Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Archivos Españoles de Urología (Ed. impresa)
versión impresa ISSN 0004-0614
Arch. Esp. Urol. vol.62 no.5 jun. 2009
NEUROLOGIC AND URODINAMIC UROLOGY
Third generation sub-mid urethral mesh: Experience with 110 TVT-Secur
Malla sub-medio uretral de tercera generación: Experiencia con 110 TVT-Secur
Vicente Sola, Paolo Ricci1 and Jack Pardo.
Uroginecology and Vaginal Surgery Unit. Obstetric and Gynecology Department. Clínica Las Condes. Chile.
SUMMARY
Objectives: To review the effectiveness and security of the TVT-Secur system in the surgical treatment of stress urinary incontinence (SUI).
Methods: Prospective analysis of 110 patients undergoing SUI surgical treatment in the Urogynecology and Vaginal Surgery Unit of Clínica Las Condes, between January 2007 and May 2008. The patients must have stress urinary incontinence over one year or more. They must not have history of a previous surgery for urinary incontinence or prolapse. They must not have mixed urinary incontinence or urge incontinence, only SUI demonstrated by clinical symptoms and non-multichannel urodynamic study.
Results: Mean surgical time was 8 minutes (6 to 16 mi-nutes). The observational period was between 2 months (4 cases) and 19 months, mean 8 months. During the intraoperative time 2 cases of bladder perforation were registered. In the immediate postoperative time 2 cases of obstruction were observed. In 97 (88,2%) of the 110 patients some concomitant gynecological surgery was performed. In 105 (95,5%) of the 110 cases cure of the SUI was registered. In 4 (3,6%) cases improvement was observed and 1 (0,9%) case was a failure. In 2 (1,8%) patients de novo urge incontinence was registered.
Conclusions: The TVT-Secur system corresponds to a third generation tape effective and safe in the surgical treatment of stress urinary incontinence. This technique has potential advantages when compared with the preceding operations. Only the long time follow-up and incorporation of new patients will allow to determine the permanence of these good results in the time.
Key words: Stress urinary incontinence (SUI). Tension-free vaginal tape (TVT-Secur). Sub-mid urethral tape.
RESUMEN
Objetivo: Revisar la eficacia y seguridad del sistema TVT-Secur en el tratamiento quirúrgico de la incontinencia de orina de esfuerzo.
Método: Análisis prospectivo de 110 mujeres ingresadas a la Unidad de Uroginecología y Cirugía Vaginal, de Clínica Las Condes, para corrección de la incontinencia de orina de esfuerzo, entre enero del 2007 y mayo del 2008. Debían tener incontinencia de orina por al menos un año y de carácter permanente. No debían tener antecedente de alguna cirugía para corrección de la incontinencia de orina de esfuerzo ni prolapso genital. No debían tener incontinencia mixta, ni urgeincontinencia, sólo incontinencia de orina de esfuerzo clínica y objetivada por urodinamia monocanal.
Resultado: El tiempo operatorio del TVT-Secur fluctuó entre 6 y 16 minutos, media de 8 minutos. Se completó un período de observación entre 2 meses (4 casos) y 19 meses, con una media de 8 meses. Durante el período intraoperatorio se registraron 2 casos de perforación vesical. En el postoperatorio se reajustaron 2 cintas por subobstrucción, detectadas por síntomas y residuos post-miccionales vesicales altos. En 97 (88,2%) de las 110 pacientes se realizó concomitantemente alguna cirugía ginecológica. En 105 (95,5%) de los 110 casos se registró cura de la IOE, que se mantuvo durante el período de observación. En 4 (3,6%) casos se observó mejoría y en 1 (0,9%) falla. En 2 (1,8%) se registró la aparición de urgencia miccional de novo.
Conclusiones: El TVT-Secur corresponde a una cinta de tercera generación, eficaz y segura en el tratamiento quirúrgico de la incontinencia de orina de esfuerzo. Se trata de una técnica con potenciales ventajas al compararla con las cirugías antecesoras. La mantención de los buenos resultados en el tiempo, deberá evaluarse con el seguimiento e incorporación de nuevas pacientes a través de los años a este protocolo de trabajo.
