Introduction
Salivary gland stones are a salivary gland disease characterized by the formation of calculi or sialoliths inside the ducts or in the glandular parenchyma itself. 1-3 Although it is a relatively common disease, in patients under 18 years, it accounts for only 3% of cases. Regarding its location, it may affect major and minor salivary glands, and most of cases involve the submandibular gland (83-94%) and less frequently the parotid (4-10%) and sublingual glands (1-7%).1,2,4
Etiology and mechanism of formation of salivary calculi are poorly known.4-7 There are several hypotheses for the formation of sialolith, and all of which are related to anatomical irregularities of the conduit or its partial obstruction, salivary composition, infectious process and eletrocoidal and ionic imbalance.1,4-8
Regarding diagnosis, in addition to the clinical examination, it is important to use complementary methods, including conventional radiographs, sialography, MRI, ultrasound and computerized tomography to determine more precisely the location of salivary calculi and correct treatment plan.7,9 Additionally, some characteristics of sialolith such as size, location, number, relationship to the surrounding tissues (adhesive, impacted, mobile) and the presence of inflammation and/or infection should be considered when choosing the best form of treatment, whether it is surgical or not.1,10 Due to the rarity of this disease in the parotid gland, especially considering its appearance in a young patient and its atypical extraductal location, which was only confirmed after computed tomography imaging, and its quite considerable size, the description of this clinical case is relevant and important.
Case report
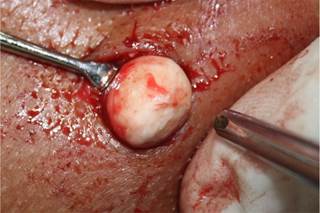
17-Year-old patient (T.P.V.) with melanoderma was referred by his orthodontist for extraction of teeth 38 and 48 and a possible supernumerary tooth present in the left posterior mandibular region. Panoramic radiograph showed the presence of a well delimited, hyperdense, rounded structure near the mandibular angle, with approximately 10mm in diameter, overlapping the bone structures and the mandibular canal (Fig. 1). During the anamnesis, the patient reported no discomfort, pain or swelling. On clinical intraoral examination, no abnormality was observed. Milking maneuver was performed in the parotid gland and the salivary flow was found to be normal and with no pus. However, on the extraoral examination, during palpation of lymph nodes and bidigital palpation of the cheek, it was observed the presence of a rounded, firm, mobile nodule, under the skin at the lateral region of the mandible angle on the left side (Fig. 2). For a better assessment of the location and diagnostic hypothesis, it was performed a computerized tomography, which revealed the extra-osseous location of the lesion in the soft tissues laterally to the left mandibular angle (Fig. 3). The diagnostic hypotheses for such an alteration were sialolith and changed lymph node. During surgical planning, excisional biopsy was chosen, under local anesthesia, in an outpatient setting. The patient underwent extra-oral infiltrative anesthesia and it was performed a linear incision in skin, followed by divulsion of the flap by planes with Metzenbaum scissors (Fig. 4). Incision on the tissue which covered the nodule allowed the removal of the round solid body with 10mm in diameter (Fig. 5). The wound was sutured with Nylon (5-0) and the specimen was sent for histopathological examination. During the clinical follow-up, the patient recovered without any complications. After routine histology, the department of pathological anatomy of the subject Oral Pathology (Federal University of Alfenas/ Unifal-MG) reported that the microscopic sections revealed that the fragment consisted of concentric laminations with slight differences in color, separated by reversal lines; peripherally it was observed fibrous connective tissue that was dense, slightly cellularized and vascularized. The diagnosis was sialolith. After 30 months no recurrence of the lesion was observed, as shown in the panoramic radiograph (Fig. 6).
The consent form was signed by the legal representative of the patient, which included the use of his radiographs, photographs, lab results and any information related to treatment for educational and scientific purposes.
Discussion
Salivary gland diseases are relatively common, and obstructive sialadenitis is the most frequent non-neoplastic salivary disorder. As for location, submandibular gland corresponds to the site of approximately 90% of sialolithiases (83-94%).1,2,4,5 Thus, the location of sialolith in this clinical case can be considered unusual, since it was developed in the parotid gland.
The occurrence rate of this disease accounts for approximately 1.2% of the population, with no predilection for race and it is more common in middle-aged young male adults (between the third and fourth decade of life), although it may affect the elderly and rarely children.1,2,4,5 The predilection for male patients is even more evident in the case of parotid gland sialolithiasis.1 This clinical case is consistent with the literature regarding the predilection for sex, since the patient of this study is a male subject and the salivary calculus developed in the parotid gland. However, sialoliths are quite rare in adolescence, which is the age group of the patient of this clinical case.
It is important to consider different conditions to perform the differential diagnosis of sialolithiasis. The unilateral parotid enlargement is characterized by the presence of a discrete palpable mass and diffuse edema. Nevertheless, sialadenitis can be considered in the absence of such mass. The superficial mass in the salivary gland may suggest a case of lymphadenitis, preauricular cyst, sebaceous cyst, benign lymphoid hyperplasia or extraparotid tumor and not the presence of a sialolith, while the mass within the salivary gland may suggest a (benign or malignant) neoplasm, intraparotid adenopathies or hamartoma.11 Thus differential diagnosis of asymptomatic bilateral enlargement of the parotid gland should be performed, eliminating the possibility of treating malignant lesions and/or other benign lesions of salivary glands. The clinical symptoms of malignant tumors include rapid growth, facial nerve paralysis, stone texture, pain and a higher rate of incidence among elderly patients. Such features of malignancy were not observed in this clinical case, and the volumetric increase had not been seen by the patient at the time of consultation, revealing a silent growth. In addition, paresthetic and/or painful changes were not observed.
