Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Nutrición Hospitalaria
versión On-line ISSN 1699-5198versión impresa ISSN 0212-1611
Nutr. Hosp. vol.33 no.2 Madrid mar./abr. 2016
https://dx.doi.org/10.20960/nh.106
TRABAJO ORIGINAL / Obesidad y síndrome metabólico
Effect of two days treatment with orlistat on plasma leptin in obese patients without weight loss
Efecto del tratamiento de dos días con orlistat sobre los niveles de leptina plasmática en pacientes obesas sin pérdida de peso
Ana Rodríguez-Valle1, María Ángeles Navarro-Ferrando2, Diana Boj-Carceller3, Jesús Fernando Escanero-Marcén2 and Alejandro Sanz-Paris3
1Department of Clinical Biochemistry. Hospital Universitario Miguel Servet de Zaragoza. Zaragoza, Spain.
2Universidad de Zaragoza. CIBER-OBN, IIS. Zaragoza, Spain.
3Unit of Nutrition and Dietetics. Hospital Universitario Miguel Servet de Zaragoza. Zaragoza, Spain
ABSTRACT
Objective: Little is known about the impact of orlistat on the leptin system. We studied the plasma leptin and satiety sensation response for two days of orlistat treatment without hypocaloric diet and weight loss.
Material and methods: Twenty obese female subjects were recruited from our medical outpatient clinics. All of these subjects had previously received advice on dietary restriction and lifestyle modification, but remained obese with a stable body weight for at least six months before recruitment for the study.
Results: Subjects were given 120 mg orlistat 3 times daily and were asked to maintain their usual diet. At baseline and two days after the treatment with orlistat, physical examination, hunger and blood analysis were repeated. There were no significant differences observed regarding energy dietary intake, body weight and waist-hip ratio, or in plasma glucose, insulin c-peptide concentrations. Only plasma leptin and triglycerides concentrations decreased (p: 0.0001 and 0.01 respectively). Decrease in plasma leptin concentration was positively correlated with changes observed in plasma triglycerides concentration (p: 0.01, r2: 0.45). Pre-dinner hunger increased and was negatively correlated with decrease in leptin (p: 0.0001, r2: 0.74) and triglycerides (p: 0.02, r2: 0.59).
Conclusion: These data suggest that the partial fat malabsorption induced by the treatment with orlistat quickly reduces plasma triglycerides and leptin. This decrease is associated with increased appetite before intake following the main meal of the day.
Key words: Leptin. Orlistat. Triglycerides. Obesity. Satiety.
RESUMEN
Objetivo: poco se conoce sobre el impacto de orlistat en el sistema leptina. Estudiamos la respuesta de la leptina plasmática y la sensación de saciedad tras dos días de tratamiento con orlistat sin dieta hipocalórica ni pérdida de peso.
Material y métodos: reclutamos veinte mujeres obesas en nuestras consultas externas de medicina. Habían recibido restricción dietética y modificación del estilo de vida, pero se habían mantenido obesas con peso corporal estable durante seis meses antes de su inclusión en el estudio.
Resultados: las pacientes tomaron 120 mg de orlistat 3 veces al día y mantuvieron su dieta habitual. Al inicio y dos días después del tratamiento con orlistat se repitieron el examen físico, la sensación de hambre y la analítica. No hubo diferencias significativas en el consumo de energía de la dieta, el peso corporal y la relación cintura-cadera, así como en glucosa sérica, insulina y péptido C. Solamente las concentraciones de leptina y triglicéridos en suero disminuyeron (p: 0,0001 y 0,01, respectivamente). La disminución de la concentración de leptina en suero se correlacionó positivamente con cambios en la concentración de triglicéridos (p: 0.01, r2: 0,45). La sensación de hambre aumento antes de la cena y se correlacionó negativamente con la disminución de la leptina (p: 0,0001, r2: 0,74) y triglicéridos (p: 0,02, r2: 0.59).
