Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Nutrición Hospitalaria
versión On-line ISSN 1699-5198versión impresa ISSN 0212-1611
Nutr. Hosp. vol.33 supl.3 Madrid 2016
https://dx.doi.org/10.20960/nh.314
Urinary hydration biomarkers and dietary intake in children
Patrícia Padrão1,2, Mafalda Neto1, Mariana Pinto3, Ana Catarina Oliveira1, André Moreira3 and Pedro Moreira1,4
1Faculty of Nutrition and Food Sciences. University of Porto (FCNAUP). Porto, Portugal.
2Institute of Public Health. University of Porto (ISPUP). EPIUnit - Epidemiology Research Unit. Porto, Portugal.
3Department of Immunology. Faculty of Medicine. University of Porto. Porto, Portugal.
4Research Centre in Physical Activity, Health and Leisure. Faculty of Sport. University of Porto. Porto, Portugal
This work was supported by ARIA Project PTDC/DTP-SAP/1522/2012 from Foundation for Science and Technology (Fundação para a Ciência e Tecnologia - FCT), co-financed by the European Regional Development Fund Through Operational Competitiveness Programme (COMPETE) FCOMP -01-0124-FEDER-028797; and by the Portuguese CCDR-N for funding the research project "E2BE" (NORTE-07-0124-FEDER-000036), through the European Union FEDER programme.
ABSTRACT
Introduction: The importance of hydration is undoubtable but reliable data on hydration status and its relation with diet is lacking.
Objectives: We aimed to evaluate the hydration status and its relation to beverages and food intake in children.
Methods: A sample of 172 (50% male), 7-11 year-old children was included in this survey. Participants completed a 24 h urine collection; a 24 hours food recall corresponding to the day of urine collection was applied, weight and height were measured and parents/caregivers filled a lifestyle and socio-demographic questionnaire. The free water reserve was used to assess the hydration status. The intakes of food and beverages were compared according to hydration status using the t-test, Mann-Whitney test or unconditional regression models as appropriate.
Results: More than half of the participants were classified as hypohydrated or at risk of hypohydration (57% in girls and 58% in boys). Compared to hypohydrated children, a significant higher consumption of water (276.2 ± 208.4 vs 188.2 ± 187.4 g/day) and fruit juices (77.6 ± 139.4 vs 14.4 ± 57.2 g/day) was reported by euhydrated boys and girls, respectively. Lower consumers of water and fruit juices showed a higher risk of hypohydration (OR = 2.16, 95% CI: 1.02-4.58, p = 0.045), adjusting for confounders.
Conclusions: Most of the children included in this analysis were classified as at risk of hypohydration and those with higher water and fruit juices consumption showed a better hydration status.
Key words: Free water reserve. Children. Dietary intake. Hydration status.
Introduction
Water is an essential nutrient for human life, the main constituent of the body, influencing the health status of individuals (1). The needs of this nutrient depend on its losses, which vary according to several factors (2).
Everyday water losses through the skin, lungs, stool and urine must be compensated with an appropriate intake. Losses through the skin and lungs vary with exercise, climate, clothing and other environmental conditions. The urinary losses are, in normal conditions, quantitatively the most important varying within a physiological range that depends on the load of solutes and fluid intake, in combination with the diluting and concentrating ability of the kidneys (2).
Children are an especially vulnerable group to dehydration since they may have a limited renal excretion ability and difficulty in expressing thirst sensation. In addition, children are susceptible to voluntary dehydration defined as the lack of complete rehydration after a dehydrating stimulus because of inadequate or lack of prolonged thirst (3).
Although acute dehydration is relatively easy to recognize and its consequences are well documented, chronic mild dehydration may pass unnoticed but have adverse consequences for the long-term health (4). In addition, children seem to be particularly at risk of impaired cognitive function (concentration, alertness and short-term memory) due to insufficient hydration (3).
Although hydration status in breastfed infants seems to be similar all over the world, children and adults from different settings show notable differences regarding hydration biomarkers (5). Thus, accurate estimates of water intake and hydration status among populations are essential to identify groups at risk of dehydration.
Since water may be obtained from beverages and foods, it is important to distinguish water sources in populations in order to design strategies to prevent dehydration.
Objectives
We aimed to evaluate children's hydration status and its relation to beverages and food intake.
Methods
A cross-sectional survey conducted between January and June 2014, included elementary school children (7-11 years old) from Portugal. Details about the aims and procedures involved in the study were explained to parents and caretakers of 488 children, attending the 3rd and 4th grade. Participants were also informed that participation was voluntary and that they were able to withdraw at any time. All students and their parents received written information on the project. Of the 202 (41.4%) children who agreed to participate, all collected a 24-h urine sample, and 30 (16.3%) were excluded for incomplete 24-h urine collection according to the coefficient of creatinine (described in detail below), remaining a final sample of 172 participants (86 girls).