In contrast, the benign lesions to be taken into account in the differential diagnosis include lymphoepithelial lesions (Mikulicz syndrome), Sjögren's syndrome, Warthin's tumor, viral sialadenitis (including mumps) and secondary sialadenitis that occur as a result of alcoholism and long-term treatment with different drugs (iodine and heavy metals). Furthermore, radiation therapy of the parotid region may lead to the formation of painful swellings. Other conditions that should be considered in the differential diagnosis, but that have no relation to the salivary glands, are hypertrophy of the masseter muscle, lesions in the temporomandibular joint and osteomyelitis of the ascending maxillary branch. Additionally, it is important to distinguish the sialoliths from other soft tissue calcifications, such as calcification of lymph nodes.12
Regarding symptomatology, in most cases the pain is present and other clinical signs are apparent, making diagnosis easier. Nevertheless, we always have to consider that pain is just one of the symptoms, and 17% of cases of sialoliths are asymptomatic,4,6 especially when duct obstruction is not complete and part of saliva can be eliminated surpassing the calculus.7 Therefore, intraductal sialolithiasis is usually more severe than intraglandular sialolithiasis, since the impairment of salivary flow is more pronounced when the calculus is located inside the duct.13 In this case the patient showed no symptoms, and this is probably associated with the rare location of the sialolith within the parotid gland, without ductal involvement, which consequently did not cause obstruction and painful symptoms.
Regarding the forms of treatment, conservative measures should be reserved for small sialoliths and surgical removal should be performed in cases of larger lesions. Conservative treatment comprises massages for drainage of the salivary gland and hydration of the patient. This last measure leads to an increased production of saliva, which by itself can expel the sialolith. Another approach to be taken into account when the sialolith is close to the duct hole is removing it by enlarging the hole using a probe.1 However, when such calculi are larger, even though they are present in the salivary duct, the standard treatment involves surgical removal with preferably intraoral approach, while intraglandular sialoliths require submandibular sialoadenectomy or partial parotidectomy.1,6 It is noteworthy that the treatment of sialolithiasis of major salivary glands underwent a fundamental change over the last 10-15 years. Different minimally invasive techniques have been developed. In addition to the simple extracorporeal shock wave lithotripsy,14 it includes, particularly, the sialoendoscopy,15 which is connected to a high success rate due to the direct visualization of sialoliths without any contrast medium and radiation exposure. However, the disadvantage of new therapies is that their clinical application is related to the availability of instruments and apparatus, which increases the time, personnel and organizational costs for the treatment.10
In this clinical case, due to the superficial location of the calculus in the soft tissues laterally to the left mandibular angle, we opted for surgical removal of the lesion by extraoral access, aiming at minimal injury to the adjacent tissues and anatomical accidents. Since an appropriate extraoral incision following the natural skin folds allows a favorable esthetic result, in the conditions of this clinical case it can be considered as a more conservative approach than intraoral access, since the sialolith was located laterally to the masseter muscle, close to the skin. Therefore, intraoral access would cause injury to a much larger number of tissue layers. Furthermore, the extraoral approach is indicated to access siloliths in the parenchyma of the gland or when they are present in the salivary duct portion laterally to the masseter muscle6 and the sialolith of this study was in the glandular parenchyma, which is one of the indications of extraoral access.
Due to the specificities of this clinical case, such as the early age of lesion onset, atypical location of lesion both in relation to the salivary gland involved and the involvement of the glandular and non-ductal portion of the parotid gland, leading to difficulties in establishing the lesion location and also because of the radiographic characteristics of radiopaque mass in the region of the mandibular angle, similar to an impacted tooth, and limited imaging, the diagnosis was difficult at first. In these situations, diagnostic aids are essential not only for the correct diagnosis, but also to perform the appropriate surgical planning. Among the available imaging exams, computerized tomography (CT) has obtained the best results concerning location and/or delimitation of mineralized structures. Thus, taking into consideration that most sialoliths contain enough calcium to be visible through this method, such that image quality is superior to those obtained by conventional radiographs and due to possible reconstructions in various planes, computed tomography was the exam of choice to determine the location of the sialolith in this clinical case.
After reviewing the CT images, it was possible to determine the precise location of the sialolith, which was located in the soft tissue, near the angle of the jaw on the left side, superficially to the masseter muscle and below the parotid duct. Thus, the surgical procedure can be planned and carried out without major complications for the patient. In addition, histopathological diagnosis allowed to conclude that the foreign body was a sialolith located in the parenchyma of the parotid gland in its superficial surface, characterizing an atypical location of salivary calculus since the ductal location is the most common one. Therefore, this case report adds information to the small number of described cases of sialoliths developed in the parotid gland, especially in its glandular portion, emphasizing that despite the majority of salivary calculi present very peculiar characteristics, some may have an atypical location and be radiographically confused with other structures, such as intraosseous pathologies or retained tooth. The authors also emphasize the importance of computerized tomography imaging for the resolution of this case, which is considered the best method for locating mineralized structures of difficult diagnosis and/or delimitation.
Conclusion
It is possible to conclude that the CT scan is very effective to precisely locate the lesion when comparing with surrounding anatomical structures, ensuring appropriate treatment plan, especially in these cases in which diseases with evident clinical signs, such as sialolithiasis that take atypical locations that make it difficult the diagnosis and its exact location.