Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Medicina Oral, Patología Oral y Cirugía Bucal (Internet)
versión On-line ISSN 1698-6946
Med. oral patol. oral cir.bucal (Internet) vol.12 no.7 nov. 2007
Sinus elevation by in situ utilization of bone scrapers: technique and results
Pedro Martos Díaz1, Luis Naval Gías2, Jesús Sastre Pérez3, Raúl González García1, Fernando Bances del Castillo3, María Mancha de la Plata1, Pablo Galindo Moreno4, Mario Muñoz Guerra2
(1) Maxillofacial Surgery Resident. Princesa University Hospital. Madrid
(2) Consultant in Maxillofacial Surgery. Princesa University Hospital. Madrid
(3) Dentist in Private practice. Santa Cruz de Tenerife
(4) Dentist. Department of Oral Surgery. University of Granada
ABSTRACT
Objectives: The objective was to present a novel technique for antrostomy performed before sinus elevation in atrophic maxilla for subsequent implant placement.
Material and methods: The study included 10 sinus elevations performed by the proposed technique in nine consecutive patients presenting with inadequate posterior maxillary height. The technique is described, calculating the antrostomy surface area, volume of bone tissue obtained and final height attained in each case. A total of 16 implants were placed.
Results: All ten elevations were accomplished. Mean antrostomy surface area was 0.55 mm2, mean bone volume obtained was 0.56 cm3 and mean height attained was 11.7 mm from a baseline mean height of 5.6 mm. Out of the 16 implants, 14 were inserted immediately after the elevation and 2 were inserted in a second step, after ossification; 93.7% of the implants were osseointegrated at 6 months after prosthesis placement.
Conclusion: The use of bone scrapers to create antrostomy for sinus elevation is a simple and very safe procedure. It provides a variable amount of particulate bone graft that is easily handled and highly useful for packing the cavity that will elevate the sinus membrane.
Key words: Sinus elevation, antrostomy, dental implants.
Introduction
Preparatory adjuvant procedures are required before the placement of osseointegrated implants in atrophic maxilla, e.g., maxillary sinus elevation, implant placement in anatomical buttresses, or maxillary reconstruction with grafts (1). In 1980, Boyne and James (2) described elevation of the maxillary sinus for restoration of posterior sectors of the upper maxilla with implants. Since that time, few changes have been made in this procedure, which mainly consists of the creation of a window in the anterior bone wall of the maxillary sinus (Caldwell-Luc approach) (3). This window affords access to the Schneider membrane, which is then detached and elevated, thereby creating a space beneath it. This space must be packed with material that supports the membrane and also has bone-forming capacity. The implants are placed after this sinus elevation. The packing material can be autogenous or allogeneic but must be capable of compressing the space so that the implant can be anchored in it.
Over the past few decades, major advances have been achieved in the bone materials used to pack the maxillary sinus as a substitute for autogenous bone (4). However, these materials do not supply the cellular elements necessary for osteogenesis and act solely as osteoconductive elements (5). Hence, autogenous bone remains the packing material of choice in maxillary sinus elevation procedures (6, 7).
The aim of the present article was to describe a simple technique for maxillary sinus membrane elevation and the in situ collection of autogenous bone, recording the amount collected, the height of elevation attained, the outcomes and the possible complications. The advantages and disadvantages of the technique are also analyzed.
Material and methods
The study included nine consecutive patients presenting with atrophy in posterior sections of the maxilla. Patients consented to a treatment plan involving elevation of the maxillary sinus membrane for subsequent placement of osseointegrated implants (Figures 1, 2, 3). Ten elevations were performed, including a bilateral elevation in one patient.



The height of the bone to the base of the maxillary sinus and the height required for insertion of the appropriate implants were calculated in each patient. A total of 16 Mozo Grau® threaded implants were placed (3 implants of 3.75 x 10 mm, 7 implants of 3.75 x 11.5, 2 implants of 3.4 x 11.5 and 4 implants of 3.75 x 13).
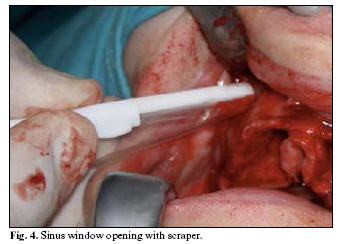
The window was then opened by using the technique described below, measuring the volume of particulate bone obtained by placing it in a calibrated (mm) insulin syringe. Bone was never taken from a site outside the field exposed for the elevation, i.e., the window (Fig 4). When inadequate particulate bone was obtained to completely pack the cavity, it was complemented with allogeneic material, i.e., hydroxyapatite or demineralised bone. In each case, data were recorded on the bone graft volume obtained, the surface area of the antrostomy, the number of implants inserted in each sinus elevation and the height (in mm) attained after the consolidation period. Surgical and post-surgical complications were also recorded.
Orthopantomography was performed in all patients at three months before and after surgery and at six months after completion of the prosthetic phase.
