Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Medicina Oral, Patología Oral y Cirugía Bucal (Ed. impresa)
versión impresa ISSN 1698-4447
Med. oral patol. oral cir. bucal (Ed.impr.) vol.10 no.5 nov./dic. 2005
Rescue surgery (surgical repositioning) of impacted lower second molars
Cirugía de rescate (reubicación quirúrgica)en segundos molares inferiores impactados
Manuel García Calderón (1), Daniel Torres Lagares(2), Maribel González Martín (2), José Luis Gutiérrez Pérez (3)
(1) Profesor Asociado de Cirugía Bucal
(2) Profesor del Master de Cirugía Bucal
(3) Profesor Titular de Cirugía Bucal. Universidad de Sevilla
Address:
Dr. Daniel Torres Lagares
C/ Sta Mª de Valverde 2 3ºC
41008 Sevilla (España)
Tlfno 954 436 724 – Fax 954 481 129
E-mail : danieltl@us.es
Received: 22-12-2004 Accepted:8-06-2005
|
García-Calderón M, Torres-Lagares D, González-Martín M, Gutiérrez-Pérez JL.
Rescue surgery (surgical repositioning) of impacted lower second molars. Med Oral Patol Oral Cir Bucal 2005;10:448-53. |
|
ABSTRACT
The impaction of lower second molars, given that its incidence is 0.03 to 0.21%, is a rare complication in tooth eruption. It has been detected more often in unilateral form than bilateral and is more common in the mandible than in the maxillary. It has a slight predilection for males, and mesial inclination is more usual. Key words: Molar pathology, dental eruption, dental impaction, surgical repositioning.
|
RESUMEN La impactación de los segundos molares inferiores es una complicación de la erupción dentaria muy infrecuente, dado que su incidencia se cifra de un 0,03 a un 0,21 %. Se ha detectado en mayor frecuencia de forma unilateral que bilateral y es más usual en mandíbula que en maxilar. Presenta una ligera predicción por el sexo masculino, y la inclinación mesial es la más habitual. Palabras clave: Patología molar, erupción dental, impactación dental, reubicación quirúrgica. |
INTRODUCTION
The impaction of lower second molars, given that its incidence is 0.03 to 0.21%, is a rare complication in tooth eruption. It has been detected more often in unilateral form than bilateral and is more common in the mandible than in the maxillary. It has a slight predilection for males, and mesial inclination is more usual (1).
The impaction of a lower second molar can cause aesthetic and mastication problems and instability of the dental arch, as well as a higher likelihood of caries in the distal side from the first lower molar. The principal cause is the osseo-dental discrepancy, the impaction, becoming worse due to the development of the third molar (2,3).
A wide variety of therapeutic approaches have been published, basically referring to surgical techniques, whether independent or complemented by means of orthodontic technical aids, with the aim of placing the tooth in the correct position, and which are encompassed under the concept of surgical rescue: surgical removal of the second molar and expected eruption of third molar in place of the second (despite the risk of it erupting in the wrong position); surgical removal of the second molar and transplant of the third molar in place of the second; surgical exposure of the second mandibular molar and the positioning of orthodontic buttons for traction and to force its proper eruption: surgical repositioning of the second molar, frequently after the extraction of the root of the third molar, etc.(4,5)
In cases resolved with repositioning of an impacted tooth, prophylactic root extraction has been proposed as obligatory (6). We present a clinical case of retention and impaction of a lower second molar successfully repositioned without extracting the root of the lower third molar.
CLINICAL CASE
We present the case of a 12 and a half year old patient referred to the Master of Oral Surgery of The University of Seville due to non-eruption of the left lower second molar (Figure 1).
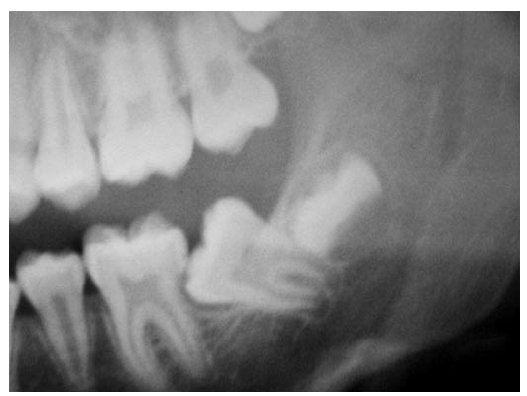
Fig. 1. Pre-operative panoramic x-ray.
The patient was referred by her orthodontist, who detected the impaction, before starting orthodontic treatment. The orthodontist requested that, if it was possible, we did not extract the root of the third molar, because its eruption would be feasible in the future (there should be sufficient space in the arch). Given the space available to us, we decided to attempt the repositioning of the impacted tooth without extracting the root of the wisdom tooth.
