INTRODUCTION
ANATOMY AND PHYSIOLOGY OF THE MAXILLARY SINUS
The maxillary sinus is a bilateral air cavity that occupies the body of the maxilla. It is internally limited by a thin mucous membrane of ciliated respiratory epithelium that is continuous with the nasal epithelium 1]. The drainage ostium of the maxillary sinus opens to the nose through the infundibulum at the level of the middle meatus. The maxillary sinus is drained as a result of the activity of the cilia and the negative pressure produced in the sinus during inspiration. This cavity has several functions: a respiratory function for heating the air that is breathed in; defence and protection against bacterial and viral invasion; resistance to mechanical shocks; and a vocal function, as it acts as a resonant cavity that supports and amplifies the emission of laryngeal sound [2].
WHAT IS THE RELATIONSHIP BETWEEN THE ANTRAL TEETH AND THE SINUS?
Modifications of the sinus mucosa as a consequence of dental pathology result from the intimate anatomical relationship that some teeth have with the floor of the maxillary sinus [3]. The roots of the posterior maxillary teeth are separated from the sinus by a variable thickness of cortical bone and there are also numerous vascular anastomoses that perforate this space and can serve as channels for the propagation of bacteria, facilitating the spread of odontogenic infections towards the maxillary sinus [4].
The teeth most frequently related to the sinus are the first and second upper molars, followed by the premolars, whose relationship depends on the size of the molar and its degree of pneumatization [5]. Furthermore, these teeth tend to have a high prevalence of periapical lesions compared to others, particularly those teeth that have been treated endodontically, in addition to a greater susceptibility to periodontal disease due to dental furcation involvement [3, 4]. This explains why 30 % of maxillary sinusitis cases are dental in origin. In addition, maxillary sinusitis is the most frequent complication after invasive dental treatments (up to 27 %), although the diagnostic criteria are not always straightforward [6].
WHICH DENTAL PATHOLOGIES MAY BE RELATED TO SINUS PATHOLOGY?
Sinusitis of dental origin should be considered in patients presenting symptoms of maxillary involvement who have a previous history of dental infection, dentoalveolar surgery, periodontal pathology, endodontics related to antral teeth, sinus elevations, implants, and those cases resistant to conventional treatment [5, 6].
Odontogenic sinus infections tend to have higher microbiological loads with a high predominance of anaerobic microorganisms. Their clinical characteristics are similar to those of non-odontogenic sinusitis, but they are generally unilateral and not necessarily associated with ostium obstructions [3]. The diagnosis of odontogenic sinus pathologies must, therefore, be multidisciplinary, and a clinical assessment must be complemented by other techniques, such as imaging [6].
WHAT TYPES OF IMAGING TESTS CAN BE PERFORMED TO EVALUATE THE SINUS? WHAT IS THE GOLD STANDARD?
X-rays and clinical dental evaluations are unable to detect antral teeth infections that may cause odontogenic sinusitis. Panoramic x-rays are the most typical two- dimensional image projections used by the majority of dentists to make a general evaluation of the orofacial complex, allowing them to determine the size of an apical lesion, visualise cysts, and evaluate the relationship between the teeth and the sinus floor. They do, however [7], have inherent limitations. In addition, cancellous bone lesions cannot be consistently detected with these radiographic techniques. In the maxilla, the degree the antral roots protrude into the maxillary sinus tends to be overestimated. Another drawback is that the soft tissues of the sinus cannot be viewed effectively [8].
Computed tomography (CT) used to be considered the gold-standard for sinus imaging, although it does have disadvantages when compared to cone beam computed tomography (CBCT), including: greater radiation exposure, and an increased likelihood of generating artifacts when hyperdense materials are present near the area of interest. For this reason, CBCT is now the procedure of choice both for the preoperative evaluation of the maxilla, and to assess sinus health status or pathology [9].
WHICH SINUS DISEASES MAY BE RELATED TO DENTAL PATHOLOGY?
