Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Revista Española de Enfermedades Digestivas
versión impresa ISSN 1130-0108
Rev. esp. enferm. dig. vol.105 no.2 Madrid feb. 2013
https://dx.doi.org/10.4321/S1130-01082013000200014
LETTERS TO THE EDITOR
Gastric outlet obstruction after the insertion of a fully filled intragastric balloon
Obstrucción del vaciamiento gástrico tras la inserción de balón intragástrico relleno
Key words: Weight reduction. Obesity. Bariatric surgery. Intragastric balloon. Gastric outlet obstruction.
Palabras clave: Pérdida de peso. Obesidad. Cirugía bariátrica. Balón intragástrico. Obstrucción del vaciamiento gástrico.
Dear Editor,
We report the case of a 68-years-old woman, who came to our emergency room because of continuous vomits and epigastric pain. She had undergone an Allergan® gastric balloon insertion two weeks before admission in another hospital, with an adequate balloon deployment. The patient reported abdominal pain, nausea and vomits for 48 hours before admission. Physical examination revealed epigastric abdominal tenderness, without peritoneal signs, in an otherwise obese patient.
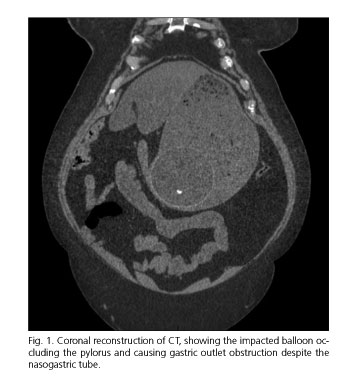
Two days before admission she presented nausea and vomits with an increasing epigastric pain, which prevented her from having solid food or liquids by mouth. After admission, a plain X-ray abdominal film was taken, showing a significant gastric distension. Then, a nasogastric tube was inserted and a CT scan was performed. The CT (Fig. 1) showed the impacted balloon occluding the pylorus and causing gastric outlet obstruction despite the nasogastric tube.
The on-call endoscopist was consulted and decided, by mutual agreement with the patient, to retire the balloon endoscopically under general anesthesia. The procedure was performed with some difficulties related with the great amount of food persisting in the stomach. The balloon was successfully removed with a foreign body mouse-tooth forceps, after emptying it (500 ml of liquid were removed from inside the balloon) by means of a echoendoscopy needle (the specific kit was not available in our hospital). The patient had an uneventful recovery, being discharged 24 hours later.
Discussion
Intragastric balloon is an easily inserted device which can lead to a rapid weight loss to patients with an otherwise high surgical risk due to morbid obesity. Its use as a previous step prior to surgery is widely accepted, but it seems to be ineffective as a single method to reduce weight and its results are transient (1,2).
Although the intragastric balloon is relatively safe, there are significant risks and potential side effects derived from its insertion (2). Several reports have shown few severe but significant complications, sometimes in patients with a previous gastric surgical procedure (3,4) or with normal stomachs, occasionally related with its retrieval (5,6) or spontaneous perforation and subsequent deflation (1), producing intestinal obstruction (7,8). This complication that causes oral intolerance (leading to balloon removal), represents a very unusual situation, appearing at about 2.5 % (9) of all technically well inserted and deployed intragastric balloons, presenting with vomits and epigastric pain few days after its insertion.
Our first suspicion was a puncture and partial emptying of the balloon, but the CT scan showed an adequate diameter. Initially, we considered likely a spontaneous resolution of balloon impaction with the pressure reduction offered by a nasogastric tube, but after 24 hours the patient worsened and we asked her opinion and offered her the removal of the device as described above.
Eduardo Redondo-Cerezo, Virgilio Martos-Ruiz, Ana Matas-Cobos, Manuel Ojeda-Hinojosa,
Juan Gabriel Martínez-Cara, Antonio Damián Sánchez-Capilla, Mercedes López-de-Hierro-Ruiz and Javier de-Teresa
Unit of Digestive Endoscopy. Department of Digestive Diseases.
Hospital Universitario Virgen de las Nieves. Granada, Spain
References
1. Fernandes M, Atallah AN, Soares BG, Humberto S, Guimarães S, Matos D, et al. Intragastric balloon for obesity. Cochrane Database Syst Rev 2007;24(1):CD004931. [ Links ]
2. Göttig S, Daskalakis M, Weiner S, Weiner RA. Analysis of safety and efficacy of intragastric balloon in extremely obese patients. Obes Surg 2009;19:677-83. [ Links ]
3. Giardiello C, Cristiano S, Cerbone MR, Troiano E, Iodice G, Sarrantonio G. Gastric perforation in an obese patient with an intragastric balloon, following previous fundoplication. Obes Surg 2003;13:658-60. [ Links ]
4. Rodríguez-Hermosa JI, Roig-García J, Gironès-Vilà J, Ruiz-Feliú B, Ortiz-Ballujera P, Ortiz-Durán MR, et al. Gastric necrosis: A possible complication of the use of the intragastric balloon in a patient previously submitted to nissen fundoplication. Obes Surg 2009;19:1456-9. [ Links ]
5. Koutelidakis I, Dragoumis D, Papaziogas B, Patsas A, Katsougianopoulos A, Atmatzidis S, et al. Gastric perforation and death after the insertion of an intragastric balloon. Obes Surg 2009;19:393-6. [ Links ]
6. del Pozo P, Flores B, Lirón R, Andrés B, Martin-Lorenzo JG, Chacón S, et al. Gastric perforation during removal of an intragastric balloon. Obes Surg 2009;19:1195-6. [ Links ]
7. Mathus-Vliegen EM. Intragastric balloon treatment for obesity: What does it really offer? Dig Dis 2008;26:40-4. [ Links ]
8. Evans JD, Scott MH. Intragastric balloon in the treatment of patients with morbid obesity. Br J Surg 2001;88:1245-8. [ Links ]
9. Dumonceau JM. Evidence-based review of the Bioenterics intragastric balloon for weight loss. Obes Surg 2008;18:1611-7. [ Links ]











 texto en
texto en