Introduction
Diabetes mellitus is a major healthcare concern, as evidenced by its high prevalence rate in the general population (8.3%). With age the proportion of patients affected increases and it reaches 11% in the population over 65 years old. These figures are only indicative since it is considered that there is a similar proportion of undiagnosed patients, leading to a six-fold increase of the number of diabetic patients in the last forty years1.
Approximately between 15 and 25% of diabetic patients will present with foot ulcers throughout their life, this being the main cause of non-traumatic amputation worldwide. The overall prevalence rate of this complication is between 1.3 and 4.8%. These are developed by the convergence of several predisposing, triggering and aggravating factors.
- The following are considered predisposing factors: peripheral neuropathy, leading to a lack of sensitivity and motor neuropathy causing an imbalance between flexion and extension muscles which give rise to arthropathy; and the autonomic neuropathy which entails hyperkeratosis and dry skin.
- Triggers: any friction or injury
- Aggravating factors: infection and ischemia which determine the future of the limb and the patient.
Diabetic foot ulcers can be neuropathic or neuro-ischemic, a fact which will strongly determine their management. A delayed etiological diagnosis can lead to chronic healing with a potential risk for both the limb and the patient2.
The main objective of presenting this clinical case is to show the importance of etiological diagnosis and taking into account all factors within a diabetic foot ulcer.
Clinical case
61 year-old male patient diagnosed with type-2 diabetes mellitus (DM2) fourteen years ago. This diagnosis was initially accompanied by sensitive and motor peripheral neuropathy, metatarsophalangeal arthropathy with no signs of osteomyelitis and diabetic arthropathy.
The patient had presented ulcers in both his feet for ten years now, in the metatarsophalangeal area. These had never completely healed in this period. He did not present partial nor total amputations. He had needed several admissions in hospital due to recurrent infections and had needed debridement and IV antibiotics in multiple occasions. Amputation had been suggested before, but he had always refused it.
Currently and according to the patient himself, although he is aware of the main considerations in managing diabetic foot ulcers his compliance has not been as constant as it should have been, especially regarding pressure relief and offloading the area. He does not smoke and has never smoked and reports no further toxic habits. He has an appropriate metabolic control of his disease with 7.4% glycated hemoglobin values.
Medical treatment at the time of hospital admission:
- Lantus® insulin 28 units: once a day in the morning
- Apidra® insulin: if hyperglycemia
- Atorvastatin® 10mg: once a day
- Adiro® 100mg: once a day
- Hidroxil B1-B6-B12®: once a day
