THE HEALTH CARE SYSTEM IN DENMARK
The population of Denmark in year 2020 was 5.8 million people. Everyone who has been granted a residence permit and lives in Denmark has free access to health care services, including visits to a general practitioner (GP), hospital, emergency room, out-of-hours medical service and when citizens have a referral from GP also visits to specialists and psychological counselling. In addition, municipal support, home care, nursing home care and care at residential facilities are paid by the government except for rent and meals.1 In 2017, the Danish government spent 182 billion DKK (24 billion EUR) on public health care, which is approximately 32,000 DKK (4,300 EUR) per citizen.2 In 2016, the public health expenditure was 9.8% of the Danish GDP compared to 7.9% in 2000.3 Citizens in Denmark pay taxes of their salary, accounting for approximately half of the salary, which include finances for health care services. The responsibility for health and social care is shared between the central government, the regions and the municipalities.
Denmark is divided into five regions and 98 municipalities. One of the main regional tasks is to manage the hospital system, which is divided into general hospitals treating all conditions and psychiatric hospitals. Health care services provided by private practitioners, including general practitioners, specialists physician, physiotherapists, chiropractors, psychologists, dentists and podiatrists are also organised by the regions.4 The municipalities handle primary health care at a local level as well as other welfare services.5 Within health care and social services the 98 Danish municipalities handle rehabilitation, home care, prevention of abuse, dental care, promotion of health, care for the elderly and disabled, psychiatric treatment, social psychiatry, placement of neglected children and specialised education following the principle of decentralisation “what can be dealt with on a local basis is dealt with on a local basis”.5
POLICIES AND STRATEGIC PLANS FOR THE DEVELOPMENT OF PRIMARY HEALTH CARE
Public health is a national and local focus. National and local strategies seek to enhance public health through national and local initiatives initiated by different stakeholders. By adopting WHO's definition of public health as “the art and science of preventing disease, prolonging life and promoting health through the organised efforts of society”, the Danish authorities have implemented good public health and uniform health care services of high professional quality across Denmark. Initiatives, such as reducing smoking, the consumption of alcohol, lack of exercise and risk factors of malnutrition are addressed nationally by the Danish Health Authority in campaigns and through funding of local initiatives at municipality level.6 The Danish Health Authority is responsible for promoting public health and setting the framework and direction for health and elderly care. The strategic mission of the Danish Health Authority is “Health for all”. The Danish Health Authority works across areas of expertise and sectors to achieve this mission.7
In 2014, the government launched a plan for health entitled: “Healthier lives for everyone - national goals for the health of Danes within the next 10 years”.8 The plan encompasses seven national goals that provide the framework for an ambitious health promotion and disease prevention policy. The goals focus on diet (obesity), smoking, alcohol, exercise, mental health (one goal for children and one goal for adults) and social inequality.8 The overall objective is to prolong the healthy years of life and to reduce inequality in health. A key element in the plan is that preventive work should be based on collaboration and partnerships between public health providers, authorities, civil society and private organisations. The government launched a partnership strategy to help achieve the national goals within 10 years, and allocated 120 million DKK (16 million EUR) to establish partnerships which ensure local ownership and anchoring of the goals.8 Professional organisations are mentioned as organisations which should enter partnerships with e.g., patient, family and GP about better health. The Association of Danish Pharmacies and the community pharmacies can play a role in this strategy.