Conclusión: estos datos sugieren que la malabsorción parcial de grasas por el tratamiento con orlistat disminuye rápidamente los niveles plasmáticos de triglicéridos y leptina. Este descenso se asoció con aumento del apetito antes de la ingesta que sigue a la comida principal del día.
Palabras clave: Leptina. Orlistat. Triglicéridos. Obesidad. Sociedad.
Introduction
Obesity is a chronic and costly disease which is increasing prevalence in many countries around the world. Hypo-caloric diet is the cornerstone of its treatment, but compliance is sometimes very difficult and almost impossible in the long term. Pharmaceutical strategies in the treatment of obesity include: drugs that regulate food intake, thermo genesis, fat absorption or fat metabolism (1).
Orlistat is a hydrogenated derivative of a fungal lipase inhibitor that blocks lipases and decreases triglyceride digestion in the intestinal lumen. Previous studies have confirmed the efficacy of orlistat in weight reduction with an improvement in cardiovascular risk factors among obese subjects (2).
Little is known about the impact of orlistat on the leptin system. Leptin is an adipocyte-derived hormone with important hypothalamic effects on the regulation of food intake and energy expenditure. In the fed state, circulating concentrations of leptin reflect the amount of energy stored in fat and correlate positively with adiposity indices. Individuals with similar degrees of adiposity exhibit great variations in plasma leptin concentrations. Hormonal and nutritional factors have been proposed to influence this (3).
Caloric deprivation and loss of fat cell mass have been shown to decrease plasma leptin concentration. This observation has led to the hypothesis that leptin serves as a signal from the adipose tissue to the brain, where it acts as a regulator of satiety. However, during 24 hours of fasting Haluzik et al. (4) described a 0.5% loss of their total body fat, while plasma leptin concentrations fell by 50%. It appears unlikely that the small change observed in fat mass could have been responsible for the profound decrease in plasma leptin concentrations.
Orlistat may cause an increase in appetite because of decreased absorption of dietary triglycerides. There are contradictory findings between the studies that examined the effects of orlistat on satiety (5-7).
In view of the postulated role of leptin as a satiety factor, we felt it would be of interest to determine plasma leptin response to two days of orlistat treatment without hypo-caloric diet. The choice of this short period aims at ruling out the loss of fat mass from the observed results.
Methods and procedures
Twenty obese female subjects were recruited from the medical outpatient clinic. These subjects were initially referred to the hospital for weight management. All of them had received previous advice on dietary restriction and lifestyle modification, but remained obese with a stable body weight for at least six months before recruitment for the study.
Exclusion criteria included: secondary obesity, pregnancy, lactation, childbearing potential with inadequate contraceptive measures, psychiatric or neurological disorders, alcohol or other substance abuse, previous gastrointestinal tract surgery for weight reduction, significant gastrointestinal symptoms, a history or the presence of malignancy, a significant history of cardiovascular complications or renal impairment.
We conducted an open-label, prospective cohort study. After giving written informed consent, eligible subjects underwent an assessment process including medical history, dietary intake using two days of food records, physical examination and measurement of laboratory variables.
All subjects were given orlistat 120 mg capsules before breakfast, lunch and dinner. Subjects were asked to maintain their usual diet. All of them returned to the clinic two days later, where physical examination, measurement of laboratory variables, dietary intake records and subjective appetite sensations were repeated and compliance with orlistat treatment was ensured. Analytical determinations were performed after 8 hours fasting.
Dietary intake was measured using a two day food diary. Entries were verified together with the patient by a dietitian using food models. Nutritional composition was determined by a Spanish DIAL program (8).
Subjects were asked about their feelings of hunger and their desire to eat before lunch and dinner. For the assessment of subjective appetite sensations, a visual analogue scale was used. Patients were asked to make a vertical mark across the line corresponding to their feeling at the present time. Quantification of the measurement was made by measuring the distance from the left end of the line to the mark on a 100 mm line from "not at all" (0 mm) to "extremely" (100 mm).
