My SciELO
Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO -
 Access statistics
Access statistics
Related links
-
 Cited by Google
Cited by Google -
 Similars in
SciELO
Similars in
SciELO -
 Similars in Google
Similars in Google
Share
Nutrición Hospitalaria
On-line version ISSN 1699-5198Print version ISSN 0212-1611
Nutr. Hosp. vol.29 n.2 Madrid Feb. 2014
https://dx.doi.org/10.3305/nh.2014.29.2.7127
ORIGINAL / Nutrición enteral
Ultrasound-guided percutaneous "push-introducer" gastrostomy is a valuable method for accessing the gastrointestinal tract
La gastrostomía percutánea por ultrasonido "push-introducer" es un método válido para acceder al tracto gastrointestinal
Stanislaw Klek1, Adam Hermanowicz2, Jerzy Salowka1, Tomasz Cegielny1, Konrad Matysiak3, Michael Chourdakis4 and Piotr Szybinski1
1Stanley Dudrick's Memorial Hospital. General and Oncology Surgery Unit. Skawina. Poland.
2Department of Pediatric Surgery. Medical University of Bialystok. Poland.
3Chair of General. Gastroenterology and Oncology and Plastic Surgery. Medical University of Poznan. Poland.
4School of Medicine. Aristotle University of Thessaloniki. Greece.
ABSTRACT
Percutaneous endoscopic gastrostomy (PEG) is the mosteffective and least invasive method for enteral nutrition (EN). The most common system for PEG is the 'pull' technique, which. It is not available in case endoscopy cannot be performed. The 'push' technique may be an option if effective identification of the abdominal structures can be achieved. X-ray or ultrasonography can be used for that purpose. The aim was to assess the clinical value of ultrasound-guided 'push' gastrostomy. A retrospective analysis of eleven patients (6 F, 5 M, mean age 65.1) including the procedure itself, complication rate, and cost was conducted. In all eleven patients the surgery was successful, and EN was introduced 4-6 hours afterwards. Complications included pain requiring removal of a supporting stitch (n = 1) and balloon deflation (n = 1). All patients were successfully fed enterally. Ultrasound-guided 'push' technique gastrostomy should become a method of choice if the 'pull' method is unavailable.
Key words: Ultrasound. Percutaneous gastrostomy. PEG. Enteral nutrition.
RESUMEN
La gastrostomía endoscópica percutánea (GEP) es el método más eficaz y menos invasivo para la nutrición enteral (NE). El sistema más frecuente para la GEP es la técnica 'pull', que no está disponible en el caso de que la endoscopia no se pueda realizar. La técnica 'push' puede ser una opción si se consigue una identificación efectiva de las estructuras abdominales. Para este propósito, se pueden usar los rayos X o la ecografía. El objetivo fue evaluar la validez clínica de la gastrostomía 'push' guiada por ecografía. Se realizó un análisis retrospectivo en 11 pacientes (6 M, 5 H, edad media 65,1) que incluía el propio procedimiento, la tasa de complicaciones y el coste. En los 11 pacientes la cirugía fue exitosa y la NE se introdujo a las 4-6 horas. Las complicaciones incluían dolor, que requirió la retirada del punto de soporte (n = 1), y el deshinchado del globo (n = 1). A todos los pacientes se les alimentó con éxito entéricamente. La técnica de gastrostomía 'push' guiada por ecografía debería convertirse en el método de elección cuando la técnica 'pull' no esté disponible.
Palabras clave: Ultrasonido. Gastrostomía percutánea. GEP. Nutrición enteral.
Introduction
Enteral nutrition should be administered when oral feeding is impossible, contraindicated or insufficient and the gastrointestinal tract is accessible and functional.1,2. The general rule is to obtain maximum safety and comfort for the patient using the wide range of equipment available3. Percutaneous endoscopic gastrostomy (PEG) has become a method of choice for enteral nutrition (EN) in all age groups since its introduction in 19804. This technique should be considered if enteral feeding is necessary for >3-4 weeks3.
