Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Archivos Españoles de Urología (Ed. impresa)
versión impresa ISSN 0004-0614
Arch. Esp. Urol. vol.62 no.3 abr. 2009
Correlation between symptoms and survival in patients with renal cell carcinoma
Correlación de los síntomas de los pacientes con cáncer de células renales con la supervivencia
Yolanda Ares Valdés
Department of Urology. Manuel Fajardo. University Hospital. Havana. Cuba.
SUMMARY
Objectives: To evaluate the correlation between type of presentation in patients with renal cell carcinoma and survival.
Methods: Longitudinal retrospective study of 42 patients with clinical and histological diagnosis of renal cell carcinoma (RCC) between July 2002 and September 2007 at University Hospital Manuel Fajardo. The following variables were studied: Sex, age, clinical presentation: 1) asymptomatic: 2) symptomatic: 3) paraneoplastic syndrome; tumor stage (TNM 1997) and survival.
Results: There is a predominance of men over women, the age of greater incidence was between the fifth a and seventh decades. The tumors were classified as: asymptomatic 7%, 3/42; symptomatic 67%, 28/42, with flank pain 31%, 13/42; with hematuria 24%, 10/42, and tumor 10%, 4/42, the classic triad of hematuria, flank pain and mass was 2.3%, 1/42 of the patients and paraneoplastic syndrome 24%, 11/42. The patients with non-metastatic disease were 57%, 24/42 and 43%, 18/42 presented metastases. Five-year survival for patients with RCC by TNM stage was T1, 100% (12/12), T2, 97% (11/12), T3, 36% (4/11), T4, 0% (0/7). The survival of localized and metastatic RCC was 95%, 23/24 and 22%, 4/18 cases respectively and all stage was 64% (27/42).
Conclusions: The asymptomatic RCCs were smaller; pain, hematuria, and mass were the most common manifestations in symptomatic RCC. The prognosis is dismal in patients with RCC showing paraneoplastic syndromes.
Key words: Renal cell carcinoma. Asymptomatic. Paraneoplastic syndrome. Survival.
RESUMEN
Objetivo: Analizar la correlación existente entre los síntomas de los pacientes con Carcinoma de Células Renales y la supervivencia.
Método: se realizó un estudio retrospectivo longitudinal de 42 pacientes con diagnóstico clínico e histológico de carcinoma de células renales tratados durante el período comprendido entre julio del 2002 a septiembre 2007 en el hospital Universitario Manuel Fajardo. Se analizaron las variables de: sexo, edad, forma de presentación de la enfermedad (asintomática, sintomática y síndrome paraneoplásico), estadio tumoral de la clasificación de TNM y sobrevida.
Resultados: El hallazgo asintomático se presentó en el 7%, 3/42 de los casos y se manifestaron por síntomas el 67%, 28/42, el dolor en el 31%, 13/42, la hematuria en el 24%, 10/42, el tumor en el 10%, 4/42, la tríada clásica (dolor, tumor y hematuria) en el 2.3%, 1/42 de los pacientes. El resto de los enfermos el 24%, 11/42 acudieron por síndrome paraneoplásico. El 57%, 24/42 al momento del diagnóstico no tenían metástasis y el 43%, 18/42 con enfermedad metastásica. La supervivencia para los estadios no metastásicos fue del 95%, 23/42 y para el metastásico del 22%, 4/18.
Conclusiones: El diagnóstico de carcinoma de células renales asintomático fue muy pobre, la presentación más frecuente fue el dolor, la hematuria y la masa palpable y representa la mayoría de las veces enfermedad avanzada. Los pacientes con síndrome paraneoplásicos tienen grave pronóstico con una baja supervivencia.
Palabras clave: Carcinoma de Células Renales. Asintomático. Síndrome paraneoplásico. Supervivencia.
Introduction
Renal cell carcinoma (RCC) represents 3% of all cancers, is de most lethal of urologic cancer, more than 40% of patients with RCC have died of cancer progression (1).