Prior to data collection, parents provided written informed consent and children gave oral assent. All schools where the study was carried out and the Ethical Committee of the University of Porto approved the protocol of study.
Trained researchers collected data through structured interviews. Dietary intake was assessed by a 24-h dietary recall; anthropometric measures were taken, and a 24-h urine samples were collected. Parents/caretakers provided information on sociodemographic characteristics, namely age and sex, parental education level, and children's physical activity. Body weight measurement was obtained using an electronic scale (TANITA® TBF- 300A, capacity 200 kg, accuracy 100 g) and the height was obtained using an estadiometer (capacity 200 cm, accuracy 1 mm) with the head in the Frankfort plane. Participants wore lightweight clothing and no shoes. Body mass index (BMI) was computed as mass, weight (kg)/height2 (m). After calculating the BMI, it was plotted on the WHO BMI-for-age growth charts and obtained a percentile ranking, classifying children as follows: underweight (less than the 3rd percentile), normal weight (3rd to less than the 85th percentile), overweight (85th to less than the 97th percentile) or obese (equal to or greater than the 97th percentile) (6). The physical activity questionnaire included the time spent watching TV/video during most days of the week (< 2 h/day; and ≥ 2 h/day); sleeping duration (≤ 8 h/day; 9 h/day; and ≥ 10 h/day); and practice of sports activities besides the physical education classes at school (≤ 1 time/week; 2-3 times/week; > 4 times/week) (7). Parents and caretakers were given verbal and written instructions in assisting children to collect a 24-h urine sample and received a standard sterilized urine collection bottle. On the first morning of the urine collection, instructions were given to discard the first specimen, and from then on to collect all specimens for up to 24 h, including the first specimen of the following day. The samples were analyzed by certified laboratories for 24-h creatinine (mg/day), 24-h urine volume (ml), and 24-h urine osmolality (mOsm/kg).
The 24-h urine collections were assessed for completeness using creatinine excretion in relation to weight (i.e., creatinine coefficient), calculated by the following formula: creatinine coefficient ¼ creatinine mg ð Þ = day body weight kg ð Þ. Creatinine coefficients above of 0.1 mmol · kg-1 · day-1 were classified as indicating an acceptable 24-h urine collection (8).
The hydration status was evaluated based on the free water reserve (FWR) parameter (ml/24 h) calculated by subtracting 24 hour urine volume to obligatory urine volume (Solutes in urine 24 h [mOsm/day]/[830-3.4] x [age - 20]) and allows for the classification of the 24 hour hydration status (euhydrated vs hypohydrated subjects or at risk of hypohydration (9).
When participants delivered the 24-h urine collection, a 24-h dietary recall questionnaire was applied, taking into account the Manual de Quantificação dos Alimentos (10). Participants were questioned accurately about their food and drinks consumption, even reporting cooking methods, brands and consuming time and place. The software Food Processor® (ESHA Research, USA) was used to convert food into nutrients.
To identify under-reporters, Goldberg cut-offs were used as direct comparison of energy intake (EI) to energy expenditure (11). Goldberg cut-off values were applied to exclude under-reporters based on physical activity level (PAL) and compared with the ratio of EI to basal metabolic rate (BMR). BMR was calculated using the Schofield equations for children based on age, gender, height and weight (12).
Food records considered as implausible were found in 19 children. As there were no significant differences detected between the two groups for the hydration variables the total sample was included for the analysis.
Food and beverages groups were created in order to estimate their contribution to total water intake in water, fruit juices, soft drinks, milk/yogurt, tea/coffee, fruit, vegetables, and others (foods with reduced water content). We also considered high and low intake of these food groups based on, respectively, intakes at or above the median, and below the median. Statistical analysis was conducted using SPSS Statistical Package® 21.0 (IBM Corporation, 2012).
Continuous variables were presented as mean and standard deviation, and percentiles, and categorical variables were summarized as counts and percentages. Kolmogorov-Smirnov test was performed to test variables for normality. Independent samples t-test (parametric variables) and non-parametric test (Mann-Whitney U) were used to identify sex differences for urinary biomarkers. Categorical variables were tested using the Chi-squared test. For food/beverages groups whose contribution for water varied according to hydration status, unconditional logistic regression models were fitted in order to estimate the magnitude of the association between their contribution for water intake and the hydration status.
Results
The mean age of the 172 children evaluated was 8.7 ± 0.8 years. The prevalence of overweight and obesity was 37.2% (36% overweight and 1.2% obesity) in girls and 33.7% (30.2% overweight and 3.5% obesity) in boys. The proportion of children engaged in physical exercise ≤ 1 time/week was 54.8% in girls and 37.2% in boys, whereas the proportion of children who sleep ≤ 8 h/day was 21.1% in girls and 29.1% in boys. The proportions of children who spent two or more hours watching TV/video during most days of the week were 9.3% in boys and 4.7% in girls. Nearly half of parents reported to have ≤ 9 schooling years (Table I).
