My SciELO
Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO -
 Access statistics
Access statistics
Related links
-
 Cited by Google
Cited by Google -
 Similars in
SciELO
Similars in
SciELO -
 Similars in Google
Similars in Google
Share
Revista Española de Enfermedades Digestivas
Print version ISSN 1130-0108
Rev. esp. enferm. dig. vol.106 n.3 Madrid Mar. 2014
CLINICAL NOTES
Insertion of self-expanding metal stent for treatment of malignant obstruction in a pregnant woman
Inserción de una prótesis metálica autoexpandible como tratamiento de una neoplasia estenosante en una mujer embarazada
Noelia Alonso-Lázaro1, Marco Bustamante-Balén1, Salvador Pous-Serrano2, Ana Braithwaite-Flores1, Marta Ponce-Romero1, Lidia Argüello-Viudez1, Eduardo García-Granero2 and Vicente Pons-Beltrán1
1Digestive Endoscopy Unit. Digestive Medicine Department. Digestive Diseases Area.
2Colorectal Unit. Surgery Department. Digestive Diseases Area. Hospital Universitari i Politècnic La Fe. Valencia, Spain
ABSTRACT
Colorectal cancer (CRC) is the second most frequent cancer both in incidence and mortality in women, especially in those over 60 years of age. Diagnosis in women at gestational age is rare, so its incidence during pregnancy is low. However, an increase in its diagnosis is expected during the next years because of the raise in the average age of pregnancy.
In most cases, the diagnosis is delayed because symptoms related to CRC can be attributed to pregnancy itself. Up to 30 % of CRC cases may present as an intestinal obstruction. In this situation, the main objective is to solve the clinical emergency in the safest way for mother and fetus, together with performing an accurate diagnostic approach to offer the best possible therapeutic management knowing the limitations and difficulties related to pregnancy. The self-expanding metallic stent (SEMS) can be particularly useful in colon obstruction in a pregnant patient with CRC because it allows solving the acute condition providing time to perform a more accurate staging study and to prepare the patient for surgery, thus reducing both post-surgical morbidity and mortality.
We report on the case of a patient who early in the second trimester of pregnancy presented with an acute colonic obstruction due to CRC which was successfully managed with the placement of a self-expanding metal stent.
Key words: Colorectal cancer. Pregnancy. Self-expanding metal stent (SEMS).
RESUMEN
El cáncer colorrectal (CCR) es el segundo tumor tanto en incidencia como en mortalidad en mujeres, sobre todo en mayores de 60 años. El diagnóstico en mujeres en edad gestacional es infrecuente por lo que su incidencia durante el embarazo es baja. Sin embargo, es posible que debido al aumento de la edad media de las gestantes se observe en los próximos años un incremento en el diagnóstico de esta patología.
En la mayoría de ocasiones el diagnóstico se retrasa debido a que la sintomatología derivada del CCR puede atribuirse al propio embarazo. Hasta en un 30 % de los casos el CCR puede debutar como una obstrucción intestinal. En este caso el objetivo principal es solucionar el cuadro agudo de la forma más segura posible para madre y feto y realizar una aproximación diagnóstica adecuada para plantear el mejor manejo terapéutico, con las limitaciones y dificultades que supone la gestación. La prótesis metálica autoexpandible puede ser particularmente útil en la obstrucción de colon por CCR en la paciente embarazada ya que permite solucionar el cuadro agudo y proporciona el tiempo necesario para el estudio de extensión y preparación para la cirugía, reduciendo la morbimortalidad derivada de la misma.
Presentamos el caso de una paciente que al inicio del segundo trimestre de gestación presentó un cuadro obstructivo secundario a una neoplasia de sigma que se resolvió satisfactoriamente con la colocación de una prótesis autoexpandible metálica.
Palabras clave: Cáncer colorrectal. Embarazo. Prótesis autoexpandible.
Introduction
Colorectal cancer (CRC) is the second leading tumor both in incidence (22.9/100,000 inhabitants) and mortality (9.5 cases/100,000 inhabitants) in women, after breast cancer. It is an infrequent neoplasm in young people. Whereas the incidence in 60-69 years-old women is 103 cases/100,000 inhabitants, diagnosing it before 30 years of age is very unusual (1).
The overall incidence of malignant neoplasms during pregnancy is extremely low (0.07 %-0.1 %). CRC comes the seventh in frequency, with an incidence of 1 case per 13,000 gestations (2,3). However, this frequency is likely to rise because women tend to get pregnant at more advanced ages. In Spain, the median age of pregnancy on 2011 was 31.7 years (4), and the incidence of CRC in that range of age is 5-6 cases/100,000 inhabitants (1).
