Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Nutrición Hospitalaria
versión On-line ISSN 1699-5198versión impresa ISSN 0212-1611
Nutr. Hosp. vol.29 no.3 Madrid mar. 2014
https://dx.doi.org/10.3305/NH.2014.29.3.7193
ORIGINAL / Obesidad
Weight and body composition variations in overweight women along outpatient nutritional treatment
Evolución del peso y de la composición corporal en mujeres con exceso de peso en tratamiento nutricional en ambulatorio
Flávia Gonçalves Micali1,4, Camila Cremonezi Japur2,4, Fernanda Rodrigues de Oliveira Penaforte3,4 and Rosa Wanda Diez-Garcia2,4
1Postgraduate Program of Ribeirão Preto Medical School. University of São Paulo. Brazil
2Nutrition and Metabolism. Department of Internal Medicine. Ribeirão Preto Medical School. University of São Paulo. Brazil
3Department of Nutrition. Federal University of Triangulo Mineiro - UFTM. Brazil
4Laboratory of Food Practices and Behavior - PrátiCA, Nutrition and Metabolism. Department of Internal Medicine. Ribeirão Preto Medical School. University of São Paulo. Brazil
ABSTRACT
Introduction: To evaluate the treatment of obesity it is necessary to understand the weight changes, to improve intervention strategies.
Objective: To assess the progression of weight and body parameters in overweight women along a diet therapy.
Methods: 163 women participated in this study. They were evaluated for weight, circumferences (waist and hip), and body composition (lean mass and body fat) along the three treatment phases.
Results and Discussion: The weight loss percentage was higher in the first treatment phase than in the second one (-6.8 ± 4.8% vs. -4.0 ± 2.7%, p < 0.0001). In the two first phases the circumferences and the lean mass decreased among women with weight loss. Body fat reduction occurred (-2.6%) during the first phase only.
Conclusion: Weight loss and reduction in body parameters occurred mainly in the first treatment phase, showing that it is necessary to rethink intervention strategies.
Key words: Body weight changes. Weight loss. Obesity. Body composition.
RESUMEN
Introducción: Para evaluar el tratamiento de la obesidad es necesario entender el curso de los cambios del peso para mejorar las estrategias de intervención.
Objetivo: Evaluar el peso y las medidas corporales de mujeres con exceso de peso durante un tratamiento nutricional.
Métodos: Fueron evaluadas 163 mujeres, con medición del peso, de las circunferencias (cintura y cadera) y de la composición corporal (masa magra y grasa corporal) en tres fases del tratamiento.
Resultados y discusión: El porcentaje de la pérdida de peso fue mayor en la primera que en la segunda fase del tratamiento (-6,8 ± 4,8% vs -4,0 ± 2,7%, p < 0,0001). En las dos primeras fases hubo disminución de las circunferencias y de la masa corporal magra entre las mujeres que perdieron peso. La reducción de la grasa corporal (-2,6%) se produjo sólo en la primera fase.
Conclusión: La reducción del peso y de las medidas corporales ocurren principalmente en la primera fase del tratamiento, alertando para la necesidad de una revisión de las estrategias de intervención.
Palabras clave: Cambios en el peso corporal. Pérdida de peso. Obesidad. Composición corporal.
Abbreviations
BMI: Body Mass Index.
C1: First visit.
WC: Waist Circumference.
HC: Hip Circumference.
C5: Fifth visit.
C10: Tenth visit.
C15: Fifteenth visit.
WHO: World Health Organization.
BEI: Bioelectrical Impedance.
C1-C5: Participants who attended at least five visits.
C6-C10: Participants who attended at least ten visits.
C11-C15: Participants who attended at least fifteen visits.
Subgroup WL: Participants that lost weight. Subgroup WG: Participants that gained weight.
BF: Body Fat.
