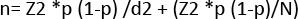INTRODUCTION
Non-communicable diseases (NCD) are now the leading cause of death worldwide. Sixty three percent (63%) of all annual deaths (which translates into over 36million deaths) are attributed to NCDs. About 80% of NCD deaths occur in low and middle income countries. Globally, cardiovascular diseases account for about 17 million deaths a year, nearly a third of the total deaths. Cardiovascular diseases have been identified to account for about a third of all deaths in middle income countries.1 Complications from hypertension also accounts for 9.4 million deaths worldwide annually.2
Medicines are vital in achieving optimal health outcomes in a wide range of medical conditions.3However, irrational use of medicines may lead to adverse events or result in the waste of scare re-sources impacting negatively on an individual health status.
Patient outcomes are likely to improve if this information is understood and used effectively.4Although there has been an increased global attention to medicines, there are still problems associated with access to essential medicines especially in the management of chronic diseases in Low Medium Income Countries.4Inequities in the access to health care delivery lead to poorer individuals having difficulty in accessing healthcare as compared to the richer individuals.5 To ensure an effective health system for any community, the healthcare seeking behaviour of the inhabitants should be considered in the development of healthcare policies and the design of programmes. 6Achieving and sustaining health involves a multifaceted interaction between the individual’s health needs, the social linkage in which the individual is entrenched, and the health systems available to meet these health needs. 7
Health services in Ghana have been decentralized as part of health sector reform, services are therefore integrated as one goes down the hierarchy of the health structure from the national to the sub-district level. Curative and public health services are provided at the regional and district hospitals mostly mission or faith-based facilities. Most district hospitals with a bed capacity of 60-80 serve an average population of 100,000 - 200,000 inhabitants in a defined geographical area. At the sub-district level, both preventive and curative services are delivered by the health centres. Outreach programmes to the communities within sub districts are usually supervised by the District Health Management Team (DHMT) but offered by the health centres. Community-based Health Planning and Services (CHPS) have been introduced to manage minor ailments at the community and household level. Most district capitals have a district hospital that provides health care to inhabitants in the capital and adjoining towns. The private sector plays a very important role in the healthcare delivery system.
In most districts private hospitals, pharmaceutical shops and over the counter medical sellers play a significant role in meeting the medical needs of inhabitants. It is reported that services sought over the counter are on the rise.8 Private health facilities on the other hand are increasingly being accepted by inhabitants in sub-Saharan Africa. Although the private health centres have its own challenges such as an observation made in a study by Triptiet al. (2014) which reported prescription errors in about half of total drugs requests submitted.9In Ghana, there is dearth of in-formation regarding source in public or private health facilities. Asigbie et al. (2016) raised concerns on equity and quality of pharmaceutical products offered in the various health centres in-country. 10
This study focuses on sources of medicine and medicine information by persons with hypertension and diabetes in both rural and urban communities in Ghana. The study further assesses predisposing and enabling factors (as defined by Andersen’s behavioural model of health service utilization) that influence participants’ source of medicine and medicine information. Understanding the health seeking behaviour particularly on medicinal access by chronic patients, who are known to be increased medicine users11 , 12will offer useful policy guidelines on managing pharmaceutical supplies and information for efficient use.
METHODS
Study design
A population based cross-sectional study design was employed to determine the disease burden of persons, living in rural and urban districts of the Ashanti Region of Ghana. The study was carried out from January 2016 to March, 2016.
The study was conducted in four (4) rural and four (4) urban districts in the Ashanti Region of Ghana. Ashanti region is one of the 10 regions in Ghana with a population of 4,780,208 representing 19.4% of the country’s population. It is therefore the highest populated region with a growth rate of 2.7% and an urban: rural population ratio of 1.5:1 and is located in the central belt of the country.
Study population
The study included persons at least 18 years of age, who have resided in the study area for not less than 2 years and consented to be part of the study.
