Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
The European Journal of Psychiatry
versión impresa ISSN 0213-6163
Eur. J. Psychiat. vol.30 no.4 Zaragoza oct./dic. 2016
Analysis of errors in verbal fluency tasks in patients with chronic schizophrenia
Flavia Galavernaa,b,c; Adrián M. Buenoa; Carlos A. Morraf; María Rocab,c,d and Teresa Torralvab,d,e
a Laboratory of Experimental Psychology, Faculty of Psychology, National University of Córdoba, Córdoba. Argentina
b Laboratory of Neuropsychology, Institute of Translational and Cognitive Neuroscience (INCyT), INECO Foundation, Favaloro University, Buenos Aires, Argentina; National Scientific and Technical Research Council (CONICET), Buenos Aires. Argentina
c National Scientific and Technical Research Council (CONICET), Buenos Aires. Argentina
d Institute of Neurosciences, Favaloro University, Buenos Aires. Argentina
e Australian Research Council (ACR), Centre of Excellence in Cognition and its Disorders
f "Prof. León S. Morra Sanitarium", Córdoba. Argentina
FSG is a beneficiary of a doctoral research fellowship PDFT SECYT-UNC FONCYT, from the Secretary of Science and Technology of the UNC, in the framework of the Human Resources Training ANPCyT. The SECYT-UNC FONCYT has had no further role in study design, collection, analysis and interpretation of data, writing of the report, or the decision to submit the paper for publication.
ABSTRACT
Background and Objectives: Even if verbal fluency deficits have been described in Schizophrenia, error pattern in this test has not been analyzed in detail in the literature. The pattern analysis of such errors could contribute to the understanding of the factors that influence poor task performance in schizophrenia. In this study we analyzed the intrusion and perseveration errors in verbal fluency tasks in patients with chronic schizophrenia.
Methods: 87 patients diagnosed with Chronic Schizophrenia and 87 healthy controls were included in this investigation and were assessed with four Phonological and Semantic Verbal Fluency tasks.
Results The results of this study showed that at least half of schizophrenic patients produced perseverative errors on verbal fluency and about made intrusion errors. The severity of negative symptoms, the severity of Formal Thought Disorder and pharmacological variables were significant moderators to errors in Verbal Fluency performance.
Conclusions Errors in Verbal Fluency can be explained by the interaction of different variables in patients with schizophrenia. Schizophrenia is a psychological pathology with great phenomenological complexity and its particularities can only be explained by the consideration of the multiple factors involved in its manifestation.
Keywords: Chronic schizophrenia; Verbal fluency; Errors; Intrusions; Perseverations.
Introduction
Verbal Fluency (VF) tasks are linguistic production tests that need start up several cognitive mechanisms (processing speed, attention, semantic memory, executive functions). The clinical application of this neuropsychological instrument has become important, because it has proven sensitivity to different brain pathologies. An example is the Schizophrenia. Impairments in VF have been reliably demonstrated in patients with schizophrenia1-16. Despite this strong evidence, some findings are contradictory when a type of task is considered; being that some studies observed more impairment in semantic verbal fluency (SVF)4,12,17-18, whereas other studies support the hypothesis of a specific alteration of performance in phonological verbal fluency (PVF)3,19-21 which has been associated with frontal lobe disturbance22.
Several factors could have an influence in the performance in VF tests. For example, there are many associations between psychotic symptoms and word production in VF7,15,20,23-26; but these associations are stronger with negative symptoms rather than positive ones. Antipsychotic medication effects have been studied by several authors; however there are controversial results; especially when effects of the new antipsychotics are compared to conventional antipsychotics27. Typical antipsychotics provide a small benefit for the treatment of cognitive disturbances in schizophrenia, and atypical antipsychotics such as clozapine, risperidone, olanzapine and quetiapine appear associated with improved cognitive27-30.
Despite the great number of studies that characterize VF in schizophrenia, there is little information about the errors that patients made in these types of verbal tests. The patients produce fewer words than healthy controls and make a higher number of mistakes than control subjects3. However, the description of the errors committed by this population is not frequently reported and the investigation of a pattern analysis of their performance is needed, because errors in neuropsychological tasks are aberrant behaviors that arise for several reasons and are associated with certain neurological conditions. These aberrant responses give a sample of the patient's behavior that allows the neuropsychologist to approach how the patient thinks and how he perceives himself, the world and its expectations32.
Perseverations and intrusions are the types of errors that can commonly be found in VF tests. Perseveration could be defined as the inappropriate repetition of an earlier response33. However, the term perseveration is used to describe a wide variety of phenomena, so we can say that perseverations are not a unitary phenomenon34. According to Sandson and Albert35 there are three possible perseveration errors: stuck-in-set, recurrent and continuous. This classification depends on the complexity of the affected behavior36. Stuck-in-set perseveration is defined as the inappropriate maintenance of a current category or framework and involves a deficit in executive functioning and it has been related to altered function in the frontal lobe35. Recurrent perseveration is an unintentional repetition of a previous response to a subsequent stimulus, involves an abnormal post-facilitation of memory traces and it has been related to posterior left hemisphere malfunction35. It consists in the repetition of an earlier response when processing a series of consecutive incentives as observed in aphasic patients36. For example, the production of the same word on successive trials of an objectnaming task. Lastly, continuous perseveration is the inappropriate prolongation or repetition of a behavior without interruption, involves a deficit in motor output and is associated with damage to the basal ganglia. For example, in word writing it's an addition of letters, "lobster: lobbster" and "door: dooor"34. According to this classification and at level of analyses, the perseveration found in VF tasks may be classified as "stuck-in-set" perseveration or recurrent perseveration; that is as an executive problem to switch from one response strategy to another34 or an abnormal post-facilitation effect in the memory traces.