Surgical technique
After elevating the mucoperiosteal flap by means of a crestal incision with lateral release incisions, a bone window (of variable dimensions) was carved into the anterior wall of the maxillary sinus using a Safescraper angled bone scraper and collector (Zimmer Dental Iberica®) (Fig. 5), thereby simultaneously obtaining a variable volume of particulate bone that was subsequently used to pack the cavity. No rotating instrument was used during the antrostomy or sinus elevation phase. Once the Schneider membrane was uncovered, it was elevated by following the usual procedure. The volume of particulate bone obtained was measured for its subsequent insertion into the cavity.
Results
Nine consecutive patients were included in the study, five males and four females; 10 sinus elevations were performed and a total of 16 implants were placed at these sites. Results are shown in Table 1. The procedure could be completed in all cases. The mean antrostomy surface area was 0.55 cm2; the mean volume of particulate graft, which was only obtained from the antrostomy opening, was 0.56 cm3; the mean height of alveolar crest previous to the procedure was 5.6 mm and a mean height of 11.7 mm was achieved by the intervention; 14 of the 16 implants were inserted immediately, and the remaining 2 implants were placed in a second stage. There was only one intraoperative membrane perforation, which was < 1mm and did not entail interruption of the procedure. In two of the elevations, supplementary allogeneic materials were required (bank bone or Bio-oss®), because the volume of bone collected was insufficient for the purpose. In the other elevations, the material obtained from the antrostomy proved adequate. All patients were followed up from the start of the treatment to 6 months after implant loading. No infectious complications were observed that caused treatment modifications. An overall success rateof 93.7% was recorded at six months after implant loading, with the loss of one implant.
Discussion
In general, there are two types of sinus elevation technique: the atraumatic technique described by Summers (8) in 1994, used for elevations of only a few millimetres (9); and the classic or open technique, performed by creating an antrostomy in the anterior wall of the maxillary sinus. There are three main procedures for performing this antrostomy (10):
1. Using a ball drill to cut a surface area of variable dimensions until visualization of the Schneider membrane by the change in colour.
2. Using a fine bur to cut a rectangle or circle that includes only the ridge until the entire perimeter of the membrane is visualized. A greenstick fracture is then performed such that the bone surface within the cut perimeter is introduced into the sinus, placed on what will be the new sinus floor.
3. Performing a complete osteotomy by antral approach on the external side of the maxilla, fully releasing the bone fragment demarcated by the fenestration and exposing the Schneider membrane.
After each of the above procedures, the sinus mucosa is then detached and elevated. The first technique is the most widely used. In all techniques, continuous irrigation is required during cutting to avoid excessive heating of the bone. There is some risk of damaging the membrane when it is pressed by the bur, which occasionally leads to interruption of the procedure. Furthermore, the use of irrigation leads to scraped bone being washed away by the solution and lost. New piezoelectric devices have been introduced for bone collection that avoids damage to the membrane, which is preserved. However a very thin bone tissue is obtained, which is difficult to collect and is mostly lost due to the constant irrigation required.
After performing the antrostomy and subsequent sinus elevation, material is required to fill the cavity. This material may be autogenous or allogeneic but must be able to compact the space so that it can serve as an anchorage for the implant. Multiple sites have been reported for autogenous bone collection. Gonzalez and Naval (11) described several extra-oral sites that gave good results, including tegmentum, tibia and anterior and posterior iliac crest (12). The most widely reported intraoral sites are the maxillary tuberosity, mandibular ramus, chin and zygomatic buttress (13, 14). However, these grafts, whether intra- or extra-oral, increase the morbidity of the procedure, and patients are sometimes unwilling to accept this risk.
In most cases, the problem is solved by using other exogenous materials, e.g., bank bone, hydroxyapatite or polyglycolic acid compounds, tricalcium phosphate or Bio-Oss® (15, 16). They are usually in the form of minute particles that must be mixed with a solvent, e.g., saline solution, blood or plasma, before they can be handled and placed within the sinus cavity.
When the bone crest height is > 4-5 mm, implants can be inserted in the same surgical act, provided that primary stability is assured (17-19).
The technique described in the present article is a simple and safe procedure that offers advantages to both patient and surgeon. There is lower morbidity for the patient, who avoids further incisions or larger mucoperiosteal flaps to uncover new areas for obtaining autogenous bone. In large elevations, it avoids or decreases the amount of allogeneic material inserted, which always entails the possibility of rejection by the recipient. The graft obtained is easily manipulated, given that the particulate bone is obtained with the clot that is formed around it, enabling practical and simple cutting, compacting and handling. Finally, the technique is less costly, which should be taken into account since the patient is directly affected.
One possible shortcoming is that the window opening process is somewhat slower than when performed with a drill. On the other hand, since there is no need for continuous irrigation, there is a better visualization of the membrane throughout the procedure. This is an important consideration because it affords greater safety, evidenced by the low frequency of sinus membrane perforations with this approach.
Evidently, the width of sinus wall differs among patients; therefore the amount of graft obtained by this technique is variable. If the graft obtained is inadequate for the purpose, it can be supplemented by harvesting additional amounts from other anatomic sites known to be appropriate. We highlight the zygomatic buttress area, due to its proximity and because it is a major source of bone graft. It is also possible to supplement the volume with commercially available allogeneic materials.