Many renal mass remain asymptomatic and non-palpable until late in the natural course of the disease. Advances in imaging technology and the increased application of radiological modalities such as ultrasonography (US) and computed tomography (CT) for health screening and evaluation of other conditions, particularly intra-abdominal pathologies, have led to an increased number of early RCC being diagnosed incidentally in developed countries. Between of 25% to 40% of RCCs are detected incidentally using non-invasive imaging's (2, 3).
The symptoms associated with RCC can be due local tumor growth, hemorrhage, paraneoplastic syndromes, or metastatic disease. The classic triad of flank pain, gross hematuria and palpable mass is now rarely found, and denotes advanced disease, and some refer to it is the "too late triad" is found in 11% of the patients. Before the advent of US and CT scanning, most patients with RCC present with one or more of these signs or symptoms and many were incurable, approximately one-third of patients will have metastatic disease at presentation, and 40% of cases treated for localized disease have a recurrence (4, 5). Paraneoplastic syndromes are found in 20% of patients with symptoms RCC, hypertension, cachexia, weight loss, anemia, abnormal liver function, hypercalcemia, and policythemia (6). In fact, RCC was previously referred to as the internist tumors because of predominance of systemic rather than local manifestations.
In 1958, Flocks and Kadesky (7) developed the first staging system for renal carcinoma. The tumors were staged according to the extent of spread found at operation and by histological examination of the tissues removed. Both surgical and pathologic stages were based on the gross physical characteristics of the tumor, and this schema is still embedded in the mindset of most urologists. Various studies have shown a strong correlation between pathologic stage and 5-years survival rates for RCC.
The treatment of choice for non-disseminated renal cell cancer is surgery. Metastatic RCC poses a therapeutic challenge due to its resistance to conventional modes of therapy such as chemo and radiotherapy. The immunotherapy can be considered standard therapy in treatment of metastatic RCC. The 5-year survival rates is around 60 to 75% is the early stages. If it has spread to the lymph nodes, 5-year survival is 5 to 15%. And has spread to other organs the probable outcome is poor, with 5- year survival at less than 5% (8). All this motivate to us to make this study with the objective to determine the correlation between symptoms for patients with renal cell carcinoma and survival.
Objetives
General
• To evaluate the correlation between mode presentation for patients with renal cell carcinoma and survival.
Specific
To evaluate the correlation:
• Clinical presentation.
• Stage of the disease.
• Survival.
Materials and methods
Longitudinal retrospective review was analyzed between July 2002 and September 2007 at University Hospital Manuel Fajardo. The cancer registry registered 52 patients with the diagnosis of RCC. 42 cases with complete records were including.
Inclusion criteria:
Patients with clinical and histological diagnosis of RCC, classified by TNM-system of both sexes, ages to 18 years, adequate renal function.
Exclusion criteria:
History of other prior malignancy in the past 5 years or other chronic diseases, patients with central nervous system metastases, prior anticancer therapy, not recovered from prior surgery and/or surgery or radiation therapy, inmunocompromised including (HIV, hepatitis B or C), active infection, unstable angina or myocardial infarction, pregnant.
Study conduction:
42 patients with RCC were classified into there symptomatic grades according to the circumstance of discovery: 1) incidental: the patients without symptoms whose tumor was incidentally discovered, 2) symptomatic: the patients present symptoms related to renal tumor (hematuria, palpable mass or back pain) 3) paraneoplastic syndrome; patients whose tumors were associated with (alteration of general state or symptomatic metastasis). The mean follow-up was 60 months, pathological TNM stage of the primary tumor presence of distant metastases and survival were analyzed. In the first years; clinical visits every 3 months, of 2 to 5 years every 6 months and more than 5 years were made visits of annual. It was made chest X-ray, ultrasound hemograma and creatinina. In the patients with disease progression was precise to make abdominal CT and bone gammagrafia.
The following variables were studied:
• Sex
• Age
• Clinical presentation
• Tumor stage (TNM 1997)
• Survival.
The data were entered a computation program and the statistical analysis was made by means of the Test of Chi-square.