On the other hand, an intrusion error could be defined as an unintentional recollection of inappropriate information37. Intrusions are inappropriate responses that can be expressed in different behaviors in VF tasks, such as bringing up a word that does not belong to the specified category in SVF, or retrieving a word that does not begin with the correct letter or words that are proper names in PVF. Examples of intrusions in the animal VF task may be: "Dog - Cat - Squirrel - Wolves - Balloons - Birthday - Yerba Mate - Sugar - Grapefruit juice - Flour". The verbal intrusions may be indicative of decreased inhibition and/or increased susceptibility to interference38,39 and have been associated with several diseases such as Huntington's disease40-42, Frontotemporal Dementia43, Alzheimer's Disease44-48, Tourette syndrome and ADHD39,49, HIV-associated dementia50 and psychiatric disorder such as Bipolar Disorder51 and Schizophrenia19,52. Allen, Liddle & Frith19 found that patients with incoherence of speech produce inappropriate words (intrusions) in VF tasks. They propose that both poverty of speech and incoherence of speech reflect problems in the retrieval of words from the semantic memory.
Even if the variables involved in the errors made in VF tests have not been extensively studied, some researchers have proposed a cognitive mechanism that could underlie perseveration errors. From studies on healthy individuals, previous studies have suggested that the failure of two mechanisms could be on the basis of this abnormal behavior: inhibition and activation. Failure on inhibition implies the use of an answer previously activated; instead of the one suitable to the present objective; because the previous answer is not correctly inhibited53. On the other hand, a failure on activation could produce a perseveration error because a wrong answer receives a slight abnormal activation phenomenon that could be explained by residual activation or enhanced learning. Even if they have been described as different mechanisms, inhibition and activation are nothing but complementary53. If there were a failure in activating an objective response, perseveration errors might occur because a previous answer remains activated and thus is mistakenly chosen as an answer.
The cognitive basis of perseverations has also been extended to explain intrusion errors, answers that have not appeared recently or omissions. The prevalence of perseveration and intrusion should be associated with varying degrees of severity of a failure-to-activate deficit53. When the deficiency in activation increases, the number of perseveration errors could increase too, as well as, the number of intrusions or omissions53. In case of a failure in inhibition, either a previous answer or the objective response could be highly activated.
In a previous study we found that psychotic positive symptoms were correlated with the generation of errors in the VF tasks in patients with schizophrenia54. However, a number of issues emerged for consideration in future studies. For example, the percentage of patients with chronic schizophrenia who are failing, and predictors may be related to the production of errors in these tasks in addition to the severity of psychotic symptoms. This study analyzed the amount of mistakes and also intended to explain their presence considering multiple factors such as sociodemographic, cognitive, clinical, and pharmacological variables.
Materials and methods
Participants
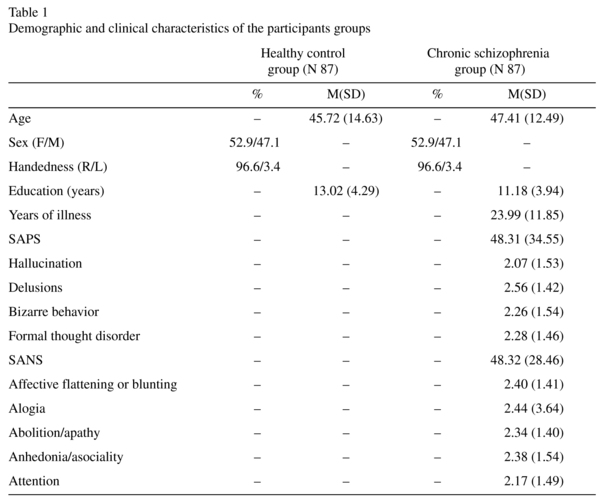
The study included 87 patients diagnosed with chronic schizophrenia from the mental health institutions of "Prof. León S. Morra" Sanitarium and the "San Nicolás" Clinic and 87 healthy controls volunteers from the Faculty of Psychology, National University of Cordoba and Retired Center "Puerreydón" and others from the city of Córdoba, Argentina. All of the participants were aged between 18 and 72 years, and were both male (N = 41) and female (N = 46). Different educational levels were included (Table 1).
The selected participants were patients who fulfilled the criteria for Schizophrenia Disorder DSM IV-TR based on the Structural Clinical Interview for DSM-IV and Chronic Schizophrenia (continuous signs of the disease for more than two years). The patients had to be psychiatrically stable for at least two weeks on their treatment with antipsychotic drugs before participating in the study. In addition, participants were required to give their informed consent during the initial interview. The exclusion criteria were neurological illness, traumatic brain injury, a history of electroconvulsive therapy, and alcohol/substance abuse or addiction.
