Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Archivos Españoles de Urología (Ed. impresa)
versión impresa ISSN 0004-0614
Arch. Esp. Urol. vol.62 no.2 mar. 2009
High power 980 nm diode laser: preliminary results in the treatment of benign prostatic hyperplasia
Láser de diodo- 980 nm- de alta potencia: resultados preliminares en el tratamiento de la hiperplasia benigna de próstata
Luis Miguel Clemente Ramos
Urology Department. CEMTRO Clinic. Madrid. Spain.
SUMMARY
Objectives: A clinical evaluation of the use of a 980 nm diode laser in the treatment of bladder outlet obstruction secondary to benign prostatic hyperplasia (BPH), focused on perioperatory morbidity and results in a short-term follow-up.
Methods: Fifteen patients were included in the study. All of them were evaluated by IPSS and Quality of Life (QoL) questionnaires, digital rectal examination, PSA, ultrasound scan and uroflowmetry. Prostate vaporization was performed with a laser of diode at 980 nm (Intermedic; Barcelona, Spain) using a 600 microns side-fire fiber. In the follow-up any event was recorded, as well as the IPSS and QoL scores and Qmax.
Results: Mean age of the patients was 66.7 years(45-75). The range of prostate volume was 20-76 cc (median 41.3 cc). Mean delivered energy was 161,012 kJ (78,3-243). No patient showed either a significant hematic loss or fluid absorption syndrome. A 22F urethral three-way catheter was inserted and removed between 12-40 hours in the postoperatory period. After a mean follow-up of 5,5 months (2-9) the average IPSS and QOL questionnaires scores changed, respectively, from 22,4 (19-26) and from 3 (2 -4) to an average of 6,8 (1 - 13) (p<0,01) and 1,4 (0 - 3), respectively, at the end of follow-up (p <0,01). Qmax increased from 6,4 ml/s (5-11,9) baseline to 19,7 ml/s (13,9-24 (p <0,01). No patient showed urinary incontinence. Retreatment was not nee-ded though three patients needed a short-time catheterization (24 hours) after developing acute urinary retention in the first 48h hours.
Conclusions: Our preliminary results suggest that prostate vaporization using 980 nm diode laser with output power up to 120 W, is effective and associated to minimal morbidity.
Key words: Diode laser. 980 nm. Benign prostatic hyperplasia.
RESUMEN
Objetivo: Evaluar clínicamente la utilización de un láser de diodo de 980 nm en el tratamiento de la uropatía obstructiva infravesical secundaria a hiperplasia benigna de próstata (HBP), poniendo énfasis en la morbilidad perioperatoria y los resultados en un seguimiento a corto plazo.
Métodos: Quince pacientes fueron incluidos en el estudio. Todos fueron evaluados mediante los cuestionarios IPSS y de calidad de vida (CV), tacto rectal, PSA, ecografía y flujometría. Se procedió a la vaporización prostática con un láser de diodo de 980 nm (120 W; Intermedic; Barcelona, España) utilizando una fibra de disparo lateral de 600 micras. En el seguimiento se recogió cualquier incidencia, así como la puntuación en los cuestionarios IPSS y CV así como en el pico de flujo máximo.
Resultados: La edad media de los pacientes fue de 66,7 años (45-75). El rango del volumen prostático fue 20-76 cc (media 41,3 cc). La media de energía utilizada fue de 161,012 kJ (78,3-243). Ningún paciente presentó una pérdida hemática significativa ni síndrome de absorción líquida. En todos los casos se colocó un catéter uretral 22F que se retiró entre las 12-40 horas postoperatorias. Tras un seguimiento medio de 5,5 meses (2-9), la puntuación media en el cuestionario IPSS y en el de CV variaron, respectivamente, de una media de 22,4 (19-26) y de 3 (2-4) previa a la intervención, hasta una media de 6,8 (1-13) (p<0,01) en el cuestionario IPSS y de 1,4 (0-3) en el de CV al final del seguimiento (p<0,01). De igual modo, el flujo máximo se incrementó de 6,4 ml/s (5-11,9) en el preoperatorio a 19,7 ml/s (13,9-24) en el postoperatorio (p<0,01). Ningún paciente presenta incontinencia. No se ha requerido la repetición del procedimiento, si bien tres pacientes precisaron un sondaje transitorio en las primeras 48h (dos de los pacientes eran portadores de sonda vesical antes del tratamiento).