Symptoms secondary to CRC (abdominal pain, nausea, vomiting, change in bowel habits or even rectal bleeding) could be easily misinterpreted as symptoms due to pregnancy or to its complications, driving a delay in diagnosis and thus worsening prognosis. In 7-30 % of the cases, CRC may present as an acute bowel obstruction (5) due to a stenosis, which is located mainly in the left colon, distal to the splenic flexure.
Therapy will depend on several factors, such as gestational age, tumor locations, complications due to cancer or to pregnancy itself, and patient's will. Clinical presentation is very important, since in case of an acute obstruction the main objective is to restore abdominal transit. In this situation, placement of a self-expanding metal stent (SEMS) as a bridge to surgery has shown good outcomes in several reports, mainly in terms of morbidity as compared to emergency surgery (6).
We report on the case of a women in her second trimester of gestation, who during several weeks suffered from non-specific abdominal symptoms initially attributed to pregnancy, and who finally was admitted with an acute bowel obstruction. A diagnosis of an obstructing sigmoid colon adenocarcinoma was made, and a SEMS was placed to solve the acute obstruction.
Case report
A 39-year old female, in her 15 week of pregnancy, was referred to our hospital because an acute bowel obstruction due to a neoplastic colonic stenosis. The patient presented to her local hospital with constipation and vomiting. An abdominal ultrasound was performed which showed a splenic flexure and left colon wall thickening, with luminal narrowing and proximal bowel dilation, along with peritoneal fluid.
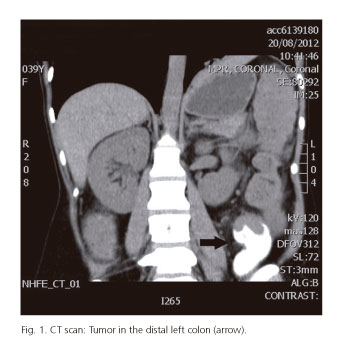
In our hospital, a CT scan without contrast and with pelvic X-ray shielding was performed showing a 3-4 cm in length tumor in the distal left colon (Fig. 1), infiltrating perivisceral fat and a metastatic nodule in the left paracolic gutter. A diagnosis of a left colon cancer T4a was made, although an accurate staging could not be made because of the absence of contrast enhancement.
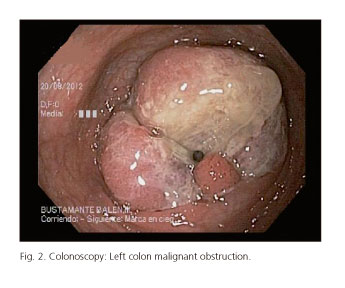
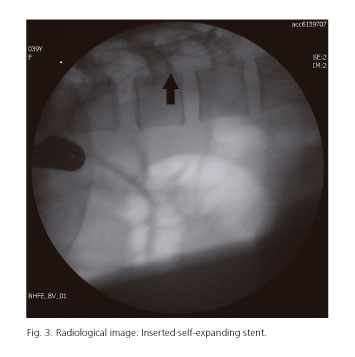
Placing a SEMS to solve the acute obstruction as a bridge to surgery was planned, because the patient initially wanted to continue with pregnancy in spite of the preliminary diagnosis and staging. During colonoscopy, a protruding and friable mass was identified at 35 cm from the anal verge, occupying the entire colonic circumference with luminal narrowing (Fig. 2). The stenosis was traversed with a guidewire under fluoroscopic and endoscopic guidance taking care of minimizing radiation exposure. Then, a 25 x 90 mm SEMS (Wallflex, Boston Scientific, Natick, MA) was placed under endoscopic control through the working channel of the endoscope (Olympus CF-H180AL, Olympus, Hamburg, Germany), with an immediate technical success (Fig. 3).
During follow-up, the patient had a favorable gastrointestinal and obstetric clinical evolution. Twelve days after the stent was placed, a left hemicolectomy with mechanical colorectal anastomosis using dual stapling was performed. A complete omentectomy was also performed, because a unique epiplon metastasis was detected and confirmed with on-site pathological evaluation (pT3N2M1). The patient was counseled about the high risk of tumoral progression, and about the two main therapeutic options: Either termination of the pregnancy and starting chemotherapy 6 weeks after surgery or continuing with pregnancy modifying the cytotoxic chemotherapy (CTC) regime to avoid the risks to the fetus as much as possible. In the end, the patient decided to terminate pregnancy. Therefore, staging was completed with a chest CT scan which showed a lung nodule, subsequently recorded as an ametabolic nodule in the PET/CT. Close follow-up was planned. Adjuvant CTC was started two months after surgery with infusional fluorouracil, leucovorin, and oxaliplatin schedule (FOLFOX). This regime has been maintained for 8 months with frequent temporary discontinuations because of neutropenia, and moderated oxaliplatin-related neurotoxicity. Currently, the patient is in her 10th month of therapy, the CT scan shows no recurrence, and she is being assessed for the eventual delivery of intraperitoneal hyperthermic chemotherapy.