The intimate relationship between the maxillary sinus and the roots of the teeth makes it possible for symptoms originating in the sinus to manifest at the dental level and vice versa. Physiologically, the roots of the teeth are separated from the maxillary sinus by a thin, sometimes non-existent, layer of cortical bone and a mucoperiosteum of variable thickness, which may explain how the sinus inflammation develops [7]. Pathological symptoms of inflammation are common in the maxillary sinus, including mucosal thickening, polypoid lesions, sinus opacification, and hydro-aerial level. The aetiology is varied, it may be secondary to inflammatory and infectious processes, such as periodontal disease, root and dental cysts, endodontic infections, retained teeth, iatrogenic causes, or extractions closely associated with the sinus [10].
Due to the difficulty of differentiating symptoms of dental and sinus origin, a detailed dental history of pathology, symptoms, previous surgeries, treatments, and trauma must be compiled, in addition to radiological studies. Both extraoral and intraoral examinations and complementary tests are also required to ensure a precise diagnosis [11].
JUSTIFICATION AND OBJECTIVE
Despite the fact that dental pathology is recognised as causing some sinus disorders, there is little literature on how to manage this in the scope of dentistry, as 90 % of the published work comes from the field of otorhinolaryngology [7]. Due to the increase in dental procedures and related diagnostic tests, this percentage may now be rising.
The primary objective of this study was, therefore, to determine how much sinus pathology originates from dental pathology or treatment. The secondary goal was to evaluate the frequency with which sinus disease appears in its various forms, by means of a CBCT study.
To this end, the following PICO question was applied: Patients -patients attending an ear, nose and throat (ENT) or dental assessment-; Interventions -CBCT-; Comparison -sinus pathology of oral origin vs. sinus pathology of non-oral origin-; Outcome -how much dental pathology is related to sinus pathology-. In patients who come for an ENT or dental check-up (Patients), who have a CBCT (Interventions) and who have sinus pathology associated or not with antral teeth (Comparison), is it possible to evaluate how much dental pathology is directly related to sinus pathology (Outcome)?
MATERIAL AND METHODS
ELIGIBILITY CRITERIA
Inclusion criteria. We incorporated the articles in English and Spanish that included the abstract and in which the pathology of the maxillary sinus was studied by means of imaging techniques (CBCT, panoramic x-ray or Waters). We included patients who attended their ENT service for sinus disease as well as those who attended their dental service for dental treatment with or without known dental or sinus disease. Meta-analyses, systematic reviews, clinical trials, prospective, and retrospective studies were reviewed.
Exclusion criteria. Papers investigating anatomical variations of the maxillary sinus or other paranasal sinuses, as well as systemic pathologies or those involving microbiology of the maxillary sinus were excluded. Articles that did not include radiological studies of the sinus were also excluded. Clinical cases were rejected.
INFORMATION SOURCES AND SEARCH
Three online databases, PubMed, Cochrane Library and Web of Science, were searched extensively without time constraints.
All types of articles were selected except for clinical cases, due to the scarcity of works in this regard, due to the scarcity of papers on the subject. There are no randomized clinical trials, so most of them are observational since they are studies with findings observed in radiology. No screening by type of article or quality criteria was performed, as it was considered that relevant information could be lost.
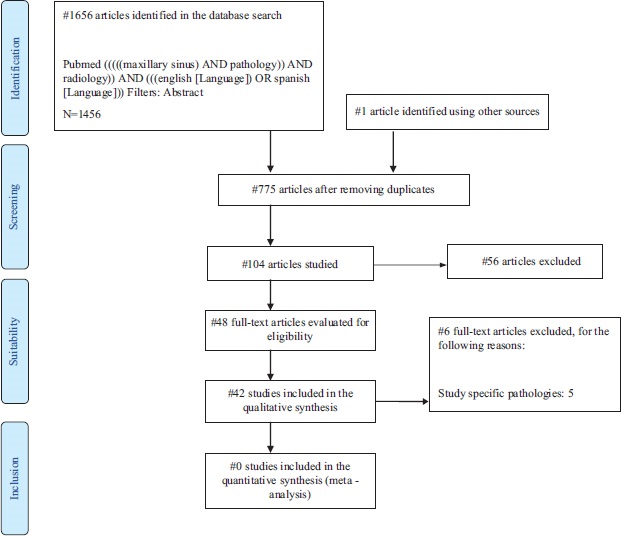
The complete search strategy is shown below and is specified in the flow chart following the PRISMA criteria [12] (Figure 1). The last bibliographic search was carried out on 25/02/2020.