Tube placement is usually performed in the endoscopic suite or at the bedside using intravenous conscious sedation and local anesthesia. Those techniques include percutaneous endoscopy gastrostomy (PEG) or PEG-jejunostomy (PEG-J) as well as direct percutaneous jejunostomy (D-PEJ). Several PEG placement techniques can be used, but the most common is the pull procedure originally described by Gauderer and Ponsky4. In cases that present technical difficulties, such as the impossibility of a safe passage through the esophagus because of a tumor, infiltration or stenosis, resulting in a lack of transillumination, PEG placement is impossible and even dangerous. Similar problems may occur with endoscopic gastric distension or endoscopically visible focal finger invagination3. In those cases, surgical gastrostomy, which is an invasive procedure, is often the only option for enteral access. However, less invasive measures would be preferable.
The so-called 'push' variant for gastrostomy placement requires only the distension of the stomach, without the need for transillumination. The former can be obtained by gas insufflation or filling with fluid, such as water or a contrast agent. In those cases, the feeding tube is placed over a Seldinger wire or using the 'introducer' and peel-away cannula. The procedure must be conducted under radiologic or sonographic guidance. 'Push' methods are used relatively rarely because they pose a much greater risk of failure or complications.
The aim of this study was to analyze whether ultrasound-guided gastrostomy tube placement can be a safe and effective method for EN in patients in whom conventional PEG placement is impossible, provided that it is performed carefully.
Materials and method
A retrospective analysis of eleven patients (6 F, 5 M, mean age 65.1), treated at surgical centers in Bialystok, Poznan and Skawina in Poland, was performed.
The main inclusion criteria were the indication for enteral nutrition and the inability to perform routine PEG placement (established by failed attempt to perform endoscopy). In all patients, the gastrointestinal tract was functional, and it was possible to access the stomach percutaneously via a thin nasogastric tube.
The nutritional status was assessed with Nutritional Risk Screening 2002 (NRS 2002) and Subjective Global Assessment (SGA). Both scales are obligatory in Polish hospitals.
The primary diseases were as follows: esophageal cancer (n = 6), head and neck cancer (n = 2), stenosis of the esophagus after chemical damage (n = 2), and sarcoma of the neck (n = 1).
Informed consent for the surgical procedure, the medical and nutritional treatment and the use of photographs was obtained from all of the patients or their legal caregiver(s). Approval from the Institutional Ethics Committee of hospital in Skawina was obtained, and the study was conducted following the World Medical Association Declaration of Helsinki.
Technique
The tube insertion was performed under general and local anesthesia after the placement of a thin (10 Cherrier, Flocare, Nutricia Polska Ltd., Poland) nasogastric tube. A single dose of an intravenous antibiotic was administered 30 minutes before the operation. The patient was placed in a supine position.
The stomach was filled with 1000 ml of water via the fine-bore (10 Cherrier) nasogastric tube, and an ultrasound scan was performed with a 7.5 MHz probe GE Logiq 5 and Voluson E8 (General Electric (GE) Healthcare, UK/USA). The stomach was located, and its location below the abdominal wall was confirmed. (Figs. 1 and 2) If there was not a clear contact between the abdominal and gastric walls, an additional 500 ml of water was infused. After the confirmation of the contact, a Freka Pexact (Fresenius Kabi, Germany) gastrostomy set was used to perform the procedure.
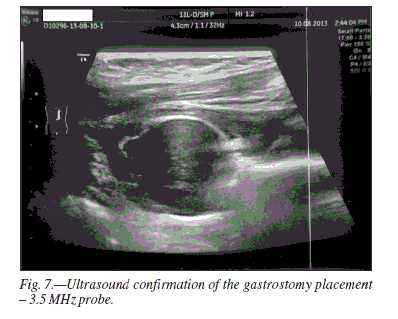
After sterilizing the skin, the anterior abdominal wall was punctured with two double needles with polyvinyl thread, and the gastropexy sutures were created (Figs. 3 and 4]). The abdominal wall was punctured with peel-away cannula, and a 15 Ch balloon gastrostomy catheter was inserted (Fig. 5). When the water began to flow through the gastrostomy, the balloon was filled with 10 ml of water. The placement of the gastrostomy tube was then confirmed with ultrasonography (Fig. 6).
