INTRODUCTION
Systemic lupus erythematosus (SLE) is an autoimmune connective tissue disease, characterized by the production of anti-nuclear and anti-double-stranded DNA autoantibodies [1, 2, 3]. Its prevalence is estimated at 17-48/10,000 population, and is particularly frequent in women of childbearing age [1, 2, 3]. It is distinguished by a large clinical polymorphism making its diagnosis a real challenge for health professionals [1, 2, 3].
Cutaneous manifestations can be seen in up to 85% of SLE cases [3, 4, 5]; the most frequent and classic are: malar rash, photosensitivity, discoid lupus, nonscaring alopecia, and oral ulcers [3].
Bullous systemic lupus erythematosus (BSLE) represents an exceptional and challenging variant of vesicobullous presentations of cutaneous lupus [4, 5].
Clinically these lesions appear as localized or diffuse tense vesicles and bullae (blisters) over erythematous or normal skin, both in sun-exposed and non-exposed skin and mucosa [3, 4, 5]. Specific histological changes of this lesion are: subepidermal cleavage with dense neutrophilic infiltration, inflammatory infiltration predominant in the upper dermis and the basement membrane zone (BMZ), leukocytoclasis, linear and/or granular deposits of immunoglobulins (IgG, IgA or IgM) and/or C3 fraction of complement on indirect immunofluorescence, ant detection of anti-type VII collagen antibodies in approximately 70% of cases [4, 5].
We report the original observation of BSLE revealing SLE in 32-year-old Tunisian Woman.
CASE REPORT
32-year-old Tunisian woman, without pathological medical history, were referred to our department by his family doctor for suspected autoimmune bullous disease.
The history of the disease dated from three weeks ago by the appearance of multiple vesiculobullous lesions, not pruriginous, with clear contents, and of which the evolution was towards the spontaneous rupture. These lesions sat on the neckline and neck. No fever or other associated functional complaints have been noted. Likewise, no toxic exposure was reported.
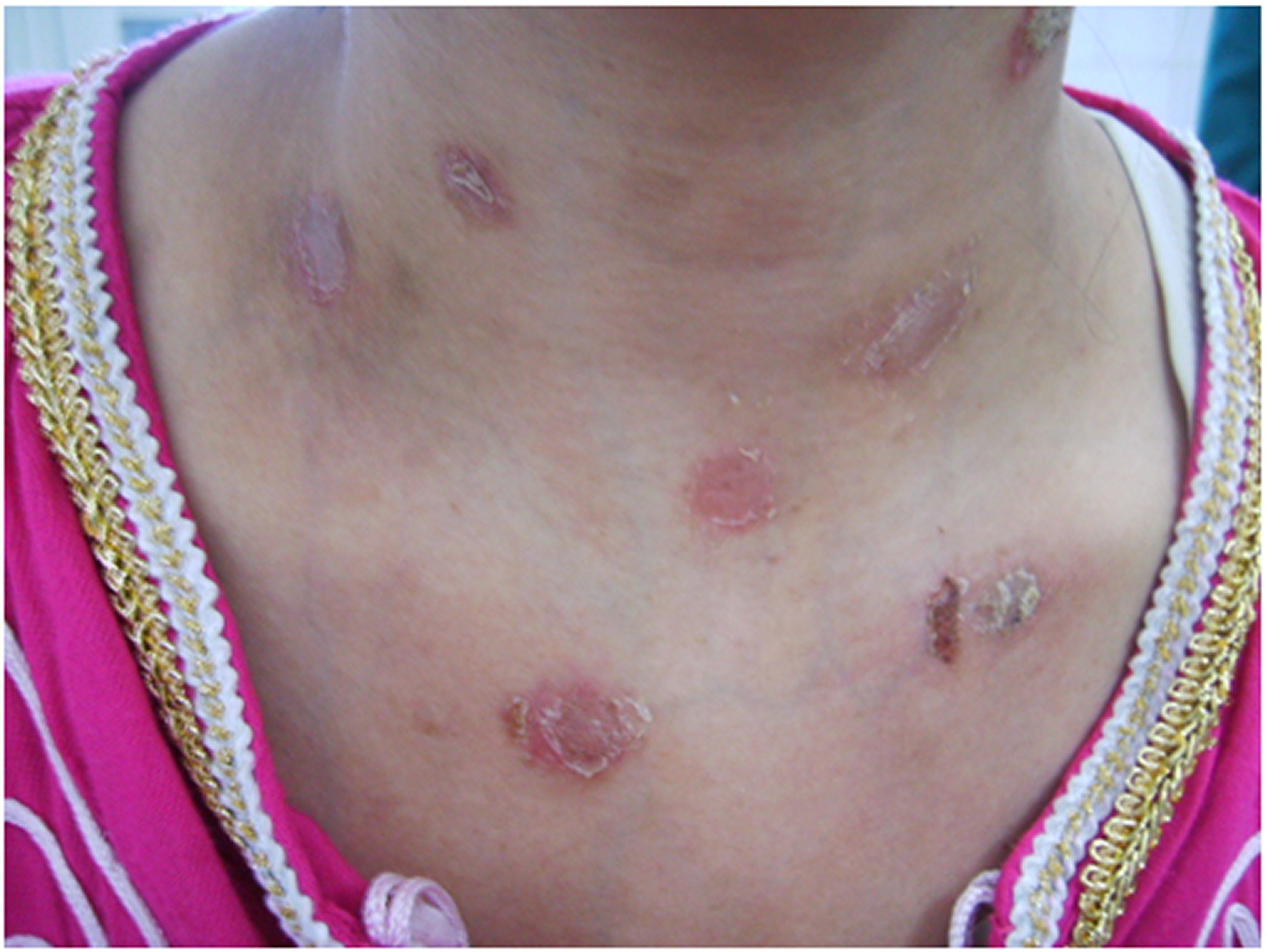
The somatic examination noted multiple ruptured bullous lesions in the neckline and neck (Figure 1), without other anomalies. In particular, no organomegaly, palpable masses, peripheral lymphadenopathy, or mucosal lesions have been noted.