Discussion
CRC is a very unusual entity during pregnancy (7). However, it is an important cause of mortality and it has relevant consequences, both for the mother and for the fetus.
CRC management during pregnancy is a challenge for the clinician. First, there are problems with diagnosis because symptoms are often non-specific and are easily misinterpreted as symptoms secondary to pregnancy itself, as it happened in our patient. Once the diagnosis is suspected, deciding which confirmatory tests are to be used taking into account gestational age is also a challenge. Our patient was in her 15th week of pregnancy. Although colonoscopy is better to be delayed until the second trimester of pregnancy, it can be performed if a potential benefit for mother and/or fetus is to be obtained (8). Moreover, in most cases tumors are located in the rectum (7), thus often there is no need to perform a complete colonoscopy, but a sigmoidoscopy with biopsies. This was not the case in our patient, whose tumor was located in the distal left colon. Regarding other image technologies, ultrasound and magnetic resonance (MR) are preferred over CT scan, because of the high levels of ionizing radiation of the latter. However, if the benefit of this test is considered to outweigh risks, an abdominal CT scan can be performed minimizing radiation as much as possible (8), as it was done in our case.
Finally, treatment will depend on symptoms, tumor stage and gestational age. Our patient presented with an acute bowel obstruction, therefore a placing a SEMS was planned as a bridge to surgery. In the literature search we have only found one report on the placement of a SEMS to solve an acute neoplastic colonic obstruction in a pregnant woman as a bridge to surgery (9). That patient was on the third trimester of pregnancy and the stent allowed gaining time to induce fetal maturity with steroids and then inducing labor at the 32th week of gestation. Then the patient underwent surgery and CTC. Unfortunately, our patient was at the beginning of the second trimester of pregnancy, thus precluding waiting until fetal maturity.
In the general population with CRC, the initial therapy for acute bowel obstruction (SEMS vs. surgery) is still controversial. In a pregnant woman with a non-obstructive CRC, surgery is a good therapeutic option especially before 20th week because of the low risk for the fetus. However, if pregnancy is more advanced, it is advisable to delay surgery beyond week 32 in order to achieve a better fetal survival. If an acute bowel obstruction is the initial presentation, surgery could add risk of maternal and fetal complications; therefore placement of a stent to overcome the acute obstructive episode and then performing a planned surgery seems appealing.
In the general population, studies comparing both options show variable results. Meta-analysis and systematic reviews are hampered by the great heterogeneity of the included studies (10,11). A recent editorial suggests that studies that show a higher technical success are those with a lower rate of complications related to stent insertion when compared with surgical morbidity. Therefore, the election of this therapeutic option has to be determined by the ability to safely and successfully place a stent (12). In this case we decided to place a SEMS to advance in the second trimester of gestation and to lower the complication rate related to emergency colonic surgery, aiming to a greater safety for mother and fetus (13). The insertion technique through the working channel of the endoscope (through the scope, TTS) allows deployment under endoscopic guidance minimizing maternal and fetal radiation exposure. The pre-deployment diameter of the stent is 10 F (3.3 mm) and the diameter of the working channel is 3.7 mm. Once the acute obstruction had been solved, the patient chose elective surgery without termination of pregnancy. Performing a programmed surgery as a second therapeutic stage also allowed a more accurate local oncological staging. The neoplasm was finally staged as a IVB TNM stage.
CTC treatment also is a challenge in pregnant patients. Secondary effects of chemotherapic agents during pregnancy are not fully understood, but they seem to induce relevant toxicity especially during the first trimester of pregnancy (13). Since our patient had a TNM stage IVB CRC, intensive therapy with a FOLFOX schedule was planned (14). There are some reports on the use of oxaliplatin integrated in the FOLFOX scheme during the second and third trimesters, without inducing any fetal malformation, and with a normal child growth and development after delivery (15). However, during the first trimester, this CTC scheme is not used because a high probability of fetal malformations. Finally, after knowing the tumor TNM staging and the need of CTC the patient chose to terminate pregnancy.