The Danish Patient Safety Authority and the Danish Medicines Agency carry out inspections in the different health care institutions and with individual health care professionals, including community pharmacies.9,10 Community pharmacies, private hospitals and clinics, pre-hospital services and municipalities are offered quality accreditation from the Danish Quality Model, and 85% (by September 2020) of the community pharmacy owners make use of this accreditation to measure and ensure the quality of their pharmacy practice.11
COMMUNITY PHARMACIES: FROM RESEARCH TO COMMUNITY PHARMACY SERVICES
As of October 2020, there were 506 community pharmacies in Denmark, including pharmacy branches, with a turnover of 12.2 billion DKK (1.63 billion EUR) in 2019.12 Community pharmacies are privately owned with only pharmacists owning a pharmacy, following a license given by the Danish Medicines Agency. Medication prices are regulated by the health authorities. Prescription medications account for 73% of the total turnover, 9% is over-the-counter (OTC) medication, 1% is health care services, 15% is other care products and free trade products and 2% is sale between pharmacies.12 Some OTC medications are sold in retail but generally Danish community pharmacies have a monopoly for medicines. The number of staff in Danish community pharmacies is approximately 12 staff per pharmacy, and the approximate turnover for the pharmacies is 25 million DKK (3.3 million EUR) with a great difference between the rural pharmacies and city pharmacies.12
The Danish pharmacy law sets the terms for community pharmacies in Denmark. In 2015 this law changed with the objective to maintain and develop the community pharmacies as part of the health care system. Community pharmacies must, both before 2015 (since early 1990's) and after the 2015 law, dispense and counsel on medication. A change in the law increased the competition between pharmacies, because the new law made it possible for every community pharmacy owner to open a maximum of seven pharmacy branches (apart from the main pharmacy) in a range of 75 km.13 This was undertaken to achieve increased patient accessibility.14 The location and distribution of main community pharmacies are regulated by the state, ensuring broad public accessibility and the branches mentioned above can be opened in a range of 75 km. In 2018, the average distance for Danish citizens to their nearest community pharmacy or pharmacy branch was reduced to approximately 3.3 km from 3.8 km in 2015.15 Every citizen in Denmark can walk into a community pharmacy without an appointment and obtain counselling on the safe and effective use of medication and disease prevention by a trained health care professional. On an annual basis, community pharmacy staff serves the majority of the Danish population (94%).16
Despite the change in law from 2015, community pharmacies in Denmark still have some of the largest pharmacy units in Europe with regard to the number of staff (approximately 12 per pharmacy) as well as the number of citizens per pharmacy (approximately 11,800 citizens per pharmacy).12 Danish community pharmacies employ 777 pharmacists (equivalent to 644 full-time employees) holding a five-year MSc degree in pharmacy and 2,737 pharmacy technicians with a three-year academy profession degree (equivalent to 2,336 full-time employees) and 446 pharmacy technician students. Approximately 210 pharmacist interns complete their pharmacy internship every year at a Danish community pharmacy.
The main activities of Danish community pharmacies are to ensure medication supply, distribute medication and counsel patients about prescription and OTC medication, to support implementation of correct medication use and to contribute to health promotion.17,18 Community pharmacists and pharmacy technicians, similarly to other health care professionals, have electronic access to patients’ prescribed medication through the so-called Shared Medication Record. The Shared Medication Record shows an overview of prescribed medications for all Danish citizens and the prescription data e.g., when is it obtained from the pharmacy, which pharmacy, how much is obtained and who is the prescribing physician. It is not a full clinical record.
Community pharmacies in Denmark have been increasingly incorporated into the health care system over the years through political negotiations, as they play a key role in delivering professional pharmacy services and as they ensure this support for patients and other professionals through wide availability of counselling and pharmacy services. At the moment there is a lack of general practitioners (GPs) in Denmark. This provides an opportunity for expanding the collaboration between community pharmacies and GPs, which could relieve the GPs in their practice and ensure patients’ needs.
Danish community pharmacies offer pharmacy services in primary health care, supporting public health with a focus on medication. The aim of these services is to ensure patient and medication safety through the implementation of rational drug therapy and correct use of medication.17,19 The number of remunerated pharmacy services available for patients have increased since the millennium and in 2020 include six services from the community pharmacies which are fully or partly remunerated by the government. The Inhalation Technique Assessment and the vaccination service for specific patient groups are fully remunerated.19-23 According to the pharmacy law, community pharmacies are obliged to deliver the New Medicines Service.19,24 The price for the service is a subsidy to the pharmacy which is imposed in the pharmacy law on payment and calculation of all fees and subsidy in the pharmacy sector. The Medication Adherence Service is agreed upon the gross profit agreement between the Ministry of Health and the Association of Danish Pharmacies with a set price for each service in a similar manner to that of medication supplied.19,25
Every second year a gross profit agreement is agreed between the Ministry of Health and the Association of Danish Pharmacies. The gross profit is the Danish community pharmacies’ total contribution margin for all goods (drugs and other products) and services. It is calculated as the entire turnover minus the consumption of goods and must cover all expenses in the pharmacy. In the gross profit agreement the total profit margin for the pharmacies is imposed.26
There are two central elements:
1) The profit margin agreed upon in the gross profit agreement, which is the limit for how much all the pharmacies in total are allowed earning on sales of medication and other products including pharmacy services. In 2020 the margin is 2.7 billion DKK (360 million EUR).
