INTRODUCTION
The mission of the Hospital Pharmacist (HP) is to "improve health, through specialised pharmaceutical care, promoting the appropriate, safe and cost-efficient use of medicines in the hospital environment and its areas of influence" [1].
This profession has evolved considerably, as initially professionals were dedicated only to dispensing medicines to cover the needs of medical prescriptions. However, over time, new professional roles have been acquired that have allowed them to develop their profession.
One of the most important challenges has been the incorporation of the fourth year of residence in the specialized health training of the Resident Internal Pharmacists [2], since it was necessary to acquire clinical skills and redefine a drug-centered activity towards one that is person-centered with the aim of achieving an optimal and quality pharmacotherapy plan, adjusted to the needs and characteristics of each individual.
At present, HP is beginning to be included in multidisciplinary clinical groups, one of which is the l Emergency Department (ED).
WHY CAN THE HOSPITAL PHARMACIST BE USEFUL FOR THE EMERGENCY DEPARTMENTS?
The ED is a complex area where, in certain occasions, time is of the essence and there is a potential risk of Medication Related Problems (MRP).
MRP are those situations in which using medication can cause the appearance of a Medication-Related Negative (MRI). These MRI have negative implications for public health as they pose a high risk of morbidity and mortality and increased health costs [3].
There are several studies such as: "To error is human", ENEAS or EVADUR that show prevalence greater than 3% and an avoidability rate between 40-70% [4, 5, 6]. Several precipitating risk factors have been identified [7]:
Chronification of diseases.
Aging population: multipathological elderly and with polypharmacy.
Some of the medication used in the ED is classified as complex such as vasoactive amines, amiodarone, intravenous insulin, etc.
Lack of standardization in the preparation of sterile and non-sterile mixtures.
High workload of professionals: high volume of patients attended, shifts, high staff rotation, inexperience, fatigue, etc.
Inability to concentrate properly: rapidity of action, multitasking and interruptions
Use of verbal orders and absence of electronic medical records.
Absence of a Hospital Pharmacist on the team.
These facts are attributed not to inadequately trained or incapable professionals, but to a system not robust enough to avoid these problems. This scenario is where HP can contribute to reduce/avoid these problems.
THE HOSPITAL PHARMACIST
There are studies, especially in the USA [8], which shows the benefit of incorporating hospital pharmacists into the ED due to their high level of knowledge in areas such as pharmacology, toxicology and pharmacokinetics. These skills seem to be capable of improving processes, reduce/avoid MRP, improve the quality of the service provided and save on health costs, without incurring in additional charges by employing a HP.
Some Spanish studies have been carried out such as the work of Crespí et al. [9], which was based on the physical presence of a pharmacist from 8:00-15:00 in the observation room and boxes. The Pharmaceutical interventions involved 235 medicines, 242 patients and 149 interventions. 51% of these interventions were considered to be MRP with an average of 1.3 patients, 43% changing medicines and 27.5% changing doses with an acceptance rate of 98%.
Another more recent study by Ucha et al. [10] also showed that the pharmacist was working from 8:00-15:00 in the observation and pre-admission rooms. In this case, the average number of interventions was 1.8 patients, with 40% of them being MRP, which reduced the risk of increasing hospital stay by 10-30%.
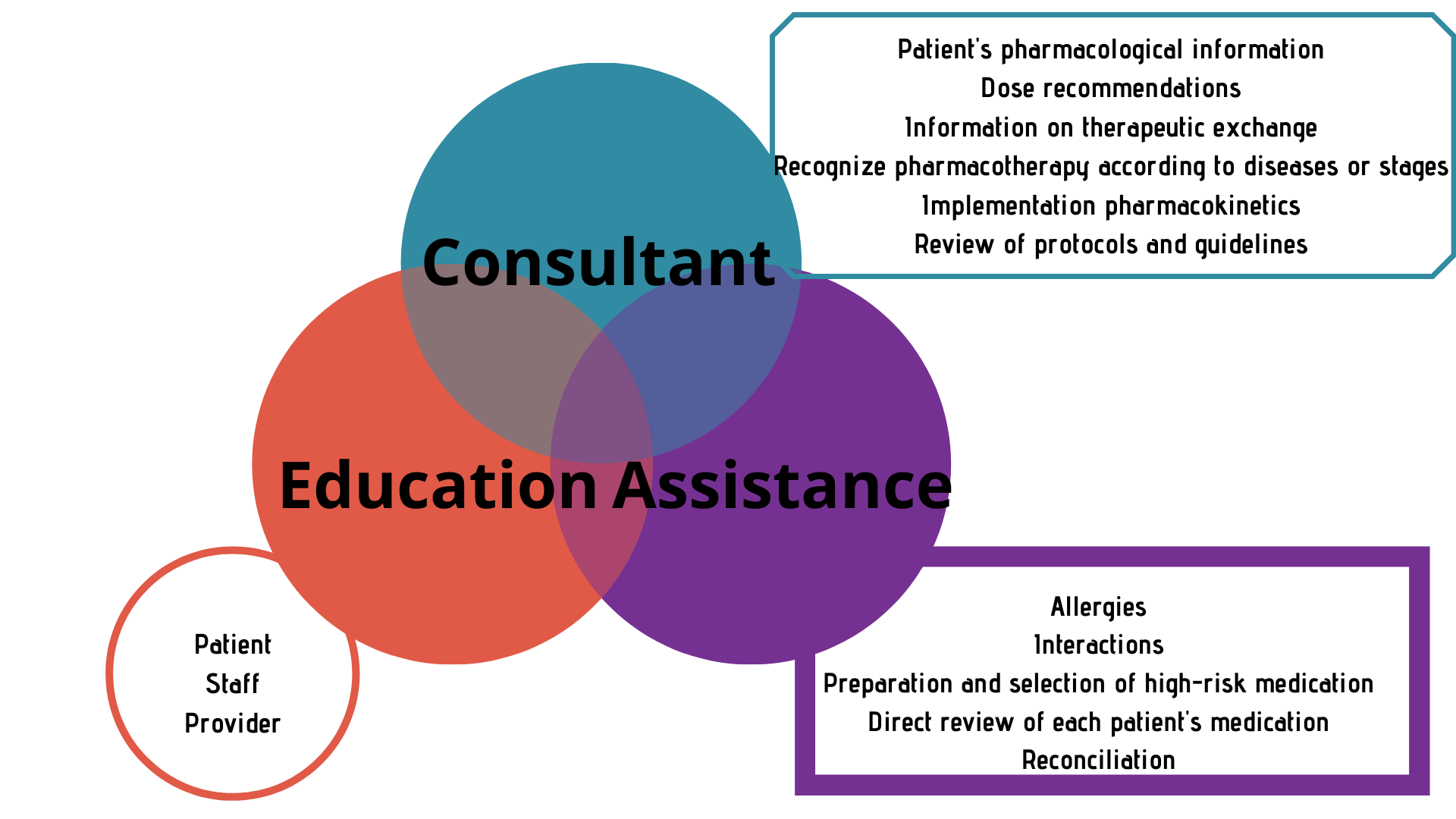
The interventions that a HP can carry out are: advisory role based on information on medications, dose adjustment, resolution of consultations with nursing staff, therapeutic exchanges, recommendation to initiate necessary medications, information on compatibility between medications, review of protocols, information on allergies, etc. (Figure 1).
CONCLUSIONS
The Hospital Pharmacy has evolved into a specialized health profession, acquiring new professional roles in recent years. The amassing of clinical skills in order to allow pharmacist to face new challenges, such as the inclusion in multidisciplinary teams stands out among these new capabilities.