Laboratory variables included fasting plasma levels of glucose, triglycerides, total cholesterol and high density lipoprotein cholesterol (HDL-C), which were measured on a Hitachi 911 automated analyzer (Boehringer Mannheim, Germany) using reagent kits supplied by the analyzer manufacturer. The precision performance of these assays was within the manufacturer's specifications. Levels of low-density lipoprotein cholesterol (LDL-C) were calculated using the Friedewald equation. Plasma total leptin, insulin and C-peptide were evaluated using a commercially available RIA method.
Data were analyzed using the Statistical Package for the Social Sciences for Windows, version 22.0 (SPSS Inc., Chicago, IL, USA). Descriptive statistics of the sample are presented. All results are shown as mean + SE. We used the Wilcoxon test for within-patient comparisons between baseline and post-treatment measurements. Spearman correlation coefficients were determined to examine the relationships between percentages of changes. The value p < 0.05 was considered to be statistically significant.
Results
All the patients were included and there were no losses recorded during the following, therefore, 20 people completed the protocol study.
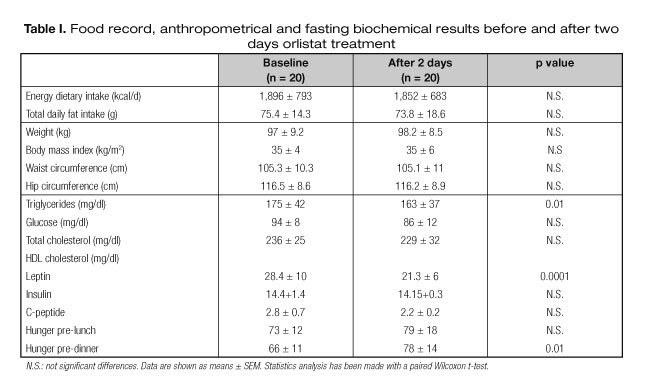
Table I shows dietary energy intake, anthropometrics and laboratory results at baseline, and after two days with orlistat treatment. There were no significant differences regarding dietary energy intake, body weight and waist-hip ratio, or plasma glucose, insulin and C-peptide concentrations.
Plasma leptin and triglycerides concentrations decreased significantly after two days of treatment without dietary restrictions.
After orlistat treatment, hunger and desire to eat before lunch and dinner increased, but only pre-dinner hunger showed statistical significance (p = 0.01).
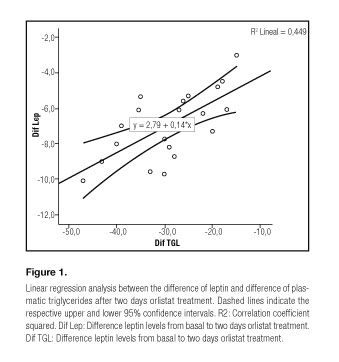
Figure 1 shows changes in plasma leptin concentration after two days with orlistat treatment, positively correlated with changes in plasma triglycerides concentration (p = 0.001, R2: 0.449, beta 0.67).
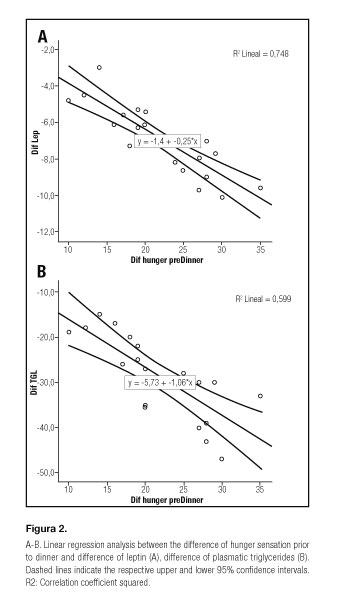
Differences between pre/post treatment on hunger sensation before dinner correlated with changes in plasma leptin (R2 = 0.75, p < 0.001, beta: -0.62) (Fig. 2A) and with changes in plasma triglycerides concentration (R2 = 0.60, p = 0.02, beta: -0.35) (Fig. 2B).
