Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Revista Española de Enfermedades Digestivas
versión impresa ISSN 1130-0108
Rev. esp. enferm. dig. vol.99 no.10 Madrid oct. 2007
CARTAS AL DIRECTOR
Chronic or recurrent appendicitis?
¿Apendicitis crónica o recurrente?
Palabras clave: Apendicitis. Apendicitis recurrente. Apendicitis crónica.
Key words: Appendicitis. Recurrent appendicitis. Chronic appendicits.
Dear Editor:
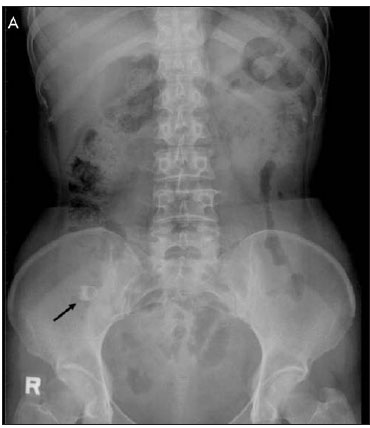
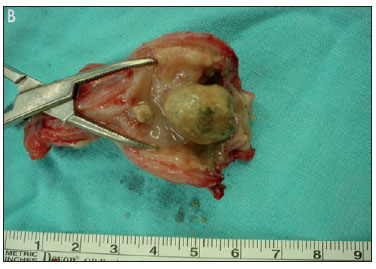
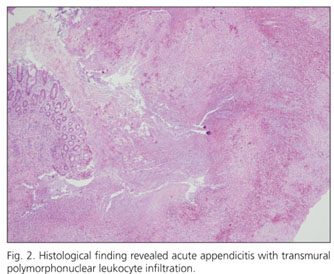
In August 2006, a 48-year-old woman, presented with epigastric dull pain off and on for two months. She ever called at local clinic twice, where gastric endoscopy was done and no obvious inflammation or ulcer were found. Physical examination showed no specific finding. X-ray of abdomen (KUB) showed a fecalith over right lower quadrant abdomen (Fig. 1A), further computed tomography (CT) proved appendicitis. Then appendectomy was done. The specimen revealed a grossly swollen, indurated and thickening wall appendix with a 2 cm fecalith in it and dilated lumen (Fig. 1B). Histological finding revealed acute appendicitis (Fig. 2). We wonder why the patient presented with symptoms for two months and the final pathological result showed acute inflammation, not chronic? Dose chronic appendicitis exit? Herein, we retrospectively analyzed 16 cases of appendicitis with the symptoms over three weeks.
Methods
From August 1996 to August 2006, 16 cases of adult patients (9 men and 7 women, mean age, 21.75 years old, range from 18 to 72 years) having appendicitis with symptoms over three weeks were reviewed. Histological finding showed not appendicitis were excluded in this series. Patients ever received antibiotics treatment during the period of symptoms were also excluded. The clinical characteristics, including age, gender, clinical presentation, physical examination, laboratory data, abdominal plain film radiograph, ultrasound, and CT results were recorded. The operative and histological findings were also recorded.
Histological identification
Acute appendicitis is identified with mucosal inflammation, necrosis and neutrophils infiltrates into or through the wall of appendix. As to identification of chronic appendicitis, Falk et al. report fibrosis, chronic inflammatory infiltrates, and neural cell proliferation are the most specific pathologic features in chronic appendicitis (1).
Results
Sixteen patients identified over 10 years were identified in this retrospective study. Nine patients were male and seven patients were female.
Clinical presentation
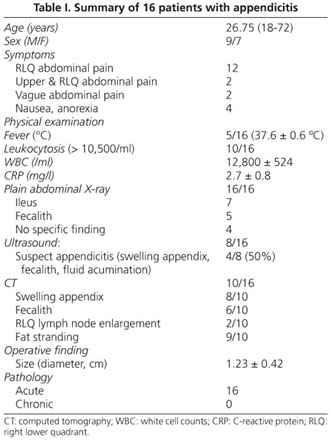
As table I showed, mean patient age was 26.75 years (range: 18 to 72 years). Twelve patients presented with right lower quadrant (RLQ) abdominal pain, 2 patients with upper and RLQ abdominal pain, and 2 patients presented with vague abdominal pain. Five patients presented with fever (mean body temperature of 16 patients was 37.6 ± 0.6 °C). Ten patients had presented with leukocytosis. Mean white blood cell count (WBC) was 12,800 ± 524 (/ml). Mean C-reactive protein (CRP) was 2.7 ± 0.8 (mg/l).