- Currently he is under no treatment for pain although previously he had been on Pregabalin® and Tramadol® but has discontinued this treatment due to secondary effects.
- Treatment for the ulcer until admission:
- Cures with therapeutic honey and cleaning with soft soap.
- Offload with 1cm-thick pads as a foot sole. He uses a stick to avoid weight bearing.
- Hyperoxygenated fatty acid compounds (HFAC): three times a day in both legs.
- Dressing to support the pad.
Physical exam upon admission
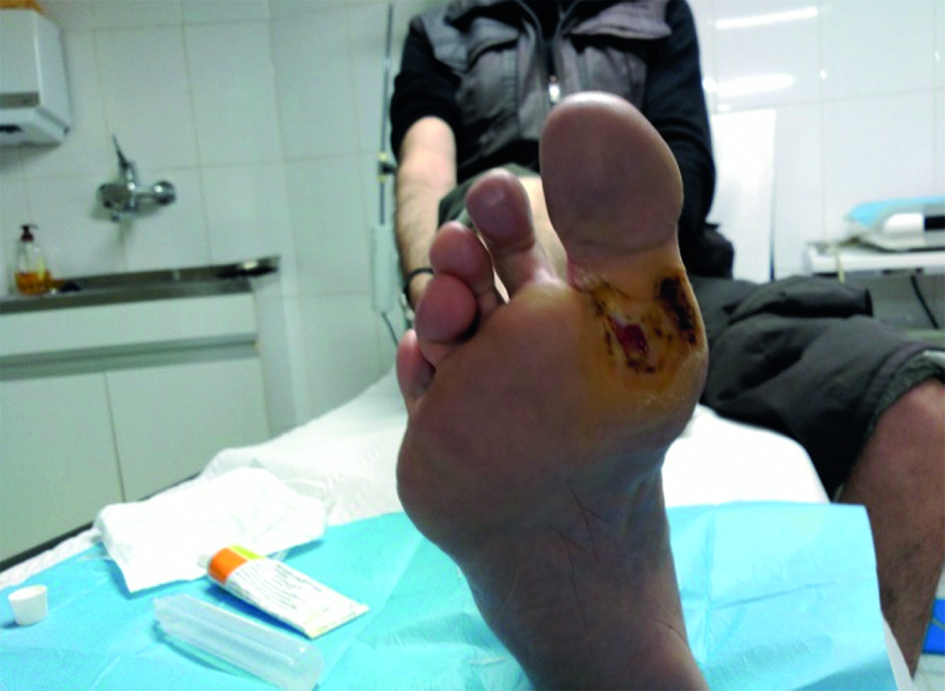
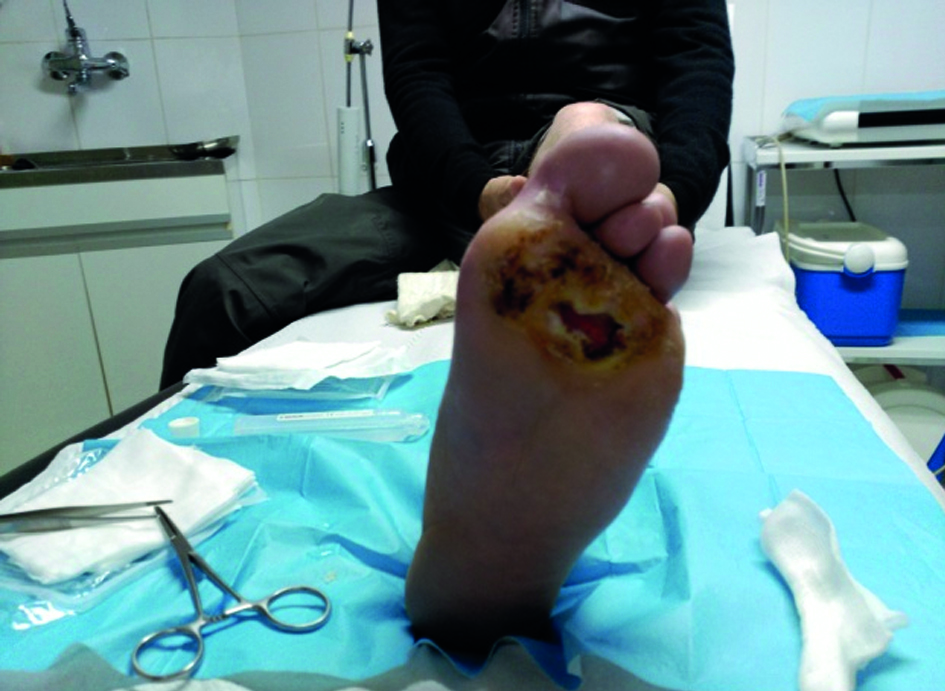
The patient presents sole ulcers on both feet: 2x3 cm wide on the right foot and 4x3 cm wide on his left foot, this being more severe (Figures 1 and 2). They present a large amount of hyperkeratosis, swollen borders with exudation and bad smell. The areas between the fingers are also moist, soft and also smell bad. Dorsal pedal and posterior tibial pulses in the right foot are very weak. Onychomycosis is present in all nails.
The patients reports cramps in both feet although more frequently in the left one, intermittent claudication of less than 150 meters and itching of the malleolar and anterior tibial regions, mostly in the left foot. He presents nighttime pain that subsides with the decline position. In the left leg he has an ocher pigmentation of the skin in the malleolar region with two areas of blisters with no further ulceration and no-pitting edema in the tibial region. He presents dermatitis in the base of the toes with no external signs of varicose veins. He has moderate Charcot arthropathy in his left foot. The patient is independent for activities of daily living (Figures 1 and 2).
- The probing to bone test is performed to determine the degree of communication between the surface of the ulcer and the joint, and it is negative.
- DopplerUS shows calcified laminar atherosclerotic plaques mainly in distal territories. He presents a biphasic flow due to impaired vascular elasticity, in the posterior retro-malleolar territories of the pedal and tibial arteries. This is compatible with moderate chronic arterial ischemia.
- The ankle-brachial index (ABI) is determined with a result of 1.2 in the right foot and 1.3 in the left one.
- Leriche-Fontaine classification: stage IV.
- Pain visual analogue scale (VAS): 6 of nighttime predominance, forcing him to wake up and move his legs.
- Blood pressure (BP): 102/63
- Weight: 75.900 kg
- Height: 1.76cm
- Body mass index (BMI): 24.
- Culture of wound: colonization by Staphilococcus aureus
Care plan
The care plan was established based on the etiological diagnosis. In this case the patient presents a neuropathic ulcer with a moderate ischemic component and venous insufficiency of the most affected limb which impairs treatment.
Therefore, this is a patient with a chronic ulcer of mixed neuropathic and ischemic origin and venous hypertension in his left leg. Neuro-ischemic ulcers are treated as ischemic until revascularization is achieved. The main basis of treatment is control of exudation since this favors infection and significantly increases the risk of amputation.