The mean volume of particulate bone obtained by this technique is very similar to the volumen of commercially supplied allogeneic materials, which usually ranges from 0.5 to 1 cm3. An additional advantage is that autogenous bone contains live osteoblasts that will favour osteogenesis and subsequent ossification.
Conclusions
The use of bone scrapers to create an antrostomy for sinus elevation is a simple and very safe procedure. It enables the collection of variable amounts of easily handled particulate bone graft that is highly useful for packing the cavity that will elevate the sinus membrane.
References
1. Sorni M, Guarinos J, Garcia O, Penarrocha M. Implant rehabilitation of the atrophic upper jaw: a review of the literature since 1999. Med Oral Patol Oral Cir Bucal 2005;10:45-56. [ Links ]
2. Boyne PJ, James RA. Grafting of the maxillary sinus floor with autogenous marrow and bone. J Oarl Surg 1980;38:613-16 [ Links ]
3. Caldwell G. Diseases of the accessory sinuses of the nose and an improved method of treatment for suppuration of the maxillary antrum. N J Med 1893;58:526. [ Links ]
4. Costantino PD, Friedman CD. Synthetic bone graft substitutes. Otolaryngol Clin North Am 1994;27:1037–74 [ Links ]
5. Aichelmann-Reidy ME, Yukna RA. Bone replacement grafts. The bone substitutes. Dent Clin North Am 1998;42: 491–503 [ Links ]
6. Sailer HF, Weber FE. Bone substitutes. Mund Kiefer Gesichtschir 2000;4 Suppl 1:384–91 [ Links ]
7. Zimmermann R, Jakubietz R, Jakubietz M, Strasser E, Schlegel A, Wiltfang J. Different preparation methods to obtain platelet components as a source of growth factors for local application. Transfusion 2001;41:1217–24 [ Links ]
8. Summers RB. A new concept in maxillary implant surgery: the osteotome technique. Compend Contin Educ Dent 1994;15:152-62. [ Links ]
9. Calvo-Guirado JL, Saez-Yuguero R, Pardo-Zamora G. Compressive osteotomes for expansion and maxilla sinus floor lifting. Med Oral Patol Oral Cir Bucal 2006;11:52-5. [ Links ]
10. Salagaray-Lamberty V, Lozada-Lorencez J. Tecnica de elevación sinusal. Injerto subantral de inducción osea. 1993, ADS Printing, S.A. [ Links ]
11. González-García R, Naval-Gías L, Muñoz-Guerra MF, Sastre-Pérez J, Rodríguez-Campo FJ, Gil-Díez-Usandizaga JL. Preprosthetic and implantological surgery in patients with severe maxillary atrophy. Med Oral Patol Oral Cir Bucal 2005;10:343-54. [ Links ]
12. Nkenke E, Weisbach V, Winckler E, Kessler P, Schultze-Mosgau S, Wiltfang J. Morbidity of harvesting of bone grafts from the iliac crest for preprosthetic augmentation procedures: a prospective study. Int J Oral Maxillofac Impl 2004;33:157–63 [ Links ]
13. Lundgren S, Moy P, Johansson C, Nilsson H. Augmentation of the maxillary sinus floor with particulated mandible: a histologic and histomorphometric study. Int J Oral Maxillofac Impl 1996;11:760–66. [ Links ]
14. Misch CM. Comparison of intraoral donor sites for onlay grafting prior to implant placement. Int J Oral Maxillofac Impl 1997;12:767–76 [ Links ]
15. Orsini G, Traini T, Scarano A, Degidi M, Perroti V, Piccirilli M, et al. Maxillary sinus augmentation with Bio-Oss particles: a light, scanning, and transmission electron microscopy study in man. J Biomed Master Res B Appl Biomater 2005 Jul;74:448-57 [ Links ]
16. Papa F, Cortese A, Maltarello MC, Sagliocco R, Felice P, Claudio PP. Outcome of 50 consecutive sinus lift operations. Br J Oral Maxillofac Surg 2005 Aug;43:309-13. [ Links ]
17. Stricker A, Voss PJ, Gutwald R, Schramm A, Schmelzeisen R. Maxillary sinus floor augmentation with autogenous bone grafts to enable placement of SLA-surfaced implants: preliminary results after 15-40 months. Clin Oral Impl Res 2003; 14: 207-12 [ Links ]
18. Khoury F. Augmentation of the sinus floor with mandibular bone block and simultaneous implantation: a 6 – year clinical investigation. Int J Oral Maxillofac Implants 1999; 14:557-64 [ Links ]
19. Peleg M, Mazor Z, Garg AK. Augmentation grafting of the maxillary sinus and simultaneous implant placement in patients with 3 to 5 mm of residual alveolar bone height. Int J Oral Maxillofac Implants 1999; 14: 549-56. [ Links ]
![]() Correspondence:
Correspondence:
Dr. Pedro Martos Díaz.
Hospital de la Princesa. Departamento de Cirugía Maxilofacial.
C/ Diego de León N° 62.
28006. Madrid. Spain
E-mail: plmartos@mixmail.com
Received: 23-08-2006
Accepted: 15-07-2007