My SciELO
Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO -
 Access statistics
Access statistics
Related links
-
 Cited by Google
Cited by Google -
 Similars in
SciELO
Similars in
SciELO -
 Similars in Google
Similars in Google
Share
Revista Española de Enfermedades Digestivas
Print version ISSN 1130-0108
Rev. esp. enferm. dig. vol.107 n.3 Madrid Mar. 2015
Individualized exercise prescription in non-alcoholic steatohepatitis: A case report
Prescripción individualizada de ejercicio en un caso de esteatohepatitis no alcohólica
Miguel Ángel Sánchez-Martos, José Manuel Gomis-Díaz, José Manuel Sarabia-Marín, Manuel Moya-Ramón and Adolfo Aracil-Marco
Research Group on Physical Conditioning for Health. Sports Research Centre. Universidad Miguel Hernández de Elche. Elche, Alicante. Spain
ABSTRACT
The effect of an individualized exercise programme on a non-alcoholic steatohepatitis case is presented. Before entering the programme the patient was treated with conventional recommendations on diet plus aerobic exercise during fourteen years, without major improvements of his analytical parameters. Two years after including him in a tailored exercise programme, aimed to fulfil the recommendations of the American College of Sports Medicine, his blood markers of liver dysfunction and cardio-metabolic risk tended to improve. Consequently, our data support the idea that in non-alcoholic steatohepatitis the exercise-based therapeutic interventions should be individualized taking into account the cardio-respiratory and muscular fitness of the patient, rather than using generic behavioural recommendations.
Key words: Non-alcoholic steatohepatitis. Exercise. Dislypemia. Hypercholesterolemia.
RESUMEN
Se presenta un caso de esteatohepatitis no alcohólica de dieciséis años de evolución, tratado durante catorce años con recomendaciones dietéticas y de práctica de actividad física regular y que, en los dos últimos años, fue incluido en un programa de ejercicio controlado, monitorizado y supervisado, acorde a las recomendaciones del American College of Sports Medicine. Tras la inclusión del paciente en este programa se observó un cambio en la tendencia de diferentes parámetros analíticos de función hepática y riesgo cardiometabólico, que pasaron de mostrar una tendencia al alza, a estabilizarse o tender a disminuir. A raíz de estas observaciones se sugiere que la mera recomendación de realización autónoma de ejercicio regularmente, sin evaluación de la condición física del sujeto, así como sin unas adecuadas planificación y periodización del mismo, puede resultar una medida ineficaz en el tratamiento de esta enfermedad.
Palabras clave: Esteatohepatitis no alcohólica. Ejercicio. Dislipemia. Hipercolesterolemia.
Background
Although the precise mechanisms are still largely unknown, the role of physical inactivity in the pathophysiology of non-alcoholic steatohepatitis has been suggested (1). Physical exercise is among the therapeutic recommendations for this clinical entity, with an evidence level of 1 and a recommendation grade of B (2). It has been discussed at the literature if exercise is a good therapeutic option (3), mainly due to: a) The common lack of adherence of individuals to exercise programmes (4); b) to the uncertainty on the best characteristics of the exercise to be performed (5); and c) because it is generally accepted that is the secondary weight reduction (rather than exercise itself) the reason of the possible clinical improvements (2). However, a recent meta-analysis including 12 controlled clinical trials has suggested that physical exercise may reduce the pathological hepatic lipid deposition, without decreasing the transaminases blood levels or body weight (6). Similarly, it has been suggested that the intensity of the effort, rather than its duration, could be the main factor to impact the clinical progression of the disease (5,7), being the exercise sessions of moderate to high intensity the ones that can alter the histological progression. However, most of the data on the relationship between physical exercise and non-alcoholic steatohepatitis come from epidemiological studies or from short duration interventions, thus limiting the possibilities to establish causal relationship and the long-time effectiveness of exercise as a clinical therapeutic resource.
Case report
We report here a case of a 36 years old male diagnosed fourteen years before of non-alcoholic steatohepatitis, confirmed by liver biopsy without data on the disease's grade. During all this time the patient was treated with general dietetic and aerobic recreational physical exercise recommendations. The last two years the patient voluntarily joined an individualized physical exercise programme at our centre, in addition to his clinical follow-up.
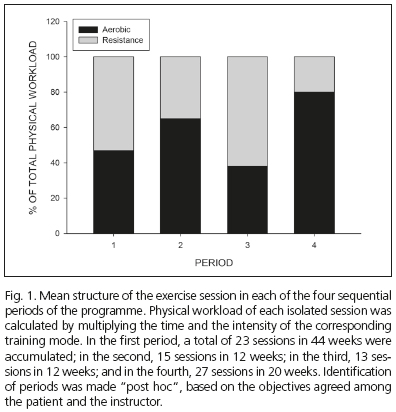
At the beginning of the programme the patient showed the anthropometric and physiological features summarized in table I. He declared to be physically active, practising paddle tennis twice per week plus long distance bike routes on weekends, without controlling the cardiorespiratory intensity of any of them. He also declared to be accomplishing a low-lipid diet and denied alcohol or drugs consumption on a regular basis. Before starting the programme his cardiorespiratory fitness (submaximal exercise test, YMCA protocol) (8), as well as his muscular fitness (Brzycki's protocol) (9), were assessed and used to estimate the corresponding aerobic and resistance training intensities to be prescribed during the programme. The patient was educated to use a pulsometer during his autonomous physical activity -that was encouraged to continue-, and to report the data of every exercise session by using a "training diary". Based on the data reported by the patient a tailored complementary exercise programme was designed to accomplish weekly with the American College of Sports Medicine recommendations on physical activity for health (10). Complementary sessions were performed at our sports centre under the advice of an exercise sciences graduate instructor. Periodically the physical fitness of the patient was tested, to properly readjust the corresponding training intensities. A "post hoc" analysis identified four main training periods, based on the mean physical workload dedicated to improve cardiorespiratory or muscular fitness (Fig. 1). During the whole intervention no changes were made on his diet.
