INTRODUCTION
Childhood food practices directly impact a child's nutritional status and health. If they are adequate, the child's growth will be healthy; if they are not, it will hinder growth and the consequences will extend into adult life 1. The multiple benefits that breastfeeding (BF) provides to the mother and child affect the immune nutritional, body, and psychological status of the child, and has economic advantages also 2.
The World Health Organization (WHO) recommends exclusive breastfeeding (EBF) up to six months of age followed by the introduction of safe and appropriate foods for this age, maintaining BF for two years or beyond 3. In Mexico, according to the National Survey of Health and Nutrition 2012 (ENSANUT 2012), the percentage of EBF in children less than six months of age has declined to 14.4% in comparison to 22.3% reported in 2006 4. As has been reported, the lack of EBF in the first months of life increases the probability of introducing foods prematurely, increasing the risk of allergies and infectious diseases 5. It has also been associated with chronic diseases such as diabetes, cardiovascular disease, and obesity in childhood 1. Furthermore, the absence of EBF, especially in low-income families, impacts the family's economy due to the need to buy maternal milk substitutes 6.
The age when complementary feeding (CF) is introduced is a particularly important moment in the child's development 7. The way the mother starts CF will determine the contribution of energy and nutrients to the child's growth and development without weaning, a situation that can prevent or favor iron and zinc deficiency, foment or not the inherent ability of the child to control food intake as well as determine the pleasure or displeasure for different food flavors, smells, and textures 8. Likewise, the introduction of foods will influence the acquisition of abilities that facilitate a smooth transition from total dependence on the parents to self-feeding, such as chewing, using a spoon and cup, etc. As shown, this period represents a key moment in the establishment of eating patterns. These are crucial moments in which there could be a stunting because of an inadequate nutritional intake or the development of overweight due to an excessive or hypercaloric intake 9. Mexico ranks first in childhood obesity 10, a situation that occurs at a young age and is associated with short stature, a hypothesis that has been tested in several studies 11.
Introducing children to the family diet is recommended at 12 months of age when the development of the nervous, digestive and renal system is similar to that of the adult 12; in other words, when the child is capable of consuming something from most food groups. Ideally, the child should have access to a diverse diet. According to the Food and Agriculture Organization (FAO) of the United Nations and the WHO, dietary diversity is a qualitative measure of food consumption that reflects household access to food and is a key factor for ensuring adequate consumption of nutrients and health promotion 13. Scientific evidence considers it a factor that protects against growth failure, a frequent nutritional problem in the country. It has been associated with nutritional adaptation, availability of foods in the home, and better food habits in adults 14.
In Mexico, less than 60% of children between six and eight months of age in rural communities consume a diet that meets nutritional recommendations 15. In Hidalgo, 78.3% of children under five years of age receive only the minimum recommended food diversity 16. The promotion of EBF and adequate CF as well as the maintenance of a diversified diet are fundamental for reducing child mortality and the burden of disease associated with nutrition in Mexico. The aim of this study is to characterize feeding practices in children under two years of age in rural communities of Hidalgo and determine their relationship with stunting. The findings can be used to identify and show the problems of nutrition and dietary patterns in infancy, and provide opportunities for designing and implementing programs for improving the diets and health of infants, in order to avoid the consequences in growth and short and long-term health.
MATERIAL AND METHODS
STUDY POPULATION
This was a descriptive cross-sectional study of a convenience sample of 189 mother-child dyads in children 1-24 months of age. The rural communities selected and evaluated during the national vaccination campaign were: Yolotepec, Patria Nueva, Ojo de Agua, San José Tepenené, La Estancia, and Dextho de Victoria, all within the Health Jurisdiction of Actopan, in the state of Hidalgo. Exclusion criteria were diseases requiring a special diet, not being a resident of the aforementioned communities, and not being the child's caretaker. Mothers and tutors provided written informed consent. The study was previously approved by the Ethics and Research Committees of the Health Services of Hidalgo.