DIAGRAM DESCRIPTION
The initial search strategy used the following combinations of terms: maxillary sinus AND pathology AND radiology. These terms were adjusted according to the requirements of each electronic database. In the three databases used, 1656 articles were identified. In addition, one study identified via other sources was included [13]. Inclusion and exclusion criteria were applied, and after eliminating duplicates, 48 publications were identified as suitable for inclusion as full texts. After reading this series of publications, 6 articles were excluded for the following reasons: study of specific sinus pathologies [14-18] and due to the absence of data in the article and the fact these could not be obtained by contacting the author [19]. Finally, 42 studies were included in the qualitative analysis.
STUDY SELECTION
Data extraction process and data list
The data extracted from each of the studies are detailed below: number of patients, age and sex, diagnostic imaging (CBCT or panoramic x-ray), and number of maxillary sinuses (pathological and physiological). Sinus findings were collected (mucosal thickening, opacification, mucocele, hypoplasia, silent sinus, retention cyst, malignant and benign tumours, polyps, sinusitis, pneumatisation, sinus-associated dental elements, antroliths, fungal infection, ostium obstruction, foreign body, aplasia, and fluid). Dental pathology and general treatments, pre-implant (sinus lift) and post- implant dental treatments were also recorded.
SYNTHESIS OF RESULTS
Of the 42 articles studied, data were extracted on the different sinus pathologies found, as well as the pathology or dental treatment associated with the pathological sinuses. Firstly, a descriptive analysis of the results obtained was carried out in Excel to ascertain the prevalence of the variables mentioned above.
Next, a quantitative parametric inferential analysis was conducted using JAMOVI software (The jamovi Project (2020) jamovi (1.2 version)), by means of the T-student test, as well as various correlations between sinus pathology, pathological sinuses and dental pathology or treatment. To study the correlations, the Pearson linear correlation coefficient was used, which is the most convenient for detecting possible relationships/associations between continuous (numerical) variables. This value can range from -1 to +1, the latter being indicative of a perfect linear relationship; values close to 0 are associated with independence, the null hypothesis in this type of contrast. The results are expressed with their confidence interval with an accuracy of 95 % (CI 0.95), and a standard error of 5 % (0.05).
Due to the high heterogeneity of the data, it was not possible to perform a meta- analysis of the prevalence of sinus pathology related to dental pathology.
RESULTS
STUDY SELECTION AND CHARACTERISTICS
Forty-two articles were selected in which 13,191 patients were examined and 17,374 CBCTs were performed, for dental reasons in 71 % of cases (9,431/13,191) and for ENT purposes in 29 % (3,760/13,191). Of the selected articles, 25 (59.52 %) were case series, 10 (23.82 %) were cross-sectional studies, 3 (7.14 %) case-controls, 2 (4.76 %) cohort studies, 1 (2.34 %) prospective study, and 1 (2.34 %) retrospective study.
Of the 13,191 patients studied, disease was found by chance in 13.05 % (1,721/13,191), while symptoms were present in 34.36 % (4,533/13,191). The other cases were not chance, but it is not specified whether the patients were symptomatic or not in 86.95 % of the cases (11,470/13,191).
RESULTS OF INDIVIDUAL STUDIES
Table 1 (Appendix 1) presents the characteristics of the types of studies included and their duration, detailing the number of pathological or physiological sinuses, as well as pathology and dental treatment.
Figure 2 shows the prevalence of physiological maxillary sinuses 66.26 % (16,918/25,533) and pathological maxillary sinuses 33.74 % (8,615/25,533) with respect to total sinuses studied (25,533).