For healthy controls exclusion criteria were: cerebrovascular accident (CVA), traumatic brain injury, episodes of coma, epilepsy, loss of consciousness for more than 20 minutes, cardiomyopathy, nephropathy, hepatic encephalopathy, thyroid problems, diabetes, chronic headaches, hypertension, recurrent sleep alterations, diagnosed psychiatric alterations and drug use. In addition, those subjects who have direct family history of severe psychiatric disorders were excluded.
The study was approved by the "Prof. León S. Morra" Sanitarium Ethics Committee, and written informed consent was obtained from all subjects.
Measures
Symptom assessment
Scale for Assessment of Positive Symptoms (SAPS) - Spanish version55. The SAPS was used to assess the display of positive psychotic symptoms of the participants as it is specifically designed to assess these kinds of symptoms.
Scale for Assessment of Negative Symptoms (SANS) - Spanish version55: The SANS was used to evaluate the negative psychotic symptoms due to its specificity in assessing psychotic symptoms present in schizophrenia.
Neuropsychological Measures
Verbal Fluency Test: It is a wordnaming task. It has two versions that can measure the fluency of speech. Just the number of intrusions and perseverations were analyzed on this evaluation.
Semantic Verbal Fluency Test (SVF).We used the "Animal" naming task32 and a variation of the test using "Fruits or Animals"56 as the stimulus. In the first one, participants had to name as many animals as possible during a minute without repeating them. In the alternating semantic fluency test, participants had to name as many fruits and animals as they could during a minute.
Phonological Verbal Fluency Test (PVF).The letter "P" was chosen as a stimulus on the first verbal fluency test, where participants had to name as many words as possible beginning with the letter "P" in one minute. On the second test participants had to name as many words as possible switching between letters "A" or "F"56. They were told that repeating words, names, places or countries were not permitted.
Boston Naming Test (BNT) - The Shortened Boston Version-1557.In this test participants were asked to name 15 different drawings of objects. Participants were instructed to name the object that appeared on each drawing. In this study they were taken into account the total number of responses called correctly and spontaneously.
Stroop Color-Word Test - Spanish version58.In this format we used three trials: in the first task the participant had to read out loud the names of the colors printed in black ink. In the second trial they were required to name the printed color. And in the third participants were instructed to name the color of the ink printed while the written color was a different one. Scoring in this assessment was by the number of items read or named in a 45-second time limit. This test was used to evaluate different basic cognitive processes. With the first trial we evaluated the capacity to maintain focused attention. And inhibitory attention control was evaluated with the third and interference score.
Procedure
The study involved three sessions. In the first session, the groups were interviewed to learn about their socio-demographic background in order to select possible participants. After this, they were explained the objectives of the study, the scientific use of the results of the study, making clear that their identity would be kept secret and that all the data collected would be referred to a number and a letter. The participants that accepted to be included in the study signed a written informed consent to participate and then underwent a structured interview regarding their relevant clinical and mental health history. This interview consisted in a series of previously established questions regarding their personal and family history of mental disorders, both suspected and positive, and the presence of any concomitant personal or family medical illness. The cognitive evaluation was then performed in a subsequent session of 45 minutes, in which two professionals specialized in neuropsychology applied to psychiatric disorders carried out the four tests of VF with a 10 minute interval between each task. The tests were recorded with the consent of the patients for a better assessment of their performance. At the same time, and with due authorization, the clinical histories of the patients were examined to corroborate their socio-demographic (i.e. level of education) and clinical data (beginning of the illness, years of illness, current medication).
Data analyses
Normal distribution of the results was tested using the Shapiro-Wilk test. T-test was used for differences between the two groups. Hierarchical regression analyses were also used to examine the relationship between errors in VF tasks and four blocks of predictive variables. The blocks were defined as follows: 1) Sociodemographic: age and education in years. 2) Clinical-psychiatric: This included the years of illness and the total scores of the scales assessing psychotic symptoms SANS and SAPS, and total scores on the assessment of each of the symptoms that were included in these scales. 3) Cognitive: that included interference score on the Stroop Color-Word Test and the answers correctly and spontaneously emitted in the Boston Naming Test. 4) Pharmacological: Daily doses in milligrams of Levomepromazine, Haloperidol, Chlorpromazine, Clozapine and Risperidone were included in this block. These antipsychotics were included because of their high percentage of administration in the patient sample. Statistical analyses were performed using SPSS 19 for Windows.
Results
Error descriptive results in Verbal Fluency. Comparison of groups: Healthy Control and Chronic Schizophrenia
The descriptive results showed that the group of chronic patients with schizophrenia made significantly more errors in the four VF tests compared to the control group (Figure 1). Significant differences between healthy controls and patients were also found in the number of errors made in the tests, except for intrusions in both semantic tests (Table 2).
Patients with schizophrenia percentage that committed intrusions and perseverations errors in PVF and SVF
Prior to commencing the descriptive analysis of the errors made in VF tests in the patient group, we analyzed the percentage of patients that made mistakes in the four verbal tasks. Of the total number of patients in the four tests (N = 87), 29.10% made intrusion errors and 51.58% perseveration errors. For the PVF "letter P", 38.40% of the patients made intrusion errors and 19.80% made more than one intrusion. On the other hand, 37.20% of the patients made perseverations and 11.60% made more than one mistake. For the PVF "letters A or F", 44.20% of the patients made intrusion errors and 20.90% made more than one, whereas 34.90% of the patients made perseveration errors and 19.80% made more than one. In the semantic tests, more specifically SVF "animals", 14% of the patients made intrusion errors, and only 4.70% committed more than one. On the other hand, 47.70% of the patients made perseveration errors and 25.60% made more than one perseveration error. For the SVF "fruits or animals", 19.80% of the patients made intrusion errors and 12.80% made more than one intrusion error; 46.50% of the patients made perseveration errors and 24.40% made more than one error. Figure 2 shows patients percentage of errors committed in VF tasks.
