Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Revista Española de Enfermedades Digestivas
versión impresa ISSN 1130-0108
Rev. esp. enferm. dig. vol.103 no.6 Madrid jun. 2011
https://dx.doi.org/10.4321/S1130-01082011000600009
Percutaneous endoscopic suturing is an alternative treatment for persistent gastrocutaneous post-PEG fistula
La sutura endoscópico-percutánea es una alternativa terapéutica en la fístula gastrocutánea persistente post-PEG
Miguel Sobrino-Faya1,2, Fernando Macías-García1,2, Raquel Souto-Rodríguez1,2, Lucía Lesquereux-Martínez3 and Juan Enrique Domínguez-Muñoz1,2
1Department of Digestive Diseases. 2Foundation for Research in Digestive Diseases (FIENAD), and 3Department of General and Digestive Surgery. University Hospital of Santiago de Compostela. A Coruña, Spain
ABSTRACT
Persistent gastrocutaneous fistula after the removal of a gastrostomy tube is an unusual complication associated with percutaneous endoscopic gastrostomy (PEG). Surgical closure has been usually the treatment of choice. Several endoscopic methods have been previously attempted to close the fistula, usually with poor results. We report a successful case of percutaneous endoscopic suturing of a persistent gastrocutaneous post-PEG fistula, using a monofilament absorbable suture. A biopsy forceps was used to de-epithelialize both ends of the fistulous tract to promote granulation tissue formation. The gastrocutaneous fistula closed completely after the procedure and there were no complications during the follow-up.
Key words: Percutaneous endoscopic gastrostomy (PEG). Gastrocutaneous fistula. Percutaneous endoscopic suturing.
RESUMEN
La persistencia de la fístula gastrocutánea tras la retirada de la sonda de gastrostomía es una complicación inusual descrita en relación con la gastrostomía endoscópica percutánea (PEG). La cirugía suele constituir su tratamiento de elección. Se ha intentado el cierre con varios métodos endoscópicos, habitualmente con escasos resultados. Presentamos el cierre con éxito de una fístula persistente gastrocutánea tras la retirada de la sonda de PEG, mediante una sutura combinada endoscópico-percutánea usando un monofilamento reabsorbible. Se tomaron biopsias de ambos extremos de la fístula para escarificar el tejido y promover la formación de tejido de granulación. La fístula gastrocutánea se cerró completamente tras el procedimiento y no se presentaron complicaciones durante el seguimiento.
Palabras clave: Gastrostomía endoscópica percutánea (PEG). Fístula gastrocutánea. Sutura endoscópico-percutánea.
Introduction
The use of percutaneous endoscopic gastrostomy (PEG) is common, not only for long-term enteral nutrition but also in those patients with temporary inability to maintain oral intake caused by any condition affecting oro-pharynx.
Since its introduction by Gauderer and collaborators in 1980 (1), one of the complications associated with the use of PEG is the persistence of the gastrocutaneous fistula after the removal of the gastrostomy tube with the consequent leaking of gastric contents. Because PEG patients are often poor surgical candidates, the closure of the fistula with various endoscopic methods has been previously attempted trying to avoid laparotomy. Those methods include the use of cyanoacrylate, fibrin sealant (2), endoclips and argon beam electrocoagulation (3). Unfortunately, in many cases they do not lead to the expected result.
We introduce a new case of percutaneous endoscopic suturing of a persistent gastrocutaneous post-PEG fistula according to the method described previously by Alberti-Flor et al. in 2002 (4) and Eskaros et al. in 2009 (5), but with some slight modifications.
Case report
The procedure was performed in a 51-year-old male, with a supraglottis squamous cell carcinoma, stage IV (T3N2bM0), treated six years ago with neoadjuvant chemoradiation and surgery (left cervical lymph node dissection). A 22F PEG tube had been placed during treatment to ensure adequate nutritional intake; it was removed seventeen months before our scheduled suture procedure, leaving a persistent gastrocutaneous fistula. Throughout these seventeen months a continuous daily leakage was observed around the cutaneous side of the fistula. Conservative management with proton pump inhibitors and prokinetic agents did not improve leakage, so the patient was referred to our department.