Conclusiones: Nuestros resultados preliminares sugieren que la vaporización prostática con láser de diodo de 980 nm utilizando potencias de hasta 120 W es efectiva y asociada a escasa morbilidad.
Palabras clave: Laser diodo. 980 nm. Hiperplasia benigna de próstata.
Introduction
The transurethral resection of the prostate (TURP) is considered to be the gold standard of care in the treatment of the benign prostatic hyperplasia (BPH) (1). The use of different lasers has been proposed in an attempt to diminish the morbidity of the TURP. Nd: YAG (Neodymium:yttrium-aluminum-garnett) laser was introduced in 1992 as a treatment for bladder outlet obstruction (BOO) secondary to benign prostatic hyperplasia (BPH). The side effects of this therapy included long-term irritative symptoms, long catheterization time, a high rate of reintervention and lower clinical results than those obtained by means of TURP (2). KTP laser provides a significant improvement in symptomatic and urodynamic outcomes and a low postoperatory morbidity, but it is a time -consuming procedure and its high cost associated has limited its widespread use (3,4).
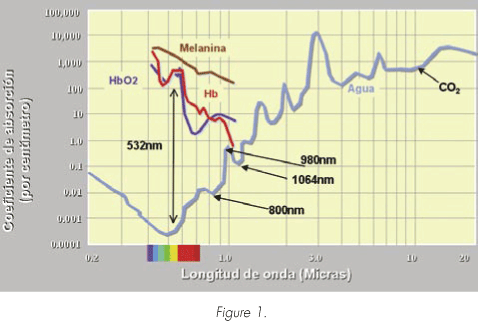
A study has been published recently addressing the usefulness of diode laser for the treatment of the BPH. Wavelengths of 1470 nm (5) and 980 nm (6) have been tried, respectively, though the latter offers, simultaneously, an excellent absorption both for water and for hemoglobin, which allows obtaining a great capacity of vaporization in a haemostatic environment (Figure 1). Nevertheless, to date no clinical study regarding prostate vaporization with 980 nm wavelength is available.
The aim of this study is to clinically evaluate the usefulness of the high power 980 nm diode laser in the treatment of the BPH.
Material and methods
Between November 2007 and June 2008, we treated fifteen patients diagnosed of BOO secondary to BPH. In all cases pharmacological treatment had been tried, with minimal or null response. Patients were evaluated by means of anamnesis (the symptoms being evaluated through the International Prostate Symptom Scores -IPSS- and a quality of life -QoL- score), physical examination including digital rectal examination (DRE), PSA, abdominal ultrasound scan (transrectal was performed just in case of disagreement between DRE and the abdominal ultrasound scan) and uroflowmetry (peak maximum flox-Qmax). Inclusion criteria were moderate to severe urinary symptoms, as determined by IPSS (score>8) and Q max of less than 15 ml/s with or without postvoided residual volume (PVR). Exclusion criteria were urethral stricture, previous prostatic surgery, prostate cancer and obvious manifested neurogenic bladder dysfunction.
Prostate vaporization was carried out by a diode laser at 980 nm (Multidiode Surgical, Intermedic, Barcelona, Spain) delivering 120 W of maximum output power with a 600 nm side-fire fiber endowed with a spot of 1 mm of diameter. In all cases saline solution was used as irrigation through a 23F cystoscope.
The procedure started at the bladder neck; the laser beam was moved towards the apical region, vaporizing the tissue when passing, using the contact technique as well as the non-contact technique depending on the characteristics of the tissue and deterioration of the fiber. The maneuver was repeated on both lobes in a TUR manner from 6 to 12 o'clock position, obtaining a TURP-like cavity. In all cases a 22F three-way catheter was placed in spite of obtaining clear urine or minimal haematuria. Once we verified that the patient voided spontaneously, he was discharged from the hospital.