After two years of this complementary training, both cardiorespiratory and muscular fitness increased (Table I), thus indicating that the programme had induced the proper physiological adaptations. During this period, his routine analysis showed a relevant change of tendency in plasma cholesterol (Fig. 2) and triglycerides (data not shown) during the period of intervention. Similarly, despite continuing above normal values, transaminases plasma concentrations showed much less dispersion as well as a trend to be reduced (Fig. 2) during the intervention. However, body weight and body mass fat increased along the duration of the programme (Table I). Taken together our data support the idea that proper "doses" of exercise, conveniently administered to the individual, can induce physiological adaptations capable of counterpart "per se" the pathophysiological mechanisms of non-alcoholic steatohepatitis. Consequently, the non-guided spontaneous recreational physical activity of the individual may have a very small impact on the disease progression.
Discussion
Despite being a case report, due to the extension of the data collection and to the long duration and exhaustive control of the intervention, our data support that is the intensity of each exercise session, rather than its duration, the major determinant of the effects of exercise on the evolution of this disease. However, well designed controlled clinical trials are necessary to confirm this hypothesis. In due case, the current generic recommendations of aerobic exercise should be revisited in favour of including the patients in individualized exercise programmes, such as the one described here. In any case, the clinical impact of this change would be largely limited by the possibilities of the patients to access to this sort of programmes.
Acknowledgements
The authors are indebted to Dr. Cristina Ripoll (Martin-Luther University, Halle Wittenberg, Germany), for the critical reading of the first draft of the manuscript, and her comments and suggestions to improve it.
References
1. Rector RS, Thyfault JP. Does physical inactivity cause nonalcoholic fatty liver disease? J Appl Physiol 2011;111:1828-35. [ Links ]
2. Chalasani N, Younossi Z, Lavine JE, Diehl AM, Brunt EM, Cusi K, et al. The diagnosis and management of non-alcoholic fatty liver disease: Practice guideline by the American Gastroenterological Association, American Association for the Study of Liver Diseases, and American College of Gastroenterology. Gastroenterology 2012;142:1592-609. [ Links ]
3. Caldwell S, Lazo M. Is exercise an effective treatment for NASH? Knowns and unknowns. Ann Hepatol 2009;8(Supl. 1):S60-6. [ Links ]
4. Frith J, Day CP, Robinson L, Elliott C, Jones DEJ, Newton JL. Potential strategies to improve uptake of exercise interventions in non-alcoholic fatty liver disease. J Hepatol 2010;52:112-6. [ Links ]
5. Kistler KD, Brunt EM, Clark JM, Diehl AM, Sallis JF, Schwimmer JB. Physical activity recommendations, exercise intensity, and histological severity of nonalcoholic fatty liver disease. Am J Gastroenterol 2011;106:460-8. [ Links ]
6. Keating SE, Hackett D, George J, Johnson N. Exercise and non-alcoholic fatty liver disease: A systematic review and meta-analysis. J Hepatol 2012;57:157-66. [ Links ]
7. Fealy CE, Haus JM, Solomon TPJ, Pagadala M, Flask CA, McCullough AJ, et al. Short-term exercise reduces markers of hepatocyte apoptosis in nonalcoholic fatty liver disease. J Appl Physiol 2012;113:1-6. [ Links ]
8. Beekley MD, Brechue WF, Dehoyos D V., Garzarella L, Werber-Zion G, Pollock ML. Cross-Validation of the YMCA Submaximal Cycle Ergometer Test to predict VO2max. Res Q Exerc Sport 2004;75:337-42. [ Links ]
9. Brzycki M. Strength testing-Predicting a one-rep max from reps-to-fatigue. J Phys Educ Recreat Danc 1993;64:88-90. [ Links ]
10. Garber CE, Blissmer B, Deschesnes M, Franklin B, Lamonte M, Lee I-M, et al. Quantity and quality of exercise for developing and maintaining cardiorespiratory, musculoskeletal, and neuromotor fitness in apparently healthy adults: Guidance for prescribing exercise. Med Sci Sport Exerc 2011;43:1334-59. [ Links ]
![]() Correspondence:
Correspondence:
Adolfo Aracil-Marco
Centro de Investigación del Deporte
Universidad Miguel Hernández de Elche
Campus de Elche. Avda. de la Universidad, s/n
03202 Elche, Alicante. Spain
e-mail: fito@umh.es
Received: 15-05-2014
Accepted: 26-07-2014











 text in
text in