Palabras clave: Incontinencia de orina de esfuerzo (IOE). Cinta vaginal libre de tensión TVT-Secur. Cinta sub-medio uretral.
Introduction
The first TVT for surgical correction of stress urinary incontinence was described in 1996 by Ul-msten et al. (1,2). At present, the benefits of this technique are recognized when it is compared with Bur-ch surgery (3), but the TVT is a operation that is not without potential complication. Between these were found the perforation of abdomino-pelvic organ, such as bowel and bladder. In addition this technique avoids bleeding complications due pelvic vessels perforation (4-7).
In order to carrying out surgical techniques with minor invasion, simpler and less potential risks, the transobturator technique born as the TOT and TVT-O (8-12). Unlike the TVT the transobturator techniques do not requires a routinely intraoperative cystoscopy and the complication as abdomino-pelvic organ perforation is reduced. The needle is moving away from the bladder.
A third-generation sub-mid-urethral tape in the urinary incontinence surgical treatment is represented by TVT-Secur (13). This is a tape smaller than all the techniques predecessors and theoretically should further reduce potential complications. With the objective of reviewing the safety and efficacy of this new technique, we present our experience with the first 110 cases.
Method
Study protocol
Prospective follow-up of 110 patients admitted for stress urinary incontinence surgery correction with TVT-Secur technique (Women's Health & Urology, Ethicon, Johnson & Johnson) between January 2007 and May 2008 at the Urogynecology and Vaginal Surgery Unit, Gynecology Department, Clínica Las Condes.
Inclusion criteria
Patients with stress urinary incontinence which had for more than a year of evolution and permanent. All had symptoms and signs of stress urinary incontinence observed in the first medical consultation. Urinary incontinence was demonstrated by non-multichannel Urodynamic test (14). All women had to have stress urinary incontinence type II or II with some degree of intrinsic sphincter deficiency (II+III) according to the McGuire's et al. classification (15). All patients should have urethral hypermobility confirmed by a Q-Tip test.
Exclusion criteria
Patients with urge o mixed urinary incontinence. Patients with a history of previous surgeries performed to correct stress urinary incontinence and/ or genital prolapse. In cases with cystocele or rectocele were discarded those with obstructive factor. Also urodynamic with and without cystocele and/or rectocele correction by a Bresky valve was performed. If the urinary incontinence disappeared with manually correction those patients were ruled out of the protocol.
Criterion of cure, improvement and failure
The outcome of the surgery was classified according to the number of episodes of urinary incontinence recorded during the monitoring period. It was considered a cure to the absence of urinary incontinence. Improvement was when the presence of incontinence episodes less than once each week.
Failure was considered to the presence of episodes more than once a week (16).
Follow-up period
We completed a follow-up period until July 2008.
Characteristics of the study group
The media age was 56 years old (31-82), body mass index 29 (25-37) and parity 3 (2-4) (Table I).
Criterion for choosing the position of the tape
In all patients in this study were positioned in "U". The criterion for admission was urinary incontinence in women with type II or type II associated with intrinsic sphincter deficiency (II+III).
Anesthesia:
- Spinal anesthesia: cases with only sub-mid-urethral tape and women with other associated vaginal surgery.
- General anesthesia: cases associated with laparoscopic surgery.
TVT-Secur Device description
It is a small device consisting of two branches. At its distal end is a polypropylene macropore mesh with effectiveness use under urethra by other techniques such as TVT and transobturator tapes. The end that holds the mesh is embedded between two sheets of absorbable material, consisting of vicryl (poliglactin 910) and suturing of PDS (polidioxanon). Each branch at its opposite end has a system that allows disconnecting the mesh by hauling a piece of metal, once that it is in the area of integration under the urethra. The right arm has a plastic piece on the end of the introduction of the mesh that covers the sharp edges (insertion zone) to avoid damage by neglect and to identify it (Figure 1).