The procedure was carried out in all cases under spinal anesthesia. The antibiotic prophylaxis consisted of only one dose of 100 mg of tobramicina IV. Any antiplatelet medication was discontinued 5 days before the procedure; heparin of low molecular weight was required in two patients with associated comorbidity.
During the follow-up, any clinical event and adverse effects was collected, as well as accomplishment of IPSS and QoL questionnaires, Qmax and PVR. The Mann-Whitney U test was used to determine the statistical significance.
Results
Mean age of the patients was 66,7 years old (45-75). Prostate volume ranged from 25 to 76 ml with a mean volume of 42 cc. All patients had a moderate to-severe prostatism (the mean baseline score in the IPSS questionnaire was 22, 4 (19-26) and in the QOL was 3 (2-4), respectively. The mean Qmax was 6, 4 ml/s (5-11, 9).
The output power changed from 80 W in continuous way at the beginning of the procedure in order to avoid the premature damage of the fiber, up to 120 W during the rest of the surgery. The fiber behaves in a similar way at a distance of 1 mm or in contact with the tissue, though in the latter circumstance its damage increases.
At the beginning of the series, a complementary resection of a small lobe by means of electrocautery was done in two cases, though after having profusely applied the laser on it, leaving a practically bloodless operative field.
Complementary resection of a small lobe by electrocautery was performed in two cases at the beginning of the series, although we profusely applied the laser on it, leaving therefore a practically bloodless operative field. In another case the photocoagulation of a superficial bladder tumor was carried out simultaneously (stage PaG1 UICC in the biopsy previously taken during preoperatory endoscopy) using a power of 20W.
Even having obtained clear urine at the end of the procedure, a prophylactic bladder irrigation was scheduled for 4-5h, proceeding in all cases to take the foley out in less than 24 hours except in a case because of the gland size, though this decision was taken again at the beginning of the series.
No transfusion was needed and there was no case of fluid absorption syndrome. In 6 of 14 cases (42,8 %) the patients referred moderated dysuria, which only needed symptomatic treatment on demand and disappeared in all cases within the 2 following weeks.
A minimal transient haematuria was seen in 8 cases (57,2 %), but it solved spontaneously in the following 4-5 days. One case with significant hematuria was observed ten days later after the procedure; the patient needed anticoagulation treatment with low mollecular weight heparine because of cardiological pathology, requiring the placement of standard foley catheter, being removed in the office 24 hours later.
In two cases an episode of acute urinary retention occurred 72 hours after the procedure; 12 hours later the foley was taken out without any incident.
Most patients reported to void a small quantity of sloughed tissue during the first 5-7 days postoperative without clinical significance. No episodes of urinary infection nor urethral stenosis have been recorded.
The mean follow-up was 5, 5 months (2-9). The mean Q max was 19,7 ml/s (13,9-24) (p <0,01), whereas the mean score of IPPS and QOL questionnaires were 6,8 (1-13) (p <0,01) and 1,4 (0-3) (p <0,01), respectively.
Discussion
Though the TUR of prostate is considered to be the golden standard of care in the treatment of BPH (1), its perioperatory morbidity (hemorrhage, urethral stenosis, reabsorption syndrome, and catheterization times) has encouraged the search of alternatives which can reduce it and offer at least similar clinical results. For the last few years, different types of laser and different wavelengths have been proposed as candidates to be considered real alternative to the TUR.
Nd: YAG laser
(1064 nm wavelength) has a low coefficient of absorption in the tissue and achieves a deep tissue penetration; it produces a necrosis by deferred coagulation, without appreciating immediate ablative effects (2). It has ben given up in the treatment of the BPH due to Its morbidity and low efficiency.