Discussion
In this study, all patients had made previous attempts to lose weight by dietary restriction and other lifestyle modifications, but weight reducing effects were only short lived. To examine the effect of orlistat on fuel metabolism and related hormones without the confounding factor of a hypocaloric diet and weight loss, subjects were asked to maintain their habits/food behavior.
Orlistat is minimally absorbed, thus, no systemic direct effects in the regulation of food intake are expected. It is a potent, specific and reversible inhibitor of gastric and pancreatic lipases that reduces fat absorption by approximately 30% (2).
We have observed that plasma leptin reduction derived from orlistat treatment was associated with a concomitant reduction in triglycerides in these obese subjects (Fig. 1). It is not certain whether orlistat has a direct effect on leptin levels independent of weight reduction. Nevertheless, the absence of a decline in body weight within the two days of treatment, and the good -correlation of leptin and triglyceride decreases, support the notion that orlistat induced triglyceride decrease could be the key to leptin response.
There is a large mass of evidence demonstrating that insulin responses to meals are the primary mediator of changes in leptin production observed during energy restriction (9). But Western dietary patterns and high-fat diet have been positively associated with plasma leptin concentrations in women and men (10).
Orlistat improves postprandial lipemia by reducing dietary triglyceride absorption (11,12). The combination of gemfibrozil and orlistat is extremely effective in reducing plasma triglyceride le-vels (13) and orlistat therapy without concomitant hypocaloric diet improved triglyceride levels (14). Reduction of plasma triglyceride levels could reduce leptin resistance in obese subjects and hence, decrease plasma leptin levels. Plasma triglycerides may underlie the impairment in blood-brain barrier transport of leptin in obesity. Rodrigues et al. (15) showed a decrease in cerebrospinal fluid/plasma leptin ratio after orlistat therapy, but not with fenproporex neither with sibutramine.
In mice, diet-induced obesity increased triglycerides and reduced leptin uptake by the brain. Sixteen hours of fasting reduced triglycerides and increased leptin uptake. Furthermore, reduction of triglyceride levels by pharmacological treatment with gemfibrozil enhanced leptin transport (16). These results could explain why mice, which are unable to synthesize triglycerides, are more sensitive to leptin infusions (17). Thus, lowering triglycerides may be therapeutically useful in enhancing the effects of leptin on weight loss.
The primary importance of leptin in the regulation of energy homeostasis is for reduced leptin production to function as a signal of negative energy balance and low energy reserves. Obesity appears to be generally associated with high circulating leptin levels and reduced responsivity to leptin. The major effect of leptin administration in leptin deficiency on food intake with normalization of hyperphagia (18) but in obesity, high circulating leptin levels are unable to suppress feeding because of leptin resistance. Decreased plasmatic leptin levels in obese patients to normal levels could be an objective of treatment to avoid this leptin resistance and improve the anorexic leptin action (19).
Plasma leptin levels depend not only on the size of adipose tissue mass, because fasting decreases leptin levels without marked changes in the body fat mass. The degree of short-term caloric restriction has an effect on acute changes in plasma leptin concentration that may not be correlated with fat mass loss. Boden et al. (20) observed a 72% decrease in plasma leptin levels in normal volunteers after 52 hours fasting, suggesting that it is regulated by factors other than changes in body fat mass. Subsequently, other authors showed similar results. Klein et al. (21) observed that at 22 hours fasting, leptin production rates decreased in adipose tissue, and Haluzik et al. (22) observed that 24-h fasting significantly decreased plasma leptin.
The impact of orlistat on plasma leptin levels in obese patients has not been extensively studied. Brook et al. (23) showed a leptin decrease in a 3 month trial. Derosa et al. (24) observed a faster decrease in leptin compared with the control group in 254 type 2 diabetic patients, after 12 months of orlistat treatment. Hsieh et al. (25), after one year of treatment in Asian obese patients, observed that over the same range of BMI, body fat% and waist circumference loss, the orlistat treatment group experienced more significant changes in plasma levels of leptin than the control group. On the other hand, Ozcelik et al. (26) showed, after 12 weeks, a similar decrease in plasma leptin in 14 patients who received orlistat and 10 patients that received placebo.