A multi-stage sampling technique was used in selecting a representative sample from both the rural and urban population (1885-642X-pharmpract-16-03-1151-suppl.pdfonline Appendix). The rural districts were defined as districts that had more that 50% of their in-habitants in rural communities as indicated by the 2010 population census report. Out of the 30 districts in the region 17 and 13 were categorized as rural and urban out of which 4 districts were randomly chosen. Five of the communities among the 20 largest communities as provided by the 2010 population and housing census report were randomly sampled. The number of prospective participants from each community was determined by calculating proportionally based on the 2010 population census report for each district. Every community was then divided into 4 clusters, and equal numbers of participants were recruited from each cluster.
The sample size for the survey was calculated to obtain a representative sample to estimate the population prevalence of NCD with a good precision. The sample size was therefore calculated using the formula as illustrated below:-
Where n = sample size
Z = statistic for a level of confidence-(CI 95%-1.96),
p= a rough approximation to the proportion (0.5)
d = allowable sampling error tolerated or accuracy of measurement (2.5%)
N=Total population of the selected districts
Total Population Size = 2,465,180.
The minimum number of inhabitants required was one thousand five hundred and thirty seven (1537) however, to make up for incomplete responses by some of the study participants, an upward adjustment of 10% was done. One thousand seven hundred (1700) participants were therefore proposed as the sample size to be enrolled. Furthermore, to allow for the comparison of urban and rural populations, proportionate sampling of the urban and rural population was done based on a ratio of 3:2, 1000 inhabitants were therefore proposed to be recruited from the urban population and 700 inhabitants to be recruited from rural populations.
Ethics approval
Approval was sought and obtained from the Committee on Human Research Publications and Ethics (CHRPE), of the School of Medical Sciences, Kwame Nkrumah University of Science and Technology (Approval number: CHRPE/AP/503/17). Participants were given comprehensive information on the purpose of the study, and the potential risks and benefits of the study by the trained data collectors. Voluntariness to participate in the study was stressed in the process. Participants who agreed to participate were then made to sign whiles illiterate participants were made to thumbprint the informed consent document to affirm their willingness to participate in the study.
Data collection
A structured questionnaire was designed based on the research objectives. The UNDP Global Multi-dimensional poverty index questionnaire served as a guide in developing the measure of income and socioeconomic status. Sixteen data collectors were recruited, two data collectors were assigned to each rural and urban district. Data collectors were invited for a one-day training programme to ensure standardization of the questionnaire. The sixteen trained data collectors pre-tested the questionnaire to ensure reliability and validity in non-selected communities. Data was then collected electronically after informed consent had been obtained from opinion leaders and from prospective participants in the selected communities. The questionnaire was used to solicit information on self- reported NCD status (defined as either having hypertension or diabetes or both), demographic characteristics of participants and source of medicines and medicine information (e.g. dosage and side effects) for managing NCD. Predisposing and enabling factors that influence the source of medicines and medicine information were also obtained.
Data Analysis
The data were exported to Stata version 13.0 (StataCorp. 4905 Lakeway Drive Station, Texas 77845, USA) for statistical analysis. Basic summary statistics of socio-demographic variables were conducted. Respondents self-reported their NCDs status. Wealth index was constructed for income and socio-economic status of the study respondents. The index was constructed from household asset data using principal components analysis.13Income status index was built from three main income variables: Number of people who earn an income in the household, average monthly income of the household and an additional money support to the household. The income status index was categorized as low and high based on scree plot of eigenvalues after principal component analysis. Access to basic utilities, sources of drinking water, and water treatment practices; access to sanitation facilities, housing structure; crowdedness of dwelling spaces; and type of fuel used for cooking are physical characteristics of a household that are used to assess the general well-being and socioeconomic status of house-hold members.13Socio-economic status index for this study was constructed from thirteen variables using principal component analysis: earned an income, average monthly income, received additional support, completed senior secondary school, under-five children death, number of school going of under-five children, number of rooms, type of materials used to make the wall of the house, house wired, have toilet facility, type of toilet facility, type of fuel and number of meals served in a day in household The socio-economic status index was categorized as low, medium and high and highest based on scree plot of eigenvalues after principal component analysis. Chi-square test of association or Fisher’s Exact where appropriate was used to compare categorical variables and Health Seeking Behaviour (HSB). Finally, Multinomial logistic regression model was used to establish an association between HSB and predisposing, and enabling factors as proposed by Andersen’s behavioural model of Health Services. Multinomial logistic regression model is suitable for comparing more than two possible outcomes; it picks a base category and calculates the odds (Relative Odds, OR) of the other possible outcomes relative to it.
