My SciELO
Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO -
 Access statistics
Access statistics
Related links
-
 Cited by Google
Cited by Google -
 Similars in
SciELO
Similars in
SciELO -
 Similars in Google
Similars in Google
Share
REC: Interventional Cardiology
On-line version ISSN 2604-7276Print version ISSN 2604-7306
REC Interv Cardiol ES vol.5 n.4 Madrid Oct./Dec. 2023 Epub Mar 04, 2024
https://dx.doi.org/10.24875/recic.m22000322
Clinical cases
Massive hemoptysis. Selective embolization of bronchial artery-left pulmonary artery fistula. Case resolution
aServicio de Cardiología, Unidad Cardiovascular, Sanatorio Allende, Córdoba, Argentina
bServicio de Neumonología, Sanatorio Allende, Córdoba, Argentina
cServicio de Diagnóstico por Imágenes, Sanatorio Allende, Córdoba, Argentina
CASE RESOLUTION
Emergency transfer of the patient to the cath lab was decided for pulmonary angiography and endovascular embolization. A 5-Fr femoral introducer sheath was used to insert a vertebral catheter with which a largely developed bronchial branch was selectively catheterized (emergency from the aortic arch) towards the pulmonary parenchyma creating a high-flow arterio-arterial fistula with a segmental arterial branch of the lung left upper lobe (video 1 of the supplementary data). Afterwards, a 2.4-Fr (proximal diameter)/1.9-Fr (distal diameter) Echelon 14 microcatheter was passed (Medtronic, United States) through which 2 6 mm × 20 mm Axium Prime 3D detachable coils (Medtronic, United States) were implanted from the distal to the middle third of the bronchial tree (figure 1). The target vessel was successfully embolized resulting in an overt decrease of the cardiac output at fistula level (video 2 of the supplementary data). Procedure was performed uneventfully. After it was completed the amount of vasopressor drugs (noradrenaline and vasopressin) administered was gradually reduced. Forty-eight hours later, the patient was extubated and weaned from mechanical ventilation. Seventy-two hours after the procedure, a follow-up coronary computed tomography angiography confirmed consolidation in the apical and posterior segments of left lower lobe and left perihilar region without evidence of contrast extravasation at the embolization site. Since the patients showed no signs of hemoptysis she was discharged from the hospital 6 days after admission.
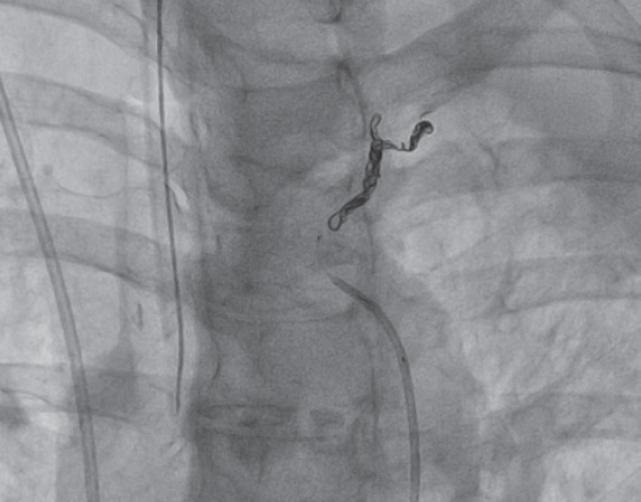
Figure 1. Angiography. Axium Prime 3D detachable coils (6 mm × 20 mm) implanted from the distal to the middle third of the bronchial tree.
Pulmonary circulation depends on pulmonary and bronchial arteries alike. While the pulmonary artery and its branches make up a low-pressure system that supplies the pulmonary parenchyma mainly, the circulation tha comes from the bronchial arteries has a relatively high pressure and supplies the endobronchial tree basically. It is responsible for only 2% of the lung overall vascular supply. In 90% of the cases of potentially life-threatening hemoptysis the origin of bleeding is the bronchial followed by the pulmonary arteries or an unidentified source of bleeding in the remaining 10% of the cases.1 Regarding the main etiologies involved, the case series published to this date include bronchiectasis, tuberculosis, and pulmonary malignant neoplasms. Although its exact incidence rate is still unknown, systemic-pulmonary fistula is rare and has often been misrepresented as the cause of hemoptysis. In cases of massive hemoptysis, treatment depends on the underlying cause. Early treatment involves stabilizing the patient and, when available in the emergency setting, bronchoscopy can be useful. In suspicious or confirmed cases on the computed tomography scan of systemic-pulmonary fistula, arteriography and endovascular embolization are elective while surgery should be spared for selected cases.2 In the metanalysis conducted by Zheng et al.2 the embolization of the bronchial artery due to massive hemoptysis (21 studies, 2511 cases) had rates of minor and major complications of 10% and 2%, respectively. Compared to the surgical treatment of hemoptysis, the endovascular procedure had a lower rate of adverse events.3 On the other hand, in these cases, conservative treatment is associated with mortality rates > 50%
The case presented here shows the severity and hemodynamic compromise due to massive hemoptysis following an extremely rare cause with effective endovascular resolution.
The patient gave her informed consent for publication purposes.
REFERENCES
1. Charya AV, Holden VK, Pickering EM. Management of life-threatening hemoptysis in the ICU. J Thorac Dis.2021;13:5139-5158. [ Links ]
2. Zheng Z, Zhuang Z, Yang M, et al. Bronchial artery embolization for hemoptysis: A systematic review and meta-analysis. J Interv Med. 2021;4:172-180. [ Links ]
3. Ittrich H, Bockhorn M, Klose H, Simon M. The Diagnosis and Treatment of Hemoptysis. Dtsch Arztebl Int. 2017;114:371-381. [ Links ]
SEE RELATED CONTENT:
https://doi.org/10.24875/RECICE.M22000324https://doi.org/10.24875/RECICE.M22000325SUPPLEMENTARY DATA
https://doi.org/10.24875/RECICE.M22000326Supplementary data associated with this article can be found in the online version available at https://doi.org/10.24875/RECICE.M22000326.











 text in
text in 