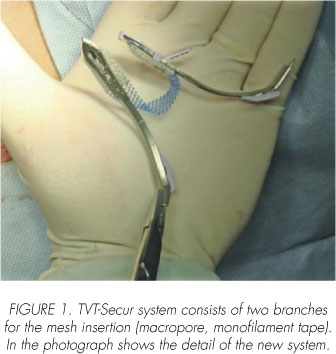
Specific surgical technique
The patient in a gynecological position with bending of thigh-abdomen of 90 degree. A 16 french catheter Foley is used ensuring the complete emptying of the bladder.
Step 1:
A 10 mm incision in the vaginal mucosa, in the sub-mid urethral third (Figure 2).
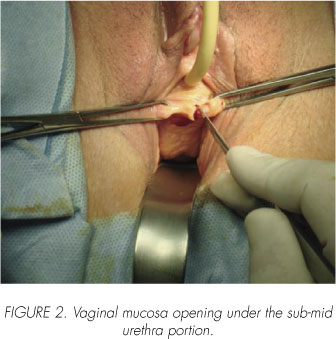
Step 2:
A.- If the option for placement the tape is in "U" the dissection is done at 45 degree by a Metzembaum scissor. The dissection should be 2 to 2.5 cm in length (Figure 3). By opting for this position must be placed within a mobilize device into the Foley catheter to move the bladder to the opposite side where the TVT-Secur branch is insert.
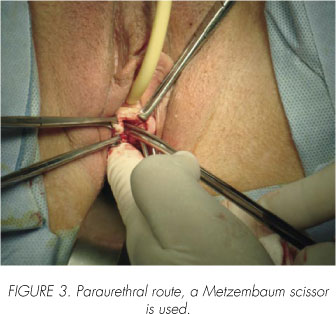
B.- If the option for placement the tape is in "V" or hammock, the paraurethral tissue dissection must be conducted in more than 45 degrees. The dissection is also performed with the Metzembaum scissor and is 2 to 2.5 cm.
Step 3:
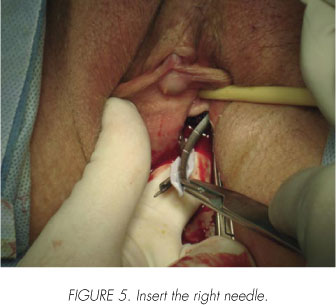
Using a needle holder takes the TVT-Secur arm which will be introduced and moves through space dissected making pressure (Figure 4). Repeat the maneuver on the opposite side (Figure 5).
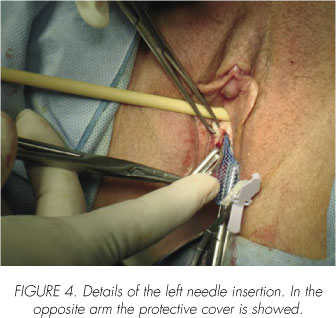
If the option is in "U" position a cystoscopy procedure should be a review to ensure the indemnity of the wall bladder and urethra after the insertion of the TVT-Secur branches.
Step 4:
Removing the insertion handle on each side by a small rotary motion and strength, pushing towards the end of fixing the bony structures of the pelvis. If necessary before removing the branches to adjust the tape through a greater or lesser pressure and/or with a Metzembaum scissor between the tape and the urethra.
Step 5:
Vaginal mucosa suture with 3-0 vycril. It is important to emphasize that in case of opting for the "U" tape position, it is necessary to place the mobilize device in the interior of the catheter Foley to move the bladder and urethra in addition to perform a cystoscopy revision. In "V" position is not necessary to complete these steps.
Removal catheter Foley:
• When TVT-Secur was placed without concomitant surgery the catheter Foley was removed at 2 hours after surgery.
• In cases with hysterectomy associated the catheter Foley was removed after 12 hours in the postoperative period.
Concomitant surgery:
In cases with hysterectomy it was performed by laparoscopic technique. The total hysterectomy was done completely by laparoscopic surgery removing the uterus vaginally and closing the vaginal cuff at the same time. In cases with perineoplasty it was realized after the TVT-Secur.
Analgesia:
Intravenous Ketoprofen was used, 100 mg every 8 hours completing three doses: then ibuprofen 600 mg every 12 hours v.o. completing 7 days.
Hospital stay:
Cases only with TVT-Secur leaved hospital at 12 hour after spontaneously urination. Cases with concomitant surgery leaved hospital at 48 hours.