RESULTS
Demographic characteristics
A total of 1703 participants were enrolled, 1019 from the urban population and 684 from the rural population. The findings revealed 336 participants self -reported they had NCD (Diabetes and Hypertension) made up of 137 in the rural communities and 199 in the urban communities. The find-ings of this study showed that the highest percentage of participants living in the rural communities with NCD were above 65 years. The median age in the rural population was 58 (IQR: 51-67). While in the urban population the highest percentage of participants living with NCD were between the ages 46-55 years. The median age of the urban population was 54 (IQR: 45- 63) (Table 1). Participants living in both the rural and urban communities were predominantly Christians and married (Table 1). The majority of participants with NCD living in the rural 77 (56.20%) communities were females while majority in the urban 106 (53. 27%) communities were males. About half of the participants with NCD in the rural communities 69 (50.29%) had attained basic education, while 47 (34.31%) had no formal education. In the urban communities, 89 (44.72%) had secondary education, while 27 (13.57%) had no formal education.
Table 1. Demographic characteristics of persons with NCD (diabetes and hypertension)
| Variable | Rural, N=137 | Urban, N=199 | ||
|---|---|---|---|---|
| Frequency | Percentage (%) | Frequency | Percentage (%) | |
| Sex | ||||
| Male | 60 | 43.80 | 106 | 53.27 |
| Female | 77 | 56.20 | 93 | 46.73 |
| Age (years) | Median(IQR)=58.00(51.00-67.00) | Median(IQR)=54.00(45.00-63.00) | ||
| <=25 years | 4 | 2.92 | 3 | 1.51 |
| 26-35 years | 3 | 2.19 | 11 | 5.53 |
| 36-45 years | 15 | 10.95 | 39 | 19.60 |
| 46-55 years | 38 | 27.74 | 55 | 27.64 |
| 56-65 years | 37 | 27.01 | 54 | 27.14 |
| >65 years | 40 | 29.2 | 37 | 18.59 |
| Marital Status | ||||
| Single | 4 | 2.92 | 19 | 9.55 |
| Married | 82 | 59.85 | 135 | 67.84 |
| Co-habiting | 0 | 0.00 | 0 | 0.00 |
| Separated | 3 | 2.19 | 2 | 1.01 |
| Divorced | 11 | 8.03 | 5 | 2.51 |
| Widowed | 37 | 27.01 | 38 | 19.10 |
| Religion | ||||
| Christian | 104 | 75.91 | 174 | 87.44 |
| Moslem | 26 | 18.98 | 22 | 11.06 |
| Traditionalist | 1 | 0.73 | 1 | 0.50 |
| Other | 6 | 4.38 | 2 | 1.01 |
| Educational Level | ||||
| None | 47 | 34.31 | 27 | 13.57 |
| Basic Level | 69 | 50.36 | 48 | 24.12 |
| Secondary Level | 17 | 12.41 | 89 | 44.72 |
| Tertiary Level | 4 | 2.92 | 35 | 17.59 |
| Income status | ||||
| Low | 82 | 59.85 | 87 | 43.72 |
| High | 55 | 40.15 | 112 | 56.28 |
| Socioeconomic status | ||||
| Low | 54 | 39.42 | 14 | 7.04 |
| Medium | 26 | 18.98 | 34 | 17.09 |
| High | 20 | 14.60 | 25 | 12.56 |
| Highest | 37 | 27.01 | 126 | 63.32 |
| Enrolled on the National Health Insurance Scheme | ||||
| Yes | 119 | 88.15 | 190 | 95.96 |
| None | 16 | 11.85 | 8 | 4.04 |
IQR: Interquartile Range
Table 2. Study participants NCD status
| NCD Status | Rural | Urban | ||
|---|---|---|---|---|
| Number (N=137) | Percentage (%) | Number (N=199) | Percentage (%) | |
| Diabetes Only | 26 | 18.98 | 28 | 14.07 |
| Hypertension and Diabetes | 11 | 8.03 | 24 | 12.06 |
| Hypertension only | 100 | 72.99 | 171 | 73.87 |
In the rural communities 82 (59.85%) of the participants were in the low income bracket, while 112 (56.28%) of the participants in the urban communities were found in the high income bracket (Table 1). About 88% of participants with NCD (88.15%, 119/137) in the rural and 95.96% (190/199) in the urban communities had registered with the National Health Insurance Scheme (NHIS) (Table 1 ).