2) The profit on each medication, which is a specific amount that the pharmacies can add to the purchase price on each medication they sell. This has since 2019 been 5.46 DKK (0.73 EUR), no matter the price of the medication. If the community pharmacies together exceed the profit margin the profit on each medication is decreased. Since 2015, the profit on each medication has halved from 10.96 DKK (1.46 EUR) to 5.46 DKK (0.73 EUR) in 2019. For prescription medication there is also a prescription fee of 8.00 DKK (1.07 EUR)) added.12
Finally, two services are partly remunerated by the government, partly by the patient; re-prescribing for a limited number of medications, e.g. insulin and blood pressure medication, and automated dose dispensing with subsidy.19,27 The year of establishment and remuneration and number of services delivered from the community pharmacies each year is described in Table 1.12 In 2019 the total turnover of pharmacy services others than distribution and counselling of medication was 122 million DKK (16.3 million EUR) (1% of the total turnover at the Danish community pharmacies).12
Table 1. National level remuneration of Danish community pharmacy services, year of establishment and remuneration, number delivered and approximately turnover in 2019
| Remunerated pharmacy service at national level | Year of establishment and remuneration | Number delivered (2019)12 | Approximately turnover (2019) |
|---|---|---|---|
| Inhaler Technique Assessment Service19,20,28-32 | 2005 | 64,000 | 3.5 million DKK (467,000 EUR) |
| New Medicine Service19,24,33 | 2015 | 20,000 | 3.2 million DKK (427,000 EUR) |
| Vaccination service for defined risk patient groups22,23 | 2015 | 120,000 (influenza vaccines) | 22.4 million DKK (3.0 million EUR) |
| Medication Adherence Service for patients with chronic conditions with signs of low adherence19,25,34-38 | 2018 | 6,800 | 1.1 million DKK (147,000 EUR) |
| Re-prescribing service27 (partly remunerated at a national level, partly by the patient) | 2019 | 17,750 (July 2019-September 2020) | 586,000 DKK (78,000 EUR) (July 2019-September 2020) |
| Automated dose dispensing with subsidy which is prescribed from a physician or a prescribing pharmacist27,39,40 (partly remunerated at a national level, partly by the patient) | 2001 (prescription from physician) 2020 (prescription from prescribing pharmacist) | 44,200 (number of patients) | 65.3 million DKK (8.7 million EUR) |
Description of Danish community pharmacy services
Since 2005, the Danish community pharmacies have been obliged to offer an Inhaler Technique Assessment Service to new or experienced patients who use any kind of inhalation device. The service is delivered by either a pharmacist or a pharmacy technician and aims to optimise patient outcome by assessing the patient's inhalation technique through demonstration and teach-back.19,20,28-32
The New Medicines Service (NMS) targets patients diagnosed with a new chronic condition and who are initializing medication within the last six months. The service is provided by pharmacists and consists of a counselling session and a face-to-face or phone-based follow-up session 2 - 4 weeks after the counselling session. The counselling focuses on the patient's new medicine and on how the pharmacy can support the patient's medication management by providing knowledge about the treatment and disease, so the patient can establish appropriate practice and handle difficulties with their medication to prevent non-adherence.19,24,33
A Medication Adherence Service, was launched in 2018. This is similar to the NMS but is offered to a different target group. The Medication Adherence Service is available for patients who have been in long-term treatment for more than one year and who show signs of low medication adherence. The Medication Adherence Service aims to support non-adherent patients in establishing an appropriate practice for their medication, e.g. with motivation, knowledge and support.19,25,34-38 As part of the pharmacy law Danish community pharmacies are obliged to provide both the New Medicines Service and the Medication Adherence Service.