Nutritional intake is described in table II. The contribution of protein (16.8% in boys and 17.1% in girls) and sugar (20% in boys and 19% in girls) for total energy intake was higher than the recommended by the World Health Organization (WHO). There were no significant differences between sexes, except for the mean intake of carbohydrates which was higher in boys (287 g vs 263 g, p = 0.033), with no statistically significant differences when carbohydrates expressed as percentage of total energy intake were compared (52% in boys vs 50% in girls, p = 0.171).
The overall mean energy intake was 2,245 ± 560 kcal for boys and 2,116 ± 542 kcal for girls (p = 0.131) and the average total water intake was 2,411 ± 595 g in boys and 2,286 ± 649 (p = 0.194).
Table III presents the urinary biomarkers by sex. Compared to girls, boys showed higher mean 24 h osmolality (667 ± 158 mOsm/kg vs 585 ± 164 mOsm/Kg in girls, p = 0.003). The mean FWR was zero in both sexes (0 ± 0.5 ml in boys and girls) and the percentiles 25 and 50 were negative values both in boys (P25 = -239 ml, P50 = -32) and girls (P25 = -299 ml, P50 = -87). The prevalence of children with hypohydration or at risk of hypohydration was 58% in boys and 57% in girls.
Table IV shows the consumption of food and beverages according to hydration status. Euhydrated boys reported a higher water intake than hypohydrated/hypohydration risk ones (276 ± 208 ml vs 188 ± 187 ml, p = 0.041). Among girls, those classified as euhydrated showed a higher intake of fruit juices, compared to hypohydrated/hypohydration risk (78 ± 139 ml vs 14 ± 57 ml, p = 0.006). No other significant differences were observed regarding the groups of food and beverages consumed according hydration status.
Regarding nutritional intake according to hydration status, euhydrated boys showed higher average contribution of protein to total energy intake, compared to hypohydrated/hypohydration risk ones (18 ± 4% vs 16 ± 3%, p = 0.034). No other statistically significant differences were observed when comparing nutritional intake between euhydrated and hypohydrated or at hypohydration risk children.
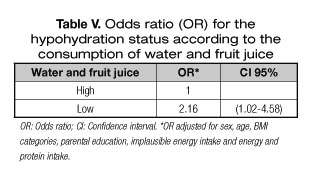
A lower consumption of water and fruit juices was associated with a higher risk of hypohydration (OR = 2.16, 95% CI: 1.02-4.58, p = 0.045), adjusted for confounders (Table V).
Discussion
Almost 60% of this sample of Portuguese children were classified as hypohydrated or at hypohydration risk according to the FWR parameter, which is considered to reflect the 24 h hydration status of individuals. Compared to other biomarkers, FWR has the advantage of considering the maximum capacity of kidney concentration and, in addition, it takes into account a safety margin to ensure adequate hydration (9).
The prevalence of inadequate hydration status is higher than the one reported by Manz in German children, although the mean 24 h urine osmolality (667 mOsm/kg in boys and 585 mOsm/kg in girls), an indirect parameter of hydration status, was similar to those described for German children (13), probably reflecting higher non-renal water losses by Portuguese children. This is a relevant aspect, given the particular susceptibility of children to voluntary hydration (14), especially after exposure to physical exercise (15) and in a warm country such as Portugal.
Mean urine osmolalities from healthy subjects from different settings are surprisingly diverse, indicating the large cultural differences that influence the hydration status of different societies. Friedrich Manz, a brilliant German researcher who proposed the free water reserve algorithm, argued that it was not possible to define a physiological or natural narrow urine osmolality range as it is always influenced by cultural context, namely food habits. This author suggested that only after additionally considering 24 h urine volume, urine solute excretion and maximum urine osmolality, it would be possible to quantify the individual 24 h hydration status (9).
In line with urine biomarkers, data from 24 h intake showed a mean total water intake of 2,411 ml and 2,286 ml in boys and girls, respectively. Although these values are above those documented in Germany, France and the USA (13,16,17), methodological differences, such as the methods used to assess dietary intake and the participants' age range, may contribute to explain the differences observed. Nevertheless, we found a very low proportion of children (18.6% of boys and 25.6% of girls) who met the European Food Safety Agency (EFSA) reference values for water (2), which ranged from 1.6 ml/day at the age of 4-8 and 2.1 ml/day at the age of 9-13.
The mean FWR was zero and the percentiles 25 and 50 were negative values on both sexes, emphasizing the need to intervene in this population in order to improve fluid intake and hydration status.