Effect of sociodemographic, clinical, pharmacological and cognitive factors on the presence of errors in VF tasks in patients diagnosed with chronic schizophrenia
In order to analyze the effect of a group of variables thought to have an influence in the production of errors in VF tests, eight linear regression analyses were performed in blocks for each type of error (intrusions and perseverations) in each test. Only patients with errors were included in the analysis and all data had a normal distribution. Descriptive data are shown in Table 3.
Three of the regression models had ANOVA results that allowed rejecting the null hypothesis. One was the intrusion errors in the alternating phonemic test of letters "A and F" including 37 patients with ANOVA values F = 6.173 (p = 0.000) and R2= 0.418. The predicting values belong to Block 2 and 3: severity of formal thought disorder [B = 0.566, p = 0.005]; degree of alogia [B = -0.896, p = 0.000]; severity of negative attention symptoms [B = 0.432, p = 0.020], dosage of Haloperidol [B = 0.401, p = 0.007] and dosage of clozapine [B = 0.319; p = 0.023].
Another model that proved acceptable was the perseveration errors made by 30 patients in the same phonemic test, with ANOVA values of [F = 4.279, p = 0.014] and R2= 0.253. This model includes the following three variables: degree of negative symptoms assessed globally by SANS [B = -0.653, p = 0.007], se-verity of apathy/abulia [B = 0.419, p = 0.073] and dosage of levomepromazine [B = 0.353, p = 0.037].
The result of the linear regression for the perseveration errors of 40 patients in the SVF test alternating between "Fruits or animals" also had ANOVA results that allowed rejecting the null hypothesis (F = 7.179, p = 0.002; R2= 0.280). Two variables were involved in this model, years of schooling [B = 0.370; p = 0.012] and degree of formal thought disorder [B = 0.414; p = 0.005]. Table 4 shows the summary of the predictive models.
Discussion
In the present investigation we studied the presence of two types of errors in single option and alternative PVF and SVF tasks in patients with chronic schizophrenia. An interesting result obtained was that at least half of the patients presented perseveration errors and about 30% presented intrusion errors in the VF tasks administered.
Our results also showed that there were a greater number of patients that made perseveration errors than the ones who made intrusion errors in semantic tasks. The opposite pattern was presented in phonemic tests, in which a larger number of intrusion errors were observed. These differences could be due to the cognitive and neurofunctional demands of each test. Although both tasks are supposed to involve the same initiation and monitoring processes controlled by a central executive component59, they present some evident differences regarding the nature of the information that must be processed (semantic or phonemic). Semantic representations processed during the SVF test were organized in categories and subcategories, which allowed an easier spontaneous recovery of associated items. On the contrary, responses processed during PVF tests depended on the phonetic level of the representation independently to their meaning or category, and this could decrease the speed with which they are activated60.
The results of this study are similar to those obtained by Azambuja et al.59 in patients with Huntington's disease, where moderate Huntington patients had a greater number of intrusions in phonologic fluency tests and a greater number of perseverations in semantic tests. Thus, the authors proposed the need to investigate the reasons of these results and established a hypothetical relation between errors and a specific loss in the elaboration of strategies to search for information, or self-monitoring, or inhibition of responses, all characteristics of executive function loss. The fact that our results are similar could indicate that these types of errors might be attributed to an alteration of the fronto-subcortical (fronto-striatal) circuits, which has been reported in this disease. Dysfunction in fronto-striato-thalamic circuitry is hypothesized to be integral to the pathophysiology of schizophrenia61.
Regarding all sociodemographic variables that were considered, only the number of years with the disease was predictive of the number of perseverations in the alternative semantic task. A former study performed on healthy individuals reported that the age factor could influence the presence of errors, particularly perseverations62. However, in this study the age factor had no effect on the number of errors.
In regards to clinical variables, especially the degree of negative symptoms and the severity of formal thought disorder seemed to be highly predictive of the number of errors produced in both semantic and phonemic alternating VF tests. The effect of psychotic symptoms over cognitive functioning of patients, and specifically on the performance in VF tasks, has been widely reported7,15,20,23-26. However, the relationship between severity of all psychotic symptoms and production errors in VF has not been previously reported, few studies have presented relations between specific symptoms such as disorganized speech19.
As to pharmacological variables, typical antipsychotics in particular seemed to be significant predictors of errors in alternating VF tests. The clinical use of this type of drug is useful for the remission of the positive symptoms of the disorder, but chronic and/or high doses induce tardive dyskinesia and other Parkinson's disease-type disorders in over 70% of the patients in addition to cognitive alterations in different processes such as executive functions, memory, processing speed, and others64-66. Tandon and Jibson66 assert the adverse effect of extrapyramidal symptoms on cognitive function, which is aggravated by treatment with anticholinergic drugs67-71. We found no previous studies that specifically established an association between VF task errors and the administration of antipsychotic drugs in patients with schizophrenia. The review of McNamara & Albert33 regarding the neuropharmacology of verbal perseveration, established some study perspectives and clinical applications, showing that some treatments had been efficient in decreasing it and combined with language therapies could be of great clinical utility. The treatment of schizophrenia involves the rational use of multiple forms of treatment among which pharmacology is the most important one66.