Introduction
The high prevalence of obesity and the adverse effects of excess weight call for treatments that take the specificities of the assisted group into account.1 The female population is the most affected by excess weight and obesity;2 in women, these conditions culminate in gender-specific complications such as higher incidence of cervical, endometrial, ovarian, and breast neoplasms; higher prevalence of amenorrhea and infertility; and complications during pregnancy.3
Weight loss improves the patient´s metabolic profile and the aforementioned comorbidities. From a clinical standpoint, between 5.0 and 10.0% weight loss at the beginning of the treatment provides positive results.1 However, patients undergoing the treatment usually wish to achieve much larger weight loss.4 Apart from losing weight, maintaining the weight loss is a common difficulty among obese patients, because this requires permanent changes in their eating habits and lifestyle. Studies have shown that 50.0% of the patients regain the lost weight within the first post-treatment year. After three to five years, approximately 85.0% of the subjects return to or even exceed the weight they had at the start of the treatment.5
Maintaining the eating habits acquired along diet therapy requires continuous motivation, which many times is difficult to sustain due to intrinsic and extrinsic factors. Short-term goals, like allowing patients to consume sweets and other food, may overlap with long-term aims, such as weight loss.6
The strategies that bring about essential behavioral changes to achieve successful weight loss are not necessarily the same strategies that are crucial to maintaining weight loss. To obtain sustained weight loss, it is vital to promote the following conditions: reduced food intake due to emotional reasons and flexible, non-conflicting self-control of food intake associated with intrinsic motivation for practising physical activities.7
Literature studies have highlighted the health benefits arising from weight loss; they have also discussed the difficulty that patients have in maintaining weight loss in the long term, which many times results in return to the initial weight.1,5 However, little has been said about patients´ progression, weight loss milestones along the diet therapy, and the way in which these milestones could help develop strategies that translate into more effective weight loss and maintenance. In this context, the present study aims to evaluate how the weight and body composition of overweight women assisted at an outpatient clinic vary during the weight loss and maintenance phases of a diet therapy.
Materials and methods
This study evaluated 163 women admitted to an outpatient clinic between September 2005 and October 2009 and who underwent diet therapy to lose weight. The clinic specialized in obesity among women of reproductive age. All the participants were overweight or obese (Body Mass Index-BMI ≥ 25 kg/m2).
The nutritional treatment directed to reduce energy intake while preserving the recommended macronutrient composition for a "balanced diet".8
On the first visit (C1), the participants had their height, weight, waist circumference (WC), and hip circumference (HC) measured; their body composition (body fat and lean mass) was also evaluated. According to the protocol followed at the clinic, patients were re-evaluated every five visits (C1, C5, C10, and C15); all the measurements, except height, were repeated. The mean time between the visits varied between one and two months.
Body weight (kg) and height (m) were recorded on a Filizola digital scale (Personal Line) with a capacity of 150 kg and sensitivity of 0.1 kg, coupled to a stadiometer. The BMI was classified according to the cutoff points advocated by the World Health Organization (WHO)1. WC and HC were measured using previously standardized techniques.9 Body composition (lean mass, in kg, and body fat, in %) was assessed by bioelectrical impedance (BEI) conducted on the equipment Biodynamics model 450.
To analyze the data, the women were divided into groups according to the number of visits. Participants who attended at least five, ten, and fifteen visits were included in groups C1-C5, C6-C10, and C11-15 (first, second, and third phases), respectively. Therefore, data analysis included 75, 20, and 6 women in phases 1, 2, and 3, respectively.
Within each group, participants were subdivided into subjects that lost weight (subgroup WL) and subjects that gained weight (subgroup WG). Weight loss and gain corresponded to a negative and positive variation higher than 0.5 kg, respectively.
The project was approved by the Research Ethics Committee of Hospital das Clínicas da Faculdade de Medicina de Ribeirão Preto-University of São Paulo, Brazil (protocol number 10137/ 2010).
The data were processed and analyzed in a descriptive way (mean values-A and standard deviation-SD) and in percentage. To analyze and compare the mean weight, circumferences, and body weight values among the groups, the nonparametric Wilcoxon test was used for paired samples. To analyze and compare the mean lean mass among groups, the ANOVA method followed by the Kruskal-Wallis test was employed. The significance level was set at 95% (p < 0.05).
Results
The age of the participants varied between 19 and 54 years (A = 30.2 years, SD = 6.6 years); the BMI ranged from 25.4 to 57.3 kg/m2 (A = 37.5 kg/m2, SD = 6.1 kg/m2). The patients had other conditions associated with excess weight or obesity: polycystic ovary syndrome, insulin resistance, diabetes mellitus, infertility, endometriosis, dyslipidemia, arterial hypertension, and metabolic syndrome.
The mean weight loss was 6.8 (SD 4.8%), within the first five treatment months among the patients included in the subgroup WL; weight loss decreased gradually thereafter. In this subgroup, weight loss was significantly higher (p = 0.0105) in the first phase as compared with the second phase. The women who continued the treatment and maintained weight loss after the first visit achieved a mean weight loss of 4.0 (SD 2.7%), between C6 and C10 (table I) and 3.6 (SD 4.9%), between C11 and C15, without significant differences.
As for the subgroup WG, the mean weight gain was 2.4 (SD 1.6%), in the initial phase. Among the women who continued the treatment, the mean weight gain was 5.6 (SD 5.5%). Considering the initial weight, the weight gain was significant both in the first (p = 0.0012) and second (p = 0.0008) treatment phases.
Concerning body measurements, the patients belonging to the subgroup WL had significantly lower WC and HC in both the first (p < 0.0001) and second treatment phases (WC: p = 0.01 and HC: p < 0.001). The body fat percentage also varied significantly in both phases (C1-C5: p < 0.0001 and C6-C10: p = 0.0004), but the amount of lean mass did not change significantly.