CHILD NUTRITION
A 24-hour recall was applied to determine CF and minimum dietary diversity (MDD) in children six to 24 months of age. The latter was defined as the diet that includes at least four of the following seven food groups: a) cereals/tubers; b) legumes/oleaginous foods; c) milk derivatives (cheese, yogurt or milk substitutes); d) animal products (red meats, fish, chicken, viscera); e) eggs; f) fruits/vegetables rich in vitamin A; and g) other fruits and vegetables 17. The total group of children was divided into: a) breastfed children; and b) not breastfed children the day before, day or night. In breastfed children less than six months of age, maternal milk is exclusive when no other food or drink (including water) is offered. It is predominant (PBF) when infant formulas are used, and complimentary (CF), when foods other than maternal milk are offered 18. Women who did not breastfeed their child or combined it with formula were asked why. A questionnaire to obtain the mother's (age, education, occupation) and the child's (sex, birth date, and if they were born by cesarean section) sociodemographic data was applied.
ANTHROPOMETRIC MEASURES
Children were weighed and measured using standardized methods by trained personnel. A SECA(r) model 874 scale (Seca GmbH & Co. KG, Hamburg, Germany) with a mother-baby function was used, together with a SECA(r) 217 stadiometer. Length-for-age was determined with WHO Anthro version 3.2.2.
RESULTS
A total of 189 mother-child dyads were evaluated. Mean age in months was 10.5 ± 0.46; 59% were girls and 40% were boys. Classified by age groups, 33.3% were between 1-6 months, 31.7% between 7-12 months, and 34.9% between 13-24 months. Mean age of the mothers was 25.5 ± 5.6 years. Regarding occupation, 82.5% were housewives, 13.2% worked, and 4.2% were students. Mean years of education was calculated as 10.3 ± 2.6 years. In relation to births, 44.1% were primiparous, and according to type of delivery, 48.1% were vaginal and 51.9% were by cesarean section. Additionally, 92.6% of children were breastfed during the first two weeks after birth; 14.6% said they did not know the advantages to breastfeeding. In relation to advice about breastfeeding, 26.8% said they received no advice, 68.7% were counseled by healthcare personnel, and 4.5% received advice from their mother or mother-in-law.
An overview of feeding practices by age groups is shown in Figure 1. As shown in this figure, 37% of children 1-6 months old were EBF, and the mean number of times children were breastfed per day was 6.4 ± 3.9, 95% CI: 0.5-7.3); 16.0% were PBF, 6.0% were fed with infant formula, and 33.0% had begun CF and were breastfed. Eight percent were not being breastfed but were consuming other foods. All of the children in the 7-12 month age group had started CF; however, 63% were still breastfed and 37% were not; the mean number of times children were breastfed per day was 2.6 ± 2.4 times (95% CI: 1.9-3.2). In the 13-24 months group, 29% were breastfed and the mean number of times children were breastfed per day was 0.98 ± 1.6 times (95% CI: 0.57-1.4), while 71.0% were not consuming maternal milk anymore.

CF: complimentary foods; BF: breastfed; PBF: predominantly breastfed; EBF: exclusively breastfed.
Figure 1 Characteristics of food practices in the study population by age groups (%).
The trend followed by food practices is shown in Figure 2. Regarding EBF, 73% of the children one month of age had received it. Nevertheless, when EBF in children two months of age was analyzed, there was a drastic decline, since only 30% were receiving it. Children three and four months of age had a similar percentage (43% and 40%, respectively) and those five months of age, 29%. Nine percent of children six months of age were EBF. Continuous breastfeeding counted from the sixth month was 54.0% for children six months of age and 91.0% for those seven months of age. In the eighth and ninth months, a decline of 50.0% and 54%, respectively, was seen. However, the trend increased again in children ten and eleven months of age (80% and 78%, respectively). After 12 months of age, continuous breastfeeding declined considerably.

Figure 2 Percentage of exclusively breastfed (EBF), continuously breastfed (CBF), complimentary foods (CF) and short stature in children 1-24 months of age.
CF were present starting at the third month of age in 57% of children, in 33% at four months, in 63% at five months, and in 90% at six months. Regarding stunting included in this figure, our study reported 10.1% in the total sample, excluding the risk of short stature classification (31.9%).
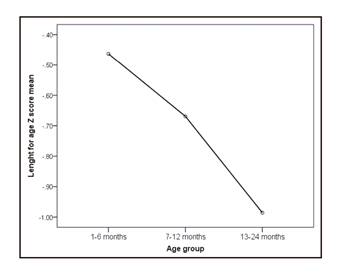
Mean ZLA were different by age group. Younger children (1-6 months) showed a score of -0.463 ± 1.445, and the values closest to low height were in the 7-12 month group (-0.669 ± 1.225). This was even greater in those 13-24 months of age (-0.985 ± 0.917; p < 0.05) (Table I). This trend is better seen in Figure 3, where, notwithstanding, the three means are negative values; in other words, they tend towards low height.