In all these studies, there was a weight loss that distorted results. We only found one publication studying the response of leptin to orlistat, without the effect of weight loss from our study. Sahin et al. (27) found in 34 obese patients that a single dose of 120 mg orlistat produced no changes in postprandial plasma leptin levels, although it increased a little in patients who had taken prlistat. Their results do not correspond with ours, maybe because their patients had a single dose of orlistat. Fat intake may be inadequate because no differences were observed in postprandial triglycerides.
More studies are needed as regards the response of postprandial leptin. In our study, two days of orlistat treatment induced plasma triglyceride and leptin reductions, which were correlated with each other.
In the present study, we have found a higher hunger sensation before dinner. This effect was not observed prior to breakfast or lunch. In the Spanish way of life, lunch is the main meal of the day, so it is expected to be the moment when orlistat could have the greatest effect on postprandial triglycerides. Unfortunately, we did not clearly define the postprandial response, but there are many studies that showed the effect of orlistat on postprandial triglyceride response to a meal (11,12).
It has been previously postulated that orlistat may increase appetite because it accelerates gastric emptying (28,29). We found three randomized controlled studies comparing the use of orlistat to a placebo in appetite after an ingested meal. In a study by Ellrichman et al. (7), the administration of orlistat led to a 15% reduction in satiety ratings and a 24% increase in appetite, with a 31% of prospective food consumption. But in both Demarchi et al. (6) and Goedecke et al. (5) studies, orlistat was not shown to alter hunger, satiety, prospective consumption or fullness rates, while examining changes over time.
It is the first time that it is possible to study the impact of orlistat on serum leptin without the confounding effect of weight loss and diet. The patients in our study did not lose weight because they did not make any qualitative or quantitative change in their diet and follow-up time was only two days. In our study, reductions in plasma triglycerides were found to be directly related to decreases in circulating levels of leptin. Moreover, this hunger increase is related to a decrease in plasma triglycerides. It is well established that orlistat reduces plasma triglycerides.
We have found a link between hunger sensation and orlistat induced leptin and triglycerides decrease. It is difficult to explain why we observed increased appetite only just before dinner after treatment with orlistat. The reason may be that in Spain lunch is the main meal, where triglycerides (TGL) intake is higher than in breakfast. Thus, the effect of orlistat on postprandial TGL could be higher after lunch than after breakfast. If we assume that appetite sensation depends on the absorption of postprandial TGL, these would further decrease after lunch than after breakfast. Unfortunately, we did not measure TGL after breakfast, lunch or dinner to determine the possible different effect of orlistat on postprandial TGL in the different meals.
Several other limitations exist in the present study: placebo controlled trial and postprandial lipemia or fecal fat excretion induced by orlistat were not determined. But, to our knowledge, there are currently no other published data on the effect of short term orlistat treatment on circulating leptin levels in humans without weight changes. Moreover, we have observed a relationship between this change in plasma leptin with hunger sensation and variations in plasma triglycerides. Hence, our finding is of relevance in day-to-day clinical practice, where restricting diet is a very difficult treatment method.
In conclusion, these data suggest that plasma leptin concentration is rapidly regulated by factors other than changes in fat cell mass. Partial fat malabsorption induced by treatment with orlistat quickly reduces plasma triglycerides and leptin. This plasma triglycerides decrease could be an important regulation factor of leptin secretion. Furthermore, this decrease in plasma leptin was associated with increased appetite before intake following the main meal of the day.