One of our hypotheses was that cognitive variables would be predictive of the errors produced in the tasks, particularly inhibitory control, but none of the variables included in the cognitive block predict errors in any of the verbal fluency in this study. Nevertheless, the combination of the different variables can explain the errors made in verbal tasks involving spontaneous word recovery. Schizophrenia is a psychological pathology with great phenomenological complexity and we can only explain its particularities considering the multiple factors involved in its manifestation.
There are certain limitations to the present study that must be taken into consideration for future work in this field. One of them is associated to clinical variables such as schizophrenia subtype, paranoid or non-paranoid patients which were not included in the present study. Some studies have demonstrated that patients with paranoid schizophrenia have a best neurocognitive performance compared to patients with non-paranoid schizophrenia (ie. disorganized schizophrenia)72-77. It seems that disorganized schizophrenia has another cognitive pattern, characterized by deficits in tasks involving the frontal lobe79. Furthermore, other psychopharmacological variables would need to be considered, such as doses of other drugs that can be administered to patients (such is the case of hypnotics, anxiolytics and others).
The novelty of this investigation not only lies in the systematic study of the type of errors made in VF tasks by a group of patients with chronic schizophrenia and the significant number of patients that were found to make these errors, but also the study of the different variables that might be involved in this process. Thus the influence of sociodemographic, clinical, cognitive and pharmacological variables were assessed on the production of errors in four VF tasks, as well as their possible joint effect.
The VF task is widely used in clinical and a qualitative analysis the patient's performance is necessary. The clinical utility of these findings supports again this type of analysis, which not only consider the number of correct words produced, but also the type of errors that can generate a patient as part of their study of cognitive mechanisms for execution of this simple task. Furthermore, the analysis of such errors can help to understand behaviors of patients with schizophrenia on a more complex level, such as disorganized speech and disexecutive function.
Acknowledgments
We thank Dr. Carlos A. Morra, Dr. León Morra, Dr. Fernando Gay, Dr. Griselda Maidana, Florencia Di Yorio, Ana Molina, Cristina Moreno, Sabrina Trovatto, Germán Rodriguez Banegas, Pablo Cumini, and all professionals, psychiatrists, psychologists and nurses for their generous help with our fieldwork.
Conflict of interest
The authors declare that they have no competing interests.
References
1. Heinrichs RW, Zakzanis KK. Neurocognitive deficit in schizophrenia: a quantitative review of the evidence. Neuropsychology. 1998; 12(3): 426-45. [ Links ]
2. Kremen WS, Seidman LJ, Faraone SV, Toomey R, Tsuang MT. The paradox of normal neuropsychological function in schizophrenia. J Abnorm Psychol. 2000; 109(4): 743-52. [ Links ]
3. Elvevåg B, Weinstock DM, Akil M, Kleinman JE, Goldberg TE. A comparison of verbal fluency tasks in schizophrenic patients and normal controls. Schizophr Res. 2001; 51(2-3): 119-26. [ Links ]
4. Bokat CE, Goldberg TE. Letter and category fluency in schizophrenic patients: a meta-analysis. Schizophr Res. 2003; 64(1): 73-8. [ Links ]
5. Vinogradov S, Kirkland J, Poole JH, Drexler M, Ober BA, Shenaut GK. Both processing speed and semantic memory organization predict verbal fluency in schizophrenia. Schizophr Res. 2003; 59(2-3): 269-75. [ Links ]
6. Henry JD, Crawford JR. A meta-analytic review of verbal fluency deficits in schizophrenia relative to other neurocognitive deficits. Cogn Neuropsychiatry. 2005; 10(1): 1-33. [ Links ]
7. Sumiyoshi C, Sumiyoshi T, Nohara S, Yamashita I, Matsui M, Kurachi M, et al. Disorganization of semantic memory underlies alogia in schizophrenia: an analysis of verbal fluency performance in Japanese subjects. Schizophr Res. 2005; 74(1): 91-100. [ Links ]
8. Keefe RSE, Eesley CE. Neurocognitive impairment. In JA Lieberman, TS Stroup, DO Perkins (Eds), Textbook of schizophrenia (pp. 245-60). Washington: American Psychiatric Publishing; 2006. [ Links ]
9. Rossell SL, David AS. Are semantic deficits in schizophrenia due to problems with access or storage? Schizophr Res. 2006; 82(2-3): 121-34. [ Links ]