Holmium: YAG laser
(2140 nm wavelength) has a high absorption in prostatic tissue, which carries a high density of energy and a minimal depth penetration, allowing the vaporization of the tissue. It has been used in the treatment of the BPH either by vaporizing the tissue (HoLap) or by performing an split of the adenoma and carry out the enucleation of the gland (HoLep) (7,8). The first procedure needs a lot of time to be carried out and for the second one is necessary a long learning curve, facts that have limited the widespread of both techniques.
The KTP laser
(532 nm wavelength) allows a good hemostasy due to the high affinity for the hemoglobin as well as the prostate vaporization; on the contrary, the water absorption is minimal and this circumstance causes the procedure to be also slow (Table I). Nevertheless, given that the technique needs a minor learning curve, its low morbidity and the published good medium-term results, have spred its use (3,4,9-15). On the contrary, the costs and the long time needed to vaporize a suitable quantity of tissue, the reason why some authors consider it only for glands of small size, have restricted its application.
Seitz et al. (5) have reported the preliminary data of a study based on the utilization of a diode laser of 1470 nm at 50 W of power, obtaining some promising results in patients with BPH. However, the combination of a good absorption both for water and for hemoglobin make the laser of diode at 980 nm a more attractive option in the treatment of the BPH by means of vaporization of the prostate tissue (Table I).
Guazzoni et al. (16) published in 1996 the use of the diode laser at 980 nm in the treatment of the BPH (VLAP modality), though only a decade later new contributions with this energy source have been collected. In an ex vivo study, the diode laser of 980 nm used at 120 W of power showed a capacity of ablation clearly superior (almost double) to the one obtained with the laser KTP of 80 W (17).
Unlike other lasers, the speed of vaporization with the diode laser at 980 nm does not seem to depend on whether the tissue is mucosa or fibromuscular stroma. Regarding its hemostatic properties, it is considered to be equivalent to KTP. Using 120 W of output power, the depth of the coagulation was similar to that obtained by monopolar RTU (6). A recent contribution comparing the results after 6 months between a group treated with KTP laser 120 W and another one with diode laser of 200 W, can barely find differences between both therapies, though the group treated with diode shows a slightly more intense dysuria than the group treated with KTP (18).
Prostate vaporization with diode laser basically shares the same principles stated for laser KTP (15, 19). The cystoscope fiber and the stages of the procedure are identical, and a side-fire fiber is also used in a similar fashion.
It should only be pointed out that when a minor performance of the fiber is noticed, it is possible to use it in the contact way to get an improvement of the vaporization, though this way of proceeding may increase the damage of the fiber. Even if it seems that the speed of vaporization and the depth of the zone of coagulation is similar in the pulsed mode and in the continuous mode of the 980 nm diode laser, the bleeding is practically absent in both modalities, though in the continuous mode seems to be even lower.
The median lobe generally slows down the process of vaporization and accelerates the deterioration of the fiber; half incision of the lobe and to proceed later to the vaporization on both sides seems the most reasonable way of handling this circumstance. The most reasonable way of handling this circumstance could be to perform half incision of the lobe in the first place, and vaporization on both sides later on.
To date, no clinical studies with 980 nm laser were available. The results that we have obtained are satisfactory both the symptomatic improvement -IIEF and QoL scores- and the urodynamic parameters (Qmx), while reporting a low intra-perioperatory morbidity. The diodes that produce the light emission are smaller, more efficient and possibly cheaper than other types of laser (20). In addition, the easy managing and installation of the device (its weight is lower than 30 Kg, includes refrigeration in the same module and only needs an ordinary electrical socket) make it attractive to the urological community.
Nevertheless, long term studies need to be carried out to confirm the favorable short-term results reported in this study.
 Correspondence:
Correspondence:
Luis Miguel Clemente Ramos
Unidad Urología
Clínica CEMTRO
Avda. Ventisquero de la Condesa, 42.
28035 Madrid. (Spain).
urologia@clinicacemtro.com
Accepted for publication:29th September, 2008.