Ambulatory monitoring was performed at 7 and 30 days at the office, and then remained monthly telephone communication and control if necessary.
For this study were signed informed consents authorizing the surgery once explained the technique and potential risks and benefits. Included with the authorization of the clinic and the Ethics Committee, with a protocol used sub-mid urethral tape for surgical treatment of urinary incontinence.
Results
In 97 (88.2%) of the 110 patients was conducted additionally to the TVT-Secur some gynecological surgery. The associated surgeries were: total laparoscopic hysterectomy, perineoplasty for symptomatic cystocele and/or rectocele and laparoscopic tubal ligation. In the cases of hysterectomy, the reason for this additional surgery was symptomatic myomas or adenomyosis. In the cases of an association of cystocele and/or rectocele repaired it was type II or III of the POP-Q classification.
In 60 women were associated three surgeries, in 15 two and one in 22. The major common association was TVT-Secur with anterior or posterior perineoplasty, followed by the association to total laparoscopic hysterectomy.
The operative time of TVT-Secur fluctuated between 6 and 16 minutes, media 8 minutes. The observation period was completed between 2 month (4 cases) and 19 months, with media of 8 months.
During the intraoperative time two cases of bladder perforation were detected, both with the right arm of the TVT-Secur. We proceed to remove the branch to reinstall immediately. An 18 french Foley catheter was used for 48 hours in both cases (Table II).
Immediate postoperative complications (before 7 days after surgery):
There were 2 cases of urethral obstruction observed immediately after removed the catheter Foley. In one patient was observed when at 2 hours after surgery the catheter was removed corresponding to a case without associated surgery. This patient was initially treated with anti-inflammatory v.o. and with Foley catheter for 48 hours. In this time the periurethral edema was reduced. But at 48 hours the obstruction was not resolved and the tape was readjusted in operating room (Table II).
The second case was a woman in who the catheter Foley was removed at 12 hours post surgery associated to hysterectomy and anterior and posterior perineoplasty. There was a partial blockage evidenced by high residual urine in bladder, in a woman with symptoms of incomplete voiding. Anti-inflammatory and catheter Foley was used for 48 hours to reduce the periurethral edema and inflammation. But at 3 weeks was necessary readjusted the tape because the patient evolution was with new partial obstruction symptoms. This woman remained with normal continent characteristics after this readjustment procedure (Table II).
Late postoperative complications (after 7 days after surgery):
There was no extrusion or erosion by the tape at vaginal mucosa or other complications. Only in the case previously described the tape was readjusted during this period (Table II).
Solution of the urinary incontinence:
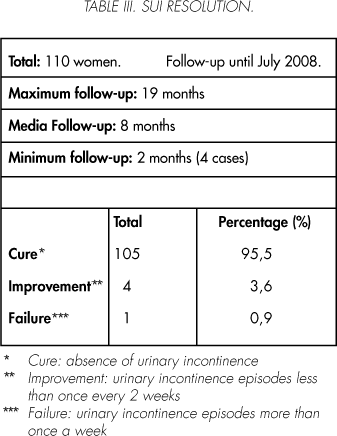
105 (95.5%) of the 110 cases were recorded cure of the SUI which was maintained during the observation period. Including the two cases of urethral obstruction, once the tape was readjusted at 48 hours and 3 weeks respectively. However in 2 of them novo urge incontinence was observed at 8 and 10 postoperative days respectively. Both were treated with Tolterodine and the symptoms were totally controlled in one woman leaved the medication without new episodes. In the other case at completing the closure of this report continued with Tolterodine with partial solution after three month.
In 4 (3.6%) cases showed improvement and 1 (0.9%) failed. This latest case filed fails immediately after the removal Foley catheter, at 12 hours in women with associated surgery. Three month after was treated with a new tape. In this time the tape consisting in a classic retro-pubic TVT achieving continence (Table III).