In conclusion, although CRC is uncommon during pregnancy, it can be diagnosed at any gestational age, requiring a high suspicion index for its diagnosis. Cases presenting as an acute obstruction can be managed by a SEMS placement as a bridge to surgery. This is a feasible, minimally invasive and effective therapy to solve the abdominal emergency, prepare the patient for surgery and gain time to make the most appropriate therapeutic decision.
References
1. Merrill RM, Anderson AE. Risk-adjusted colon and rectal cancer incidence rates in the United States. Dis Colon Rectum 2011;54:1301-6. [ Links ]
2. Pavlidis NA. Coexistence of pregnancy and malignancy. The Oncologist 2002;7:279-87. [ Links ]
3. De Carolis S, Grimolizzi F, Garofalo S, Fatigante G, Ferrazzani S, Carducci B, et al. Cancer in pregnancy: Results of a series of 32 patients. Anticancer Res 2006;26:2413-8. [ Links ]
4. Instituto Nacional de Estadística (Internet). Disponible en: http://www.ine.es/buscar/searchResults.do?searchString=nacimientos+a%F1o+2011&Menu_botonBuscador=Buscar&searchType=DEF_SEARCH&startat=0&L=0. Acceso en Marzo 2013. [ Links ]
5. Cirocchi R, Farinella E, Trastulli S, Desiderio J, Listorti C, Boselli C, et al. Safety and efficacy of endoscopic colonic stenting as a bridge to surgery in the management of intestinal obstruction due to left colon and rectal cancer: A systematic review and meta-analysis. Surg Oncol 2012;22:14-21. [ Links ]
6. Cennamo V, Luigiano C, Manes G, Zagari RM, Ansaloni L, Fabbri C, et al. Colorectal stenting as a bridge to surgery reduces morbidity and mortality in left-sided malignant obstruction: A predictive risk score-based comparative study. Dig Liver Dis 2012;44:508-14. [ Links ]
7. Bernstein MA, Madof RD, Caushai PF. Colon and rectal cancer in pregnancy. Dis Colon Rectum 1993;36:172-8. [ Links ]
8. ASGE guideline for endoscopy in pregnant and lactating women. Gastrointest Endosc 2012;76:18-24. [ Links ]
9. Healey AJ, Bansi D, Dhanjal MK, Blunt D, Dawson P, Buchanan GN. Colorectal stenting: A bridge to both Caesarean section and elective resection in malignant large-bowel obstruction in pregnancy: A multidisciplinary first. Colorectal Dis 2011;13:e248-9. [ Links ]
10. Tan CJ, Dasari BV, Gardiner K. Systematic review and meta-analysis of randomized clinical trials of self-expanding metallic stents as a bridge to surgery versus emergency surgery for malignant left-sided large bowel obstruction. Br J Surg 2012;99:469-76. [ Links ]
11. Zhang Y, Shi J, Shi B, Song CY, Xie WF, Chen YX. Self-expanding metallic stent as a bridge to surgery versus emergency surgery for obstructive colorectal cancer: A meta-analysis. Surg Endosc 2012;26:110-9. [ Links ]
12. Dayyeh BKA, Baron TH. Endoscopic stent placement as a bridge to surgery in malignant colorectal obstruction: A balance between study validity and real-world applicability. Am J Gastroenterol 2011;106:2181-2. [ Links ]
13. Moran BJ, Yano H, Zahic NA, Farquharson M. Conflicting priorities in surgical intervention for cancer in pregnancy. Lancet Oncol 2007;8:536-44. [ Links ]
14. NCCN clinical practice guidelines in Oncology (Internet). Colon cancer. Version 3.2013. Disponible en: http://www.nccn.org/professionals/physician_gls/f_guidelines.asp#colon. Acceso junio 2013. [ Links ]
15. Jeppesen J, Sterlind K. Successful twin pregnancy outcome after in utero exposure to FOLFOX for metastatic colon cancer: A case report and review of the literature. Clin Colorectal Cancer 2011;10: 348-52. [ Links ]
![]() Correspondence:
Correspondence:
Noelia Alonso Lázaro.
Digestive Endoscopy Unit.
Digestive Medicine Department.
Digestive Diseases Area.
Hospital Universitari i Politècnic La Fe.
Bulevar Sur, s/n.
46026 Valencia, Spain
e-mail: noelia_al84@hotmail.com
Received: 06-05-2013
Accepted: 15-07-2013











 text in
text in