Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Revista Española de Enfermedades Digestivas
versión impresa ISSN 1130-0108
Rev. esp. enferm. dig. vol.109 no.11 Madrid nov. 2017
https://dx.doi.org/10.17235/reed.2017.5009/2017
Colonic diverticulosis and the metabolic syndrome: an association?
Cristina Teixeira, Daniel Trabulo, Suzane Ribeiro, Claudio Martins, Ana Luísa Alves, Isabelle Cremers and Ana Paula Oliveira
Gastroenterology Department. Centro Hospitalar de Setubal. Setubal, Portugal
ABSTRACT
Background and objectives: Colonic diverticulosis (CD) is related to advanced age and a lack of dietary fiber. Recently, several studies have shown that metabolic syndrome (MS) is also implicated in the etiopathogenesis of CD. This study aimed to assess the association between MS, obesity and CD.
Methods: This was a prospective study of a one-year duration. The MS was defined according to the National Cholesterol Education Program-Adult Treatment Panel III (NCEP-ATP III). Demographic data, risk factors for MS and endoscopic findings of patients who underwent a total colonoscopy in the department were collected. Obesity was defined as a body mass index ≥ 30 kg/m2. Informed consent was obtained. The local Ethics Committee and National Data Protection Committee approved the study. Statistical analysis was performed with SPSS 21 and statistical significance was defined as p < 0.05.
Results: The study included 203 patients, 95 males with a mean age of 65.5 years. CD was diagnosed in 30.5% of patients. Univariate analysis showed that age, hypertension, increased waist circumference and hyperlipidemia were associated with colonic diverticulosis. There was no association with gender, obesity or type 2 diabetes mellitus. Multivariate analysis showed that age and a greater waist circumference increased the risk of diverticulosis. Age-adjusted analysis showed that MS was associated with diverticulosis. The prevalence of adenoma in patients with CD was similar to that in patients without CD.
Conclusion: In this series, MS was significantly associated with CD. The identification of risk groups is important since diverticulosis can have serious and potentially fatal complications. To our knowledge, this is the first Southern European prospective study evaluating the association between MS and CD.
Key words: Colonic diverticulosis. Metabolic syndrome. Risk factors.
Introduction
Diverticulosis is a frequent benign condition of the colon with a prevalence ranging from 10% to 66% of the population; the frequency increases with age (1-3). Diverticulosis results from the herniation of the mucosa and submucosa through the muscular layer of the colonic wall. However, the etiopathology is not fully understood. In Western societies, diverticulosis generally affects the left colon (4). The clinical spectrum of diverticular disease is vast, varying from asymptomatic (in about 80% of affected individuals) to symptomatic disease with severe complications (4,5). A study by Peery et al. (6) has shown that diverticular disease costs an estimated amount of 2.6 billion dollars per year in the USA.
Although studies are controversial, some factors have been associated with a higher risk of colonic diverticulosis and its associated complications. It is thought that colonic wall structure abnormalities, disordered intestinal motility, and environmental, genetic, dietary and behavioral factors influence diverticulosis development. A low-fiber diet was traditionally considered to be a major risk factor for diverticular disease (7). However, recent studies have found no evidence of an effect of dietary fiber intake on the development of diverticulosis (8,9). Constipation was believed to be a risk factor for diverticulosis due to an increased intraluminal pressure (7). However, recent studies have not found an association between diverticulosis and less frequent bowel movements or other classic symptoms of constipation such as straining or incomplete bowel movement (8,10,11). Smoking (12), red meat ingestion (13) and insufficient physical activity physical activity (14) have also been identified as potential factors that increase the risk of diverticular disease. A genetic study in twins has recently demonstrated that genetic susceptibility contributes significantly to the development of diverticulosis (15). The role of obesity and metabolic factors has also been studied, but the results are heterogeneous (16,17). The aim of this study was to evaluate the possible role of the metabolic syndrome (MS) as a risk factor for diverticulosis.
Methods
This was a prospective study with a series of patients who underwent a screening colonoscopy at the Gastroenterology Department of Centro Hospitalar de Setúbal, Portugal, between March 2013 and March 2014. This study was approved by the institution's Ethics Committee and National Data Protection Committee. Informed consent was obtained from all patients.
A colonoscopy was performed that reached at least the cecum, and the colonoscopic features of diverticulosis and colonic polyps were identified. Diverticulosis was classified as pancolonic, left-diverticulosis or right diverticulosis according to the location.
