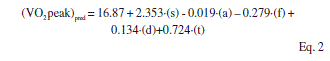Meu SciELO
Serviços Personalizados
Journal
Artigo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Acessos
Acessos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em
SciELO
Similares em
SciELO -
 Similares em Google
Similares em Google
Compartilhar
Nutrición Hospitalaria
versão On-line ISSN 1699-5198versão impressa ISSN 0212-1611
Nutr. Hosp. vol.29 no.6 Madrid Jun. 2014
https://dx.doi.org/10.3305/nh.2014.29.6.7383
Cardiovascular fitness in youth; association with obesity and metabolic abnormalities
Entrenamiento cardiovascular en la juventud; asociación con obesidad y anomalías metabólicas
Jaime Guixeres1, Pau Redon, PhD1, Javier Saiz, PhD1, Julio Álvarez, MD2,3, María Isabel Torró, MD2,3, Laura Cantero3 and Empar Lurbe MD, PhD2,3
1Polytechnical University of Valencia, Spain.
2Pediatric Department, Consorcio Hospital General Universitario, University of Valencia, Valencia, Spain.
3CIBERObn, Instituto de Salud Carlos III, Madrid, Spain.
ABSTRACT
Therapies currently implemented for obesity are focused on nutritional aspects and on physical activity. In order to make physical activity a positive therapy instead of triggering disabilities it is relevant to accurately assess cardiovascular fitness.
Objective: To assess the cardiovascular fitness by measuring the peak oxygen consumption and to asses their relationship with classical cardiometabolic parameters.
Methods: A modified Balke protocol was applied to one hundred and twenty-six Caucasians (60% males), ranging between 9 and 16 years old, who underwent an assessment of obesity. The non-obese group consisted of healthy age and sex matched subjects who were invited to participate from the general population.
Results: Significant differences in consumption of oxygen peak between non-obese and obese individuals were observed. In contrast, no significant differences existed between the categories of obesity. Furthermore in obese subjects consumption of oxygen peak was inversely correlated with parameters of cardiometabolic risk, particularly insulin and HOMA index. In addition, two predictive equations of consumption of oxygen peak, with an R2 of 0.74 and 0.84, respectively, have been developed.
Conclusion: The consumption of oxygen peak is a relevant clinical parameter that should be included in the routine clinical assessment of obese subjects. Therefore, it is crucial to make exercise tests more affordable which can be achieved by employing predictive equations.
Key words: Cardiovascular fitness. Children and adolescents. Exercise test. Obesity. VO2 peak.
RESUMEN
Las terapias que se implantan actualmente para la obesidad se centran en los aspectos nutricionales y sobre la actividad física. Con el fin de hacer que la actividad física sea una terapia positiva en vez de un desencadenador de discapacidades, es relevante evaluar de forma precisa el entrenamiento cardiovascular.
Objetivo: evaluar el entrenamiento cardiovascular midiendo el consumo máximo de oxígeno y evaluar su relación con los parámetros cardiometabólicos clásicos.
Métodos: se aplicó el protocolo modificado de Balke a 126 individuos caucásicos (60 % de varones), con edades entre 9 y 16 años, que se sometieron a una evaluación de obesidad. El grupo de no obesos consistía de individuos sanos, de la población general, emparejados por edad y sexo y a los que se les invitó a participar.
Resultados: se observaron diferencias significativas en el consumo máximo de oxígeno entre los indiviudos obesos y no obesos. Por contra, no existían diferencias significativas entre las categorías de obesidad. Además, en los sujetos obesos, el consumo máximo de oxígeno se correlacionó de forma inversa con los parámetros de riesgo cardiometabólico, particularmente con la insulina y el índice HOMA. Además, se han desarrollado dos ecuaciones predictivas del consumo máximo de oxígeno con una R2 de 0,74 y de 0,84, respectivamente.
Conclusión: el consumo máximo de oxígeno es un parámetro clínico relevante que debería incluirse en la evaluación clínica rutinaria de los sujetos obesos. Por lo tanto, es crucial hacer que las pruebas de esfuerzo sean más asequibles, que puedan alcanzarse empleando las ecuaciones predictivas.
Palabras clave: Entrenamiento cardiovascular. Niños y adolescentes. Prueba de esfuerzo. Obesidad. VO2 máximo.