Source of Medicine
The findings indicated that participants with NCD in the rural communities sourced medicines mainly from the health centre 49 (35.77%) followed by sourcing from the hospital in the urban areas 45 (32.85%). In the urban communities, the majority of participants 153 (76.88%) sourced medicines from the hospital while 33 (16.58%) indicated the pharmacy was their source of medicines. In the urban communities the family member was least utilized as a source of medicine (Table 3).
A Fisher exact test of independence on the above trend observed in Table 3indicates that there is a statistically significant difference among participants with NCD, place of residence and source of medicine (p-value<0.001) (Table 4)
Table 3. Chi Square Test on Place of Residence of Participants (NCD) and Sources of Medicines
| Source of medicines | Rural, n(%), N=137 | Urban, n(%), N=199 | P value |
|---|---|---|---|
| OTCMS | 35(25.55%) | 9(4.52%) | <0.001* |
| Family member | 0(0.00%) | 1(0.50%) | |
| Health Centre | 49(35.77%) | 3(1.51%) | |
| Hospital | 45(32.85%) | 153(76.88%) | |
| Pharmacy | 4(2.92%) | 33(16.58%) | |
| Others | 4(2.92%) | 0(0.00%) |
OTCMS- Over the Counter Medicine Shop.
*Fischer Exact Test.
Table 4. Sources from which participants with NCD sought Medicine Information
| Source of Medicine Information | Rural, n(%) N=137 | Urban, n(%) N=199 | p value |
|---|---|---|---|
| Family Member | 11(8.03%) | 3(1.51%) | <0.001* |
| Friend Health Professional | 19(13.87%) | 7(3.52%) | |
| Pharmacy | 1(0.73%) | 24(12.06%) | |
| Nearest Health Institution | 99(72.26%) | 164(82.41%) | |
| OTCMS | 6(4.38%) | 0(0.00%) | |
| Others | 1(0.73%) | 1(0.50%) |
Nearest Health Institutions: Public Hospital, Health Centre.
*Fischer Exact Test for Trend.
Source of Medicine Information
The majority of participants with NCD in the rural 99 (72.26%) and the urban 164 (82.41%) communities sourced medicine information from the nearest health institution. In the rural communities, other sources of medicine information were from health professional friends 19 (13.87%) while in the urban communities it was from the pharmacy. A Fisher exact test of independence indicated an association between participant’s place of residence and source of medicine information (p-value<0.001) (Table 4).
A test for association using the multinomial logistic regression model revealed that there was no relationship between participants with NCD and their health seeking behaviour in the rural communities with respect to source of medicine. In the urban communities, participants with NCD with increasing age were 10% (OR 1.1, 95%CI 1.040 -1.210 p =0.003), more likely to source medicines from Over the Counter Medicine Shop (OTCMS) and 1.0 times (OR 1.0, 95%CI 1.002 -1.066 p=0.040), likely to source medicine from the hospital than the pharmacy (Table 5 ). The results also indicated that participants with low socioeconomic status were 0.3 times more likely to source medicines from the hospital than from the pharmacy (OR 0.3, 95%CI 0.085 -0.855 p=0.026) (Table 6 ).