Results
The gastrostomy placement was successful in all patients. The mean duration of the procedure was 7.5 minutes (5.5-14.4). The administration of enteral nutrition commenced after 4-6 hours with a standard isocaloric diet.
Complications were observed in 2 (18%) of the patients. These were minor technical complications that included the following:
- Deflation of the catheter's balloon, requiring reinsertion of a new balloon catheter (the reinsertion was uncomplicated)
- Postoperative pain, resulting in the removal of one of the gastropexy sutures after 3 days. The pain was the result of the contact between the left lower rib's periosteum and the suture and abated immediately following the suture's removal.
No postoperative complications were observed in the remainder of the patients. The mean duration of hospital stay was 2.5 day [range: 2-5]. All of the patients were discharged from the hospital and successfully fed afterwards using bolus methods at long-term facilities. The follow-up for 6 months did not reveal any complications. The nutritional status of the patients improved significantly after treatment.
The cost of the procedure was calculated as the cost of the hospital stay plus the cost of the procedure, which was approximately 700 EURO.
Discussion
Tube feeding is the method of choice when enteral nutrition is recommended and an oral diet cannot be administered due to the dysfunction of the upper gastrointestinal tract1. PEG placement should always be considered a 'gold standard', as it is a safe procedure that is minimally invasive with a very low rate of complications3,5-7. The safe placement of a PEG tube, however, requires successful gastroscopy, the location of the puncture site and the transillumination of the stomach through the abdominal wall3. Impaired coagulation, severe ascites, peritonitis, local esophageal or general gastrointestinal obstruction are considered to be absolute contraindications3,4,8. Ascites, peritoneal dialyses, obesity, enlargement of the spleen and/or liver and distorted anatomy are considered to be relative contraindications8-10.
Major complications related to PEG are colonic perforation, esophageal tears, small bowel injury, liver or splenic injury, tube migration with or without intestinal obstruction, gastrointestinal bleeding and site or generalized infection. These complications have been reported with variable incidence (5% to 17%) in published series3-5,11,12. Predisposing factors include anatomic anomalies in up to 50% of cases3. Patients, in whom the transverse colon lies anterior to the stomach are predisposed to colonic injury during a PEG procedure3,11.
Transillumination during endoscopy ensures a safe PEG placement and the avoidance of the above-mentioned complications, but it is impossible when an endoscopy cannot be performed. Historically, those patients only qualify for traditional surgery. With the introduction of the 'push' technique for tube placement, many patients in whom there is no endoscopic access to the stomach may be able to avoid the surgery that was previously their only option.
The other may qualify for a less invasive procedure, which is the percutaneous gastrostomy with the 'push' technique enhanced by an introducer. This method requires insufflation of the stomach and either radiologic or ultrasound guidance. The latter is more feasible because it does not require a contrast agent or an X-ray. Although the ultrasound-guided introducer procedure has been known for many years, it has not been implemented into everyday practice.
The aim of our study was to analyze whether ultrasound-guided gastrostomy tube placement can be a safe and effective method for enteral nutrition in patients in whom PEG placement is impossible. It was proven to be effective in all of the patients who were unable to undergo the standard placement. The complications after the procedure can be described as minor and manageable, which emphasizes the efficacy of the method. The complication rate was comparable to or lower than the complication rate described by other authors3,4,8,11,12.
The minor complications that were observed in our study have also been described by other authors, who even observed them in 50% of their patients3,4,10,13,14. In our series- the number of postoperative complications reached only 18.1% and were easily managed. Moreover- the cost of the procedure was relatively low- approximately 700 EURO- showing that the method is also cost-effective.
Conclusions
The ultrasound-guided 'push-introducer' gastrostomy technique should be recommended over open surgical techniques when the 'pull' method of PEG placement is unavailable and enteral nutrition is necessary. It represents a clinically effective and valuable option.
Conflicts of interest
None declared.
Statement of authorship
All authors state that they have made substantial contributions to the study and that they give their approval to the final version of the manuscript.
Acknowledgements
Stanislaw Klek was the coordinator of the trial. He was responsible for the conception and contributed to the experimental design, data interpretation and writing of the manuscript. All authors critically revised the intellectual content of the study and contributed to the writing of the manuscript, the data and statistical analysis and the data collection.