Discussion
Undoubtedly this new system for surgical correction of stress urinary incontinence is a third generation tape with fewer invasions when compared with the predecessor surgeries. The classic retro-pubic TVT system have a long tape and a greater potential risk of bleeding complications due to the large irrigated areas where the needle passes. The new system is not without potential complications of this type but it should be less risk. On the other hand being a small tape, less mesh is inserted; just what is required under the urethra. Theoretically reduces inflammation after surgery providing a rapid stand up, early ambulation and a reduced hospital stay. According to the above mentioned the new TVT-Secur system responds with great property to the minimally invasive surgeries that the previous techniques (13,17-19). But we must not forget that this technique is not without potential complications as demonstrated by the few publications that exist (13,17-19).
Different studies have compared TVT with the transobturator techniques showing that there are minor complications due to not pass in retro-pubic space as in the second generation tapes (20,21). The new TVT-Secur system newly accumulated cases and to publish the first series, for this reason the long follow-up will allow us to perform in the future an objective comparison with the first and second generation tapes, in order to verify that not only theoretically is expected fewer complications.
Another advantage of this third-generation tape is the ability to choose if we put in "U" as the classic TVT or in "V" as the transobturator technique. In a previous publication with the first 16 patients, 6 cases were included in "V" and 10 in "U". In this series we use the tape only in "U" position. The cases corresponded to SUI type II or with some degree of intrinsic sphincter deficiency (II+III). Currently we prefer techniques that leave the tape in "U" position in patients with some degree of intrinsic sphincter deficiency. Different series have shown a high degree of efficiency in the use of TVT ("U" position) in patients with SUI, urethral hypermobility and intrinsic sphincter deficiency (22). We must not forget that in patients with tape in "U" position, a cytoscopy review is necessary. As was done in all patients in this series in which two cases of side wall bladder perforation were identify. The tape of this new system is proven successful. It is a macropore, monofilament, polypropylene mesh, is a type I (23). These features allow the mesh a good "biointegration". The 75 micron pores allow the passage of macrophages to act on possible bacteria also will facilitate the formation of new vessels and the arrival of supporting elements like collagen allowing the reinforcement of uroligament under the urethra.
The system that holds the TVT-Secur is innovating because the mesh at the ends is enclosed as in a sandwich, consisting of Vicryl (poliglactin 910) and PDS (polidioxanon). The tip allows for adherence to the pubic bone that gives a proper subject. The pre-clinical evaluation published by Rezapour (24) et al during 2007 showed that the strength of fixation afforded by this system is equivalent to the originally delivered by TVT and this increases over time. This experience was conducted in sheep and demonstrated that a force grater than 5 N (500 gm) is required to alter the structure tape. This equates to a force 10 times higher than normally support by the fascia. Another important point of this study is that revealed by histology good mesh integration to the under mid-urethra tissues. With an 8 months media follow-up (between 2 and 19 month) the results of cure (95.5%) are very promising. However, we must remember that the tape was placed in "U" as a classic TVT and the patients were strictly selected (SUI type II or II+III). For this reason the results may not be good in patients selected solely by clinical (symptoms and signs without urodynamic study) since could undergo surgery patients with other types of incontinence. On the other hand, in all our patients according a protocol, when they have vaginal mucosa atrophy they were prepared with local vaginal estriol to improve the trophism. This decreases the likelihood of extrusion or erosion mesh in vagina. In our series there were not observed cases with this complications during the follow-up period, however we must continue to observe this potential complication in the late postoperative period. Table IV
During 2007 the publication of Martan et al (13) with 15 women (10 in "V" and 5 in "U") under an observation period between 1 and 2 months, showed a 93% of cure. The complications were minor in this series: 2 strips meshes, 1 case of vaginal pain and 1 case of erosion vaginal wall.
During 2008 the manuscript of Debodinance et al (17) published an experience with 110 women (71 SUI, 39 MUI, 23 with intrinsic sphincter deficiency) under TVT-Secur surgery. 85.5% in "V" and 2 months follow-up, with 70.4% of cure (83% for women only with SUI, 72.2% SUI with intrinsic sphincter deficiency, 50% for MUI). The complications in this series: 19.6% novo urge incontinence, 13.2% dysuria de novo, 1 mesh exposure, 1 granuloma, 1 urinary tract infection and 7 cases in whom a cord was touch, but without pain. Thirteen cases had moderate pain for 4 to 30 days.