References and recomended readings (*of special interest, **of outstanding interest)
1. Madersbacher S, Alivizatos G, Nordling J et al. EAU 2004 guidelines on assesment, therapy and follow-up of men with lower urinary tract symptoms suggestive of benign prostatic obstruction (BPH guidelines). Eur Urol 2004;46:547-54. [ Links ]
2. Costello AJ, Bosher WG, Bolton DM et al. Laser ablation of the prostate in patients with benign prostatic hypertrophy. Br J Urol 1992:69:603-8. [ Links ]
*3. Reich O, Bachmann A, Siebels M et al. High power (80w) potassium-titanyl-phosphate laser vaporization of the prostate in 66 high risk patients. J Urol 2005;173:158-60 [ Links ]
*4. Te AE, Malloy TR, Stein BS et al. Photoselective vaporization of the prostate for the treatment of benign prostatic hyperplasia:12 months results from the first United States multicenter prospective trial. J Urol 2004; 172:1404-08. [ Links ]
**5. Seitz M, Sroka R, Gratzke C et al. The Diode Laser: A novel side-findding approach for Láser vaporisation of the human prostate-Inmediate efficacy and 1 -year follow up. Eur Urol 2007; 52:1717-22. [ Links ]
**6. Wendt-Nordahl G, Huckele S, Honeck P et al. 980 nm diode laser: a novel laser technology for vaporization of the prostate. Eur Urol 2007; 52:172328. [ Links ]
7. Elzayat EA, Habib E, Elhilali MM. Holmium láser enucleation of the prostate: a size-independent new "gold standard". Urology 2005; 66: 108-13. [ Links ]
*8. Gilling PJ, Aho TF, Frampton CM et al. Holmium laser enucleation of the prostate: results at 6 years. Eur Urol 2008; 53: 744-9. [ Links ]
9. Sarica K, Alkan E, Luleci H et al. Photoselective vaporization of the enlarged prostate with KTP laser: long term results in 240 patients. J Endourol 2005;19:1199-202 [ Links ]
10. Volkan T, Ihsan TA, Yilmaz O et al.Short term outcomes of high power (80W) potassium.titanyl-phosphate laser aporization of the prostate.Eur Urol 2005;48:608-13 [ Links ]
11. Sulser T, Reich O, Wyler S. Photoselective KTP laser vaporization of the prostate: first experiences with 65 procedures. J Endourol 2004;18:976-81 [ Links ]
12. Malek RS. GreenLight HPS Láser therapy for BPH: Clinical outcomes and surgical recommendations from the international GreenLight user group (IGLU). Eur Urol Suppl; 2008:7:361-362 [ Links ]
13. Woo H, Reich O, Bachmann A et al. Outcome of Greenlight 120-W Laser therapy in specific patient population: those in retention, on anticoagulants, and with large prostates (>80 ml). Eur Urol Suuppl, 2008; 7: 378-383 [ Links ]
14. Choi B, Tabatabaei S, Bachmann A. Geernlight HPS 120-W Laser for Benign Prostatic Hyperplasia: Comparative complications and technical recommendations. Eur Urol Suppl 2008; 7:384-392 [ Links ]
15. Cecchetti W, Guazzeri S, Tasca A et al. 980 nm diode laser and fiber optic resectoscope in endo-urological surgery. European Biomedical Optics Week, BiOS Europe '96. [ Links ]
*16. Seitz M, Ackerman A, Gratzke C.Diode Laser:ex vivo studies on vaporization and coagulation characteristics. Urologe A 2007;46: 1242-1247. [ Links ]
**17. Ruszat R. Prospective single-centre comparison of 120 watt photo selective vaporization of the prostate and 200 watt high-intensive diode laser ablation of the prostate. Eur Urol Suppl 2008; 7 (3): 203. [ Links ]
18. Barber NJ,Muir GH. High power KTP laser prostatectomy: the new challenge to transurethral resection of the prostate. Curr Opin Urol 2004; 14:21-5. [ Links ]
19. Grasso M y Green AD. Lasers in Urology. eMedicine eMedicine Clinical Reference, Updated Continually. [ Links ]











 texto en
texto en