A, Aremyr I, Soop M, Jerström S, Classon I, Cederholm T et al. Energy dense meals improve energy intake in elderly residents in a nursing home. Clin Nutr 2003; 22 (2):125-131. [ Links ]
29. Cockram D, Baumgartner R. Evaluation of accuracy and reliability of caliper for measuring recumbent knee height in elderly people. Am J Clin Nutr 1990; 52: 397-400. [ Links ]
30. Block G. A review of validations of dietary assessment methods. Am J Epidemiol 1982; 115 (4): 492-505. [ Links ]
31. Farran A, Zamora R, Cervera P i (CESNID) CdESdNiD (2004). Tablas de composición de alimentos del CESNID. Barcelona: McGraw-Hill/Interamericana de España, S.A.U. Edicions Universitat de Barcelona. [ Links ]
32. Farran Codina A. Desarrollo y aplicación de un sistema de información para la elaboración de tablas de composición de alimentos [Tesis Doctoral]. Barcelona; Universidad de Barcelona; 2004. [ Links ]
33. Arbonés G, Carvajal A, Gonzalvo B, González-Gross M, Joyanes M, Marques-Lopes I et al. Nutrición y recomendaciones dietéticas para personas mayores. Grupo de trabajo "Salud Pública" de la Sociedad Española de Nutrición (SEN). Nutr Hosp 2003; 18 (3): 109-37. [ Links ]
34. Grieger JA, Nowson CA. Nutrient intake and plate waste from an Australian residential care facility. Eur J Clin Nutr 2007; 61:655-63. [ Links ]
35. Barton AD, Beigg CL, Macdonald IA, Allison SP. High food wastage and low nutricional intakes in hospital patients. Clin Nutr 2000; 19 (6): 445-49. [ Links ]
36. Suominem M, Laine T, Routasalo P, Pitkala KH, Rasanen L. Nutrient content of served food, nutrient intake and nutritional status of residents with dementia in a finnish nursing home. J Nutr Health Aging 2004; 8 (4): 234-8. [ Links ]
37. Milà R, Abellana R, Farran A. Nutritional assessment of the menus in five geriatric homes and their adaptation to the recomended intakes for the elderly population. Actividad Dietética 2009; 13 (02): 51-8. [ Links ]
![]() Correspondence:
Correspondence:
Raimon Milà Villarroel.
Dept. Salud Pública.
Facultad Medicina.
Hospital Clínic Barcelona.
C/ Casanova, 143.
08036 Barcelona. España.
E-mail: rmila@ub.edu
Recibido: 10-I-2012.
1.a Revisión: 11-I-2012.
Aceptado: 30-I-2012.