A standardized questionnaire was performed during the medical consultation in order to collect the following data: sex, age, height (m), weight (kg), body mass index (BMI) (kg/m2), waist circumference (cm) measured 1 cm above the umbilicus at minimal respiration, medical history of hypertension, type 2 diabetes mellitus, hyperlipidemia and medication. In the absence of these data, a laboratory evaluation of the following data was obtained prior to the colonoscopy: fasting glucose, triglyceride, and HDL cholesterol levels. Obesity was defined as a BMI ≥ 30 kg/m2.
MS was diagnosed according to the NCEP-ATP III (18) if three or more of the following criteria were present: a) waist circumference ≥ 102 cm in men and ≥ 88 cm in women; b) hypertriglyceridemia ≥ 150 mg/dl; c) low HDL cholesterol < 40 mg/dl in men and < 50 mg/dl in women; d) high blood pressure ≥ 130 mmHg systolic or ≥ 85 mmHg diastolic; and e) high serum fasting glucose ≥ 110 mg/dl.
Statistical analysis
Statistical analysis was performed using SPSS version 21.0 (SPSS Inc., Chicago, IL, USA). The Chi-squared test was used for the comparison of discrete variables and the Student's t-test for the comparison of continuous variables. Variables found to be associated with colonic diverticulosis in the univariate analysis were reassessed using logistic regression analysis. A p-value ≤ 0.05 was considered as statistically significant.
Results
Two hundred and three patients were included; 95 were males (47%) with a mean age of 65.5 ± 9.2 years. CD was present in 62 patients (30.5%), 79% of CD patients had left-sided diverticulosis, 3% had right-sided diverticulosis and 18%, pancolonic diverticulosis.
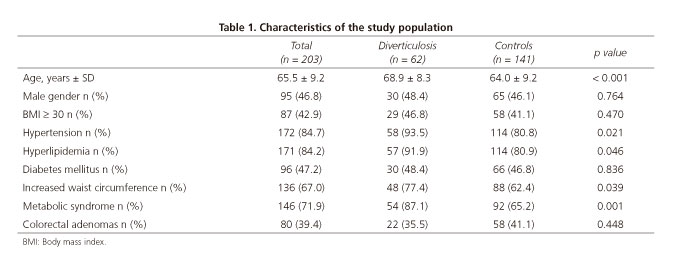
In addition, 84% of patients had elevated blood pressure, 84% had hyperlipidemia and 47%, diabetes mellitus; 67% presented an increased waist circumference and 43% were obese. MS was present in 72% of patients. Table 1 shows the characteristics of patients with and without diverticulosis.
Patients with diverticulosis were significantly older than patients without diverticulosis (68.9 ± 8.3 years vs 64.0 ± 9.2 years, p < 0.001). There was no difference with regard to gender between groups; 48% of patients in the diverticulosis group and 46% in the no diverticulosis group were males (p = 0.764). Among patients with and without diverticulosis, 47% and 41%, respectively, were obese (p = 0.47).
A positive association with colonic diverticulosis was found for increased waist circumference (77% vs 62%, p = 0.039), elevated blood pressure (94% vs 81%, p = 0.021) and hyperlipidemia (91.9% vs 80.9%, p = 0.046). There was no difference with regard to the prevalence of diabetes mellitus between patients with or without diverticulosis (48% vs 47%, p = 0.836).
All the characteristics that comprise the MS were evaluated and MS was more frequent in patients with diverticulosis (87%) than in patients without diverticulosis (65%) (p = 0.003). The variables included in the multivariate analysis were age, hypertension, increased waist circumference and hyperlipidemia. An association with diverticulosis was found for age (p = 0.001, OR 1.068, 95% CI 1.027-1.111) and increased waist circumference (p = 0.049, OR 2.129, 95% CI 1.005-4.510).
MS adjusted for age was evaluated and there was an association with colonic diverticulosis (p = 0.002, OR 3.682, 95% CI 1.587-8.546). There was no difference in the prevalence of colorectal adenomas between patients with colonic diverticulosis (36%) and control patients (41%) (p = 0.448).
Discussion
Colonic diverticulosis is a prevalent condition with an unknown etiology. Colonic diverticulosis can result from a weakness of supporting connective tissue and a subsequent increase in intraluminal pressure, which occurs with aging (19).