After a detailed explanation of upper endoscopy and percutaneous-endoscopic suturing procedures, informed consent was obtained from the patient. Premedication consisted of intravenous administration of midazolam (5 mg) and meperidine (25 mg) for conscious sedation. Antibiotic prophylaxis was also administered -ceftriaxone 2 g intravenous (only dose), followed by oral amoxicillin-clavulanic acid, 875/125 mg t.i.d. for 1 week-.
The cutaneous end of the fistula was identified and cleaned with povidone-iodine and then was anesthetized with local injection of 2% mepivacaine.
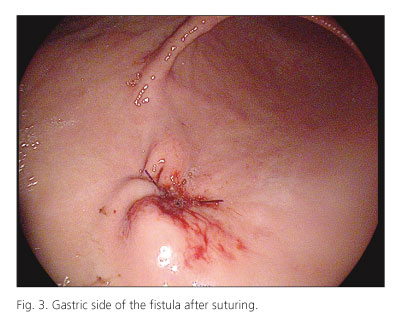
The gastric end of the fistula was located under endoscopic view (Fig. 1). Several biopsies were taken from both ends of the fistula by using standard biopsy forceps to de-epithelialize the fistulous tract (Fig. 2 D). Scarification with argon plasma electrocoagulation had previously been attempted, but the diameter of the fistula was insufficient to insert the argon probe. Under endoscopic guidance, a 14-gauge trocar was inserted through the abdo-minal wall next to the fistula. A 120-cm-long 2-0 mo-nofilament absorbable suture (PDS II®) was inserted through the trocar and was grasped with a snare inside the stomach and pulled out through the mouth. The first two steps were then repeated so that four monofilament sutures traversed the abdominal and gastric walls on the four quadrants of the fistula in a criss-cross fashion (Figs. 2 A-C); all suture ends were externalized through the mouth. Two surgical crossed-knots were made with the sutures recovered through the mouth. The ends of the sutures in the cutaneous side were then pulled, so the knots made outside the mouth were pulled into the gastric lumen to close the gastric side of the fistula (Fig. 3). Finally, another two surgical knots were made at the cutaneous side of the fistula (Figs. 4 A-B). A sterile, dry dressing was applied to the sutured area.
Proton pump inhibitors were prescribed (b.i.d.) after procedure, and oral feeding (liquid diet) was reintroduced six hours after the procedure. Entire procedure was performed on an outpatient basis and was carried out without significant incidents.
Results
In the early days following the closure of the fistula, the patient had sporadic and mild epigastric discomfort that was controlled with oral paracetamol. There were neither evidences of leakage of gastric content nor signs of local infection during the follow-up period.
In the sixth week the gastric side of the fistula was evaluated endoscopically, confirming its good healing and discovering the incorporation of the absorbable suture to the gastric mucosa (Fig. 5). During this visit, the external knots were cut because they were causing mild skin erosion. The rest of the suture was left in place to be absorbed.
After twelve weeks follow-up the patient had remained asymptomatic with proper healing of both sides of the fistula, so he was discharged from our department.
Discussion
The formation of a gastrocutaneous fistula is the goal and outcome after PEG placement. After tube removal, the fistula usually resolves without problems in a short time and without requiring any treatment. Infrequently, the fistula can continue leaking and alternative therapeutic approach could be needed (6). Poor tissue healing, delayed gastric emptying, acid hypersecretion or fibrosis are factors associated with this non-closure of the fistula. The endoscopic closure of a fistula has been previously described, but surgery has been so far the therapy of choice for persistent gastrocutaneous fistula.
Our patient had an acceptable anesthetic risk but, after being informed of the risk- benefit of all procedures, he preferred to carry out an attempt of percutaneous endoscopic suturing instead of a new surgical intervention.