Introduction
Over the last decades the prevalence of obesity in children and adolescents has increased worldwide1. This fact not only affects health expectancy and quality of life but also Health Care programs. Most of the therapies currently implemented for obesity are focused on nutritional aspects and on physical activity. Regarding the latter, it is relevant to accurately assess the individual physical limitations in order to make physical activity a positive therapy instead of triggering disabilities.
In addition to physical limitations it is interesting to assess cardiovascular fitness (CVF), one of the most reliable markers of cardiovascular risk, which can help to individualize recommended programs of physical activity. Oxygen consumption (VO2) is the single best indicator of cardiovascular fitness in either its maximal (VO2 max) or submaximal form (VO2 peak)2-5 during a physical exercise test. Furthermore, studies performed in adults6-11 and recently in non-obese children12,13 have related this parameter with metabolic abnormalities, like insulin resistance, assessed by the homeostatic model assessment (HOMA) index, and life expectancy in adults. Consequently, it is a relevant clinical parameter that could be included in the routine assessment of obese subjects.
The evaluation of CVF requires a standardized exercise protocol, of which the most popular ones include cycling, climbing steps on running in a treadmill, coupled with a calorimeter to measure the O2 consumption. Focusing on the treadmill exercise, or exercise test, the main protocols are: the Balke14, the Taylor15 and the Bruce16. Differences among them, which include speed and ramp inclination have resulted in some discrepancies. A second version of the Balke protocol was proposed by Marinov et al.17 focuses exclusively on the pediatric population, which is very susceptible to exercise modality and harshness. This new version, known as the modified Balke protocol, changes the ramp inclination twice as fast as the original. This contributes to shorter exercise duration and slightly higher VO2 peak values.
Even though these tests are apparently simple, they are time consuming and expensive mainly because costly equipment is required, treadmills and/or cycles and calorimeters. In an attempt to eliminate calorimeters, multiple studies18-24 have analyzed the influence of different parameters on the VO2 peak value to build predictive tools. Despite the fact that the gold standard is the treadmill running test, it hasn't been until recently that such a protocol has been used in the obese pediatric population25,26 as well as a predictive empirical equation has been developed26,27.
Considering the importance of VO2 peak in evaluating CVF and planning treatment for obesity, a better and easier assessment may report benefits. Therefore the objectives of the present study were: 1) To assess the CVF by measuring the VO2 peak parameter in nonobese and obese pediatric populations using a modified version of the Balke protocol, 2) to analyze the relationship between VO2 peak and classical cardiometabolic parameters and 3) to develop predictive equations to calculate the VO2 peak with or without data from the treadmill test in order to make them more affordable and less uncomfortable.
Methods
One hundred and twenty-six Caucasians (60% males), ranging between 9 and 16 years old were enrolled from those who underwent an assessment of obesity in the Pediatric Department, Consorcio Hospital General, Valencia, Spain. Patients with secondary obesity syndromes and/or with acute illnesses were excluded from the study. The non-obese were healthy age and sex matched subjects who were invited to participate from the general population. The protocol was approved by the Ethical Committee of the Consorcio Hospital General of Valencia, and all of participants gave their assent and had written parental consent. In all participants, anthropometrics and treadmill tests were performed. Additionally, analytical data were obtained in the obese group.
Anthropometrics
Body weight (± 0.1kg) and height (± 0.1cm) were measured using a standard beam balance scale with the subjects wearing light indoor clothing, no shoes and employing a standardized wall-mounted height board. Afterwards each individual was classified as nonobese or obese (moderate or severe) based on BMI percentiles and BMI zScore. Both were calculated using the World Health Organization tables28. The threshold values established were the following: nonobese individuals (BMI percentile ≤ 85th) and obese (BMI percentile > 97th). Additionally, obese population was distinguished between moderate (zScore ≤ 3) and severe obese (zScore > 3).
Blood Pressure Measurement and Metabolic Assessment
Following the published recommendations of the European Society of Hypertension Guidelines29 trained nurses measured the blood pressure (BP) and heart rate (HR) of each individual three times consecutively in the seated position, at five-minute intervals, using a mercury sphygmomanometer. Office BP was taken as the mean of three measurements. The subjects were classified as: hypertensive, high-normal or normotensive29. In obese subjects metabolic assessment was performed under fasting conditions in the early morning. Peripheral blood samples were obtained to determine: glucose30, insulin31 and lipid profile. Afterwards, the homeostatic model assessment (HOMA) index was calculated by dividing the product of insulin (units/mL) and glucose (mmoles/L) by 22.532.
