Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Medicina Oral, Patología Oral y Cirugía Bucal (Ed. impresa)
versión impresa ISSN 1698-4447
Med. oral patol. oral cir. bucal (Ed.impr.) vol.10 no.5 nov./dic. 2005
Intraoral tumor with rapid growing. Report of a case
Masa intraoral de rápido crecimiento. A propósito de un caso
Javier González Martín-Moro (1), Jose Luis Cebrián Carretero (2), Elena Gómez García (2),
Jose Luis del Castillo Pardo de Vera (1), Daniel del Val (3)
(1) Médico residente. Servicio de Cirugía Oral y Maxilofacial
(2) Médico adjunto. Servicio de Cirugía Oral y Maxilofacial
(3) Médico residente. Servicio de Anatomía Patológica. Hospital Universitario La Paz. Madrid. España
Address:
Secretaría de Cirugía Oral y Maxilofacial, 7ª planta del Hospital General.
Hospital Universitario La Paz. Paseo de la Castellana 261. 28046 Madrid
Teléfono: 679224393/616415881
E-mail: javigmoro@hotmail.com
jgonzalezma.hulp@madrid.salud.org
Received: 21-03-2004 Accepted:11-02-2005
|
González-Martín-Moro J, Cebrián-Carretero
JL,
Gómez-Gar-cía E, del Castillo-Pardo de Vera JL, del
Val D. Intraoral tumor with rapid growing. Report of a case. Med Oral
Patol Oral Cir Bucal 2005;10:440-3. |
|
ABSTRACT
The appearance of an intraoral mass is common in our speciality. Most are benign lesions, but some are primary malignancies. Metastases account for less than 1% of all oral malignances. Key words: Mandibular metastasis, intraoral mass, oral metastasis. |
RESUMEN La aparición de una masa intraoral supone un motivo de consulta frecuente en nuestra especialidad. La mayoría de los casos corresponden a lesiones benignas y, dentro de las malignas, a tumores primarios intraorales. Las metástasis suponen menos del 1 % de las lesiones malignas. Palabras clave: Metástasis mandibulares, masas intraorales, metástasis orales. |
INTRODUCTION
Among the great variety of intraoral pedunculated soft tissue masses, benign primary lessons such as pyogenic granuloma or fibroma the most frequent ones, and metastatic tumors account for approximately 1% of all oral malignant tumors (1). Definitive diagnosis requires histological study by biopsy or mass excision. Metastatic tumours in the jaw bone are more frequent than those in the oral mucosa (by a ratio of 2.5:1). There is no differences in incidence between men and women, although in men, the lung is the most frequent origin of soft tissue metastases while breast cancer in woman usually spreads to the jaw bone (3-5).
Once the primary tumor and its posible dissemination have been determined, it will be possible to plan an individualized treatment with curative or palliative aims.
CASE REPORT
A 86-year-old edentolous woman was referred to the Oral and Maxillofacial department of La Paz hospital, in Madrid, for the evaluation of a fast-growing intraoral lump. Her medical history included congenital deafness, high blood pressure, and lacunar ictus on the left CMA. Clinical examination revealed an asymptomatic, erythematous, 2x2 cm, pedunculated mass on the left lateral mandibular incisor gingiva. She did not refer sensitive alterations in the inferior alveolar nerve territory. There were no palpable lymph nodes or abnormal laboratory results.
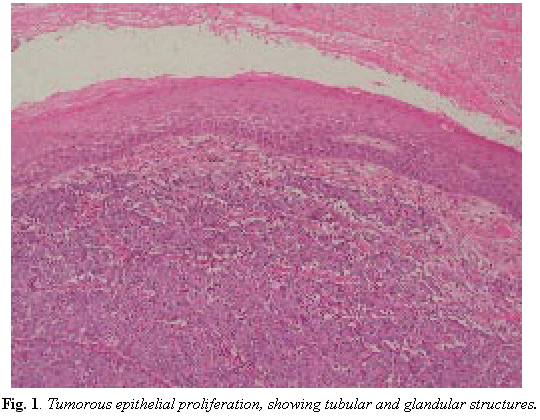
As inflammatory or reactive lesions were suspected, an excisional biopsy under local anaesthesia was performed without any complementary studies. The preliminary histopathological findings indicated a tumoral epithelial proliferation that was suggestive of adenocarcinoma (Fig. 1).