10. Vogel AP, Chenery HJ, Dart CM, Doan B, Tan M, Copland DA. Verbal fluency, semantics, context and symptom complexes in schizophrenia. J Psycholinguist Res. 2009; 38(5): 459-73. [ Links ]
11. Ojeda N, Sánchez P, Peña J, Elizagárate E, Yoller AB, Larumbe J, et al. Verbal fluency in schizophrenia: does cognitive performance reflect the same underlying mechanisms in patients and healthy controls? J Nerv Ment Dis. 2010; 198(4): 286-91. [ Links ]
12. Juhasz BJ, Chambers D, Shesler LW, Haber A, Kurtz MM. Evaluating lexical characteristics of verbal fluency output in schizophrenia. Psychiatry Res. 2012; 200(2-3): 177-83. [ Links ]
13. Stain HJ, Hodne S, Joa I, Hegelstad WT, Douglas KM, Langveld J, et al. The relationship of verbal learning and verbal fluency with written story production: implications for social functioning in first episode psychosis. Schizophr Res. 2012; 138(2-3): 212-7. [ Links ]
14. Sung K, Gordon B, Vannorsdall TD, Ledoux K, Pickett EJ, Pearlson GD, et al. Semantic clustering of category fluency in schizophrenia examined with singular value decomposition. J Int Neuropsychol Soc. 2012; 18(3): 565-75. [ Links ]
15. Brébion G, Villalta-Gil V, Autonell J, Cervilla J, Dolz M, Foix A, et al. Cognitive correlates of verbal memory and verbal fluency in schizophrenia, and differential effects of various clinical symptoms between male and female patients. Schizophr Res. 2013; 147(1): 81-5. [ Links ]
16. Sumiyoshi C, Ertugrul A, Anil Yağcıoğlu AE, Roy A, Jayathilake K, Milby A, et al. Language-dependent performance on the letter fluency task in patients with schizophrenia. Schizophr Res. 2014; 152(2-3): 421-9. [ Links ]
17. Gourovitch ML, Goldberg TE, Weinberger DR. Verbal fluency deficits in patients with schizophrenia: semantic fluency is differentially impaired as compared to phonemic fluency. Neuropsychol.1996; 10: 573-7. [ Links ]
18. Rossell SL, Rabe-Hesketh SS, Shapleske JS, David AS. Is semantic fluency differentially impaired in schizophrenic patients with delusions? J Clin Exp Neuropsychol. 1999 Oct; 21(5): 629-42. [ Links ]
19. Allen HA, Liddle PF, Frith CD. Negative features, retrieval processes and verbal fluency in schizophrenia. Br J Psychiatry. 1993; 163: 769-75. [ Links ]
20. Joyce EM, Collinson SL, Crichton P. Verbal fluency in schizophrenia: relationship with executive function, semantic memory and clinical alogia. Psychol Med. 1996; 26(1): 39-49. [ Links ]
21. Rinaldi R, Lefebvre L, Trappenier J. Language, executive functioning and symptomatology - Is fluency a transversal tool in schizophrenia? Open Journal of Psychiatry. 2013; 3: 358-69. [ Links ]
22. Troyer AK, Moscovitch M, Winocur G, Alexander MP, Stuss D. Clustering and switching on verbal fluency: the effects of focal frontal- and temporal-lobe lesions. Neuropsychologia. 1998; 36(6): 499-504. [ Links ]
23. Basso MR, Nasrallah HA, Olson SC, Bornstein RA. Neuropsychological correlates of negative, disorganized and psychotic symptoms in schizophrenia. Schizophr Res. 1998; 31(2-3): 99-111. [ Links ]
24. Kerns JG, Berenbaum H, Barch DM, Banich MT, Stolar N. Word production in schizophrenia and its relationship to positive symptoms. Psychiatry Res. 1999; 87(1): 29-37. [ Links ]
25. O'Leary DS, Flaum M, Kesler ML, Flashman LA, Arndt S, Andreasen NC. Cognitive correlates of the negative, disorganized, and psychotic symptom dimensions of schizophrenia. J Neuropsychiatry Clin Neurosci. 2000; 12(1): 4-15. [ Links ]
26. Docherty AR, Berenbaum H, Kerns JG. Alogia and formal thought disorder: differential patterns of verbal fluency task performance. J Psychiatr Res. 2011; 45(10): 1352-7. [ Links ]
27. Keefe RS, Goldberg TE, Harvey PD, Gold JM, Poe MP, Coughenour L. The Brief Assessment of Cognition in Schizophrenia: reliability, sensitivity, and comparison with a standard neurocognitive battery. Schizophr Res. 2004; 68(2-3): 283-97. [ Links ]
28. Lee MA, Thompson PA, Meltzer HY. Effects of clozapine on cognitive function in schizophrenia. J Clin Psy-chiatry. 1994; 55 Suppl B: 82-7. [ Links ]
29. Meltzer D. Perspective and the measurement of costs and benefits for cost-effectiveness analysis in schizophrenia. J Clin Psychiatry. 1999; 60 Suppl 3: 32-5; discussion 36-7. [ Links ]
30. Blyer CR, Gold J M. Cognitive effects of conventional antipsychotics: another look, in cognitive functioning in schizophrenia: characteristics, correlates, and treatment. Edited by Sharma T, Harvey P. Oxford University Press; 2000. p. 241-65. [ Links ]
31. Harvey PD, Keefe RS. Studies of cognitive change in patients with schizophrenia following novel antipsychotic treatment. Am J Psychiatry. 2001; 158(2): 176-84. [ Links ]