Biology showed a marked biological inflammatory syndrome (erythrocyte sedimentation rate at 120mmH1, C-reactive protein at 86mg/l, and polyclonal hypergammaglobulinemia at 28g/l), normochrome normocytic anemia at 10g/dl, leukopenia at 3600/mm3, neutropenia at 2050/mm3, and thrombocytopenia at 89,000/mm3.
The other basic laboratory tests were within normal limits: creatinine, transaminases, calcemia, blood glucose, serum ionogram, muscle enzymes, lipid parameters, and thyroid hormones.
The chest X-ray and the electrocardiogram were without significant abnormalities.
Histological examination of a skin biopsy specimen with direct immunofluorescence objectified subepidermal blistering, significant inflammatory infiltrate of the dermis, predominantly neutrophilic, and linear deposition of immunoglobulin G (IgG) at the basement membrane zone compatible with a lupus band. Tests with circulating BMZ antibodies were negative.
The immunological assessment revealed positive anti-nuclear, anti-double-stranded DNA, anti-Sm, and anti-phospholipid antibodies.
Investigations for specific visceral SLE disorders (renal, cardiovascular, pulmonary, and neurological) were negative.
Thus, the diagnosis of SLE with cutaneous and hematological involvement was retained. The patient was treated with systemic glucocorticoids at the dose of 1mg/kg/day for four weeks followed by progressive decrease, hydroxychloroquine at 400mg/d, and salicylate at 100mg/d.
The outcome was rapidly favorable: disappearance of skin lesions, normalization of total blood count, and normalization of biological parameters of inflammation.
DISCUSSION
Vesiculobullous lesions are rare in patients with SLE; they can be developed by less than 5% of them [5]. Among these lesions, BSLE is observed only in less than 1% of cases [5, 6].
The first well-documented case of BSLE was published by Hall RP et al, in 1982 [7]; since the majority of cases are reported as sporadic observation or small series not exceeding ten cases [4, 5, 6, 7, 8, 9, 10]. Indeed, the latest systemic review of the world literature by de Risi T et al, in 2017 found only 118 published cases of BSLE [8].
As a result, the exact frequency of this exceptional cutaneous presentation of lupus remains difficult to estimate. Pons-Estel GJ et al, cohort of 1480 patients with SLE and cutaneous involvement from nine Latin American countries found only six cases of BSLE (0.41%) [6], and the largest series of patients with cutaneous lupus of Chanprapaph K et al, (5149 patients from Thailand) reported only 10 cases of BSLE (0.19%) [5].
The positive diagnosis of this unusual skin form represents a real challenge for the clinician; it poses the differential diagnosis of all other subepidermal autoimmune bullous skin diseases [5]. Therefore clinical, histological, and immunological criteria have been proposed and validated for the diagnosis of BSLE [11].
The best treatment for BSLE is dapsone [7, 8, 10, 12]. In cases of intolerance or ineffectiveness of dapsone, systemic glucosteroids alone or in combination with hydroxychloroquine or other immunosuppressants can be used with success [8, 10, 12]. In refractory and/or severe cases, biotherapy (rituximab) finds its indication [13].
Classically, BSLE is an acute condition which responds favorably to specific treatment. These lesions heal without scar or milia, and recurrences are exceptional [5, 6, 8, 10]. Indeed, the frequency of recurrences is very difficult to assess since the majority of observations reported in the literature are sporadic cases; in the series of Chanprapaph K et al of 12-year retrospective review of BSLE in cutaneous and systemic lupus erythematosus patients, only two cases of recurrence were noted respectively six weeks and four months after the diagnosis [5].
CONCLUSIONS
The cutaneous manifestations of systemic lupus erythematosus are very polymorphic and sometimes non-specific. The vesicubullous forms of these manifestations are exceptional, unusual, and very little known by health professionals. BSLE is one of the rarest and most challenging of these lesions. It deserves to be known by clinicians and discussed in front of any bullous dermatosis, particularly in young woman.