Table I Z-score means of the growth indicators length for age and weight for age in children aged 1-24 months by age and by type of lactation
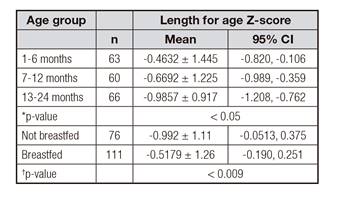
*ANOVA; †Student's t-test.
The study population according to type of breastfeeding is described in Table II. Of the total sample, 40.7% were not breastfed the day before and 59.3% were.
In those 1-6 months, the proportion of children who were not breastfed (11.7%) was lower than that of those who were (48.2%), while in the 7-12 month group the proportions were similar (27.3% and 34.8%, respectively). In those older than 12 months, the number of children who were not breastfed was greater (61.0%; p < 0.000).
Table II Study population according to type of breastfeeding
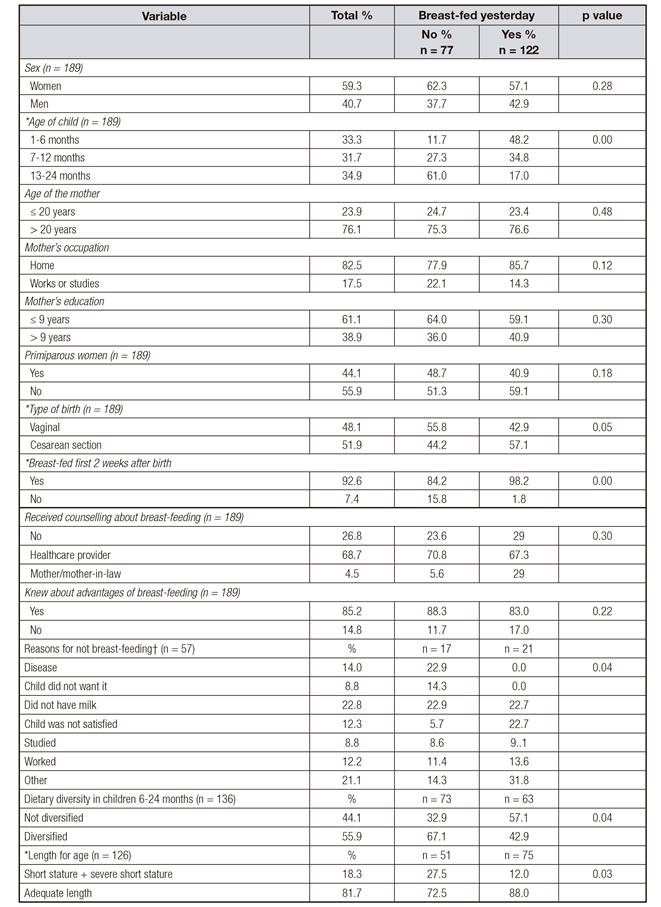
*Differences between breast-fed and not breast-fed children p < 0.05. †Exclusive breast-feeding.
With regard to the type of birth, the high number of cesarean sections is notable (51.9%). Of those born by cesarean section, 44% were not breastfed and 57.1% were. Of the children born by vaginal delivery, a greater number were not breastfed (55.8%), against 42.9% who were (p < 0.05). On the other hand, the mothers of 1.8% of the group of children who were not breastfed the day before the survey indicated that they did not do it in the first two weeks, which means that they resumed the practice later. In the group of children who were not breastfed, there was a large percentage that was breastfed in the first days of life (84.2%). The rest (15.8%) were not breastfed at any time regardless of their age (p < 0.000).
When the mothers were asked why they fed their children formula or alternated breast milk and formula during the first six months of life, 38.6% of those who breastfed the previous day stated that they did not have enough milk (22.7%); they had a feeling that the child was not satiated (22.7%); they studied (9.1%) or worked (13.6%); and others (31.8%) complained of weakness, a cesarean birth, pregnancy, lactose intolerance, and advice of a healthcare provider or use of contraceptives. Of the women who did not breastfeed, 22.9% answered that they were sick, 14.3% that the child did not want it, 22.8% that did not have milk, 5.7% said that their child was not satiated, 8.6% argued that they studied and 11.4%, that they worked (p < 0.04).