We started the intervention under local anaesthetic, and we performed a bayonet incision, lifting a full thickness flap. After slightly loosening the tooth from the bone which surrounds it, we proceeded to gently raise it. We confirmed the stability of the tooth in its new position. To avoid losing the position we introduced a stranded wire which would fix the new contact point. This wire was removed after three weeks (Figure 2). We sutured the flap with stranded silk which was removed after 15 days.

Fig. 2. Repositioned and stabilised tooth.
The progression of the case was monitored, clinically and radiologically during the year following the surgery. No signs of disease were observed in the pulp and there was evidence of correct bone regeneration (Figure 3).

Fig. 3. X-ray image 9 months after the surgery.
DISCUSSION
According to the classification by Andreasen and Kurol (7), the absence of eruption of the second molar can be classified into three events:
Impaction: caused by a physical obstacle, basically due to lack of space, and which could provoke a collision between the follicles of the second and third molar. In fact, ectopic eruption with mesial inclination of the second molar, the most common, is often related to the packing together of the front teeth (8).
It can also be caused by other obstacles; extra teeth, odontomas, odontogenic tumours or giant cell fibromatosis in the eruption line. Finally, impaction can be caused by an ectopic eruption pathway (7).
Primary retention (eruption arrested before the rupture of the gum): in the majority of cases is due to an unknown cause. In the remaining situations it is associated with syndromes where osteoclastic activity is compromised (9).
Secondary retention (cessation of the eruption after gingival rupture, without the presence of a physical obstacle): is more common than primary retention and is caused by a small area of ankylosis, especially in the interradicular zone (10). As regards the appearance of this ankylosis, the influences of genetic (11) and systemic factors (1) have been discussed.
As regards the treatment of this pathology, we must point out that it is difficult to propose clinical procedure protocols, given the low prevalence of this problem, and the great clinical diversity that it can present. In the same way, the difficulty in distinguishing between primary and secondary retention and impaction does not help in the development of these protocols.
With an impaction, if it is caused by lack of space, we must opt for extraction of the impacted tooth or increase the space available, whether it is orthodontically or by extraction of the root of the third molar. Possibly, in this latter case, it may be opportune to perform surgery over the retained second molar, instead of waiting for its spontaneous eruption.
If the impaction is due to ectopic eruption, we can choose between the following approaches: surgical exposure, repositioning, surgical-orthodontic re-implantation, transplant or extraction of the impacted tooth. In teeth which erupt mesially and ectopically, the impaction can be resolved spontaneously, but active treatment is normally required.
Where the impaction is caused by an obstacle in the eruption, we would proceed to eliminate this, deciding whether we should carry out any other beneficial procedure or we can wait for the spontaneous eruption of the tooth.
As regards a primary retention, some authors place special emphasis on the fact that treatment is no different if we are confronted with an impaction. The main variable in the choice of treatment should be the clinical situation pertaining to the retained tooth (12).
The same does not apply to a secondary retention. In this case the treatment options are preservation of the tooth and its prosthetic reconstruction, or extracting it and transplanting the third molar root in its place. If the third molar is between Nolla stages 5 and 8 (13), only by extracting the retained second molar can the third molar erupt in its place.
Considering the use of repositioning as a treatment for impaction of a lower second molar, there is a series of points which should be evaluated in the selection of this option and a set of rules which should be followed whilst performing this.
Among them is the available space in the dental arch, the formation of roots, the arc of rotation, occlusion, the periodontal state and the vertical growth of the mandible (14). With the aim of creating space in the arch to correctly reposition the second molar, prophylactic extraction of the third molar root is proposed, although as we have discussed earlier it does not have to be obligatory.
The best time to treat patients with an impacted second molar is in adolescence (between 10 and 17 years), when the roots of the third molar are not formed and the roots of the second molar, optimally, are from a third to a half of their total length and their apexes are still open (14).
The arc of rotation in the repositioning should not be more than 90 degrees, given that if it was outside this, we would, very possibly, be making a transplant and would be decreasing the possibilities of post-surgical pulp revascularisation (6).
Once the repositioning is carried out, the tooth must be stabilised and occlusal contact avoided. We must be careful and not damage, inasmuch as possible, the periodontal cement and glue, as well as correctly reposition the keratinised gum. The use of fill materials is not indicated. All this is associated with the aim of good long term periodontal health and proper bone regeneration (6).
It is desirable that the vertical growth of the mandible is almost complete, given that it could avoid the possibility of the repositioned tooth remaining submerged during growth if there is not adequate periodontal healing.
As regards the extraction of the root of the third molar, there is a consensus that the third molar cannot be considered as a cause of lower second molar impaction, given that it does not get involved in either the time or in the path of the eruption of the lower second molar. In fact, simply extracting it does not lead to the proper eruption of an impacted second molar (13).