Euhydrated boys and girls reported a higher water and fruit juice consumption, respectively, than hypohydrated or at hypohydration risk children. Given the small sample size, for the logistic regression analysis we merged in one category water and fruit juice, and it was observed that a low (below the median) consumption of those beverages was associated with an increased odds of hypohydration oy hypohydration risk, adjusting for confounders. No other food or beverage group showed a significant association with hydration status. Water and fruit juices were significantly associated with a better hydration status, which may indicate action tips for caregivers, educators and politicians who should provide an environment where the access to beverages and food rich in water is encouraged.
In conclusion, a high proportion of this sample of Portuguese children were classified as hypohydrated or at risk of hypohydration, which reinforces the need to implement policies to increase the consumption of fluids and foods rich in water in children, an age group particularly vulnerable to the negative effects of hypohydration on cognitive performance (18). In addition, strategies promoting a good hydration status may be associated with the prevention of non-communicable diseases throughout life (1).
Declaration of interest
P.P. was a member of the Scientific Board of the Portuguese Institute of Hydration and Health between 2008 and 2015.
References
1. Manz F, Wentz A. The importance of good hydration for the prevention of chronic diseases. Nutr Rev 2005;63(6 Pt 2):S2-5. [ Links ]
2. EFSA Panel on Dietetic Products Nutrition and Allergies (NDA). Scientific opinion on dietary reference values for water. EFSA Journal 2010;8(3):1459. [ Links ]
3. Popkin BM, D'Anci KE, Rosenberg IH. Water, hydration, and health. Nutr Rev 2010;68(8):439-58. [ Links ]
4. Manz F. Hydration and disease. J Am Coll Nutr 2007;26(Suppl. 5):535s-41s. [ Links ]
5. Manz F. Hydration in children. J Am Coll Nutr 2007;26(Suppl. 5):562s-9s. [ Links ]
6. Growth reference 5.19 years. Available at: http://www.who.int/growthref/who2007_bmi_for_age/en/. [ Links ]
7. Moreira P, Santos S, Padrao P, Cordeiro T, Bessa M, Valente H, et al. Food patterns according to sociodemographics, physical activity, sleeping and obesity in Portuguese children. International Journal of Environmental Research and Public Health 2010;7(3):1121-38. [ Links ]
8. Remer T, Neubert A, Maser-Gluth C. Anthropometry-based reference values for 24-h urinary creatinine excretion during growth and their use in endocrine and nutritional research. Am J Clin Nutr 2002;75(3):561-9. [ Links ]
9. Manz F, Johner SA, Wentz A, Boeing H, Remer T. Water balance throughout the adult life span in a German population. Br J Nutr 2012;107(11):1673-81. [ Links ]
10. Marques M, Pinho O, Almeida MDV. Manual de quantificação de alimentos. Faculdade de Ciências da Nutrição e Alimentação da U. Porto (FCNAUP); 1996. [ Links ]
11. Rangan AM, Flood VM, Gill TP. Misreporting of energy intake in the 2007 Australian Children's Survey: Identification, characteristics and impact of misreporters. Nutrients 2011;3(2):186-99. [ Links ]
12. Schofield WN. Predicting basal metabolic rate, new standards and review of previous work. Human Nutrition Clinical Nutrition 1985;39(Suppl. 1):5-41. [ Links ]
13. Manz F, Wentz A. Hydration status in the United States and Germany. Nutr Rev 2005;63(6 Pt 2):S55-62. [ Links ]
14. Bar-David Y, Urkin J, Landau D, Bar-David Z, Pilpel D. Voluntary dehydration among elementary school children residing in a hot arid environment. J Hum Nutr Diet 2009;22(5):455-60. [ Links ]
15. Bar-Or O, Wilk B. Water and electrolyte replenishment in the exercising child. International Journal of Sport Nutrition 1996;6(2):93-9. [ Links ]
16. Kant AK, Graubard BI, Atchison EA. Intakes of plain water, moisture in foods and beverages, and total water in the adult US population - Nutritional, meal pattern, and body weight correlates: National Health and Nutrition Examination Surveys 1999-2006. Am J Clin Nutr 2009;90(3):655-63. [ Links ]
17. Bellisle F, Thornton SN, Hebel P, Denizeau M, Tahiri M. A study of fluid intake from beverages in a sample of healthy French children, adolescents and adults. Eur J Clin Nutr 2010;64(4):350-5. [ Links ]
18. Bar-David Y, Urkin J, Kozminsky E. The effect of voluntary dehydration on cognitive functions of elementary school children. Acta Paediatrica (Oslo, Norway: 1992) 2005;94(11):1667-73. [ Links ]
![]() Correspondence:
Correspondence:
Patrícia Padrão.
Faculty of Nutrition and Food Sciences.
University of Porto (FCNAUP).
Porto, Portugal
e-mail: patriciapadrao@fcna.up.pt