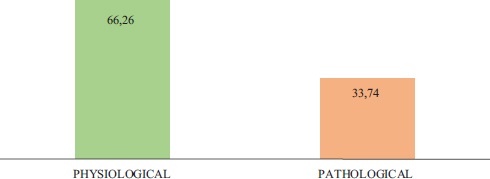
Figure 2. Prevalence of physiological maxillary sinuses and pathological maxillary sinuses with respect to the total number of sinuses studied.
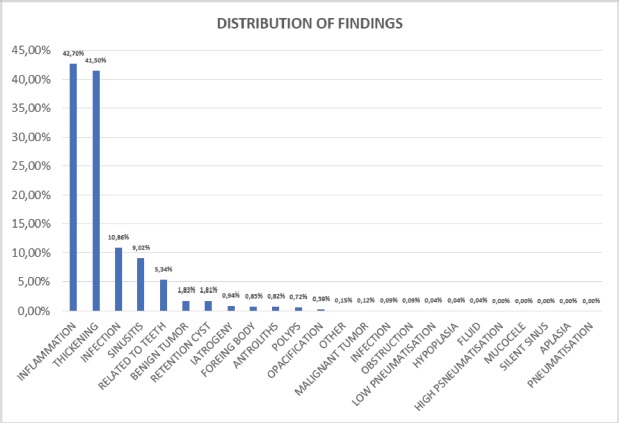
Figure 3 shows the distribution of sinus findings broken down, the most frequent being mucosal inflammation with 42,70 % followed by mucosal thickening 41.50 % and infection with 10,86 %. Absent sinus findings were high pneumatization, mucocele, silent sinus, aplasia and pneumatization.
Table 2 shows the 17 articles that related dental and sinus pathology. As can be seen, within dental pathology (2,495), periapical inflammatory cysts were found in 54.19 % (1,352/2,495) of cases, followed by periodontal disease/bone loss in 34.91 % (871/2,495).
Table 2. Dental pathology associated with the maxillary sinuses studied.
|
AUTHOR/YEAR |
TOTAL No. SINUSES STUDIED |
TOTAL DENTAL PATH |
PERIODONTAL DIS./BONE LOSS |
PERIAPICAL CYST |
DENTAL CARIES |
OTHER |
|---|---|---|---|---|---|---|
|
Aksoy et al., 2018 |
588 |
224 |
No data |
224 |
No data |
No data |
|
Bajoria et al., 2019 |
1,000 |
128 |
60 |
17 |
47 |
4 |
|
Bornstein et al., 2018 |
268 |
18 |
10 |
8 |
No data |
No data |
|
Connor et al., 2000 |
330 |
0 |
No data |
No data |
No data |
No data |
|
Dorothea et al., 2013 |
76 |
17 |
17 |
No data |
No data |
No data |
|
Drage et al., 2013 |
584 |
115 |
No data |
15 |
No data |
100 |
|
Goller-Bulut et al., 2015 |
410 |
159 |
No data |
159 |
No data |
No data |
|
Horwitz et al., 2017 |
162 |
23 |
No data |
23 |
No data |
No data |
|
Kawai et al., 2018 |
338 |
19 |
8 |
11 |
No data |
No data |
|
Maillet et al., 2011 |
164 |
100 |
No data |
100 |
No data |
No data |
|
Nascimento et al., 2016 |
766 |
589 |
254 |
335 |
No data |
No data |
|
Nunes et al., 2015 |
321 |
92 |
No data |
92 |
No data |
No data |
|
Phothikhun et al., 2012 |
500 |
539 |
500 |
39 |
No data |
No data |
|
Pokorny et al., 2013 |
33 |
24 |
9 |
15 |
No data |
No data |
|
Tassoker et al., 2019 |
400 |
141 |
No data |
141 |
No data |
No data |
|
Terlemez et al., 2019 |
570 |
157 |
No data |
157 |
No data |
No data |
|
Troeltzsch et al., 2015 |
174 |
150 |
13 |
16 |
No data |
121 |
|
TOTAL |
6,684 |
2,495 |
871 |
1,352 |
47 |
225 |
Figure 4 shows the distribution of sinus findings broken down, the most frequent being mucosal thickening with 60.65 % (6132/10111), followed by sinusitis 11.20 % (1132/10111) and retention cyst and mucocele with 5.46 % (552/10111).