During 2008 the publication of Neuman with 100 patients showed 2 cases of obstruction and one case with paravesical hematoma of 50cc. In the first 50 patients was observed a 20% (10 women) fault. In the second part of the study also with 50 patients registered 8% (4 patients) fault. About complications in the first 50 patients: 8% (4 women) with vaginal mucosa perforate during the needle passage, 12% (6 female) with extrude tape, 10% (5 women) tape outside the original position requiring a second TVT-Secur. In the second group of 50 patients in who were taken care to avoid complications observed in the first group, showed 8% (4 patients) tape extrusion. Regarding urinary continence registered by telephone communication at 12 months, in the first 50 patients was 88.6%, while second group was 93.5%.
Like any new technique has a learning curve to improve the results and reduce the complication possibility, as demonstrated by the publication presented by Neuman (18), which compares the two groups of patients.
It is essential to make a small incision in the vaginal mucosa, so that the tape is moving or bending. We must be meticulous paravaginal dissection in order to avoid the rupture of blood vessels that lead to abundant bleeding or the hematomas formation.
Another point to discuss, the TVT-Secur is a technique that reduces the operative time. In our series there was a media of 8 minutes (6 to 16 minutes). In the series presented by Debodinance et al (17) the operative time was similar with 8 to 30 minutes. This is a new surgical technique that requires less time for implementation, this advantage only shows the ease of insertion of mesh and less invasion.
The follow-up of this series will continue and incorporating new cases to report on the maintenance of good results in the long time.
Conclusions
In our experience the TVT-Secur is a third-generation tape, securely and efficiently in the stress urinary incontinence surgical treatment.
The TVT -Secur presents potential advantages when is compared with the predecessor surgery techniques, however only the long time follow-up and incorporation of new cases in the study protocols will determine the permanence of good results.
 Correspondence:
Correspondence:
Paolo Ricci
Lo Fontecilla 441
Las Condes. Santiago de Chile.
pricci@clc.cl
pricci@vtr.net
Accepted: August 16th, 2008.
References and recommended readings (*of special interest, **of outstanding interest)
**1. Ulmsten U, Henriksson L, Johnson P, Varhos G. An ambulatory surgical procedure ander local anesthesia for treatment of female urinary incontinence. Int Urogynecol J Pelvic Floor Dysfunct, 1996; 7:81-5. [ Links ]
**2. Ulmsten U, Johnson P, Rezapour M. A three-year follow up of tension free vaginal tape for surgical treatment of female stress urinary incontinence. Br J Obstet Gynaecol, 1999; 106:345-50. [ Links ]
3. Palma P. A requiem to the Burch. Int Urogynecol J Pelvic Floor Dysfunct, 2007; 18:589-90. [ Links ]
4. Jiménez Calvo J, Hualde Alfaro A, Santiago González de Garibay A, Pinós Paul M, Jiménez Aristu J, Montesino Semper M, et al. TVT: three years of experience. Actas Urol Esp, 2004; 28:13-20. [ Links ]
5. Sola Dalenz V, Pardo Schanz J, Ricci Arriola P, Guiloff Fische E, Chiang Miranda H. TVT associated with other gynecological operations in the same procedure: results and complications. Arch Esp Urol, 2005; 58:983-8. [ Links ]
*6. Ulmsten U, Falconer C, Johnson P, Jomaa M, Lannér L, Nilsson CG, et al. A multicenter study of tension-free vaginal tape (TVT) for surgical treatment of stress urinary incontinence. Int Urogynecol J Pelvic Floor Dysfunct, 1998; 9:210-3. [ Links ]
7. Abouassaly R, Steinberg JR, Lemieux M, Marois C, Gilchrist LI, Bourque JL, et al. Complications of tension-free vaginal tape surgery: a multi-institutional review. BJU Int, 2004; 94:110-3. [ Links ]