Treadmill Test Protocol
The Balke protocol14 was used as baseline in the exercise test employed in the current study and afterwards slightly modified by: including an initial 3 min warm-up period, considering a constant speed of 4.8 km/h while increasing the slope by 1% each minute, from an initial 2o slope. Once a 15o slope is reached, this remains constant while the speed is increased in 0.3 km/h each minute. When a speed of 6.3 km/h has been reached, this remains constant until the subject reaches the stopping criterion. The reason for these modifications was to enhance a secure environment, avoiding running in steep slopes and taking subjects to exhaustion, especially for the youngest population for both moderate and severe obese individuals. Because children infrequently achieve a plateau in VO2, the defining criterion for VO2max, the peak, or highest, VO2 during an exhaustive effort is accepted as the representation of maximal fitness in children. Children were considered to have achieved maximal effort when reaching or surpassing the 90% of the expected maximum theoretical heart rate (HRmax) depending on the age. In figure 1 both protocols are compared with respect to ramp inclination and speed.
While performing the test, besides the VO2 peak, other parameters were continuously measured, like: the respiratory exchange ratio (RER), consumption of oxygen (VO2), breath rate (BR) and heart rate (HR). The VO2 peak, RER, VO2 and BR were recorded using the indirect calorimeter VO200033. The HR was measured with the Nuubo TIPS t-shirt34.
Statistical analysis
The statistical analysis of the results was performed using the SPSS version 16 (SPSS Inc., Chicago, Illinois, U.S.A). The analyses performed were: 1) oneway ANOVA between the three groups in which the studied population was divided; 2) Bonferroni procedure, included in the one-way ANOVA analysis menu, to analyze the significance degree of key variables by pairwise comparison between the studied groups; 3) linear regression, using the ENTER procedure, to determine the empirical equations; and 4) correlation tests to determine the correlation of the VO2 peak variable with cardiometabolic variables.
Results
Study Population
The general characteristics of the study population, grouped as non-obese or obese, moderate and severe are in table I. Age and sex distribution was not different among the three groups. By definition significant differences in weight, BMI and BMI z-score among the groups were determined by the Bonferroni procedure. Baseline systolic BP was significantly higher in the moderate obese subjects as compared to severe and non-obese due to 3 stage-one hypertensive individuals who were included in the study. In obese subjects mean values for cardiometabolic parameters were glucose (84.6 ± 7.3), insulin (10.6 ± 5.7), HOMA index (2.0 ± 1.5), triglycerides (103.4 ± 44.3), total cholesterol (157.3 ± 31.9), and uric acid (4.2 ± 0.9). No differences existed between obese groups and no diabetic subjects were included.
The key parameters obtained from the exercise test are summarized in table I: VO2 peak, HRmax, RER peak, test duration and BP values. The VO2 peak, HRmax and test duration were significantly lower in obese subjects as compared to non-obese, although no differences were observed between the moderate and severe obese. No differences in RER peak were observed among the groups. Finally, only diastolic BP showed significant differences between non-obese and obese subjects after 10 minutes of recovery from the exercise test.
Relationship between VO2peak and anthropometric and cardiometabolic parameters
In the obese subjects, the relationship between VO2 peak, anthropometric parameters, carbohydrate metabolism, and lipid profile was analyzed. Adjusted by age and sex, the VO2 peak was inversely correlated with BMI and BMI zScore, as well as with insulin and HOMA index, see table II.
VO2 peak Prediction
VO2 peak prediction with baseline data
Based on age, sex, fat content and diastolic BP a predictive equation of VO2 peak with a R2 = 0.74 was obtained (Equation 1). This equation can predict reasonably accurate the VO2 peak without performing an exercise test.
where s is sex (0: female, 1: male), a is age in years, f is amount of fat in kg and d is the diastolic blood pressure during resting conditions in mmHg.
The individual predicted value of VO2 peak was plotted against the values obtained with the calorimeter, figure 2.