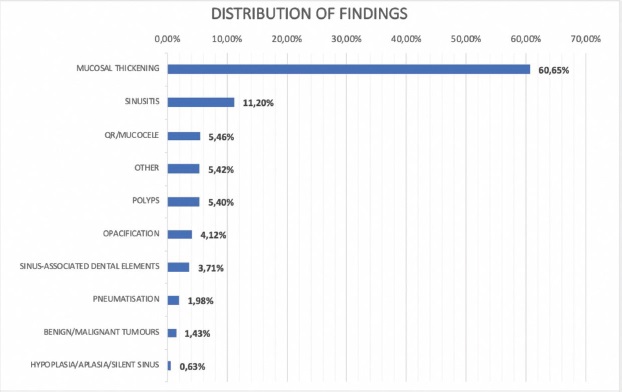
Figure 4. Distribution of sinus findings with respect to maxillary sinuses presenting dental pathology.
Table 3 shows the number of dental pathologies and treatments found, as well as the sum of these in relation to the number of teeth studied (5,558) in the articles that examined one or more teeth per patient.
Table 3. Relationship between number of teeth with pathology and dental treatment.
|
AUTHOR |
DENTAL PATHOLOGY |
DENTAL TMT |
SUM DP-DT |
No. TEETH (relation to the pathology, dental tmt) |
|---|---|---|---|---|
|
Aksoy et al., 2018 |
224 |
143 |
367 |
1,720 |
|
Bajoria et al., 2019 |
132 |
197 |
329 |
No data |
|
Bornstein et al., 2018 |
18 |
3 |
21 |
25 |
|
Connor et al., 2000 |
0 |
192 |
192 |
No data |
|
Dorothea et al., 2013 |
17 |
No data |
17 |
No data |
|
Drage et al., 2013 |
120 |
No data |
120 |
No data |
|
Goller-Bulut et al., 2015 |
159 |
No data |
159 |
1,169 |
|
Horwitz et al., 2017 |
23 |
No data |
23 |
No data |
|
Kawai et al., 2018 |
19 |
12 |
31 |
No data |
|
Maillet et al., 2011 |
100 |
21 |
121 |
534 |
|
Nascimento et al., 2016 |
580 |
234 |
814 |
No data |
|
Nunes et al., 2015 |
92 |
No data |
92 |
No data |
|
Phothikhun et al., 2012 |
539 |
21 |
560 |
No data |
|
Pokorny et al., 2013 |
24 |
No data |
24 |
No data |
|
Tassoker et al., 2019 |
141 |
No data |
141 |
400 |
|
Terlemez et al., 2019 |
157 |
112 |
269 |
1,710 |
|
Troeltzsch et al., 2015 |
150 |
150 |
300 |
No data |
|
TOTAL |
2,495 |
1,085 |
3,580 |
5,558 |
Dental tmt; Dental treatment, Sum DP-DT; Sum of pathology and dental treatment
SYNTHESIS OF RESULTS
The general correlations between the different sinus pathologies with the number of maxillary sinuses, pathological sinuses and dental pathology are described below. The H0 established shows that there is no relationship between the previously mentioned variables, while the Ha indicates the existence of a relationship between them. For the total number of maxillary sinuses with clustered findings, using Pearson's linear correlation coefficient it can be seen that there is a practically direct association with inflammation (0.992), tumours (0.973), infection (0.951), and low pneumatisation (0.814). Among the inflammatory findings, mucosal thickening (0.988), opacification (0.975), and retention cyst (0.960) stand out. The number of pathological maxillary sinuses shows practically the same degree of high linear correlation as described above. Within dental pathology, direct correlation is observed with polyps (1) and opacification (0.999) and there is practically a direct correlation with retention cyst (0.981) and with sinus-associated dental elements (0.972). From the data available, we observed a significant positive relationship between inflammatory cases (0.526) and benign tumours (0.598). Furthermore, there is little inverse relationship between infectious findings (-0.064) and antroliths (-0.273).