*8. Delorme E. Transobturator urethral suspension: mini-invasive procedure in the treatment of stress urinary incontinence in women. Prog Urol, 2001; 11:1306-13. [ Links ]
*9. Delorme E, Droupy S, De Tayrac R, Delmas V. Transobturator tape (Uratape). A new minimally invasive method in the treatment of urinary incontinence in women. Prog Urol, 2003; 13:656-9. [ Links ]
10. Pardo Schanz J, Ricci Arriola P, Tacla Fernández X, Betancourt Ortiz E. Trans obturator tape (TOT) for female stress incontinence. Experience with three years follow-up in 200 patients. Actas Urol Esp, 2007; 31:1141-7. [ Links ]
11. Pardo Schanz J, Ricci Arriola P, Sola Dalenz V, Tacla Fernández X. Trans-obturator-tape (TOT) for the surgical repair of stress urinary incontinence: our experience". Arch Esp Urol, 2006; 59:225-32. [ Links ]
12. Sola Dalenz V, Pardo Schanz J, Ricci Arrióla P, Guiloff Fische E, Chiang Miranda H. Minimal invasive surgery in female urinary incontinence: TVT-O. Actas Urol Esp, 2006; 30:61-6. [ Links ]
**13. Martan A, Masata J, Svabík K. TVT SECUR System-tension-free support of the urethra in women suffering from stress urinary incontinence-technique and initial experience. Ceska Gynekol, 2007; 72:42-9. [ Links ]
14. McGuire EJ, Fitzpatrick CC, Wan J, Bloom D, Sanvordenker J, Ritchey M, et al. Clinical assessment of urethral sphincter function. J Urol, 1993; 150:1452-4. [ Links ]
*15. Solà Dalenz V, Ricci Arriola P, Pardo Schanz J. Estudio urodinámico en la evaluación de la incontinencia urinaria femenina, con el nuevo sistema MoniTorr MR (urodinamia monocanal con medición de presión de retro-resitencia uretral). Experiencia con 100 pacientes. Actas Urol Esp, 2008; 32:325-31. [ Links ]
16. Blaivas JG, Jacobs BZ. Pubovaginal facial sling for the treatment of complicated stress urinary incontinence. J.Urol, 1991; 145:1214-8. [ Links ]
**17. Debodinance P, Lagrange E, Amblard J, Lenoble C, Lucot JP, Villet R, et al. TVT Secur: more and more minimal invasive. Preliminary prospective study on 110 cases. J Gynecol Obstet Biol Reprod (Paris), 2008; 37:229-36. [ Links ]
**18. Neuman M. Perioperative Complications and Early Follow-up with 100 TVT-SECUR Procedures. J Minim Invasive Gynecol, 2008; 15:480-4. [ Links ]
**19. Sola Dalenz V, Ricci Arriola P, Pardo Schanz J. Stress urinary incontinence surgical correction with third generation sub-mid-urethra sling: TVT-Secur. Actas Urol Esp, 2008; 32:222-9. [ Links ]
20. Novara G, Galfano A, Boscolo-Berto R, Secco S, Cavalleri S, Ficarra V, et al. Complications rates of tension-free midurethral slings in the treatment of female stress urinary incontinence: a systematic review and meta-analysis of randomized controlled trials comparing tension-free midurethral tapes to other surgical procedures and different devices. Eur Urol, 2007; 53:288-308. [ Links ]
21. Sola V, Pardo J, Ricci P, Guiloff E, Chiang H. TVT versus TVT-O for minimally invasive surgical correction of stress urinary incontinence. Int Braz J Urol, 2007; 33:246-52. [ Links ]
22. Meschia M, Pifarotti P, Buonaguidi A, Gattei U, Spennacchio M. Tension-free vaginal tape (TVT) for treatment of stress urinary incontinence in women with low-pressure urethra. Eur J Obstet Gynecol Reprod Biol, 2005; 122:118-21. [ Links ]
23. Roth CC, Holley TD, Winters JC. Synthetic sling: which material, which approach. Curr Opin Urol, 2006; 16:234-9. [ Links ]
**24. Rezapour M, Novara G, Meier PA, Holste J, Landgrebe S, Artibani W. A 3-month preclinical trial to assess the performance of a new TCT-like mesh (TVTx) in a sheep model. Int Urogynecol J Pelvic Floor Dysfunct, 2007; 18:183-7. [ Links ]











 texto en
texto en 