Venous hypertension should be treated with compression by means of a low-elasticity multilayer bandage with the necessary precautions in view of his chronic moderate arterial ischemia3. The care plan is developed according to the DOMINATE management system to encourage wound healing4.
The DOMINATE acronym wound care management system:
- Debridement: removal of nonviable tissue that impedes healing by means of mechanical and cleaning techniques.
- Offloading: it eliminates wound stress and trauma which interfere with healing with a 1.5cm thick pad and walking devices. Appropriate shoes with anterior offload should be used.
- Moisture, malignant, medications, mental health: control of chronic exudates by proper absorbent dressing (calcium alginate). Education of patients on the need of their cooperation for the care plan. Continuous supervision of instructions. Verification of medications that may interfere with wound healing. Control of stress and its effects on tissue inhibitors of metalloproteases (TIMPs).
- Infection, inflammation: control of infection, identification of infection signs, antimicrobial therapy such as polyhexanide-betaine solution (Prontosan®), cadexomer iodine (Iodosorb®). Wound culture and systemic antibiotics under medical prescription5.
- Nutrition: identification of malnutrition, correction of deficits and early referral no dieticians (endocrinology). Glycated hemoglobin levels should be kept under 7.
- Arterial insufficiency: weak pedal and posterior tibial pulses in the right foot and absent in the left foot. Non-significant ankle-brachial index in view of calcification shown on the US. Referral to specialist (vascular surgeon) to assess potential revascularization.
- Technical advances: moist control with daily cures and moist-free products.
- Edema: control of edema. The patient will exercise his lower limbs while avoiding weight bearing (cycling, strengthening lower limb muscles), low-elasticity multi-layer bandage in his left leg.
- Education: on his disease.
- Empowerment: He is notified that without his cooperation good results are difficult to achieve.