In 2015, the first community pharmacies commenced travel vaccination. An increasing number of community pharmacies now offer this vaccination service. The program also includes influenza vaccination and, most recently (in April 2020), pneumococcal vaccination which both are remunerated for defined risk groups.22,23 Community pharmacists and pharmacy technicians in Denmark handle vaccinations on the responsibility of a physician for a patient group, defined by law and by the physician. Danish law describes that some tasks in the health care sector can be delegated from the physician to another health care professional e.g. a pharmacist, pharmacy technician or nurse.41
Since 2019 it has been obligatory for all Danish pharmacies to offer a re-prescribing service for specific target groups. This service must be provided by a prescribing pharmacist to a patient who has run out of prescription medication but does not have any prescriptions left. A prescribing pharmacist can then re-prescribe and dispense the medication for the patient once without the patient needing to visit the physician. Re-prescribing can be carried out once for a limited number of medications, e.g., insulin and blood pressure medication, to patients. Community pharmacists are trained as so-called prescribing pharmacists. The title is given to community pharmacists who have obtained a task-specific authorisation from the health authorities to re-prescribe specific medication and prescribe remunerated, automated dose-dispensing (described next).27 Furthermore, the law made it possible in 2020 for the prescribing pharmacists to also provide an automated dose-dispensing with subsidy from the government. The Automated dose-dispensing can be fully paid by the patient or with subsidy when getting a prescription on the dose-dispensing from a physician or a prescribing pharmacist. All medication in the dose-dispensing package need to be prescribed by a physician.27,39,40
Danish community pharmacies also provide pharmacy services for other health care sites and professionals e.g., nursing homes, home care and residential facilities. Some of these services are remunerated at a local level by the municipalities. Examples of these are smoking cessation, medication review, educational programme and quality assurances of the medication process for staff handling medication in order to improve work procedures and medication information for patients and relatives.16,19,29,30,35,37,38,42,43,44-55 These services are remunerated by local contracts with municipalities or individual institutions. For example, a municipality may have a contract with a community pharmacy to provide an educational programme about medication handling with three days of teaching for all staff handling medication at all adult residential facilities in the municipality. Another example is that a nursing home make contract with a community pharmacy about medication review for all residents taking more than five medications. In 2019, the estimated number by the Association of Danish Pharmacies’ was that the Danish community pharmacies collaborated with 64 out of 98 municipalities about one or more of the above mentioned services.
A limited number of the pharmacy services such as medication review and smoking cessation are paid by individual patients but there is no data on the number, and it is estimated to be happening to only a limited degree.
The foundation of Danish community pharmacy services
Pharmaceutical services at Danish community pharmacies commenced with the adoption of the concept pharmaceutical care, as defined by Hepler and Strand in 1990.56 The development of community pharmacy services in Denmark is founded on scientific evidence to ensure that the benefits intended for patients and society are accomplished. Research studies have been conducted by the Danish College of Pharmacy Practice, The University of Copenhagen, The University of Southern Denmark, the Danish community pharmacies, the Association of Danish Pharmacies and international collaborators, e.g., Pharmaceutical Care Network Europe.17-19 In recent years, the Danish government and authorities have provided project funding to establish collaboration and partnerships between pharmacies and municipalities on health promotion and disease prevention. These studies showed that the municipalities see an unutilised potential in the community pharmacies for access to vulnerable citizens and want the community pharmacies to play a role in early health promotion and disease detection for these citizens.57-63 The Association of Danish Pharmacies support the community pharmacies in entering into pharmacy service agreements.