32. Lezak MD, Howieson DB, Loring DW. Neuropsychological assessment. New York: Oxford University Press; 2004. [ Links ]
33. McNamara P, Albert ML. Neuropharmacology of verbal perseveration. Semin Speech Lang. 2004; 25(4): 309-21. [ Links ]
34. Caccappolo-van Vliet E, Miozzo M, Marder K, Stern Y. Where do perseverations come from? Neurocase. 2003; 9(4): 297-307. [ Links ]
35. Sandson J, Albert ML. Varieties of perseveration. Neuropsychologia. 1984; 22(6): 715-32. [ Links ]
36. Cohen L, Dehaene S. Competition between past and present. Assessment and interpretation of verbal perseverations. Brain. 1998; 121(Pt 9): 1641-59. [ Links ]
37. Dalla Barba G, Wong C. Encoding specificity and intrusion in Alzheimer's disease and amnesia. Brain Cogn. 1995; 27(1): 1-16. [ Links ]
38. De Beni R, Palladino P. Intrusion errors in working memory tasks: are they related to reading comprehension ability? Learning and Individual Differences. 2000; 12: 131-43. [ Links ]
39. Mahone EM, Koth CW, Cutting L, Singer HS, Denckla MB. Executive function in fluency and recall measures among children with Tourette syndrome or ADHD. J Int Neuropsychol Soc. 2001; 7(1): 102-11. [ Links ]
40. Shindler AG, Caplan LR, Hier DB. Intrusions and perseverations. Brain Lang. 1984; 23(1): 148-58. [ Links ]
41. Butters N, Wolfe J, Granholm E, Martone M. An assessment of verbal recall,recognition and fluency abilities in patients with Huntington's disease. Cortex. 1986; 22(1): 11-32. [ Links ]
42. Kramer JH, Delis DC, Blusewicz MJ, Brandt J, Ober BA, Strauss M. Verbal memory errors in Alzheimer's and Huntington's dementias. Developmental Neuropsychology. 1988; 4: 1-15. [ Links ]
43. Rouleau I, Imbault H, Laframboise M, Bédard MA. Pattern of intrusions in verbal recall: comparison of Alzheimer's disease, Parkinson's disease, and frontal lobe dementia. Brain Cogn. 2001; 46(1-2): 244-9. [ Links ]
44. Fuld P, Katzman R, Davies P. Intrusions as a sign of Alzheimer dementia: chemical and pathological verification. Ann Neurol. 1982; 11: 155-9. [ Links ]
45. Loewenstein DA, D'Elia L, Guterman A, Eisdorfer C, Wilkie F, LaRue A, et al. The occurrence of different intrusive errors in patients with Alzheimer's disease, multiple cerebral infarctions, and major depression. Brain Cogn. 1991; 16(1): 104-17. [ Links ]
46. Lorscheid T, Thompson SL. Intrusion errors in patients with degenerative or vascular dementia: The cholinergic connection? Dementia. 1991; 1: 202-7. [ Links ]
47. Davis KL, Price CC, Kaplan E, Libon DJ. Error analysis of the nine-word California Verbal Learning Test (CVLT-9) among older adults with and without dementia. Clin Neuropsychol. 2002; 16(1): 81-9. [ Links ]
48. McDowd J, Hoffman L, Rozek E, Lyons KE, Pahwa R, Burns J, et al. Understanding verbal fluency in healthy aging, Alzheimer's disease, and Parkinson's disease. Neuropsychology. 2011; 25(2): 210-25. [ Links ]
49. Hurks PP, Hendriksen JG, Vles JS, Kalff AC, Feron FJ, Kroes M, et al. Verbal fluency over time as a measure of automatic and controlled processing in children with ADHD. Brain Cogn. 2004; 55(3): 535-44. [ Links ]
50. Woods SP, Conover E, Rippeth JD, Carey CL, Gonzalez R, Marcotte TD, et al.; HIV Neurobehavioral Research Center (HNRC) Group. Qualitative aspects of verbal fluency in HIV-associated dementia: a deficit in rule-guided lexical-semantic search processes? Neuropsychologia. 2004; 42(6): 801-9. [ Links ]
51. Lebowitz BK, Shear PK, Steed MA, Strakowski SM. Verbal fluency in mania: relationship to number of manic episodes. Neuropsychiatry Neuropsychol Behav Neurol. 2001; 14(3): 177-82. [ Links ]
52. Christodoulou T, Messinis L, Papathanasopoulos P, Frangou S. Dissociable and common deficits in inhibitory control in schizophrenia and bipolar disorder. Eur Arch Psychiatry Clin Neurosci. 2012; 262(2): 125-30. [ Links ]
53. Fischer-Baum S, Rapp B. Underlying cause(s) of letter perseveration errors. Neuropsychologia. 2012; 50(2): 305-18. [ Links ]
54. Galaverna FS, Morra CA, Bueno AM. Verbal fluency in chronic schizophrenia and severity of psychotic symptoms. Consideration of their relationship with errors in the tasks. Eur. J. Psychiat. 2014; 28(3): 154-64. [ Links ]
55. Andreasen NC. The Scale for the Assessment of Positive Symptoms (SAPS). Spanish version. Iowa City, IA: The University of Iowa; 2000. [ Links ]
56. Schwartz S, Baldo J, Graves RE, Brugger P. Pervasive influence of semantics in letter and category fluency: a multidimensional approach. Brain Lang. 2003; 87(3): 400-11. [ Links ]