Of the total number of patients, 8.6, 73.4, and 70.0% (n = 14, 88, and 55) quit between visits C1 and C2, C6 and C10, and C11 and C15, respectively. Nevertheless, in all the phases the percentage of patients that lost weight was higher (C1-C5: 68.0%, C6-C10: 65.0%, and C11-C15: 66.7%) than the percentage of patients that gained weight (C1-C5: 21.3%, C6-C10: 35.0%, and C11-C15: 33.3%). On average, the WC, HC, and body fat (BF) values decreased progressively along the first ten visits.
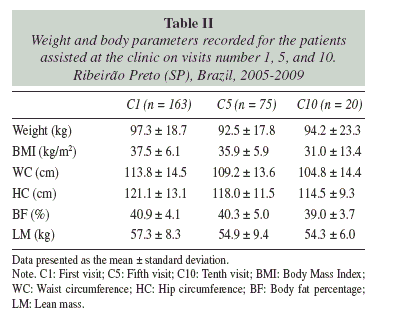
Only six women reached the third treatment phase. The mean weight and BMI varied from 109.3 kg (SD = 31.0 kg), and 43.7 kg/m2 (SD = 9.2 kg/m2), at the start of the treatment (C1) to 95.8 kg (SD = 23.6 kg), and 36.5 kg/m2 (SD = 6.2 kg/m2), at the fifteenth visit (C15), respectively. In the third phase, four women presented weight loss (A = 3.6 kg, SD = 4.9%), whereas two women gained weight (A = 1.4 kg, SD = 0.2%) (table II).
Discussion
Results revealed larger weight loss during the first treatment phase (first five visits), which corresponded to the first seven months of diet therapy on average. Thereafter, patients´ weight stabilized, but some patients even returned to their initial weight. High and progressive dropout rates along the treatment was yet another finding of the present study.
The aforementioned results stem from the difficulty that overweight patients have in maintaining food restrictions-these individuals can tolerate restrictions in the short and medium term, but not in the long term. Therefore, these patients require social support to maintain the new eating habits and ensure long-term changes in the pattern of food intake.10 Another point to consider is the patient´s expectations with respect to weight loss. Obese female patients start the treatment wishing to lose a large amount of weight,4 preferably over a short period. When the patients begin to encounter difficulty in achieving the weight loss they consider satisfactory, they become frustrated. The feeling that their effort is not being paid off diminishes their motivation to comply with the treatment.
The high dropout rates attested to the situation described above. Even the patients that continued attending the visits often presented reduced weight loss or gained the weight they lost, because they did not have the same motivation or did not make the same effort as compared with their commitment at the beginning of the treatment. A study investigating a group of patients under diet therapy reported a dropout rate of 50.0% during a 10-week follow-up.11 West et al.12 described that although many individuals were highly motivated at the start of the treatment, this motivation diminished along time. This finding might justify why two practices-rewarding for compliance with the diet or physical activity plan and remembering the reason why it is necessary to control weight-are associated with maintenance of weight loss and not with the loss itself.
Cooper & Fairburn13 proposed that when obese patients feel frustrated about not reaching the desired weight, they do not maintain the behavior they had while they were attempting to lose weight; i.e., they stop consuming food with low fat content, practising physical activities regularly, and monitoring weight constantly. The patients also neglect the need to use strategies to maintain weight. Consequently, they return to their previous eating habits and gain the weight they had lost.
Various psychological factors seem to be involved in regaining weight, such as inability to reach goals, dissatisfaction with the amount of lost weight, self-consciousness about body weight and physical shape, low self-esteem, lack of surveillance of weight control, dichotomous thinking, and tendency to use food as a way to compensate for mood swings and adversities.14
Bearing in mind possible explanations for the change in the pace of weight loss and the reasons for patient dropout, it is necessary to adopt strategies that prevent treatment cessation and lack of motivation, to maintain compliance with the new eating habits. The WC, HC, and body fat percentage values decreased along the treatment, showing that the adoption of new patterns of food intake improved health.
Nevertheless, except for weight loss, many patients disregard the positive changes arising from the treatment of obesity. Many women are dissatisfied with the weight loss rate and underestimate the meaning of the weight loss they achieved. Patients that gain the lost weight usually express dissatisfaction.4,14 Therefore, it is important to highlight that the treatment of obesity does not focus on weight loss only; it should also target improved eating habits and quality of life.