VISION, MISSION, AND STRATEGIC PLANS FOR COMMUNITY PHARMACIES
In 2016, the Association of Danish Pharmacies, in consultation with the community pharmacies, decided on a strategy to 2020 with the title “The community pharmacy close to you”. The strategy takes patients, society's and community pharmacy's perspectives on the community pharmacy.14 The vision is: “The community pharmacy is acknowledged as the medication expert in society. We promote health and help patients achieve optimal use of medication. We take responsibility for coherence in medical treatment. Professionalism, quality and the safety of the patients are the foundations of our work.” The mission of the strategy is: “We ensure the provision and distribution of medication in Denmark, and with our knowledge about medication and disease prevention, we help patients achieve better health”.14
The strategy describes seven focus areas that will realise the three perspectives on the community pharmacy (patients’, society's and community pharmacy's):
Professionalism and counselling
Availability and service
Quality and safety
Business development and operation optimisation
Recruitment and competency development
Use of technology
Image and communication.14
Opportunities for Danish community pharmacies
The Association of Danish Pharmacies has suggested several new functions and services to be carried out by the community pharmacies (Figure 1).64
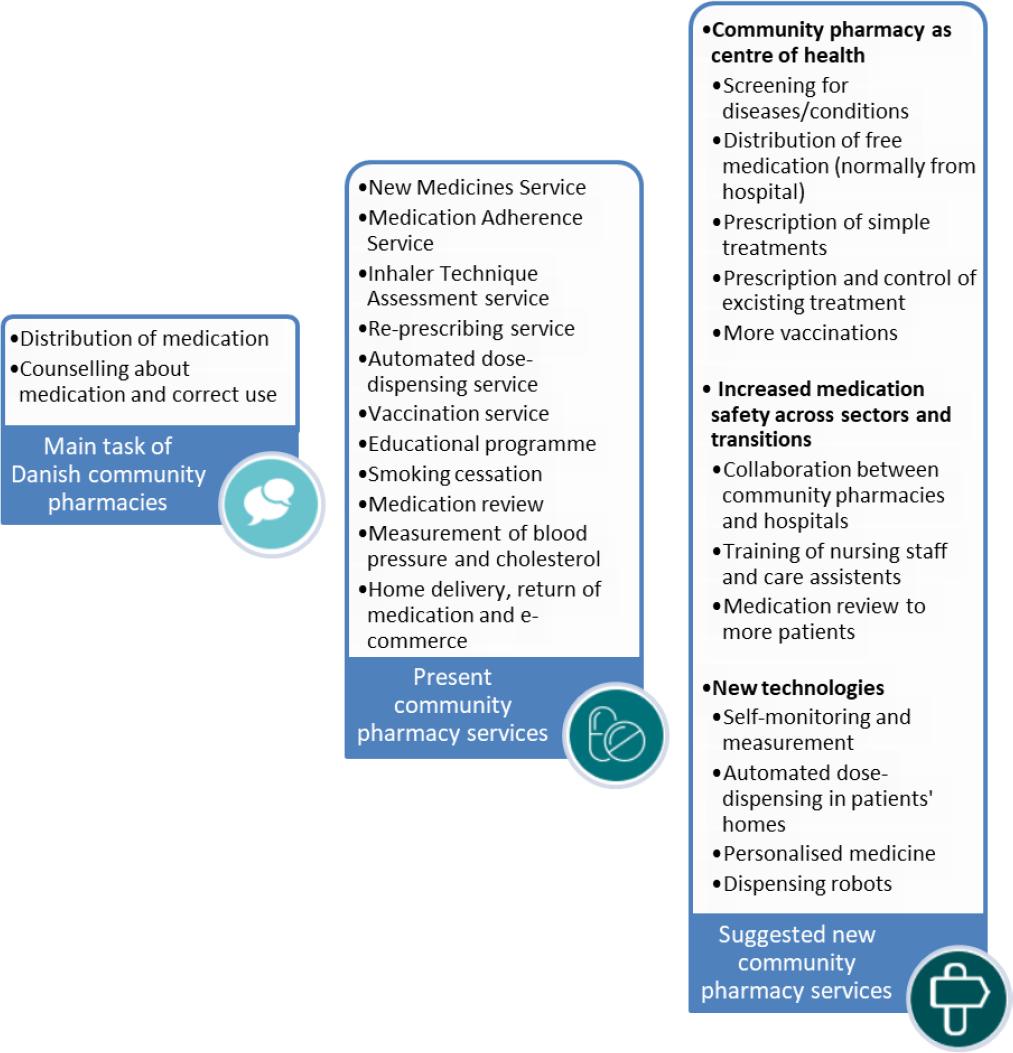
Figure 1 The main tasks, present services and suggested new services at community pharmacies in Denmark64
The future will bring new technology for dispensing, distributing and using medication, e.g., drones, robots and 3D printing. Danish community pharmacies should consider how their practice and counselling can be adjusted to these new technologies.65 There is also a potential in using new technology in communication with patients, such as health apps, video counselling and video follow-up on pharmacy services. Today, communication between community pharmacy staff and patients in Denmark most often takes place at the actual pharmacy, whereas studies of the use of virtual communication could lead to new and better ways to reach patient groups that rarely visit the pharmacy. However, pharmacies still need to oblige patients who need and want to have counselling and follow-up at the community pharmacy.