Table 5. Multinomial Logistics Regression test of Predisposing factors and Source of Medicine in the urban and rural communities of the Ashanti Region
| Source of Medicine | Urban | Rural | ||||||
|---|---|---|---|---|---|---|---|---|
| OR | p value | [95% CI] | OR | p value | [95% CI] | |||
| Pharmacy (base outcome) | ||||||||
| OTCMS | ||||||||
| Age | 1.1 | 0.003 | 1.040 | 1.210 | 0.9 | 0.266 | 0.866 | 1.040 |
| Sex (male=ref) | ||||||||
| Female | 1.1 | 0.950 | 0.188 | 5.947 | 0.6 | 0.664 | 0.040 | 7.729 |
| Marital Status (not married = ref) | ||||||||
| Married | 2.0 | 0.459 | 0.326 | 11.995 | 3.0 | 0.411 | 0.216 | 42.406 |
| Educational Level (none = ref) | ||||||||
| Educated | 2.1 | 0.574 | 0.160 | 27.385 | 2.0 | 0.551 | 0.203 | 19.781 |
| Occupation (Unemployed = ref) | ||||||||
| Employed | 4.3 | 0.290 | 0.286 | 65.739 | 1.0 | 0.985 | 0.041 | 23.084 |
| Health Centre | ||||||||
| Age | 1.0 | 0.626 | 0.879 | 1.081 | 1.0 | 0.438 | 0.882 | 1.056 |
| Sex (male = ref) | ||||||||
| Female | 1.7 | 0.682 | 0.125 | 24.002 | 0.6 | 0.715 | 0.046 | 8.263 |
| Marital Status (not married = ref) | ||||||||
| Married | 2.4 | 0.559 | 0.133 | 41.915 | 2.8 | 0.441 | 0.208 | 36.833 |
| Educational Level (none = ref) | ||||||||
| Educated | - | - | - | - | 0.8 | 0.835 | 0.087 | 7.179 |
| Occupation (Unemployed = ref) | ||||||||
| Employed | 0.3 | 0.394 | 0.016 | 5.090 | 1.0 | 0.980 | 0.053 | 17.676 |
| Hospital | ||||||||
| Age | 1.0 | 0.040 | 1.002 | 1.066 | 1.0 | 0.456 | 0.883 | 1.057 |
| Sex (male = ref) | ||||||||
| Female | 1.0 | 0.988 | 0.447 | 2.264 | 1.2 | 0.905 | 0.087 | 15.822 |
| Marital Status (not married = ref) | ||||||||
| Married | 2.1 | 0.088 | 0.896 | 4.886 | 1.8 | 0.648 | 0.136 | 24.757 |
| Educational Level (none = ref) | ||||||||
| Educated | 1.0 | 0.964 | 0.323 | 3.264 | 2.0 | 0.538 | 0.217 | 18.700 |
| Occupation (Unemployed = ref) | ||||||||
| Employed | 0.9 | 0.836 | 0.305 | 2.612 | 3.2 | 0.462 | 0.144 | 71.414 |
OR: Relative Odds ratio. CI: Confidence interval. ref: Reference point. p < 0.05 was considered statistical significant.
Table 6. Multinomial logistics regression test of enabling factors and source of medicines in the urban and rural Communities of the Ashanti region
| Source of Medicine | Urban | Rural | ||||||
|---|---|---|---|---|---|---|---|---|
| OR | p value | [95% CI] | OR | p value | [95% CI] | |||
| Pharmacy (base outcome) | ||||||||
| OTCMS | ||||||||
| Income Status (low = ref) | ||||||||
| High | 4.5 | 0.091 | 0.786 | 25.901 | 5.0 | 0.189 | 0.453 | 54.637 |
| Socio-economic status (high = ref) | ||||||||
| Low | - | - | - | - | - | - | - | - |
| NHIS (no = ref) | ||||||||
| Yes | 0.2 | 0.250 | 0.009 | 3.447 | - | - | - | - |
| Health Centre | ||||||||
| Income Status (low = ref) | ||||||||
| High | - | - | - | - | 1.2 | 0.863 | 0.108 | 14.183 |
| Socio-economic status (high = ref) | ||||||||
| Low | - | - | - | - | - | - | - | - |
| NHIS (no = ref) | ||||||||
| Yes | - | - | - | - | - | - | - | - |
| Hospital | ||||||||
| Income Status (low = ref) | ||||||||
| High | 1.7 | 0.196 | 0.768 | 3.633 | 9.1 | 0.069 | 0.843 | 97.918 |
| Socio-economic status (high = ref) | ||||||||
| Low | 0.3 | 0.026 | 0.085 | 0.855 | - | - | - | - |
| NHIS (no = ref) | ||||||||
| Yes | 0.7 | 0.718 | 0.075 | 5.939 | - | - | - | - |
OR: Relative Odds ratio. CI: Confidence interval. ref: Reference point. p < 0.05 was considered statistical significant.