Imaging finding
Plain film radiographs (KUB) of all 16 patients were reviewed. Seven patients had ileus. Five patients had suspect fecalith over RLQ. The other four patients didn't have specific finding.
Sonography of the abdomen was performed in 8 of the 16 patients. Of these, only 4 patients had been suspected as appendicitis (swelling appendix, fecalith or fluid collected in the pelvis).
CT of abdomen was performed in 10 of the 16 patients, including swelling appendix was found in 8 patients, fecalith in 6 patients, RLQ lymph node enlargement in 2 patients, and fat stranding in 9 patients.
Operative finding and histological finding
The mean diameter of appendix was 1.23 ± 0.42. Histopathology revealed that all 16 patients proved to have acute inflammation of appendix. No chronic inflammation was found.
Discussion
Acute appendicitis is common and its symptoms usually intense. Most of the cases are easily identified. Although acute appendicitis is the most common disease of appendix, chronic appendicitis is uncommon. It usually refers to milder form of the illness and its symptoms are less pronounced, in some cases even undetectable (2,3). Chronic appendicitis was diagnosed when lymphocytes and eosinophils were presented within the wall of appendix, with or without associated fibrosis in the histopathological examination (3). If the patient presented with recurrent attacks of abdominal pain and histology revealed acute inflammation, we can't define it as "chronic" appendicitis, but we called "recurrent" appendicitis (4).
Chronic appendicitis is rare; about 1.5 to 10% of all appendix inflammations (1,3). But in our study, we reviewed the patients with three weeks symptoms of abdominal pain and their histological finding. We found all patients were acute inflammation. That implied chronic appendicitis is really rare. Besides, we were surprised why symptoms seems not consistent with histological finding? We think the possible explanations were partial obstruction of appendiceal lumen or mild infection.
Luminal obstruction is the usual initiating cause of acute appendicitis. The obstruction may be due to fecalith, lymphoid hyperplasia, tumor, foreign body, parasite or anatomic variance. Obstruction can also be partial or intermittent (5). While the fecalith (or foreign body, parasites, etc.) was small, this may induce partial obstruction of appendiceal lumen. The symptoms may be intermittent and could be resolved by conservative treatment. Once the fecalith "grows up", it may induce complete obstruction, and the mild infection may develop into severe infection.
Although acute appendicitis is common and most of them could be easily diagnosed. Chronic or recurrent appendicitis may present with vague gastrointestinal symptoms, that's easily been neglected. But most of cases presented with recurrent RLQ abdominal pain. That's relatively easily gives us a hint of appendicitis. As to patients with upper or vague abdominal pain, it would be more difficultly in making diagnosis; we have to keep it in mind.
In conclusion, chronic appendicitis is rare. We suggest that we had better use the name of "recurrent appendicitis" but not "chronic appendicitis". Appendicitis should be considered as a differential diagnosis in patients with chronic abdominal pain. In this kind of patients, they may not present with fever or leukocytosis. Once the plain film showed the fecalith over right lower abdomen, the appendicitis should be highly suspected.
Funding acknowledgement: Civilian Administration Division of Tri-Service General Hospital, National Defense Medical Center
Lai DH, Chuang CH1, Yu JC1, Hsieh CB1, Wu HS2 and Lin CH1
Department of Surgery. Yee-Zen General Hospital. Taoyuan, Taiwan. 1Division of General Surgery.
Department of Surgery. Tri-Service General Hospital. National Defense Medical Center. Taipei, Taiwan.
2Department of Surgery. Show Chwan Memorial Hospital. Changhua, Taiwan
References
1. Falk S, Schutze U, Guth H, Stutte HJ. Chronic recurrent appendicitis. A clinicopathologic study of 47 cases. Eur J Pediatr Surg 1991; 1: 277-81.
2. Savrin RA, Clausen K, Martine EW, Cooperma M. Chronic and recurrent appendicitis. Am J Surg 1979; 137: 355-7.
3. Mattei P, Sola JE, Yeo CJ. Chronic and recurrent appendicitis are uncommon entities often misdiagnosed. J Am Coll Surg 1994; 178: 385-9.
4. Andiran F, Dayi S, Çaydere M, Üstün H. Chronic recurrent appendicitis in children: An insidious and neglected cause of surgical abdomen. Turk J Med Sci 2002; 32: 351-4.
5. Van Winter JT, Wilkinson JM, Goerss MW, Davis PM. Chronic appendicitis: dose it exist? J Fam Pract 1998; 46: 507-9.