Although some authors (15) support the extraction when a surgical exposure or a surgical repositioning of the second molar is performed, we think that if the intervention is carried out on patients with the optimal age and the root of the third molar does not make the surgical technique difficult, its extraction is purely an orthodontic decision. Therefore, if the orthodontist is of the opinion that there will be space for its eruption in the future, its sacrifice does not have any advantages. At the same time we lose a future treatment option (transplant of the wisdom tooth root) if the surgical approach is not successful.
Other authors believe that the third molar root can compromise the position of the repositioned second molar during its healing (13). However, if the position obtained is stable with an adequate point of contact and the age of the patient is appropriate this does not have to be the case. In our case, we have not extracted the third molar root due to the instruction given by the orthodontist, we have achieved a stable situation, and at the time when the third molar begins its eruptive movements the healing of the periodontal apparatus for the second molar will have finished. Obviously, this latter point is fundamental, given that the eruptive force of the third molar, applied on a tooth without adequate bone fixation could cause it to move and bring about its subsequent loss.
Finally, and despite the wide range of treatment possibilities that we have set out, according to some studies, only half of the cases treated conservatively achieve an adequate position of the impacted tooth in the arch (13).
The severity of the case and the advanced age of the diagnosis are the factors associated with the lack of an acceptable result of the treatment. The most successful therapeutic option is orthodontic, although it cannot be used in the more severe cases.
As regards the other factor, the advanced age of the diagnosis, the lack of eruption of a front tooth is easily detected by the parents or by the child him/herself, while this does not happen with back teeth, which also do not have any symptoms (13), therefore it is normally detected routinely or casually. This leads to delays in diagnosis with a significant implication in the treatment result, given that the apexes of the teeth involved can be closed.
Patient follow up is essential, not only because it is possible that pulp necrosis (15) develops, but also because on not detecting alterations or premature occlusal contacts, which should be resolved during the surgical intervention, versions of lower second molar, extrusions or incomplete eruptions can take place. Equally, in teeth which have developed ankylosis it is not unusual for it to return.
REFERENCES
1. Varpio M, Wellfelt B. Disturbed eruption of the lower second molar: clinical appearance, prevalence, and etiology. ASDC J Dent Child 1988; 55: 114-8. [ Links ]
2. Reynolds LM. Uprighting lower molar teeth. Br J Orthod 1976; 3: 45-51. [ Links ]
3. Terry BC, Hegtvedt AK. Self-stabilizing approach to surgical uprighting of the mandibular second molar. Oral Surg Oral Med Oral Pathol 1993; 75: 674-6. [ Links ]
4. Bishara SE, Ortho D, Burkey PS. Second molar extractions: a review. Am J Orthod 1986; 89: 415-24. [ Links ]
5. Hale ML. Autogenous transplants. J Am Dent Assoc 1954; 49: 193-8. [ Links ]
6. Shipper G, Thomadakis G. Bone regeneration after surgical repositioning of impacted mandibular second molars: a case report. Dent Traumatol 2003; 19: 109-14. [ Links ]
7. Andreasen JO, Kurol J. The impacted first and second molar. En: Andreasen JO, Petersen JK LD, eds. Textbook and color atlas of tooth impactions. Copenhage:Munksgaard; 1977. p. 197-218. [ Links ]
8. Evans R. Incidence of lower second permanent molar impaction. Br J Orthod 1988; 15: 199-203. [ Links ]
9. Oliver RG, Richmond S, Hunter B. Submerged permanent molars: four case reports. Br Dent J 1986; 160: 128-30. [ Links ]
10. Raghoebar GM, Boering G, Jansen HW, Vissink A. Secondary retention of permanent molars: a histologic study. J Oral Pathol Med 1989; 18: 427-31. [ Links ]
11. Reid DJ. Incomplete eruption of the first permanent molar in two generations of the same family. Br Dent J 1954; 96: 272-3. [ Links ]
12. Raghoebar GM, Boering G, Vissink A. Clinical, radiographic and histological characteristics of secondary retention of permanent molars. J Dent 1991; 19: 164-70. [ Links ]
13. Valmaseda-Castellon E, De-la-Rosa-Gay C, Gay-Escoda C. Eruption disturbances of the first and second permanent molars: results of treatment in 43 cases. Am J Orthod Dentofacial Orthop 1999; 116: 651-8. [ Links ]
14. Tinerfe TJ, Blakey GH, eds. Oral and maxillofacial surgery. Philadelphia: Saunders; 2000. p. 308-16. [ Links ]
15. Owen AH. Early surgical management of impacted mandibular second molar. J Clin Orthod 1998; 32: 446-50. [ Links ]











 texto en
texto en 