Table 7. Summary of Multinomial Logistics Regression test of Predisposing factors and Source of Medicine information in the rural communities of Ashanti
| Source of Medicine Information | Urban | Rural | ||||||
|---|---|---|---|---|---|---|---|---|
| OR | p value | [95% CI] | OR | p value | [95% CI] | |||
| Pharmacy (base outcome) | ||||||||
| Family Member | ||||||||
| Age | 1.1 | 0.011 | 1.032 | 1.270 | 1.0 | 0.517 | 0.941 | 1.129 |
| Marital Status (Not married = ref) | ||||||||
| Married | 0.9 | 0.922 | 0.040 | 18.253 | 2.3 | 0.484 | 0.228 | 22.544 |
| Educational Level (none = ref) | ||||||||
| Educated | - | - | - | - | 10.2 | 0.142 | 0.462 | 223.926 |
| Occupation (Unemployed = ref) | ||||||||
| Employed | 2.1 | 0.661 | 0.074 | 60.987 | - | - | - | - |
| Friend Health Professional | ||||||||
| Age | 1.1 | 0.009 | 1.022 | 1.167 | 1.1 | 0.171 | 0.973 | 1.167 |
| Sex (male = ref) | ||||||||
| Female | - | - | - | - | - | - | - | - |
| Marital Status (Not married = ref) | ||||||||
| Married | 0.04 | 0.009 | 0.003 | 0.441 | 10.6 | 0.046 | 1.044 | 106.835 |
| Educational Level (none = ref) | ||||||||
| Educated | - | - | - | - | 26.1 | 0.034 | 1.271 | 537.279 |
| Occupation (Unemployed = ref) | ||||||||
| Employed | 0.7 | 0.732 | 0.088 | 5.533 | 0.8 | 0.868 | 0.038 | 15.787 |
| Nearest Health Institution | ||||||||
| Age | 1.1 | <0.001 | 1.050 | 1.147 | 1.1 | 0.044 | 1.002 | 1.187 |
| Marital Status (Not married = ref) | ||||||||
| Married | 0.7 | 0.474 | 0.208 | 2.074 | 6.0 | 0.090 | 0.756 | 48.331 |
| Educational Level | ||||||||
| Educated | 3.6 | 0.058 | 0.956 | 13.219 | 30.6 | 0.020 | 1.718 | 546.668 |
| Occupation (Unemployed = ref) | ||||||||
| Employed | 1.4 | 0.649 | 0.360 | 5.155 | 2.2 | 0.560 | 0.158 | 30.327 |
OR: Relative Odds ratio. CI: Confidence interval. ref: Reference point. p < 0.05 was considered statistical significant.
Furthermore, the relative odds for married and educated participants with NCD in the rural communities were 10.6 times (OR 10.6, 95%CI 1.044 -106.835, p=0.046), and 26.1 times (OR 26.1, 95%CI 1.271 - 537.279, p=0.034) more likely to seek information on medication from a friend Health Professional than from the pharmacy respectively.
With increasing age, participants were 1.1 times (OR 1.1, 95%CI 1.002 - 1.187, p=0.044), more likely to seek information on medication from the nearest health institution, than from a pharmacy. Again, participants with NCD in the rural communities who were educated were 30.6 times (OR 30.6, 95%CI 1.718 - 546.668, p=0.020), more likely to obtain information on their medication from the nearest health institution than from the pharmacy. Also, low socio-economic status of participants with NCD in the rural communities were 60% (OR 6.6, 95%CI 1.016 - 43.510), likely to seek information on medication from the nearest health institution than from the pharmacy (Table 8).