The prevalence of diverticulosis in this study was 30.5%, which is similar to other studies (2,20), and it increased with age, as previously demonstrated in other studies (21,22). The majority of patients with diverticulosis had left-sided diverticulosis, which is consistent with other European studies (23,24). Asian studies, in contrast, found a higher prevalence of right-sided diverticular disease (17,25).
There was no correlation between gender and diverticulosis. Initial studies have demonstrated a male preponderance for colonic diverticulosis (26). However, more recent studies found a higher rate of diverticular disease in females, especially in advanced ages (27). A study of the incidence of complicated diverticular disease based on gender and age by Mcconell et al. (28) found that strictures and obstructions occur more commonly in females, while diverticular bleeding occurs more often in men.
Although some studies found an association between obesity (BMI ≥ 30 kg/m2) and asymptomatic colonic diverticulosis (16), others did not find such an association (17). Other studies have found that obesity increased the risk of symptomatic diverticular disease (29-31). In this study, obesity did not represent a risk factor for diverticulosis development. However, increased waist circumference was associated with diverticulosis. A Portuguese study by Afonso et al. (32) that assessed visceral and subcutaneous fat by ultrasound demonstrated an association between diverticulosis and visceral fat. In addition, two other studies that assessed central obesity via computed tomography (CT) scan demonstrated that visceral fat area, but not BMI, was an independent risk factor for diverticulosis (25,33). Furthermore, the study by Yamata et al. (34) showed that patients with left sided diverticula that developed diverticulitis were more likely to have a visceral fat area ≥ 100 cm than patients with asymptomatic diverticulosis. Some studies have shown that visceral fat produces elevated serum levels of several proinflammatory cytokines that induce chronic subclinical inflammation (35,36). In addition, nitric oxide synthase elevation (35) can lead to a decrease in the action of nonadrenergic and noncholinergic inhibitory nerves that induces colonic segmentation and contributes to diverticulosis development (37,38).
There is controversy with regard to the association of other metabolic factors in the development of colonic diverticulosis. A study by Kopylov et al. (16) demonstrated that diabetes mellitus was a protective factor for colonic diverticulosis and found no association with hypertension or hyperlipidemia. By contrast, a study by Sakuta et al. found that hypertension and diabetes mellitus frequency rates were higher among patients with diverticulosis than in control patients (39). The study by Rosemar et al. (31) demonstrated that elevated blood pressure was also a risk factor for symptomatic diverticular disease. Another study by Joaquim et al. (40) found no association between hypertension, hyperlipidemia or DM and recurrence of diverticular bleeding. In this series, hypertension, diabetes mellitus and dyslipidemia were not independent risk factors for diverticulosis, and the prevalence of colonic adenoma or adenocarcinoma was similar in patients with or without diverticulosis, which is similar to the findings from other studies (16).
There are several limitations with regard to this study. Firstly, other potential confounders such as smoking, intake of dietary fiber, physical activity and constipation were not assessed. Secondly, the study population included patients who underwent a screening colonoscopy after referral from a general practitioner or a specialist physician rather than subjects from the general population, which may constitute a selection bias. In addition, data collection of some metabolic factors such as arterial hypertension, hyperlipidemia and diabetes mellitus was performed using the patients' medical history, medication reports and recent laboratory analysis. New laboratory tests were performed only when this information was not available.
In summary, this study demonstrated an association between age, increased waist circumference and MS with diverticulosis development. Studies assessing the relation between MS and diverticulosis are scarce. This study supports the hypothesis that MS plays a role in diverticulosis development. However, further studies are needed to confirm these results and to understand the importance of several metabolic factors in the pathogenesis of diverticular disease.