Discussion
Diabetic foot ulcers, which associate neuropathy, ischemia and venous hypertension need specialized care. An appropriate knowledge of the lesion etiopathology provides the key to understand the diagnosis and approach its treatment reducing the risks associated to delayed diagnosis or inappropriate treatments. The scientific evidence supports the use of compressive therapies as an efficient and safe alternative for ulcers of mixed origin. Compression significantly improves edema and reduced exudates3.
The selection of products for debridement was based on available evidence after performing a bibliographical search. Calcium alginate dressings control moist as well as cadexomer iodine which provides quick cleaning of the wound and nonviable tissue with a significant antimicrobial activity without excessive moist5.
Generally speaking, chronic wounds do not heal with dressings but epithelize when the cause is solved. According to some publications between 49 and 85% of all diabetic foot complications are evitable. This can be achieved by a combination of appropriate care, interdisciplinary strategies and specific health education for diabetic patients2.
Education for patients, caregivers and healthcare providers is an essential aspect of efficient treatment strategies. Therefore, we need efficient systems and structures ensuring appropriate evaluation and compliance by the patient by providing appropriate care. Patients’ involvement and that of their environment improve results.
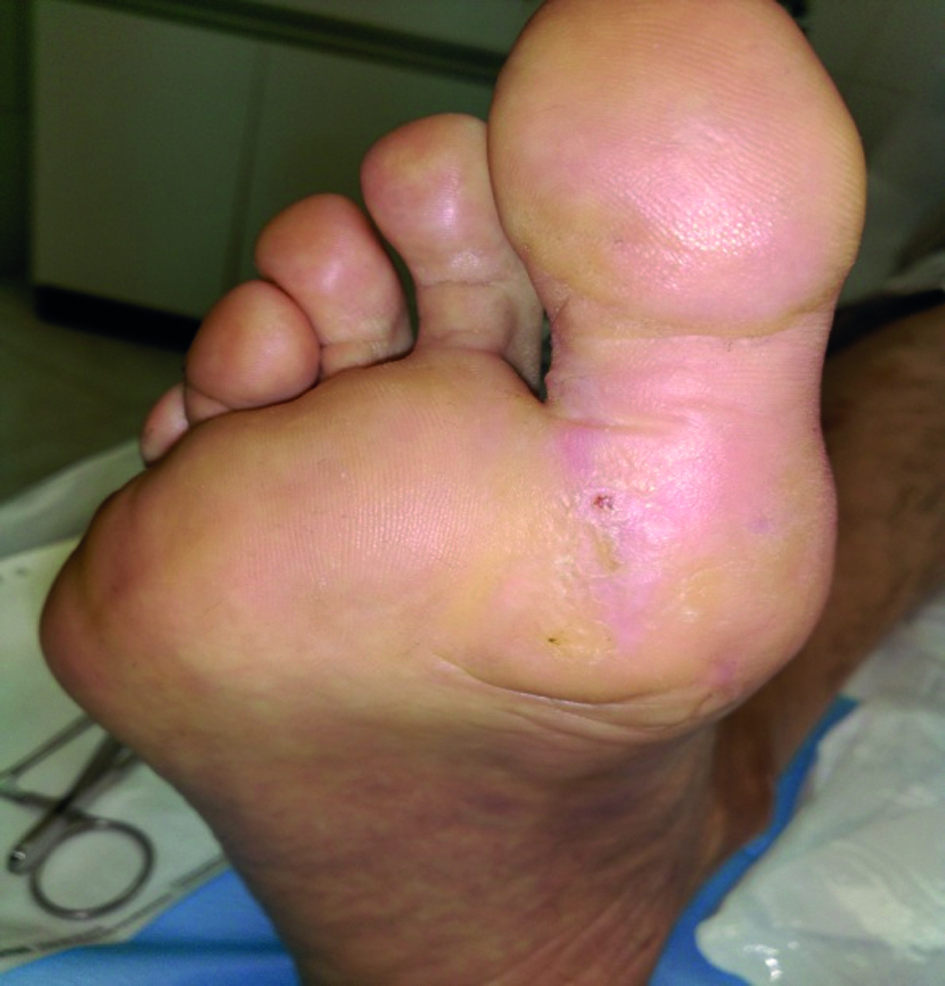
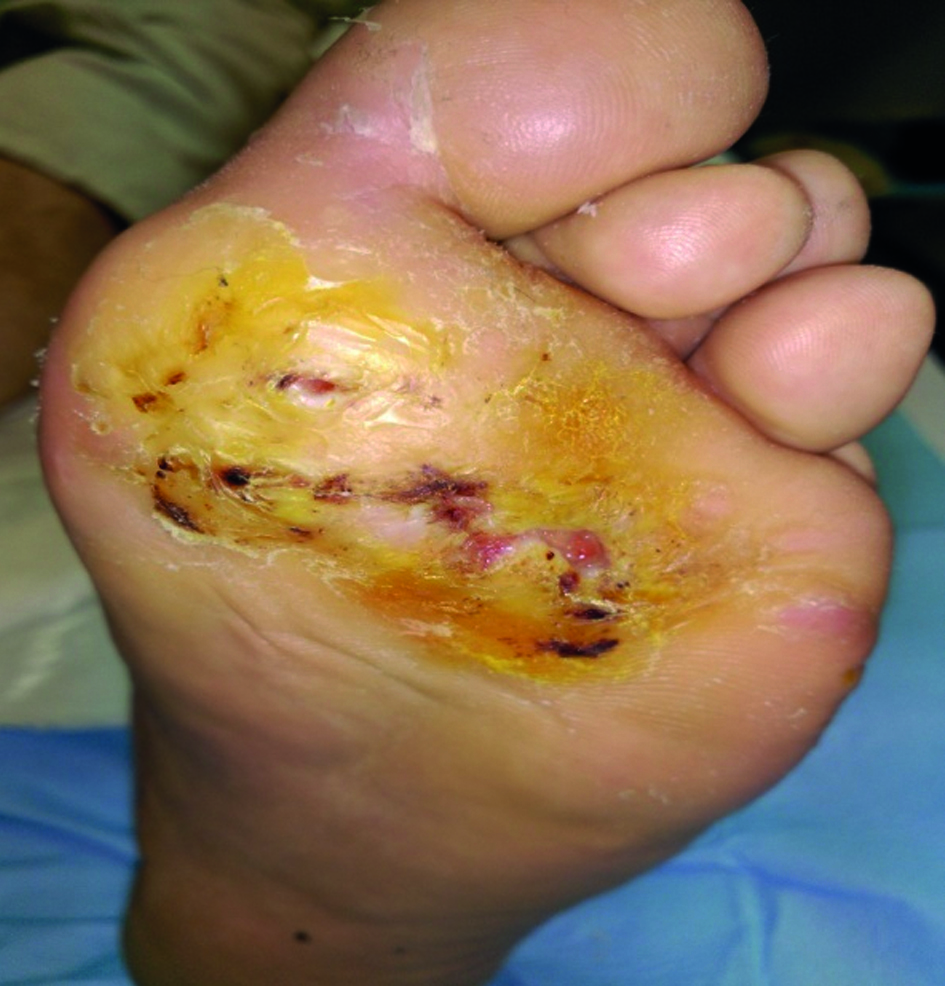
In this case, imprisonment lead to the reduction of complications and presumably to avoiding amputation, at least temporarily since he was able to focus on his disease. During the process the patient became aware of the importance of taking care of himself6 7. After one year of treatment the right foot has completely healed and the left one has gone through several stages although complete healing has not been achieved (Figures 3 and 4).