Table 8 Multinomial logistics regression test of enabling factors and source of information medicines in the rural communities of the Ashanti region
| Source of Medicine | Urban | Rural | ||||||
|---|---|---|---|---|---|---|---|---|
| OR | p value | [95% CI] | OR | p value | [95% CI] | |||
| Pharmacy (base outcome) | ||||||||
| Family Member | ||||||||
| Income Status (Low = ref) | ||||||||
| High | 0.5 | 0.603 | 0.040 | 6.469 | - | - | - | - |
| Socio-economic status (High = ref) | ||||||||
| Low | - | - | - | - | 2.4 | 0.411 | 0.294 | 20.078 |
| NHIS (no = ref) | ||||||||
| Yes | - | - | - | - | 1.9 | 0.612 | 0.152 | 24.636 |
| Friend Health Professional | ||||||||
| Income Status (Low = ref) | ||||||||
| High | 0.9 | 0.856 | 0.153 | 4.765 | - | - | - | - |
| Socio-economic status (High = ref) | ||||||||
| Low | 0.7 | 0.814 | 0.066 | 8.431 | 0.4 | 0.386 | 0.044 | 3.348 |
| NHIS (no = ref) | ||||||||
| Yes | - | - | - | - | 1.6 | 0.704 | 0.133 | 19.752 |
| Nearest Health Institution | ||||||||
| Income Status (Low = ref) | ||||||||
| High | 1.6 | 0.301 | 0.659 | 3.852 | - | - | - | - |
| Socio-economic status (High = ref) | ||||||||
| Low | 0.3 | 0.052 | 0.072 | 1.010 | 6.6 | 0.048 | 1.016 | 43.510 |
| NHIS (no = ref) | ||||||||
| Yes | - | - | - | - | 0.3 | 0.285 | 0.021 | 3.096 |
OR: Relative Odds ratio. CI: Confidence interval. ref: Reference point. p < 0.05 was considered statistical significant.
In the urban communities, increasing age of participants with NCD were 1.1 times (OR 1.1, 95% CI 1.032 - 1.270, p=0.011), likely to seek information on medication from a family member rather than from the pharmacy.
The results also revealed that with increasing age and been educated were 1.1 times (OR 1.1, 95%CI 1.022 - 1.167, p=0.009) and 0.04 times (OR 0.04, 95%CI 0.003 - 0.441) likely to source medicine in-formation respectively from a friend health professional than the pharmacy.
In the urban communities, participants with NCD, with increasing age were 10% (OR 1.1, 95% CI 1.050-1.147), more likely to source medicine information from the nearest health institution than from the pharmacy.
DISCUSSION
Source of medicines
The Ghana health system operates at different levels: from the CHPS compounds being the lowest, to health centres, polyclinics, district and private hospitals, regional and tertiary hospitals being the highest. The services that are provided differ at each level and becomes more sophisticated as the level rises. Although the gate-keeper referral system is proposed by the MOH in collaboration with NHIS in a number of circumstances self- referral takes place because some of the facilities are not well re-sourced. The results revealed that most participants with hypertension and diabetes in the rural communities sourced medicines from the health centre while in the urban communities, the participants’ source of medicines was from the hospital. This compares with a study conducted in Brazil where medications were mainly obtained with a medical prescription at the pharmacy or hospital.14 In South Africa, chronic dispensing units are set up as the main sources of medications for stable patients with chronic conditions.15This practice is different from what pertains in Ghana, where patients with chronic diseases do not have designated places for medicines. Participants with hypertension and diabetes in both communities also obtained medicines from health institutions in the public sector, presumably, when they go for regular follow up visits. Most of the participants with hyperten-sion and diabetes are enrolled on the NHIS and hence are entitled to free medicines for the manage-ment of hypertension and diabetes when they go on follow-up visits.