57. Goodglas H, Kaplan E, Barresi B. Evaluación de la Afasia y de Trastornos Relacionados. 3ra Edición. Ed. Panamericana. Madrid; 2005. [ Links ]
58. Golden CJ. Stroop Color and Word Test: a Manual for Clinical and Experimental Uses. Chigaco: Skoelting; 1978. [ Links ]
59. Azambuja MJ, Haddad MS, Radanovic M, Barbosa ER, Mansur LL. Semantic, phonologic, and verb fluency in Huntington's disease. Dementia Neur J. 2007; 1(1): 381-5. [ Links ]
60. Rosser A, Hodges JR. Initial letter and semantic category fluency in Alzheimer's disease, Huntington's disease, and progressive supranuclear palsy. J Neurol Neurosurg Psychiatry. 1994; 57(11): 1389-94. [ Links ]
61. Andreasen NC, Arndt S, Swayze V 2nd, Cizadlo T, Flaum M, O'Leary D, et al. Thalamic abnormalities in schi-zophrenia visualized through magnetic resonance image averaging. Science. 1994; 266(5183): 294-8. [ Links ]
62. Henry JD, Phillips LH. Covariates of production and perseveration on tests of phonemic, semantic and alternating fluency in normal aging. Neuropsychol Dev Cogn B Aging Neuropsychol Cogn. 2006; 13(3-4): 529-51. [ Links ]
63. Hori H, Noguchi H, Hashimoto R, Nakabayashi T, Omori M, Takahashi S, et al. Antipsychotic medication and cognitive function in schizophrenia.Schizophr Res. 2006; 86(1-3): 138-46. [ Links ]
64. Elie D, Poirier M, Chianetta J, Durand M, Grégoire C, Grignon S. Cognitive effects of antipsychotic dosage and polypharmacy: a study with the BACS in patients with schizophrenia and schizoaffective disorder. J Psychopharmacol. 2010; 24(7): 1037-44. [ Links ]
65. Knowles EE, David AS, Reichenberg A. Processing speed deficits in schizophrenia: reexamining the evidence. Am J Psychiatry. 2010; 167(7): 828-35. [ Links ]
66. Tandon R, Jibson MD. Safety and tolerability: How do second-generation atypical antipsychotics compare? Current Psychosis & Therapeutics Reports. 2003; 1: 15-21. [ Links ]
67. Tune LE, Strauss ME, Lew MF, Breitlinger E, Coyle JT. Serum levels of anticholinergic drugs and impaired recent memory in chronic schizophrenic patients. Am J Psychiatry. 1982; 139(11): 1460-2. [ Links ]
68. Strauss ME, Reynolds KS, Jayaram G, Tune LE. Effects of anticholinergic medication on memory in schizophrenia. Schizophr Res. 1990; 3(2): 127-9. [ Links ]
69. Saykin AJ, Shtasel DL, Gur RE, Kester DB, Mozley LH, Stafiniak P, Gur RC. Neuropsychological deficits in neuroleptic naive patients with first-episode schizophrenia. Arch Gen Psychiatry. 1994; 51(2): 124-31. [ Links ]
70. Casey DE. The relationship of pharmacology to side effects. Journal of Clinical Psychiatry. 1997; 58: 55-62. [ Links ]
71. Richard IH, Justus AW, Greig NH, Marshall F, Kurlan R. Worsening of motor function and mood in a patient with Parkinson's disease after pharmacologic challenge with oral rivastigmine. Clin Neuropharmacol. 2002; 25(6): 296-9. [ Links ]
72. Venables P. Input dysfunction in schizophrenia. In B. A. Maher Ed. Progress in Experimental Personality Research. Orlando, FL: Academic Press; 1964. p. 1-47. [ Links ]
73. Cromwell RL. (1975). Assessment of schizophrenia. Annual Review of Psychology; 26: 593-619. [ Links ]
74. Chan MW, Yip JT, Lee TM. Differential impairment on measures of attention in patients with paranoid and nonparanoid schizophrenia. J Psychiatr Res. 2004; 38(2): 145-52. [ Links ]
75. Heaton R, Paulsen JS, McAdams LA, Kuck J, Zisook S, Braff D, et al. Neuropsychological deficits in schizophrenics. Relationship to age,chronicity, and dementia. Arch Gen Psychiatry. 1994; 51(6): 469-76. [ Links ]
76. Paulsen JS, Romero R, Chan A, Davis AV, Heaton RK, Jeste DV. Impairment of the semantic network in schizophrenia. Psychiatry Res. 1996; 63: 109-21. [ Links ]
77. Zalewski C, Johnson Selfridge MT, Ohriner S, Zarrella K, Seltzer JC. A review of neuropsychological differences between paranoid and non-paranoid schizophrenia patients. Schizophr Bull. 1998; 24(1): 127-45. [ Links ]
78. Brazo P, Marié RM, Halbecq I, Benali K, Segard L, Delamillieure P, et al. Cognitive patterns in subtypes of schizophrenia. Eur Psychiatry. 2002; 17: 155-62. [ Links ]
![]() Correspondence:
Correspondence:
Laboratory of Neuropsychology
Institute of Translational and Cognitive Neuroscience (INCyT), INECO Foundation, Favaloro University
Buenos Aires, Argentina
National Scientific and Technical Research Council (CONICET)
Buenos Aires, Argentina
Pacheco de Melo 1854, Capital Federal, C1126AAB
Buenos Aires, Argentina
Tel: + 54 11 4812-0010
E-mail: fgalaverna@ineco.org.ar
fgalaverna@psyche.unc.edu.ar
Received: 20 February 2016
Revised: 9 May 2016
Accepted: 8 July 2016