References
1. Arends J, Bodoky G, Bozzetti F, Fearson K, Muscaritoli M, Selga G, van Bokhorstde van der Schueren MAE, von Meyenfeldt M, Zürcher G, Fietkau R, Aulbert E, Frick B, Holm M, Berger SA, Zarling EJ. Colocutaneous fistula following migration of PEG tube. Gastrointest Endosc 1991; 37: 86-8. [ Links ]
2. Weimann A, Braga M, Harsanyi L, Laviano A, Ljungqvist O, Soeters P, DGEM (German Society for Nutritional Medicine), Jauch KW, Kemen M, Hiesmayr JM, Horbach T, Kuse ER, Vestweber KH, ESPEN (European Society for Parenteral and Enteral Nutrition). ESPEN Guidelines on Enteral Nutrition: Surgery including organ transplantation. Clin Nutr 2006; 25 (2): 224-44. [ Links ]
3. Sobotka L, et al. Basics in Clinical Nutrition. Galen, 2007. [ Links ]
4. Gauderer MW, Ponsky JL, Izant R Jr. Gastrostomy without laparotomy: a percutaneous endoscopic technique. J Pediatr Surg 1980; 15: 872-5. [ Links ]
5. Baere de T, Chapot R, Kuoch V, Chevallier P, Dellile JP, Domenge C, Schwaab G, Roche A. Percutaneous gastrostomy with fluoroscopic guidance: single-center experience in 500 consecutive cancer patients. Radiology 1999; 210: 651-4. [ Links ]
6. Bleck JS, Reiss B, Gebel M, Wagner S, Strassburg CP, Meier PN, Boozari B, Schneider A, Caselitz M, Westhoff-Bleck M, Manns M. Percutaneous sonographic gastrostomy: method, indications, and problems. Am J Gastroenterol 1998; 93: 941-5. [ Links ]
7. Lorentzen T, Skyoldbye B, Nolsoe C, Torp-Pedersen S, Mygnid T. Percutaneous gastrostomy guided by ultrasound and fluoroscopy. Acta Radiol 1995; 36: 159-62. [ Links ]
8. Loser C, Asch G, Hebuterne X, Mathus-Vliegen EMH, Muscaritoli M, Niv Y, Rollins H, Singer P, Skelly RH. ESPEN guidelines on artificial enteral nutrition-percutaneous endoscopic gastrostomy (PEG). Clin Nutr 2005; 24: 848-61. [ Links ]
9. Broscious SK. Preventing complications of PEG tubes. Dimens Crit Care Nurs 1995; 14: 37-41. [ Links ]
10. DeLegge RL, DeLegge MH. Percutaneous endoscopic gastrostomy evaluation of device materials: Are we "failsafe"? Nutr Clin Pract 2005; 20: 613-7. [ Links ]
11. Froehlich F, Gonvers JJ, vader JP, Dubois RW, Burnand B. Appropriateness of gastrointestinal endoscopy: risk of complications. Endoscopy 1999; 31: 684-6. [ Links ]
12. Khattak IU, Kimber C, Kiely EM, Spitz L. Percutaneous endoscopic gastrostomy in children practice: complications and outcome. J Pediatr Surg 1998; 33: 67-72. [ Links ]
13. Guloglu R, Taviloglu K, Alimoglu O. Colon injury following percutaneous endoscopic gastrostomy tube insertion. J Laparoscopic Adv Surg Tech 2003; 13: 69-72. [ Links ]
14. Segal D, Michaud L, Guimber D, Ganga-Zandzou PS, Turck D, Gottrand F. Late-onset complications of percutaneous endoscopic gastrostomy in children. J Pediatr gastroenterol Nutr 2001; 33: 495-500. [ Links ]
![]() Correspondence:
Correspondence:
Stanislaw Klek.
Stanley Dudrick Memorial Hospital.
15 Tyniecka Street.
32-050 Malopolska. Skawina. Poland.
E-mail: klek@poczta.onet.pl
Recibido: 11-XI-2013.
Aceptado: 14-XI-2013.




