Table 4 (Appendix 2) presents the sinus findings grouped into subgroups; inflammation included mucosal thickening, opacification, ostium obstruction, mucocele, and polyps. We also included sinusitis and fungal infection in the infection findings. Tumours were subsequently grouped into malignant, benign, and retention cyst. Low pneumatisation included silent sinus, hypoplasia and aplasia, while high pneumatisation included the data related to pneumatisation. The foreign body group included foreign bodies and antroliths. Finally, symptoms and iatrogeny were grouped together.
DISCUSSION
SUMMARY OF THE EVIDENCE
Maxillary sinusitis is a pathology that, although traditionally viewed as falling within the field of otolaryngology, often involves the participation of dentists, in both diagnosis and prevention [7]. Some researchers have studied the frequency of odontogenic maxillary sinusitis and have presented various treatment methods. However, the information available from a dental perspective is limited, and it is likely that the information in the literature on the incidence of maxillary sinusitis of dental origin is an underestimate [20].
Forty-two articles were included in this review (25 case series [21-45], 10 cross- sectional studies [13, 46-54], 3 case-control studies [55-57], 2 cohort studies [58-59], 1 prospective study [60], and 1 retrospective study [61]). It involved a total of 13191 patients and 17374 CBCTs. The most frequent pathological findings were, by a considerable degree, inflammatory diseases, which represented 75.16 % of the total findings, followed by infection (12.13 %), tumours (6.88 %), and high pneumatisation (2.07 %). Finally, iatrogenic findings, the presence of a foreign body, low pneumatisation and symptoms occurred with a frequency of less than 2 %.
For inflammation, the most frequent finding was the thickening of the mucosa of the maxillary sinus (60.65 %). Of the 42 studies included in this review, 33 found mucosal thickening, with a mean frequency of 69.34 % (range 13.04-100.00 %). In 500 subjects undergoing CBCT tests, Almeida Da Silva et al. [46] observed that most pathological findings were classified as mucosal thickening, representing almost 80 % of the sinus pathology encountered. Connor et al. [41] reviewed 330 CT images of the maxillary sinus in 165 patients to determine whether the presence of dental restoration might predispose to maxillary sinusitis and, in particular, to focal thickening of the maxillary sinus mucosa as a characteristic of dental origin. They found that focal thickening of the sinus mucosa, with or without evidence of rhinogenic aetiology, occurred significantly more frequently in the sinus adjacent to dental restoration. However, the incidence of general pathology in the adjacent maxillary sinus was not significantly different from that in the sinus not adjacent to the dental restoration. These findings suggest a relationship between focal thickening of the maxillary sinus mucosa and the presence of dental restoration, which is likely to be due to an associated dental pathology. For that reason, dental restoration should be identified through a clinical exam and a CT scan, as it is a potential aetiological factor for sinusitis of dental origin. This study found a 37.5 % prevalence of mucosal thickening on CBCT images [46]. Similar results were also observed by Ritter et al. who reported a 38.1 % prevalence of mucosal thickening in a CBCT imaging study of 1029 patients [53].
Of the 42 studies analysed here, 17 related maxillary sinus pathology to dental conditions and, specifically, 7 studies [21, 26, 29, 41, 49, 56, 59] found an association between mucosal thickening of the maxillary sinus and dental modifications.
Aksoy et al. [21] retrospectively evaluated the thickening of the maxillary sinus mucosa and its relationship with dental conditions using CBCT imaging in a total of 294 patients and involving 588 maxillary sinuses. In 172 patients (58.5 %) they found mucosal thickening of more than 2 mm, which was considered the pathological threshold, in one or both maxillary sinuses. In addition, the prevalence of pathological mucosal thickening for maxillary sinuses with and without periapical lesions was 42.1 % and 53.6 %, respectively (p<0.05), and this increased significantly (p<0.05) in patients with alveolar bone loss. On this basis, they concluded that multiple conditions, including periapical infections, endodontics, and the close relationship of the maxillary teeth with the sinuses, may have a precursor effect on the appearance of maxillary sinus mucosa thickening. Consequently, the periodontal status and its role as a risk factor for triggering sinus infections should be considered not only by dentists, but also by medical professionals to establish the treatment of maxillary sinus injuries.