References
1. Cabrerizo García L, Ramos-Leví A, Moreno Lopera C, Rubio Herrera MA. Update on pharmacology of obesity: Benefits and risks. Nutr Hosp 2013;28(Suppl 5):121-7. [ Links ]
2. García Díaz E, Martín Folgueras T. Systematic review of the clinical efficacy of sibutramine and orlistat in weigth loss, quality of life and its adverse effects in obese adolescents. Nutr Hosp 2011;26:451-7. [ Links ]
3. Allison MB, Myers MG Jr. 20 years of leptin: Connecting leptin signaling to biological function. J Endocrinol 2014;223:T25-T35. [ Links ]
4. Haluzik M, Matoulek M, Svacina S, Hilgertova J, Haas T. The influence of short-term fasting on plasma leptin levels and selected hormonal and metabolic parameters in morbidly obese and lean females. Endocr Res 2001;27:251-60. [ Links ]
5. Goedecke J, Barsdorf M, Beglinger C, Levitt N, Lambert E. Effects of a lipase inhibitor (Orlistat) on cholecystokinin and appetite in response to a high-fat meal. International Journal of Obesity & Related Metabolic Disorders 2003;27:1479-85. [ Links ]
6. Demarchi B, Vos R, Deprez P, Janssens J, Tack J. Influence of a lipase inhibitor on gastric sensitivity and accommodation to an orally ingested meal. Alimentary Pharmacology & Therapeutics 2004;19:1261-8. [ Links ]
7. Ellrichmann M, Kapelle M, Meier J, Ritter PR, Holst JJ, Herzig KH, et al. Orlistat inhibition of intestinal lipase acutely increases appetite and attenuates postprandial glucagon-like peptide-1-(7-36)-amide-1, cholecystokinin, and peptide YY concentrations. The Journal of Clinical Endocrinology and Metabolism 2008;93:3995-8. [ Links ]
8. http://www.seh-lelha.org/calena.aspx [ Links ]
9. Havel PJ. Control of energy homeostasis and insulin action by adipocyte hormones: Leptin, acylation stimulating protein and adiponectin. Curr Opin Lipidol 2002;13:51-9. [ Links ]
10. Yannakoulia M, Yiannakouris N, Blüher S, Matalas AL, Klimis-Zacas D, Mantzoros ChS. Body fat mass and macronutrient intake in relation to circulating soluble leptin receptor, free leptin index, adiponectin, and resistin concentrations in healthy humans. J Clin Endocrinol Metab 2003;88:1730-6. [ Links ]
11. Suter PM, Marmier G, Veya-Linder C, Hänseler E, Lentz J, Vetter W, et al. Effect of orlistat on postprandial lipemia, NMR lipoprotein subclass profiles and particle size. Atherosclerosis 2005;180:127-35. [ Links ]
12. Abejuela ZR, Macaballug A, Sumpio J, Zacarias M, Mercado-Asis L. Orlistat abolishes postprandial lipid peaking. Int J Endocrinol Metab 2009;7:179-86. [ Links ]
13. Tolentino MC, Ferenczi A, Ronen L, Poretsky L. Combination of gemfibrozil and orlistat for treatment of combined hyperlipidemia with predominant hypertriglyceridemia. Endocr Pract 2002;8:208-12. [ Links ]
14. Tong PC, Lee ZS, Sea MM, Chow CC, Ko GT, Chan WB, et al. The effect of orlistat-induced weight loss without concomitant hypocaloric diet on cardiovascular risk factors and insulin sensitivity in young obese Chinese subjects with or without type 2 diabetes. Arch Intern Med 2002;162:2428-35. [ Links ]
15. Rodrigues AM, Bento Radominski R, De Lacerda Suplicy H, Monteiro de Almeida S, Artigas Niclewicz P, Boguszewski CL. The cerebrospinal fluid/plasma leptin ratio during pharmacological therapy for obesity. J Clin Endocrinol Metab 2002;87:1621-6. [ Links ]