VO2 peak prediction with exercise test parameters
A second equation, Equation 2, capable of predicting the VO2 peak with data from the exercise test was also calculated. This new equation, with a R2 = 0.84 employs the same anthropometric data as the previous equation plus the test duration. As expected higher accuracy can be obtained if some relevant variable data of the exercise test is included in the equation. In figure 3 the results yielded by this equation were plotted against the ones measured by the calorimeter.
where s is sex (0: female, 1: male), a is age in years,f is amount of fat in kg, d is the diastolic blood pressure during the resting phase and t is the test duration in minutes.
Discussion
In the present study, a modified version of the Balke protocol was used to assess the CVF by measuring the VO2 peak in a cohort of obese subjects recruited from an obesity clinic as compared to healthy non-obese subjects from a general population. The main findings can be summarized as follows: 1) Significant differences in VO2 peak between non-obese and obese individuals were observed, in contrast, no differences existed between the categories of obesity. 2) In obese subjects, VO2 peak inversely correlates with parameters related with the carbohydrate metabolism, insulin and HOMA index, and 3) two equations were developed from baseline and/or with parameters obtained after the treadmill test to predict the VO2 peak. The results indirectly show that the modifications performed on the treadmill test protocol are appropriate, not only to discriminate between non-obese and obese subjects, but also to detect clinically relevant findings in this pediatric population.
Interestingly, up to now the assessment of VO2 peak in obese children has been performed in very few studies25,26. In both cases maximal treadmill protocols were used comparing non-obese with obese25 or exclusively in obese26. As in the Loftin study25 the present research directly compares between non-obese and obese children. As expected, the time duration and the VO2 peak values were lower in obese children than in non-obese. These differences were significant for both parameters even though it disappears when comparing within the obese (moderate and severe obese). A reasonable explanation could be found in the duration of the test. Some studies17 point out that the recommended interval time should be between 8-12 minutes. Longer periods could have the effect that, instead of evaluating the cardiovascular system, endurance conditions start playing a role. Regarding exhaustion, quantified by RER peak was not significant between groups. This means that the individuals independently of the obesity degree were equally challenged physically. This makes the different individuals participating in the study comparable and therefore supporting future findings.
Recent studies performed in non-obese children12,13 have corroborated the inverse correlation between VO2 peak and increased insulin levels and HOMA index, found in previous studies focused on adults6-11. In the present research this finding has also been demonstrated, but in this case in the obese population (table II). Therefore, the low VO2 peak is inversely associated with fasting insulin and HOMA index, indicating that the lower the CVF the higher the risk for insulin resistance at this early stage of life, foreseeing future risk to develop metabolic syndrome and type 2 diabetes. Enhancing CVF surely influences positively to improve insulin sensitivity.
From the previous findings, the relevance of the VO2 peak parameter is clear to determine CVF and its association with cardiometabolic risk factors. Undoubtedly, this parameter should be considered in the routine clinical assessment of obese subjects. Consequently, it is necessary to make the exercise test protocols more popular and affordable to measure this parameter. To do so, the authors have developed two equations. The equations, applicable to the 126 subjects included the study, with a wide BMI range, were derived from baseline parameters (Equation 1), as well as from parameters obtained from the exercise test (Equation 2). These baseline parameters (percentage of body fat and the diastolic blood pressure in resting conditions) are easily measured variables. The inclusion of diastolic blood pressure in the equation versus systolic blood pressure can be explained by its substantially lower variability in comparison with systolic blood pressure.
Equation 2 will be employed once the exercise test has been performed. The main advantage is undoubtedly that it can eliminate the need to use a calorimeter, which is expensive and uncomfortable equipment. This predictive equation is dependent on the same anthropometric data as in Equation 1 plus the test duration variable.
Additional analyses were performed in both contexts in search of patterns which could help identify the reasons why some individuals did not have reasonable accurate VO2 peak predictions. However, no patterns were observed, reflecting that the current equations have been fully optimized for the studied population.
As far as we know, there are few published studies that develop an equation for obese children to predict VO2 peak26 27. Melendez-Ortega et al.26, using the treadmill proposes an equation that is dependant of the maximal stage reached by the subject and independent of any physiological variable. The accuracy of this equation (R2) is not published. As the author states, only 35% of the test was considered as maximal and a 49% of subjects stopped the test because of pain in their legs. On the other hand, Nemeth et al.27 proposed an equation using subject's weight, height, sex, heart rate and maximum speed of the treadmill reached during the protocol. This equation was adapted for obese children with an accuracy of R2 = 0.74. In our model the accuracy is R2 = 0.84, without the heart rate variable, simplifying the test.