Challenges for Danish community pharmacies
The 2015 pharmacy law created extensive competition between community pharmacies with the number of pharmacies or pharmacy branches increasing by 60% by 2020.66 However, the gross profit agreement mentioned earlier has not been increased despite the 2015 law. This in turn, due to many community pharmacies have increased their sale of care products and free trade products e.g., vitamins, minerals, skin care products and bandages has unfortunately resulted in decreased profits on dispensing and counselling on medicines for all community pharmacies, due to the financial regulation in the gross profit agreement where the amount which the pharmacies can add to the purchase price on each medication they sell have decreased. Since 2015, the profit on medication has halved from 10.96 DKK (1.46 EUR) to 5.46 DKK (0,73 EUR) in 2019 possibly leading to a decreased focus on medication counselling.12 At the same time, the 2015 law has improved accessibility to community pharmacies in all Danish regions. The increased competition between pharmacies has changed the focus for the pharmacies because the competition places great demands on the pharmacies to optimise their operation while still maintaining a high quality of service and professionalism. Accordingly, there is a risk that less attention is paid to new community pharmacy services. On the other hand, each community pharmacy may have been given an incentive to develop their specific pharmacy and become the best community pharmacy for the patients. The extensive number of new community pharmacy branches requires highly qualified staff. For small pharmacies with only 2-3 staff providing pharmacy services in addition to counselling is rather challenging. The level of trust between pharmacy staff and patients is high in Denmark, with 83% of patients reporting satisfaction with pharmacy-based advice and counselling.67 Therefore, it is pivotal for community pharmacies to maintain their good image with the population. The trust is based on professionalism, safety and quality and continuing communication and clarity on the role of community pharmacies.
In Denmark, like in many other countries, there is an increasing problem with drug shortages. This creates demands on physicians and community pharmacies for the patients to receive their medication. As suggested in the section above on opportunities, the community pharmacies may have a role in prescribing and changing prescriptions to ensure dispensing of correct medication for the patients.
CONCLUSION
Community pharmacies provide and offer services in the primary health care sector in Denmark, offering six remunerated services as well as distribution of and counselling on medication. Community pharmacies are working to be seen as partners in the health care system. Interprofessional collaboration is recognised to be essential for an integrated health care sector. For community pharmacies to fulfil their potential of providing counselling and community pharmacy services, stronger bonds must be established between pharmacies and other health care professionals, from general practitioners and hospitals to elderly care and residential facilities. This role is increasingly being supported by the government through the remunerated pharmacy services and through contract with municipalities.
Denmark faces ongoing, unsolved problems with the use of medication, and the community pharmacies have excellent competencies in medication that must be utilised to a greater extent to solve these problems for patients as well as society. At the same time, community pharmacies need to focus on their main tasks of supply of medicines and implementation of services. This requires efficient management and an increased use of technology. The future may bring a pharmacy without walls (no psychical room or a smaller one) and therefore new distribution and communication channels must be investigated and implemented.
The education and further training of pharmacists and pharmacy technicians must develop, together with the community pharmacy sector meeting patients’ demands for high-level counselling and health care services in all Danish regions
Other critical issues in health care that can make demands on and affect the policy for community pharmacies in Denmark are multi-disease, an aging population, personalised medicine, green pharmacy, antibiotic resistance and challenges with medication in the transition of care and transitions between sectors.
This will enable community pharmacies to help patients with medication handling and treatment and to navigate in a complex health care system.