16. Banks W, Coon AB, Robinson SM, Moinuddin A, Shultz JM, Nakaoke R, et al. Triglycerides induce leptin resistance at the blood-brain barrier. Diabetes 2004;53:1253-60. [ Links ]
17. Chen HC, Smith SJ, Ladha Z, Jensen DR, Ferreira LD, Pulawa LK, et al. Increased insulin and leptin sensitivity in mice lacking acyl CoA: Diacylglycerol acyltransferase1. J Clin Invest 2002;109:1049-55. [ Links ]
18. Farooqi IS, Jebb SA, Langmack G, Lawrence E, Cheetham CH, Prentice AM, et al. Effects of recombinant leptin therapy in a child with congenital leptin deficiency. New England Journal of Medicine 1999; 341: 879-84. [ Links ]
19. DePaoli AM. Leptin in common obesity and associated disorders of metabolism. Journal of Endocrinology 2014;223;T71-T81. [ Links ]
20. Boden G, Chen X, Mozzoli M, Ryan I. Effect of fasting on plasma leptin in normal subjects. J Clin Endocrinol Metab 1996;81:3419-23. [ Links ]
21. Klein S, Horowitz JF, Landt M, Goodrick SJ, Mohamed-Ali V, Coppack SW. Leptin production during early starvation in lean and obese women. Am J Physiol Endocrinol Metab 2000;278:E280-7. [ Links ]
22. Haluzik M, Matoulek M, SvacÏina S, Hilgertova J, Haas T. The influence of short term fasting o plasma leptin levels, and selected hormonal and metabolic parameters in morbidly obese and lean females. Endocrine Research 2001;27:251-60. [ Links ]
23. Brook RD, Bard RL, Glazewski L, Kehrer C, Bodary PF, Eitzman DL, et al. Effect of short-term weight loss on the metabolic syndrome and conduit vascular endothelial function in overweight adults. Am J Cardiol 2004;93:1012-6. [ Links ]
24. Derosa G, Maffioli P, Salvadeo SA, Ferrari I, Gravina A, Mereu R, et al. Comparison of orlistat treatment and placebo in obese type 2 diabetic patients. Expert Opin Pharmacother 2010;11:1971-82. [ Links ]
25. Hsieh CJ, Wang PW, Liu RT, Tung SC, Chien WY, Chen JF, et al. Orlistat for obesity: Benefits beyond weight loss. Diabetes Res Clin Pract 2005;67:78-83. [ Links ]
26. Ozcelik O, Dogan H, Kelestimur H. Effects of a weight-reduction program with orlistat on plasma leptin levels in obese women: A 12-week, randomized, placebo-controlled study. Curr Ther Res Clin Exp 2004;65:127-37. [ Links ]
27. Sahin M, Tanaci N, Yucel M, Kutlu M, Tutuncu NB, Pamuk B, et al. Acute effects of orlistat on postprandial plasma leptin levels in nondiabetic obese patients. Minerva Endocrinol 2008;33:169-73. [ Links ]
28. Pilichiewicz A, O'Donovan D, Feinle C, Lei Y, Wishart JM, Bryant L, et al. Effect of lipase inhibition on gastric emptying of, and the glycemic and incretin responses to, an oil/aqueous drink in type 2 diabetes mellitus. J Clin Endocrinol Metab 2003;88:3829-34. [ Links ]
29. O'Donovan D, Horowitz M, Russo A, Feinle-Bisset C, Murolo N, Gentilcore D, et al. Effects of lipase inhibition on gastric emptying of, and on the glycaemic, insulin and cardiovascular responses to, a high-fat/carbohydrate meal in type 2 diabetes. Diabetologia 2004;47:2208-14. [ Links ]
![]() Correspondence:
Correspondence:
Alejandro Sanz-Paris.
Unit of Dietetics and Nutrition.
Department of Endocrinology and Nutrition.
Hospital Universitario Miguel Servet.
Paseo Isabel la Católica, 1-3.
50009 Zaragoza, Spain
e-mail: sanzparisalejandro@gmail.com
Received: 29/9/2015
Accepted: 03/02/2016