Dear Editor,
The relationship between cystic fibrosis (CF) and the risk of developing inflammatory bowel disease (IBD) is not clear. CFTR mutations can influence dysbiosis and increased intestinal permeability, which are two key elements in the pathophysiology of IBD. These patients have increased intestinal inflammation, as demonstrated by increase pro-inflammatory gene expression in the bowel, specific fecal markers (fecal calprotectin), gross lesions (capsule endoscopy) and histological lesions on examination of surgical specimens 1.
Historical retrospective studies have reported more than a seven-fold higher risk of developing IBD. However, these studies were perhaps biased by cases of fibrosing colonopathy, which was an unknown condition at the time. Although one study suggested that the most common mutation in CF (deltaF508) might have a protective role against Crohn's disease 2, stricter criteria subsequently demonstrated an increased risk (about five-fold) of developing IBD 3. The literature contains very few case reports about the therapeutic management of patients with CF who develop IBD 4.
We describe the case of a 29-year-old patient diagnosed with CF (deltaF508/L365P) at the age of two years due to poor growth in terms of height and weight. There was no significant respiratory involvement (FVC: 5.33 L, 111%; FEV1: 4.29 L, 104%) and no pancreatic insufficiency, despite repeated bouts of acute pancreatitis. Gastrointestinal manifestations of CF consisted of constipation and gastro-esophageal reflux disease, treated with osmotic laxatives and omeprazole, respectively. The notable surgical history included a postnatal surgery for an enterocutaneous fistula and an appendectomy at five years of age. The patient sought advice due to a six-month history of abdominal pain, associated with raised acute-phase reactants (C-reactive protein 38 mg/dl, fibrinogen 570 g/l) and mild iron deficiency (10 micrograms/ml) with no anemia (hemoglobin 14.6 g/dl). Colonoscopy showed inflammatory changes in the cecum with signs of chronic involvement (deformity); the histology was consistent with IBD. The extent of the disease was investigated via magnetic resonance enterography (Fig. 1A), which showed wall thickening that affected the entire ascending colon and a short segment of the ileum. Following the diagnosis of Crohn's disease, treatment began with 9 mg of oral budesonide in a tapering regimen, with clinical and radiological (Fig. 1B) improvement and the laboratory parameters returned to normal. The patients did not require maintenance treatment with immunomodulators.
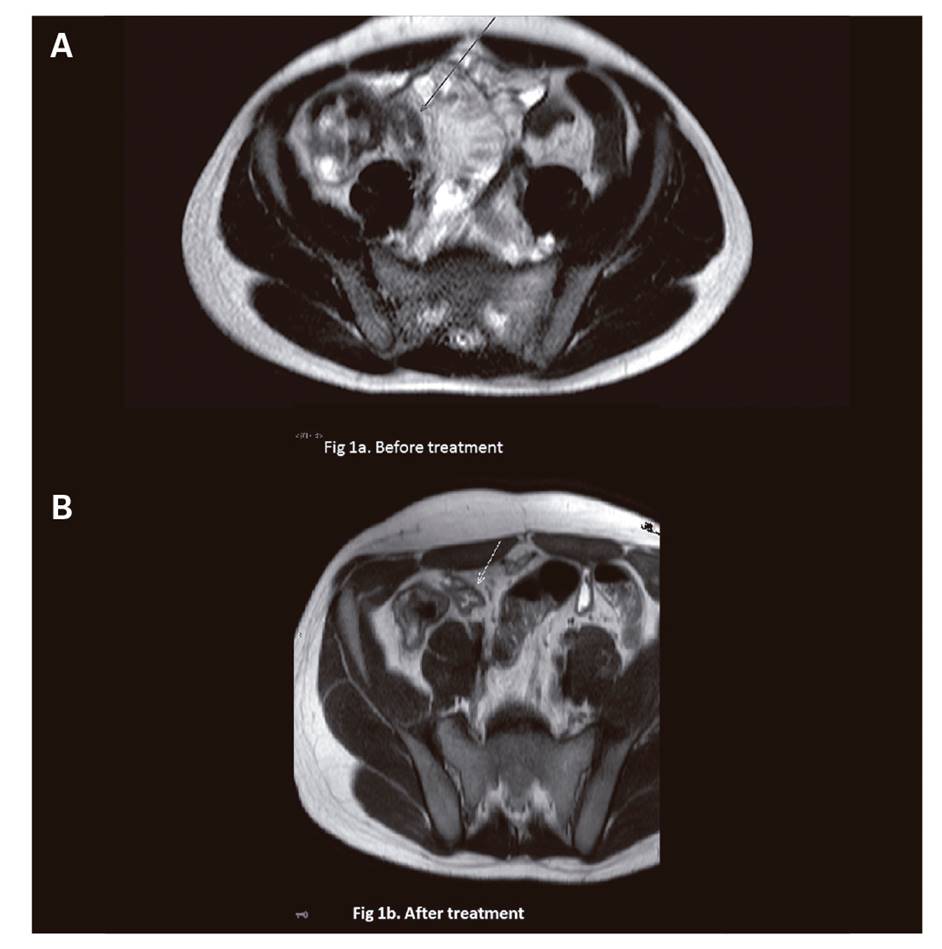
Fig. 1 A. Wall thickening that affected the entire ascending colon and a short segment of the ileum, with layered wall enhancement as a sign of activity. B. Radiological improvement.
Discussion
The reason why IBD occurs in patients with CF is still unknown. It is doubtful whether the pro-inflammatory pathways are the same as in "typical" patients. The same is true in other diseases (e.g., immunodeficiency disorders) that favor the onset of IBD-like conditions. There is also no consensus as to whether this type of treatment should be given to standard patients, or whether it should involve boosting immunosuppressant therapy or optimizing the treatment of dysbiosis (which is common in these patients). We report the case of a patient with CF who developed Crohn's disease and responded well to budesonide therapy.