In conclusion, the present study reflects the importance of the VO2 peak parameter, not only to quantify the CVF, but also its inverse correlation with fasting insulin and HOMA index, considered as a fingerprint of future metabolic disease. The VO2 peak is a relevant clinical parameter that should be included in the routine clinical assessment of obese subjects. In order to facilitate the use of the exercise test, they need to be made more affordable. Therefore, two empirical VO2 peak predictive equations have been developed for pediatric obese and non-obese populations, yielding reasonably accurate results.
References
1. WHO. Prevention and control of non-communicable diseases. Report of the Secretary-General. United Nations General Assembly A/66/83, 19 May 2011. Available at URL: (http: //www.un.org/ga/search/view_doc.asp?symbol=A/66/83&Lang=E). Accessed December 9, 2013. [ Links ]
2. Perez-Farinos N, Lopez-Sobaler AM, Dal Re MA, et al. The ALADINO study: a national study of prevalence of overweight and obesity in Spanish children in 2011. Biomed Res Int 2013; 2013. p. 163687. [ Links ]
3. Shephard RJ, Allen C, Benade AJ, et al. The maximum oxygen intake. An international reference standard of cardiorespiratory fitness. Bulletin World Health Organization 1968; 38: 757-64. [ Links ]
4. Taylor HI, Buskrik E, Henschel A. Maximal oxygen intake as objective measurement of cardio-respiratory performance. Journal Applied Physiology 1955; 8: 73-80. [ Links ]
5. Ortega FB, Ruiz JR, Castillo MJ, Sjöström M. Physical fitness in childhood and adolescence: a powerful marker of health. International Journal of Obesity 2008; 32: 1-11. [ Links ]
6. Tunstall RJ, Mehan K.A, Wadley GD, et al. Exercise training increases lipid metabolism gene expression in human skeletal muscle. Am J Physiol Endocrinol Metab. 2002; 283: 66-72. [ Links ]
7. Goodpaster BH, Katsisaras A and Kelley DE. Enhanced fat oxidation through physical activity is associated with improvements in insulin sensitivity in obesity. Diabetes 2003; 52: 2191-7. [ Links ]
8. Bruce CR, Kriketos AD, Cooney GJ and Hawley JA. Disassociation of muscle triglyceride content and insulin sensitivity after exercise training in patients with type 2 diabetes. Diabetologia 2004; 47: 23-30. [ Links ]
9. Ouyang P, Sung J, Kelemen MD, et al. Stewart. Journal of Women's Health 2004, 13: 177-85. [ Links ]
10. Bruce CR, Thrush AB, Mertz VA, et al. Endurance training in obese humans improves glucose tolerance and mitochondrial fatty acid oxidation and alters muscle lipid content. Am J Physiol Metab 2006; 291: 99-107. [ Links ]
11. Cortright RN, Sandhoff KM, Basilio JL, et al. Skeletal muscle fat oxidation is increased in African-American and White women after 10 days of endurance exercise training. Obesity 2006; 14: 1201-10. [ Links ]
12. Anderssen LB., Sardinha LB, Froberg K, Riddoch CJ, Page AS, Anderssen SA. Fitness, fatness and clustering of cardiovascular risk factors in children from Denmark, Estonia and Portugal: The European Youth Heart Study. Int Journal Pediatric Obesity 2008;3:58-66. [ Links ]
13. Gobbi RM, Davies IG, Fairclough SJ, et al. Clustered Cardiometabolic Risk, Cardiorespiratory Fitness and Physical Activity in 10-11 years old children. The CHANGE! Project Baseline. Archives of Exercise in Health and Disease 2012; 3: 207-13. [ Links ]
14. Balke J, Ware RW. An experimental study of physical fitness of Air Force personnel. US Armed Forces Medical Journal 1959; 10: 675-88. [ Links ]
15. Taylor HI, Wang Y, Rowell R, et al. The standardization and interpretation of submaximal and maximal tests of working capacity. Pediatrics 1963; 32: 703-22. [ Links ]
