Meu SciELO
Serviços Personalizados
Journal
Artigo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Acessos
Acessos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em
SciELO
Similares em
SciELO -
 Similares em Google
Similares em Google
Compartilhar
Revista Española de Enfermedades Digestivas
versão impressa ISSN 1130-0108
Rev. esp. enferm. dig. vol.105 no.1 Madrid Jan. 2013
https://dx.doi.org/10.4321/S1130-01082013000100008
PICTURES IN DIGESTIVE PATHOLOGY
Loculated hydrothorax: An unusual complication of hepatic cirrhosis
Hidrotórax loculado: una complicación inusual de la cirrosis hepática
Rogger Álvaro Bendezú-García, Marta Lázaro-Sáez, Álvaro Hernández-Martínez, Gustavo Oliver Patrón-Román, Marco Antonio Rodríguez-Manrique, Sergio Amat-Alcaraz and José Luis Vega-Sáenz
Department of Digestive Diseases. Hospital Torrecárdenas. Almería, Spain
Introduction
Ascites is the most common complication in hepatic cirrhosis and is a bad prognosis factor. Predominantly located in the abdomen, it can sometimes affect the thorax, representing a challenge to the physician when it presents with a peculiar morphology, such as loculated intrathoracic ascites.
Clinical case
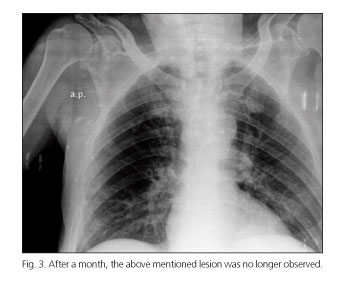
A 67-year-old man with hepatic cirrhosis caused by alcoholism and with no cardiopulmonary history was admitted for symptoms of hepatic encephalopathy secondary to constipation. The chest X-ray showed a radio-opaque lesion, rounded with regular edges in the left hemithorax that was not present in previous check-ups (Fig. 1). Empirical antibiotic treatment was started due to suspected pneumonia. In the thorax CT, the collection showed smooth, regular edges and content with "water" density, suggesting the possibility of loculated intrathoracic ascites (Fig. 2). The patient's symptoms rapidly improved, but the above lesion persisted on discharge, disappearing after a month of diuretic therapy (Fig. 3).
Discussion
Hepatic hydrothorax or intrathoracic ascites is the pleural effusion in a patient with cirrhosis with no cardiopulmonary disease (1). Mainly located on the right side (2), it can appear loculated due to the existence of adherences or walls between both pleura, preventing the liquid from flowing to the adjoining areas. When present, it is important to consider the possibility of haemothorax or empyema as differential diagnoses. In our case the absence of respiratory clinical symptoms, the radiological characteristics of the lesion and the favourable development with diuretics confirmed the diagnosis. A chest CT is recommendable to rule out lung, mediastinal or pleural diseases and even a thoracentesis for suspected empyema or haemothorax. The treatment consists of diuretic treatment, thoracentesis or insertion of a TIPS if there is no response to medical treatment (3), even considering the possibility of medical procedures (4).
References
1. Cárdenas A, Arroyo V. Management of ascites and hepatic hydrothorax. Best Pract Res Clin Gastroenterol 2007;21:55-75. [ Links ]
2. Lazaridis KN, Frank JW, Krowka MJ, Kamath PS. Hepatic hydrothorax: Pathogenesis, diagnosis, and management. Am J Med 1999;107:262-7. [ Links ]
3. Xiol X, Castellote J, Cortes-Beut R, Delgado M, Guardiola J, Sese E. Usefulness and complications of thoracentesis in cirrhotic patients. Am J Med 2001;111:67-9. [ Links ]
4. Meyer CA, White CS, Sherman KE. Diseases of the hepatopulmonary axis. RadioGraphics 2000;20:687-98. [ Links ]











 texto em
texto em