Stunting was also related to the absence or presence of BF. Regarding this relationship, it is notable that children who were not breastfed had a greater proportion of short stature (27.5%) than those who were breastfed (12.0%).
Finally, and according to the results of MDD in children six to 24 months, 55.9% received a diverse diet that included at least four of the seven food groups described in the methodology. In relation to not breastfed (67.1%) and breastfed (42.9%) children, it was found that the former had a higher proportion of MDD (p < 0.04). On the other hand, when this variable was compared, it was found that less than half of the children six to 12 months of age did not reach DMM (42.9%) and that those 13 to 24 months represented a greater proportion (69.7%) (p < 0.02) (Table III). It is important to point out that this difference could be influenced by inadequate introduction of CF in the first group.
DISCUSSION
The percentage of EBF found in our study was 22.3%, in contrast with the results of the last state report in rural population, which was 18.5% 18. A good precedent is that more than 90% of the mothers exclusively breastfed their baby at least during the first two weeks after birth. At one month of age, the percentage was still high (73.0%); however, after this month the decline is drastic, since only 30% provided EBF. A study carried out in a low-income population in South America found a similar trend: 95.4% of children began with EBF, followed by a gradual decline 19. Another study carried out in the rural area of Gambia, where children have a high risk of malnutrition, reported that the mean interruption of EBF was 5.2 months and that the decline in growth began at 3.5 months of age 20. This study was able to identify that stunting becomes evident in the fourth month of age, a problem that in our study corresponded graphically to the month of decline of EBF and the early introduction of CF in the third month of age. It is important to point out that the problem with introducing foods at an early age (under four months) is that it favors a reduction in maternal milk consumption. With food, a child becomes satiated more quickly, which impedes reaching nutritional goals. In addition, there is a tendency to offer watery porridges, and a low energy density food, such as fruits and vegetables, which favors the risk of undernourishment 21; or overfeeding, which leads to overweightness 22.
The ENSANUT 2012 reported that 75% of children consumed fruits and vegetables before six months of age 4. Nevertheless, the recommendation is to begin CF at six months 23, considering that the signs that indicate that the infant is capable of receiving solid foods, such as axial tone and head control, motor coordination between the eyes, hands and mouth as well as the disappearance of the extrusion reflex, are present. It is also known that taste buds reach their maximum development at six months 24.
Stunting in this study population was determined as 10.1%; however, the high percentage of children classified at risk of short stature (31.9%) is noteworthy. Likewise, children who were not breastfed had a higher proportion of stunting than children who were breastfed, a finding that confirms the nutritional relevance of maternal milk during this stage.
Chronic malnutrition occurs because of a constant and inefficient consumption of energy and nutriments in the first years of life; this is the most common nutritional deficit in Mexico. Chronic malnutrition first affects weight and later, lineal growth. In Hidalgo, stunting was estimated in 2012 as 12.9% in children under five years of age, a figure similar to the estimated prevalence in Latin America in 2015 (11.6%, 5.9 million children) 25. Nevertheless, when the urban setting (9.6%) is separated from the rural setting in Hidalgo, it is seen that the latter is more affected (16%) 16. The delay in growth increases the risk of mortality from infectious diseases during infancy and deteriorates cognitive development. It is also associated with low financial resources and a low education in adolescents and adults 26. There is evidence that children who do not reach their development in height or muscle mass require less energy to gain weight in comparison with those who did because of changes in hormone response due to abnormal deceleration of lineal growth, an event that increases the risk of obesity 11.
In addition to EBF in the first six months of life, the WHO recommends that maternal milk be continued until two years of age or more if the child and the mother are willing 3. In our work, the decline in breastfeeding occurred starting at the 13th month (with 30% of children being breastfed, and the mean number of times children were breastfed being 2.6 times per day, 95% CI: 1.9-3.2); this was not greater after this age. Several studies have reported that long-lasting breastfeeding has a protective effect against obesity in childhood; however, this practice is rapidly disappearing 1,27.
In the past several years, a decline in the provision of maternal milk has been reported in groups with greater social vulnerability, such as those who live in rural communities, those with a low income, those who do not have health services and mothers who do not have a paying job 28. It is important to mention that maternal milk has also been related to economical convenience related to family savings associated with the purchase of formula and accessories as well as a smaller number of medical consultations and drug purchases 29; however, the abandonment of maternal milk is still notable. Scientific evidence suggests that the incorporation of women in the workplace could also be a factor for premature abandonment 30; however, most women in the evaluated study population were housewives (82.5%).