References
1. Parks T. Natural history of diverticular disease of the colon. Clin Gastroenterol 1975;4:53-69. [ Links ]
2. Delvaux M. Diverticular disease of the colon in Europe: Epidemiology, impact on citizen health and prevention. Aliment Pharmacol Ther 2003;18:71-4. DOI: 10.1046/j.0953-0673.2003.01720.x. [ Links ]
3. Manousos N, Truelove S, Lumsden K. Prevalence of colonic diverticulosis in general population of Oxford area. Br Med J 1967;3:762-3. [ Links ]
4. Faucheron J, Roblin X, Bichard P, et al. The prevalence of right-sided colonic diverticulosis and diverticular haemorrhage. Color Dis 2013;15:266-70. [ Links ]
5. Medina-Fernández FJ, Díaz-Jiménez N, Gallardo-herrera AB, et al. New trends in the management of diverticulitis and colonic diverticular disease. Rev Esp Enferm Dig 2015;107(3):162-70. [ Links ]
6. Peery AF, Dellon ES, Lund J, et al. Burden of gastrointestinal disease in the United States: 2012 update. Gastroenterol 2012;143:1179-87. DOI: 10.1053/j.gastro.2012.08.002. [ Links ]
7. Painter NS, Burkitt DP. Diverticular disease of the colon: A deficiency disease of Western civilization. Br Med J 1971;ii:450-4. DOI: 10.1136/bmj.2.5759.450. [ Links ]
8. Peery AF, Sandler RS, Ahnen DJ, et al. Constipation and a low-fiber diet are not associated with diverticulosis. Clin Gastroenterol Hepatol 2013;11:1622-7. [ Links ]
9. Peery AF, Barrett PR, Park D, et al. A high-fiber diet does not protect against asymptomatic diverticulosis. Gastroenterol 2012;142:266-72. DOI: 10.1053/j.gastro.2011.10.035. [ Links ]
10. Braunschmid T, Stift A, Mittlböck M, et al. Constipation is not associated with diverticular disease - Analysis of 976 patients. Int J Surg 2015;19:42-5. [ Links ]
11. Yamada E, Inamori M, Watanabe S, et al. Constipation is not associated with colonic diverticula: A multicenter study in Japan. Neurogastroenterol Motil 2015;27:333-8. [ Links ]
12. Hjern F, Wolk A, Hakansson N. Smoking and the risk of diverticular disease in women. Br J Surg 2011;98:997-1002. [ Links ]
13. Crowe FL, Appleby PN, Allen NE, et al. Diet and risk of diverticular disease in Oxford cohort of European Prospective Investigation into Cancer and Nutrition (EPIC): prospective study of British vegetarians and non-vegetarians. BMJ 2011;343:d4131. DOI: 10.1136/bmj.d4131. [ Links ]
14. Strate L, Liu Y, Aldoori W, et al. Physical activity decreases diverticular complications. Am J Gastroenterol 2009;104:1221-30. DOI: 10.1038/ajg.2009.121. [ Links ]
15. Granlund J, Svensson T, Olén O, et al. The genetic influence on diverticular disease - A twin study. Aliment Pharmacol Ther 2012;35:1103-7. [ Links ]
16. Kopylov U, Gen-Horin S, Lahat A, et al. Obesity, metabolic syndrome and the risk of development of colonic diverticulosis. Digestion 2012;86:201-5. DOI: 10.1159/000339881. [ Links ]
17. Song JH, Kim YS, Lee JH, et al. Clinical characteristics of colonic diverticulosis in Korea: A prospective study. Korean J Intern Med 2010;25:140-6. [ Links ]
18. Executive summary of the Third Report (NCEP) Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel III). JAMA 2001;285:2486-97. DOI: 10.1001/jama.285.19.2486. [ Links ]
19. Spiller R. Changing views on diverticular disease: Impact of aging, obesity, diet, and microbiota. Neurogastroenterol Motil 2015;27:305-12. DOI: 10.1111/nmo.12526. [ Links ]
20. Loffeld R, Van Der Putten A. Diverticular disease of the colon and concomitant abnormalities in patients undergoing endoscopic evaluation of the large bowel. Color Dis 2002;4:189-92. [ Links ]
21. Commane DM, Arasaradnam RP, Mills S, et al. Diet, ageing and genetic factors in the pathogenesis of diverticular disease. World J Gastroenterol 2009;15(20):2479-88. DOI: 10.3748/wjg.15.2479. [ Links ]
22. Böhm SK. Risk factors for diverticulosis, diverticulitis, diverticular perforation, and bleeding: A plea for more subtle history taking. Viszeralmedizin 2015;31:84-94. DOI: 10.1159/000381867. [ Links ]