Since the patient was in such good condition we decided to perform the entire process on an outpatient basis, but under strict monitoring. The adequate performance of the procedure, the absence of immediate complications and the patient basal condition allowed us to be more aggressive on reintroduction of oral feeding. None of these circumstances appear to have affected the final outcome in our case.
The percutaneous endoscopic suturing method to close a persistent gastrocutaneous post-PEG fistula was first described by Alberti-Flor et al. in 2002 using only one suture knot (3). Despite the success of the two patients described in this publication, we have applied in our case the changes including recently by Eskaros et al. (4), consisting in: a) adding a second suture-crossed knot, which gives greater strength to the suture and provides tighter contact between the debrided surfaces; and b) the second change concerns to scarification of both ends of the fistula with biopsy forceps, trying to achieve tissue de-epithelialization to promote granulation tissue formation which allows early closure. We believe that these changes increase the options for fistula closure.
Argon plasma electrocoagulation has been previously used by van Bodegraven et al. (2) to treat esophagopleural fistula, and perhaps it may achieve a more uniform de-epithelialization than with biopsy forceps. In our case, the inadequate caliber of the fistulous tract did not allow us to use argon beam for a complete scarification. However, we have already employed argon beam electrocoagulation associated with endoclips in the successful closure of another fistula secondary to bariatric surgery.
PDS II® suture is a monofilament synthetic absorbable suture that is indicated for use in all types of soft tissue approximation. These sutures are particularly useful where the combination of an absorbable suture and extended wound support (up to 6 weeks) is desirable. However, maintained tension on the skin could eventually cause pressure necrosis. In our case there was no evidence of skin damage until the sixth week, when the external sutures were cut. Given the need for vigilance to prevent pressure ulceration, in future percutaneous endoscopic suturing procedures it could be considered the use of other kind of suture or other techniques that allow suturing in layers, leaving the resorbable material at subcutaneous level where it does not produce ulceration.
In conclusion, percutaneous endoscopic suturing may be an effective treatment of persistent gastrocutaneous post-PEG fistula, at least in selected patients.
References
1. Gauderer MWL, Ponsky JL, Izant RJ Jr. Gastrostomy without laparotomy: a percutaneous endoscopic technique. J Pediatr Surg 1980; 15:872-5. [ Links ]
2. García Moreno JL, Suárez Grau JM, Gómez Bravo MA, Alamo Martínez JM, Domínguez Usero D, et al. Closure of gastrocutaneous fistula using endoscopic biological glue injection. Rev Esp Enferm Dig 2007;99(11):676-7. [ Links ]
3. van Bodegraven AA, Kuipers EJ, Bonenkamp HJ, Meuwissen SG. Esophagopleural fistula treated endoscopically with argon beam electrocoagulation and clips. Gastrointest Endosc 1999;50(3):407-9. [ Links ]
4. Alberti-Flor JJ. Percutaneous-endoscopic suturing of gastrocutaneous fistula: report of 2 cases. Gastrointest Endosc 2002;56(5):751-3. [ Links ]
5. Eskaros S, Ghevariya V, Krishnaiah M, Asarian A, Anand S. Percutaneous endoscopic suturing: an effective treatment for gastrocutaneous fistula. Gastrointest Endosc 2009;70(4):768-71. [ Links ]
6. Safadi BY, Marks JM, Ponsky JL. Percutaneous endoscopic gastrostomy. Gastrointest Endosc Clin N Am 1998;8:551-68. [ Links ]
 Correspondence:
Correspondence:
Fernando Macías García.
Servicio de Aparato Digestivo.
Complejo Hospitalario Universitario de Santiago de Compostela.
C/ Choupana s/n. 15706 Santiago de Compostela. A Coruña, Spain.
e-mail: fmacgar@yahoo.es
Received: 21-10-10.
Accepted: 25-10-10.











 texto en
texto en