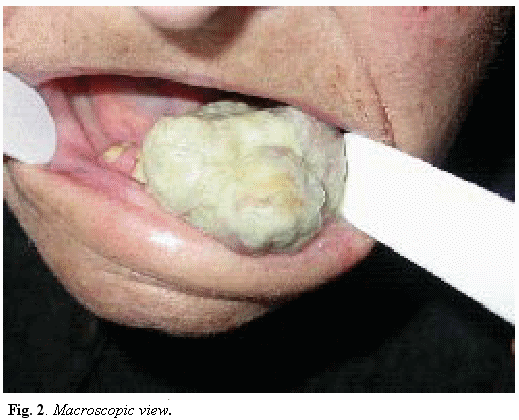
Several days later, the patient returned with an even bigger mass in the same location (3x3 cm.), which kept her from eating or even shutting her mouth (Fig. 2). This rapid growih can be easily understood since the inicial extirpation of what was thought to be a benign lesion had been incomplete.
The radiographic study (ortopantomography) showed a lytic lesion in the upper border of the anterior mandible, and the extension study (CT) showed a left adrenal 4x4x5.5 cm mass, as well as celiac trunk adenopathies.
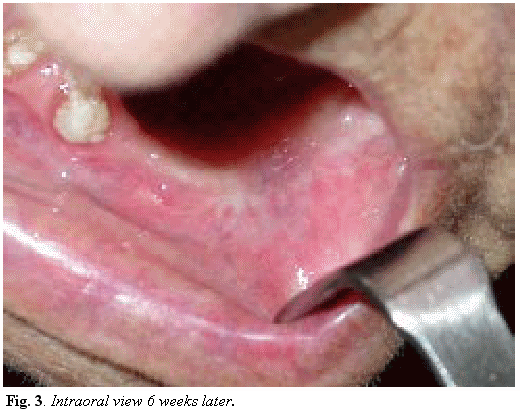
Considering the age of the patient, her basal status, the toxicity of radio and chemiotherapy , and the ominous prognosis for mandibular metastasis, the multidisciplinary team of the centre decided not to perform any invasive diagnostic tests, but to apply a palliative treatment consisting in excision of the mass and curettage of the bone. No recurrence has been referred to this moment (Fig. 3).
DISCUSSION
The differential diagnosis for a gingival soft-tissue mass should include developmental, reactive or inflammatory, and neoplastic entities. Although the definite diagnosis will be given exclusively by the biopsy, the clinical history, location of the mass, growing speed, clinical appearance, age and sex of the patient, as well as radiological findings, will guide us to one diagnosis or another.
Among the benign fast-growing pedunculated lesions, pyogenic granulomas, peripheral giant cell granulomas, fibromas, hemangiomas and epulis should be always considered since they are often clinically confused (2,6,7). On the other hand, the squamous cell carcinoma and Non-Hodgkin’s lymphoma are the most frequent malignant lesions in the oral cavity (8). Oral metastases are uncommon and account for less than 1% of all oral malignancies: metastatic tumors are more frequently reported in the jawbones than in the oral mucosa (ratio 2.5:1). The most common primary sources are lung, kidney and prostate in men and breast and genital organs in women (3-5,9). Although really extraordinary, thyroid and oesophagus carcinoma metastases have also been reported (10-11).
The primary tumor is usually diagnosed before the metastasis is discovered, and in less than 1 in 3 cases the metastasis is the first sign of the disease (1-3). In some of these cases, it is not possible to identify the primary source.
Oral metastasis generally carries a poor prognosis, as they indicate a widespread disease with metastatic deposits in many other organs and tissues; the expected survival does not exceed several months (7).
As we see in Fig.1 the histological study showed a tumorous epithelial proliferation growing in solid nests, under and unrelated to the polystratified epithelium of the oral mucosa. A magnified view showed tubular and glandular structures with necrotic centres. Inmunohistochemical techniques did not identify a known cytokeratin pattern. As metastatic abdominal adenocarcinoma was suspected, a body TC was performed and discovered a left suprarenal 4x4x5.5 cm mass, as well as celiac trunk lymph nodes and other small adenopathies near the iliac vessels, compatible with metastatic spread.