Patients that can maintain weight loss for two years reduce the risk of gaining weight by 50.0%.15 Some strategies that help maintain effective weight loss in the long term exist: engaging in high-level physical activity, maintaining constant eating habits that include food with low fat and energy content, having breakfast on a daily basis, and self-monitoring the body weight.15 However, it is necessary to analyze how these strategies should be adopted along the treatment. Assessing weight progression is a necessary task if one wishes to implement intervention strategies at each therapeutic stage, mainly after the first six months of diet therapy, so that treatment becomes more effective in terms of improved eating habits, weight loss, and weight maintenance in the long term. During exploratory qualitative studies, it might be necessary to know the difficulties patients encounter in these stages; it might also be crucial to investigate what triggers weight gain after the start of the treatment.
Conclusion
Weight loss occurs mainly during the first months of diet therapy treatment. Therefore, it is necessary to implement periodic assessments and to change strategies along the treatment, because the process of weight loss is long and demands constant motivation. Modifications made to the eating habits and lifestyle may be difficult to maintain along the treatment. New diagnostic studies on the problems and difficulties related to diet therapy must be conducted, to improve our understanding of the treatment phases and to implement more effective strategies toward weight loss and maintenance.
Acknowledgements
We thank the team working at the Ginecological Endocrinology Nutrition Outpatient Clinic of Hospital das Clínicas da Faculdade de Medicina de Ribeirão Preto.
References
1. WHO Consultation on Obesity. Obesity: Preventing and Managing the Global Epidemic. Geneva, Switzerland: World Health Organization. 2000; 894: 1-253. [ Links ]
2. World Health Organization (WHO). World Health Statistics. Part II: Highlighted topics. 2012. [ Links ]
3. Ogbuji QC. Obesity and reproductive performance in women. Afr J Reprod Health 2010; 14 (3): 143-51. [ Links ]
4. Foster GD, Wadden TA, Vogt RA, Brewer G. What is a reasonable weight loss? Patients´ expectations and evaluations of obesity treatment outcomes. J Consult Clin Psychol 1997; 65 (1): 79-85. [ Links ]
5. Wadden TA, Frey DL. A multicenter evaluation of a proprietary weight loss program for the treatment of marked obesity: A five-year follow-up. Int J Eat Disord 1997; 22 (2): 203-12. [ Links ]
6. Assis MAA, Nahas MV. Aspectos motivacionais em programas de mudança de comportamento alimentar. Rev Nutr 1999; 12 (1): 33-41. [ Links ]
7. Teixeira PJ, Silva MN, Coutinho SR, Palmeira AL, Mata J, Vieira PN, Carraia EV, Santos TC, Sardinha LB. Mediators of weight loss and weight loss maintenance in middle-aged women. Obesity (Silver Spring) 2010; 18 (4): 725-35. [ Links ]
8. World Health Organization. Food and Agriculture Organization (WHO/FAO). Diet, nutrition and the prevention of chronic diseases. Geneva; 2003. (WHO-Technical Report Series, 916). [ Links ]
9. Kissebah AH, Krakower GR. Regional adiposity and morbidity. Physiol Rev Suppl 1994; 74 (4): 761-811. [ Links ]
10. Diez-Garcia RW. Mudanças Alimentares: implicações práticas, teóricas e metodológicas. In: Diez-Garcia RW, Cervato-Mancuso AM (Org.). Nutrição e metabolismo: mudanças alimentares e educação nutricional. Rio de Janeiro: Guanabara Koogan; 2011, pp. 3-17. [ Links ]
11. Bueno JM, Leal FS, Saquy LPL, Santos CB, Ribeiro RPP. Educação alimentar na obesidade: adesão e resultados antropométricos. Rev Nutr 2011; 24 (4): 575-84 . [ Links ]
12. West DS, et al. A Motivation-Focused Weight Loss Maintenance Program is an Effective Alternative to a Skill-Based Approach. Int J Obes (London) 2011; 35 (2): 259-69. doi:10.1038/ijo.2010.138. [ Links ]
13. Cooper Z, Fairburn CG. A new cognitive behavioural approach to the treatment of obesity. Behav Res Ther 2001; 39 (5): 499-511. [ Links ]
14. Byrne S, Cooper Z, Fairburn C. Weight maintenance and relapse in obesity: a qualitative study. Int J Obes 2003; 27 (8): 955-62. [ Links ]
15. Wing RR, Hill JO. Successful weight loss maintenance. Annu Rev Nutr 2001; 21: 323-41. [ Links ]
![]() Correspondence:
Correspondence:
Rosa Wanda Diez-Garcia
Faculdade de Medicina de Ribeirão Preto USP
Departamento de Clínica Médica
Avenida dos Bandeirantes, 3900, Monte Alegre
14049-900, Ribeirão Preto, SP. Brazil
E-mail: wanda@fmrp.usp.br
Recibido: 23-IX-2013
1.a Revisión: 3-XII-2013
Aceptado: 6-XII-2013