Connor et al. [41] reviewed 330 CT images of the maxillary sinus in 165 patients to determine whether the presence of dental restoration might predispose to maxillary sinusitis and, in particular, to focal thickening of the maxillary sinus mucosa as a characteristic of dental origin. They found that this thickening of the sinus mucosa, with or without evidence of rhinogenic aetiology, occurred significantly more frequently in the sinus adjacent to dental restoration. However, the incidence of general pathology in the adjacent maxillary sinus was not significantly different from that in the sinus not adjacent to the dental restoration. These findings suggest a relationship between localised thickening of the maxillary sinus mucosa and the presence of dental restoration, which is likely to be due to an associated dental pathology. For that reason, dental restoration should be identified through a clinical exam and a CT scan, as it is a potential aetiological factor for sinusitis of dental origin.
Nascimento et al. [26] evaluated the most common types of maxillary sinus disorder (generalised and localised mucosal thickening, maxillary sinusitis, and retention cysts) and their association with dental conditions (inadequate endodontic treatment, periapical lesions and periodontal bone loss) in CBCT images of 400 patients with disease in one or both maxillary sinuses. The most prevalent sinus pathologies were generalised (65.2 %) and localised (24.8 %) mucosal thickening, which were also the only ones related to dental conditions (periodontal bone loss and periapical lesions, respectively).
The case series study by Dagassan-Berndt et al. [56], based on CBCT images, looked at the presence of maxillary sinus mucosa thickening in two groups of patients with advanced dental pathology: 17 patients scheduled for maxillary molar surgery who underwent a CBCT for preoperative diagnosis (dentate group) and 21 patients who required a CBCT for the insertion of an implant in the posterior maxilla and who served as controls (edentulous group). The thickness of the sinus mucosa was significantly greater in the dentate group than in the edentulous group, both in the first molar position (p=0.028) and in the second (p<0001). In addition, periapical lesions(p=0.008) and the distance between the tooth apices and the maxillary sinus (p=0.036) was significantly associated with the thickness of the maxillary sinus membrane.
In our review, the dental modifications that were most frequently related to sinus pathology were periapical inflammatory cysts (54.19 %) and periodontal bone loss (34.91 %). Other systematic reviews and meta-analyses [7] have also investigated the aetiologies of maxillary sinusitis and its relationship with dental pathology, with mixed results.
Furthermore, the review by Terlemez et al. [59] described the fact that anatomically associated periapical lesions of the maxillary sinus, seen on CBCT images, were a risk factor (OR: 2.7; p<0.05) for mucosa thickening.(59) The retrospective study by Goller- Bulut et al. [49] looked at the relationship between maxillary sinus mucosa thickness and periodontal bone loss with related periapical tooth conditions, as well as the association between the tooth apices and the lower wall of the maxillary sinus, in CBCT images of 250 patients, involving 410 maxillary sinuses. They found a significant correlation between mucosal thickness and the severity of bone loss and apical lesions. Phothikhun et al. [29] also observed an association between the severity of periodontal bone loss, as assessed by CBCT, and mucosal thickening of the maxillary sinus (OR: 3.02; p<0.001), but no association was found with periapical lesions.This is consistent with the results of our review which revealed mucosal thickening to be the most frequent disease (60.65 %) in the studies analysed, while retention cysts and opacification accounted for only 5.46 % and 4.12 % of the total findings, respectively.
Arias-Irimia et al. [7] found iatrogeny to be the most frequent cause (55.97 %) of odontologenic maxillary sinusitis. Other possible aetiologies were periodontitis (40.38 %) and odontogenic cysts (6.66 %). The most prevalent iatrogenic causes were oroantral fistulas and root remains, taken together as iatrogeny after dental extraction, which accounted for 47.56 %, while dressings for closing these oroantral fistulas and non-specific foreign bodies constituted 19.72 %, and extrusion of filling materials for endodontics in the maxillary sinus represented 22.27 %. These results are not in line with the findings of our review, which showed that iatrogenic findings were very rare, making up only 1.78 % of the total number of pathological findings observed.