Results
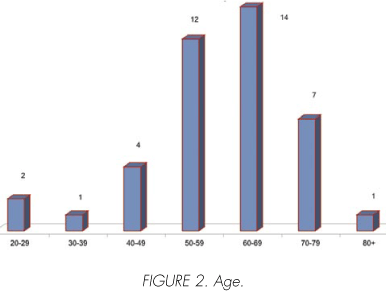
We reviewed the records of 42 with RCC. Of this 28/42, 67% masculine and 14/42, 33% feminine, the age of greater incidence was between the fifth a and seventh decades with a peak in the sixth 14/42, 33% (Figures 1 and 2).
The clinical manifestations were: Asymptomatic 7%, 3/42; symptomatic 67%, 28/42, with flank pain 31%, 13/42; with hematuria 24%, 10/42, and tumor 10%, 4/42, the classic triad of hematuria, flank pain and mass was 2.3%, 1/42 of the patients, and paraneoplastic syndrome 24%, 11/42. The most common of these are: weight loss with anemia and cachexia (Figure 3).
The patients with non-metastatic disease were 57%, 24/42 and 43%, 18/42 with metastases. (Table I).
Five-year survival for patients with RCC by TNM stage was T1, 100% (12/12), T2, 97% (11/12), T3, 36% (4/11), T4, 0% (0/7) (Figure 4). The survival of localized and metastatic RCC was 95%, 23/24 and 22%, 4/18 cases respectively and all stage was 64% (27/42) (Table II).
Discussion
Incidental detection of RCC has increased significantly in recent years because of use of abdominal imaging. The primary factor that limits the widespread implementation of screening for RCC is the relatively low incidence of RCC in the general population 9, 10. Screening for those target population at high risk for RCC may be beneficial. These include patients with end-stage renal disease, von Hipper-Lindau disease, and patients with other familiar syndromes such hereditary papillary renal cancer, tubular sclerosis, and autosomal dominant polycystic kidney disease.
The US should be considered the primary method of detection of RCC (11). In Cuban where abdominal US is not performed routinely during health examinations, and a large number of patients with RCC are still diagnosed due to clinical symptoms, such as palpable mass and hematuria, paraneoplastic and metastatic symptoms.
The presence of clinical signs and symptoms in RCC patients has long been accepted as a prognosticator of poor outcome. Weight loss and decreased performance status suggest a negative impact of tumor on a patients overall health and decrease in the ability to tolerate aggressive therapies. Similarly, other findings on physical examination denote a poorer prognosis. Presence of a palpable mass correlates with tumor size and locally advanced disease, and lower extremity edema and varicocele suggest venous involvement.
The sex, age and race are factors with no independent prognostic value. Patients with incidentally diagnosed RCC, who have a disease presentation without symptoms, generally have smaller tumors, less advanced stage and better survival. The paraneoplastic syndromes are usually associated with high tumor stage (6, 12). Clinical stage, which demonstrates the anatomical extent of the malignancy, is still the most important and powerful prognostic factor. The role of tumors size in the clinical outcome seems to be stage-dependent. Also, small tumors < 3 cm have local tumor invasion and are diagnosed with metastatic disease (13).
In 2002, the American Joint Committee on Cancer proposed a revision of the TNM systems that is now the recommend staging system for RCC-takes into account tumor size, extent of local invasion, lymph node and adrenal involvement and distant metastatic (14). Partard and colleagues (15) have shown that mode of presentation (incidental or symptomatic) can be combined with tumors size to better stratitify patients after primary surgical management.
However, when compared between T1N0M0 and T2N0M0 tumors only, there no significant differences in survival. The 5-year survival, and in patients with lymph node or systemic metastatic portend a particularly poor prognostic for RCC.
The variable natural history of RCC highlights the need for prognostic factors used to predict outcome for an individual patient. The development of a reliable prognostic model can help in specific treatment strategies and follow-up strategies, and can provide patient with valuable information. New agents for metastatic disease are oral multi tyrosine kinase inhibitors, sunitinib and sorafenib. Sunitinib has been reported to extend progression-free survival with better quality of life than cytokine therapy and is recommended in Europe as first line therapy for metastatic disease (16).