Access to medicines plays an important role in the health care delivery system. It serves as an input that should be available for an efficient and effective service delivery. It has been found that health systems are usually strengthened when adequate structures are in place to ensure equitable access to good quality medicines.16In the rural communities there was no significant association between predisposing and enabling factors and source of medicine by participants after multinomial analysis. In the urban communities however, increasing age was associated with a more likelihood to source medicines from the Over the Counter Medicine Shop (OTCMS) than the pharmacy and an equal likelihood to obtain medicines from the hospital as pharmacy. Participants with hypertension and diabetes in the urban communities have more access to pharmacies than in the rural communities; likewise, also they are able to obtain medicines from the hospital as well. This finding compares with a study that identified age as a predisposing factor among others that influences health service utilization. 17 Essential medicines have been found to be a foundation of almost all public health programmes that aim at reducing morbidity and mortality.18 Access and source of medicines therefore form part of the essential services that should effectively be accomplished to ensure improved health outcomes. The multinomial logistic regression analysis indicated that there was no significant association between the enabling factors of sourcing of medicines in the rural communities. However, in the urban communities, participants within low socioeconomic status were less likely to source medicines from the hospital than the pharmacy. This practice was observed since participants, especially those enrolled on NHIS could obtained their medications at the pharmacy. This finding is similar to a study conducted in Cambodia where it was found that the social health systems in place ensured that persons with hypertension and diabetes had access to medicines appropriate for the management of disease conditions.19 Availability of medicines alone however does not ensure improved health outcomes.20
Source of medicine information
The relevance of medicine information through education and counselling empowers patients in decision making, which can ultimately improve patient outcomes.21A study conducted in Finland indicated that parents’ source of information regarding their children’s medicine use regardless of the age was from health professionals, mostly from the physician and from patient information leaflet. Parents further indicated that information obtained from health care professionals including physicians and pharmacist were found to be reliable.22 In this study, similarly, majority of participants with hypertension and diabetes both in rural and urban communities mostly sought medicine information from the nearest health institutions. Results of this study differ slightly from a study conducted in the US where patients with rare disease conditions used physicians and the internet more often as their medication information source. Male patients were found to use their spouse/partner more often than did female patients. Female patients however, were more likely to use medication package inserts and the internet and were less likely to use nurses than were the male patients.23, 24 A study conducted among Arabic speaking Australians revealed that there was limited access to verbal and written medication and disease information, hence the over-reliance on health care practitioners who do not provide quality and adequate information.25The need to obtain reliable and valid information is very critical for patients who have non-communicable diseases, hence the source of medicine information should be acknowledged as an important tool in improving patient outcomes, as adherence to medication will usually be based on information obtained from the health professional.
The source of medicine or drug information for patients is usually preferred from the physician, while the pharmacist is mentioned as the second preferred source.26This assertion was confirmed in this study as participants in both the rural and urban communities indicated they obtained medicine information from the nearest health institution, while the pharmacy was the second preferred choice. Further analysis to determine what influenced participants’ choice using the multinomial logistic regression test revealed association of increasing age, educational level attained and marital status in both urban and rural communities. Increasing age of participants, increased the relative odds of seeking information on medicines from a family member, friend health professional and nearest health institution than a pharmacy, and less likely for married participants to seek medicine information from a friend health professional in urban communities. This is similar to studies that propose that the physicians are a key source of medicine information.26,27 28 29In the rural communities, married status and educational level obtained by participants with hypertension and diabetes increased the likelihood to source information on medicines from a friend health professional; also increasing age and educational level, were likely to source information from the nearest health institution than the pharmacy.
The participants with low socio-economic status in rural communities preferred to obtain medicine information from the nearest health institution than the pharmacy. This could be as a results of pharmacies are not closer to the rural folds and they to travel a long distances to access them. However, in the urban communities none of the enabling factors shown statistical significance with medicine information.
Limitations
Participants were classified as hypertensive and or diabetic based on their self-report. This could results in a lower prevalence of the disease since some participants are usually in a state of denial when they are diagnosed of chronic diseases such as hypertension and diabetes. Furthermore, some participants might be having the conditions but have not yet been diagnosed.
CONCLUSIONS
Participants with hypertension and diabetes in rural and urban communities sourced medicine and medicine information similarly with a few variations. Most participants with hypertension and diabetes sourced medicines and medicines information from public health institutions- the healthcare centre in the rural communities and the hospital in the urban communities. A few participants in the rural communities sourced for medicine information from friends who were health professionals whereas in the urban communities a few also sourced medicine and medicine information from the pharmacy. Participants’ source of medicines and medicine information were influenced differently by the predisposing factors: age, marital status, education and enabling factor, and socioeconomic status in rural and urban Ghana.