Although there were no significant differences with regard to knowledge and lack of knowledge of mothers regarding the advantages of breastfeeding and the fact that they did or did not receive counseling, the proportion of women who said that they did not receive counseling (26%) or who did not know the advantages of breastfeeding (15%) was noteworthy. Some advantages for infants are protection from diarrhea and other infections, protection against obesity and chronic diseases in adulthood, and healthy growth; in women, breastfeeding delays fertility, helps them lose the weight gained during pregnancy, decreases the risk of cancer (breast and ovarian) and improves the relationship between the mother and baby 1. On the other hand, 35% of women who did not breastfeed said that "the child was not satisfied" or that "she had no milk." Scientific evidence suggests that regardless of maternal body mass index, lactating women are able to produce sufficient volume and macronutrient concentrations to support the child's needs, but tests are limited regarding micronutrient concentrations over a long period of time in those who experience nutritional vulnerability 31. This is why we believe that the nutritional status of the mother should be assessed in later studies with the aim of identifying if it is a mother's perception or a physiological cause 32. Nevertheless, the decision to breastfeed is strongly influenced by the information that mothers receive through physical, psychological, and social support provided during pregnancy, birth, and puerperium, and family, medical, and cultural attitudes, which can favor or hinder breastfeeding 33. A lack of counseling and a fear of breastfeeding can also possibly influence the decision to carry it out. A study performed in low-income African-Americans identified that the difference between women who breastfed for long periods and those who did it for a short period of time or did not do it at all was related to a clear intention of breastfeeding with positive experiences in hospital nutrition programs and with feeling more comfortable breastfeeding in public 34.
Also, the industry has been responsible for low breastfeeding rates and its consequences, with aggressive practices of commercialization of food for infants, such as the distribution of misleading information on food for infants with maternal milk substitutes, the distribution of free samples to mothers, and the direct and indirect publicity about the feeding of infants with maternal milk substitutes 35.
Regarding the quality of CF, Mexico has registered positive changes in recent years 16. In this study, the significant difference observed between the 6 to 12-month age group and the 12 to 24-month age group suggests a low level of knowledge about when, how, and what foods to introduce correctly. According to current recommendations, the group of meats, cereals, vegetables and fruits should be introduced starting at the sixth month of life, beginning each separately, observing their tolerance, and with an appropriate consistency; legumes should be started at seven to eight months of age; and milk derivatives, egg and fish, at eight to 12 months of age. The recommendation of meat at six months of age has to do, first, with avoiding iron deficiency since body iron reserves are depleted at that age, and second, with the high biological value proteins that meat provides 23. It is important to mention that the mother's fear regarding the ability of the child to eat these foods reduces the opportunity to offer them; 36 this should also be considered, together with the low availability and accessibility characteristic of this food group in rural communities.
In Mexico, a nationally-representative sample of infants showed that the alarming dietary problems arise before 12 months of age. They develop quickly during the second year of life and persist during the first few years of life, emphasizing the low prevalence of the consumption of meats and iron-fortified cereals for infants, in the second half of their infancy, especially children from 6-8,9 months of age 37. On the other hand, MDD in children 6-24 months was 55.9% (a diverse diet includes at least four of the seven food groups). In Hidalgo, this percentage was 78.3% of children under five years. Nevertheless, it calls our attention that children that were breastfed the day before (42.9%) had lower proportions of MDD than those who had not been breastfed (67.1%) (p < 0.04). It is important to remember that, in this period, a high or low consumption of calories and nutrients from foods rapidly affects the increase or loss of weight in children 38. In this work, the difference in the means of the ZLA indicator evidenced the progression of the risk of short stature in relation to age.
Maternal education on breastfeeding and CF as well as improvements in childhood dietary diversity have been found to be a major factor in reducing stunting, according to a study carried out in children at risk of malnutrition, which reported a total indicator change of up to 20 percent 39. Accordingly, the evident decline of breastfeeding makes it necessary to propose and perfect strategies that aim at increasing its prevalence among women, both in rural and urban environments 40. Likewise, the inappropriate promotion of formulas must be eliminated, and support during pregnancy and planned breastfeeding should be promoted. Finally, the introduction of complementary foods represents a critical period in which basic questions regarding when, what, and how they should be started and established with the correct feeding pattern should be answered. The evidence that this project presents suggests that there is a low level of knowledge about this topic, which is why we propose approaching this with nutritional counseling.