23. Dore M, Pes G, Marras G, et al. Risk factors associated with colonic diverticulosis among patients from a defined geographic area. Tech. Coloproctol 2016;20:177-83. DOI: 10.1007/s10151-015-1401-7. [ Links ]
24. Jansen A, Harenberg S, Grenda U, et al. Risk factors for colonic diverticular bleeding: A Westernized community based hospital study. World J Gastroenterol 2009;15:457-61. DOI: 10.3748/wjg.15.457. [ Links ]
25. Nagata N, Sakamoto K, Arai T, et al. Visceral abdominal obesity measured by computed tomography is associated with increased risk of colonic diverticulosis. J Clin Gastroenterol 2015;49:816-22. DOI: 10.1097/MCG.0000000000000267. [ Links ]
26. Weizman A, Nguyen G. Diverticular disease: Epidemiology and management. Can J Gastroenterol 2011;25:385-9. DOI: 10.1155/2011/795241. [ Links ]
27. Kang JY, Hoare J, Tinto A, et al. Diverticular disease of the colon - On the rise: A study of hospital admissions in England between 1989/1990 and 1999/2000. Aliment Pharmacol Ther 2003;17:1189-95. DOI: 10.1046/j.1365-2036.2003.01551.x. [ Links ]
28. Mcconnell EJ, Tessier DJ, Wolff BG. Population-based incidence of complicated diverticular disease of the sigmoid colon based on gender and age. Dis Colon Rectum 2003;46:1110-4. DOI: 10.1007/s10350-004-7288-4. [ Links ]
29. Strate LL, Liu YL, Aldoori WH, et al. Obesity increases the risks of diverticulitis and diverticular bleeding. Gastroenterol 2009;136:115-22. DOI: 10.1053/j.gastro.2008.09.025. [ Links ]
30. Aldoori W, Giovannucci E, Rimm E, et al. A prospective study of diet and the risk of symptomatic diverticular disease in men. Am J Clin Nutr 1994;60:757-64. [ Links ]
31. Rosemar A, Angerås U, Rosengren A. Body mass index and diverticular disease: A 28-year follow-up study in men. Dis Colon Rectum 2008;455:450-5. DOI: 10.1007/s10350-007-9172-5. [ Links ]
32. Afonso M, Pinto J, Veloso R, et al. Visceral fat: A key factor in diverticular disease of the colon. Port J Gastroenterol 2012;19:62-5. [ Links ]
33. Lee SP, Ahn YW, Lee OY, et al. The relationship between colonic diverticulosis and abdominal visceral and subcutaneous fat accumulation measured by abdominal CT scan. Turk J Gastroenterol 2014;25:192-7. DOI: 10.5152/tjg.2014.4581. [ Links ]
34. Yamada E, Ohkubo H, Higurashi T, et al. Visceral obesity as a risk factor for left-sided diverticulitis in Japan: A multicenter retrospective study. Gut Liver 2013;7:532-8. DOI: 10.5009/gnl.2013.7.5.532. [ Links ]
35. John BJ, Irukulla S, Abulafi AM, et al. Systematic review: Adipose tissue, obesity and gastrointestinal diseases. Aliment Pharmacol Ther 2006;23:1511-23. [ Links ]
36. Fontana L, Eagon J, Trujillo M, et al. Visceral fat adipokine secretion is associated with systemic inflammation in obese humans. Diabetes 2007;56:1010-3. DOI: 10.2337/db06-1656. [ Links ]
37. Tomitta R, Fujisaki S, Tanjoh K, et al. Role of nitric oxide in the left-sided colon of patients with diverticular disease. Hepatogastroenterol 2000;47:692-6. [ Links ]
38. Tomitta R, Tanjoh K, Fujisaki S, et al. Physiological studies on nitric oxide in the right sided colon of patients with diverticular disease. Hepatogastroenterol 1999;46:2839-44. [ Links ]
39. Sakuta H, Suzuki T. Prevalence rates of type 2 diabetes and hypertension are elevated among middle-aged Japanese men with colonic diverticulum. Environ Health Prev Med 2007;12:97-100. [ Links ]
40. Joaquim N, Caldeira P, Antunes A, et al. Risk factors for severity and recurrence of colonic diverticular bleeding. Rev Esp Enferm Dig 2017;109(1):3-9. [ Links ]
![]() Correspondence:
Correspondence:
Cristina Teixeira.
Gastroenterology Department.
Centro Hospitalar de Setubal.
Rua Camilo Castelo Branco.
2910-446 Setubal, Portugal
e-mail: ac.corda.teixeira@gmail.com
Received: 18-04-2017
Accepted: 14-07-2017