Pearson’s correlation analysis of the number of pathological maxillary sinuses revealed very high and significant associations with inflammation (r=0.992, p<0.001), tumour (r=0.976, p<0.001), infection (r=0.949, p<0.001), and low pneumatisation (r=0.879, p=0.021). In the case of inflammation, the most important correlations were with mucosal thickening (r=0.898, p<0.001), opacification (r=0.978, p<0.001), and retention cysts (r=0.971, p<0.001). For dental pathology, direct correlations were observed with polyps (r=1.000; p=0.007), and opacification (r=0.999; p<0.00), and practically direct correlations were seen with retention cysts (0.981; p<0.00) and sinus-associated dental elements (r=0.972; p=0.006). Finally, when we analysed the correlations between sinus pathology and the sum of pathology and dental treatment, we observed a positive and significant association with inflammatory findings (r=0.526; p=0.044) and, specifically, with sinus mucosa thickening (r=0.536; p=0.040). In contrast, the other pathological findings showed no association with dental pathology and/or treatment.
In summary, the results of this review demonstrate remarkable evidence for a relationship between maxillary sinus pathology and, particularly, sinus mucosa thickening and the presence of dental modifications in CBCT images. However, although most studies describe an association between sinus pathology and dental pathology, the most frequently observed dental aetiologies are inconsistent. Finally, we found that the presence of an inflammatory sinus pathology, and specifically the thickening of the mucosa of the maxillary sinus, correlates positively and significantly with dental pathology and/or treatment.
LIMITATIONS
The aim of this study was to review the data available in the literature on odontogenic maxillary sinus pathology. The results highlight the importance of dental modifications, observed by means of CBCT, as a frequent cause of maxillary sinusitis, offering a new perspective on the pathology of the maxillary sinus. However, the study has a number of limitations.
Selection bias is one of the most important aspects to be addressed in a review article. For this review, we selected studies that included CBCT images of otolaryngology patients with maxillary sinusitis and dental patients with or without dental and/or sinus pathology. One limitation is the existence of possible confounding factors resulting from the heterogeneous characteristics of the patients.
Other limitations are linked to the very nature of the case series, cross-sectional and case-control studies, which have inherent bias in their retrospective design. In addition, we did not assess the methodological quality of the selected studies.
Finally, due to the heterogeneity of the data collected from the included studies, it was not possible to perform a meta-analysis on the prevalence of odontogenic maxillary sinusitis.
CONCLUSIONS
The incidence of sinusitis of dental origin is probably underestimated in the available literature. The most recent studies suggest a much higher incidence, close to 30-40 % of all cases of chronic maxillary sinusitis. Inflammatory processes and, in particular, the thickening of the mucosa of the maxillary sinus are frequently related to the presence of dental modifications observed in CBCT images, either due to pathologies or complications after dental treatment. However, given the heterogeneity of the studies included in this review, it was not possible to estimate the prevalence of maxillary sinusitis originating from dental pathologies and/or treatments.
Inflammatory-type alterations of the maxillary sinus account for approximately three thirdsof all pathological findings observed on CBCT images. We also identified infections, tumours and the presence of high pneumatisation in the maxillary sinus, although at a lower frequency. In contrast, other possible causes of sinus pathology, such as iatrogeny, the presence of foreign bodies, and low pneumatisation are very rare in the work included in this review. The majority of the studies agree on an association between maxillary sinus pathology and dental pathology, but diverge in terms of the dental causes most commonly observed in patients with maxillary sinusitis. The dental disorders most frequently associated with sinus pathology are periapical inflammatory cysts and periodontal bone loss.
In conclusion, our results further support the argument that dental modifications and treatments are an important cause of sinus pathology. For this reason, dental aetiologies must be taken into account by both dentists and maxillofacial surgeons when considering the most appropriate treatment for patients with maxillary sinusitis.