16. Bruce RA. Exercise testing of patients with coronary artery disease. Annals Clinical Research 1971; 3: 323-32. [ Links ]
17. Marinov B, Kostianev S, Turnovska T. Modified treadmill protocol for evaluation of physical fitness in pediatric age group-Comparison with Bruce and Balke protocols. Acta Physiologica & Pharmacologica Bulgaric. 2003; 27: 47-51. [ Links ]
18. Krahenbuhl GS, Skinner JS, & Kohrt WM. Developmental aspects of maximal aerobic power in children. Exercise and Sport Sciences Reviews 1985; 13: 503-38. [ Links ]
19. Léger LA, Mercier D, Gadoury C, and Lambert J. The multistage 20 meter shuttle run test for aerobic fitness. J Sports Sci 1988; 6: 93-101. [ Links ]
20. Barnett A, Chan LYS, Bruce IC. A preliminary study of the 20-m multistage shuttle run as a predictor of peak VO2 in Hong Kong Chinese Students. Pediatr Exerc Sci 1993; 5: 42-50. [ Links ]
21. Flouris AD, Koutedakis Y, Nevill A, Metsios GS, Tsiotra G, Parasiris Y. Enhancing specificity in proxy-design for the assessment of bioenergetics. J Sci Med Sport 2004; 7: 197-204. [ Links ]
22. Rowland T. Children's exercise physiology (2nd edition). Champaign, IL: Human Kinetics. 2005. [ Links ]
23. Chia M, Aziz AR, Tan F, Chuan K. Examination of the performances of youth soccer players in a 20-metre shuttle run test and a treadmill run test. Adv Exerc Sports Physiol 2005; 11: 95-101. [ Links ]
24. Metsios GS, Flouris AD, Koutedakis Y, Nevill A. Criterion-related validity and test-retest reliability of the 20m square shuttle test. J Sci Med Sport 2008; 11: 214-7. [ Links ]
25. Loftin M, Sothern M, Warren B, Udall J. Comparison of VO2 peak during treadmill and cycle ergometry in severely overweight youth. Journal of Sports Science and Medicine 2004; 3: 254-60. [ Links ]
26. Melendez-Ortega AM, Davis CL, Barbeau P, Boyle CA. Oxygen uptake of overweight and obese children at different stages of a progressive treadmill test. Rev Int Cienc Deporte 2010; 6: 74-90. [ Links ]
27. Nemeth A, Carrel AL Eickhoff J, Clark RR, Peterson SE, Allen DB. Submaximal treadmill test predicts VO2max in overweight children. J Pediatr 2009; 154: 677-81. [ Links ]
28. Cook S, Auinger P, Huang TTK. Growth curves for cardio-metabolic risk factors in children and adolescents. J Pediatr 2009; 155: S6.e26. [ Links ]
29. Lurbe E, Cifkova R, Cruickshank JK, et al. European Society of Hypertension. Management of high blood pressure in children and adolescents: recommendations of the European Society of Hypertension. J Hypertens 2009; 27: 1719-42. [ Links ]
30. Morrison B. Use of the Beckman glucose analyzer for low and high glucose values. Clinical Chimia Acta 1972; 42: 192. [ Links ]
31. Hales CN, Randle PJ. Immunoassay of insulin with insulin antibody precipitate. Biochem J 1963; 88: 137. [ Links ]
32. Quon MJ. Limitations of the fasting glucose to insulin ratio as an index of insulin sensitivity. J Clin Endocrinol Metab 2001; 86: 4615-7. [ Links ]
33. Wahrlich V, Anjos LA, Going SB, Lohman TG. Validation of the VO2000 calorimeter for measuring resting metabolic rate. Clinical Nutrition 2006; 25: 687-92. [ Links ]
34. Guixeres J, Zaragoza I, Alcaniz M, Gomis-Tena J, Cebolla A, Zaragoza I, Alcaniz M. A new protocol test for physical activity research in obese children (etiobe project). Stud Health Technol Inform 2009; 144: 281-3. [ Links ]
![]() Correspondence:
Correspondence:
Empar Lurbe.
Pediatric Department.
Consorcio Hospital General Universitario.
University of Valencia.
Avda. Tres Cruces, 2.
46014 Valencia. Spain.
E-mail: empar.lurbe@uv.es
Recibido: 26-II-2014.
Aceptado: 12-III-2014.