As the patient suffered no abdominal complaints, no invasive diagnostic procedures were performed because of her age and basal status, the differential diagnosis of the primary source is wide and includes gastro-intestinal locations as well as genito-urinary tumors. Among the firsts, a colorectal adenocarcinoma is the most common, producing intestinal rythm alteration, weight loss and microcytic anemia. The definite diagnosis is endoscopic, being the CT not sufficient. Hepatic and follicular thyroid carcinoma are associated with massive bleeding during biopsy. Pancreatic tumours reach a large size before producing symptoms, being the metastasis the first sign of the disease (11-13). If a genito-urinary tumor is suspected, the first to be considered should be the renal cell carcinoma, associated with abdominal mass, pain and haematuria (15).
Curative treatment is only possible if the extension study reports a single metastases and the tumor is resectable, but this is quite rare (3). Much more frequently, the metastases reflects a widespread disease, with an expected survival of a few months, so the aim of the treatment becomes improving the quality of life rather than increasing the survival (4-7).
REFERENCES
1. Fukuda M, Miyata M, Okabe K, Sakashita H. A case of 9 tumors metastatic to the oral and maxillofacial region. J Oral Maxillofac Surg 2002; 60: 942-4. [ Links ]
2. Monson ML, Postgate J, Bowe R, Williams TP. Pedunculated soft tissue mass on the alveolar gingiva. J Oral Maxillofac Surg 1990; 48: 1311-6. [ Links ]
3. Schwartz ML, Baredes S, Mignogna FV. Metastatic disease to the mandible. Laryngoscope 1988; 98: 270-3. [ Links ]
4. Yoshii T, Muraoka S, Sano N, Furudoi S, Komori T. Large cell carcinoma of the lung metastatic to the mandibular gingiva. J Periodontol 2002; 73: 571-4. [ Links ]
5. Rodado C, González J, Huguet P, Ávila M, Raspall G. Lung adenocarcinoma presenting as an oral metastasis. Med Oral 1997; 2: 315-20. [ Links ]
6. Schenberg ME, Slootweg PJ, Koole R. Leiomyosarcomas of the oral cavity. Report of four cases and review of the literature. J Oral Craniomaxillofac Surg 1993; 21: 342-7. [ Links ]
7. Ellis GL, Jenses JL, Reingold IM, Barr RJ. Malignant neoplasm metastatic to gingivae. Oral Surg Oral Med Oral Pathol 1977; 44: 238-45. [ Links ]
8. Soderholm AL, Lindqvist C, Heikinheimo K, Forssell K, Happonen RP. Non-Hodgkins lymphomas presenting through oral symptoms. Int J Oral Maxillofac Surg 1990; 19: 131-4. [ Links ]
9. Sanchez Aniceto G, Garcia Penin A, de la Mata Pages R, Montalvo Moreno JJ. Tumors metastatic to the mandible: análisis of nine cases and review of the literature. J Oral Maxillofac Surg 1990; 48: 246-51. [ Links ]
10. Jimenez Y. Oral metastasis in esophagus cancer. Med Oral 2004; 9: 182. [ Links ]
11. Ostrosky A, Mareso EA, Klurfan FJ, González MJ. Mandibular metastasis of follicular thryoid carcinoma. Case report. Med Oral 2003; 8: 224-7. [ Links ]
12. Doval DC, Kannan V, Kumaraswamy SV, Reddy BK, Bapsy PP, Rao CR. Mandibular metastasis in hepatocellular carcinoma. Int J Oral Maxillofac Surg 1992; 21: 97-8. [ Links ]
13. Marker P, Clausen PP. Metastases to the mouth and jaws from hepatocellular carcinomas. A case report. Int J Oral Maxillofac Surg 1991; 20: 371-4. [ Links ]
14. Vahatalo K, Ekfors T, Syrjanen S. Adenocarcinoma of the pancreas metastatic to the mandible. J Oral Maxillofac Surg 2000; 58: 110-4. [ Links ]
15. Yoskovitz A, Nguyen LH, Sadegui N, Auger M. Renal cell carcinoma presenting as a mandibular mass. Otolaryngol Head Neck Surg 2001; 125: 654-5. [ Links ]











 texto en
texto en