RCC continues to be a devastating cancer, which currently has few effective treatment options. The significant advances in the diagnosis, staging and treatment of patients with RCC, recurrence rates following surgical resection of locally aggressive tumors remain high, the concept the adjuvant therapy has been proposed. Unfortunately, the incidence of RCC is gradually increasing, and despite a trend toward earlier detection, mortality rates remain high At present, no systemic agent has been proven to be uniformly effective in the management of metastatic or locally advanced renal cell carcinoma. In the future, integrating prognostic systems with both clinical and molecular markers will enhance the ability to predict the tumors behaviour of an individual patient.
Conclusions
The asymptomatic RCCs were smaller; pain, hematuria, and mass were the most common manifestations in symptom RCC. The prognosis is dismal in patients with showing paraneoplastic syndromes.
 Correspondence:
Correspondence:
Yolanda Ares Valdés
Indio 113 / Gloria y Corrales
Habana Vieja. Ciudad Habana. (Cuba).
ares@infomed.sld.cu
Accepted for publication: February, 2nd 2008.
References and recomended readings (*of special interest, **of outstanding interest)
**1. Ares VY, Campo AR. Factores pronósticos de la supervivencia en los pacientes intervenidos por cáncer de células renales. Arch Cir Gen Dig, Disponible en: http://www.cirugest.com/revista/2007/07/2007-05-07.htm, 2007 [ Links ]
2. Volpe A, Jewett MA. The natural history of small renal masses. Nat Clin Pract Urol 2005;2(8):384. [ Links ]
*3. Ares VY, Fragas VR. Carcinoma de células renales Incidental. Arch Esp Urol 2005; 58:417. [ Links ]
4. Luciani LG, Cestari R, Tallarigo C. Incidental renal cell carcinoma-age and stage characterization and clinical implications: study of 1,092 patients (1982-1997). Urol, 2000; 56:58. [ Links ]
**5. Jacobsohn KM, Wood CG. Adjuvant therapy for renal cell carcinoma. Semin Oncol 2006; 33:576. [ Links ]
6. Gold PJ, Fefier A, Thompson TA. Paraneoplastic manifestations of renal cell carcinoma. Semin Urol Oncol, 1996; 4:216. [ Links ]
7. Flocks RH, Kadesky MC. Malignant neoplasms of the kidney: An analysis of 353 patients followed five years or more. J Urol, 1958; 79:196. [ Links ]
**8. Mickisch GH, Mattes RH. Combination of surgery and immunotherapy in metastatic renal cell carcinoma. World J Urol , 2005; 23:191. [ Links ]
**9. Malaeb BS, Martin DJ, Littooy FN, el al. The utility of screening renal carcinoma in an elderly asymptomatic population. BJU Int, 2005; 95:977. [ Links ]
10. Jayson M, Sanders H. Increased incidence of serendipitously discovered renal cell carcinoma. Urol, 1998; 51:203. [ Links ]
11. Motzer RJ, Barder RH, Nancis DM. Renal cell carcinoma. N Engl J Med, 1996; 335:865. [ Links ]
12. Laski ME, Vugrin D. Paraneoplastic syndromes in hypenephroma. Semin Nephro, 1989; 7:123. [ Links ]
*13. Bell ET. A classification of renal tumours with observation on the frequency of various types. J Urol 1938; 39:238. [ Links ]
*14. Leibovich BC, Pantuck AJ, Bui MHT, et al. Current staging of renal cell carcinoma. Urol Clin N Am 2003; 30:481. [ Links ]
**15. Patard JL, Shvarts O, Lam JS, et al. Safecty and efficacy of partial nephrectomy for all T1 tumors based an international multicenter experience. J Urol 2004; 171:2181. [ Links ]
*16. Robert J, Motzer, Thormas E, et al. Sunitinib versus interferon alfa in metastatic renal-cell carcinoma. N Engl J Med, 2007; 356:115. [ Links ]











 texto en
texto en