My SciELO
Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO -
 Access statistics
Access statistics
Related links
 Cited by Google
Cited by Google -
 Similars in
SciELO
Similars in
SciELO  Similars in Google
Similars in Google
Share
Nutrición Hospitalaria
On-line version ISSN 1699-5198Print version ISSN 0212-1611
Nutr. Hosp. vol.20 n.3 Madrid May./Jun. 2005
Original
Nutritional risks and colorectal cancer in a portuguese population
P. Ravasco*, I. Monteiro-Grillo*,**, P. Marqués Vidal* y M.ª E. Camilo*
*Unit of Nutrition and Metabolism, Institute of Molecular Medicine of the Faculty of Medicine of the University of Lisbon, Avenida Prof. Egas Moniz 1649-028 Lisboa, Portugal. p.ravasco@fm.ul.pt **Radiotherapy Department of the Santa Maria University Hospital, Avenida Prof. Egas Moniz 1649-035 Lisboa, Portugal and Unit of Nutrition and Metabolism, Institute of Molecular Medicine of the Faculty of Medicine of the University of Lisbon, Avenida Prof. Egas Moniz 1649-028 Lisboa, Portugal. imonteiro.grillo@hsm.min-saude.pt
| Abstract Background: Food and nutrition as major causes of colorectal cancer (CRC) are still debatable. (Nutr Hosp 2005, 20:165-172) Key words: Colorectal cancer. Risk factors. Diet. Nutrients. Alcohol. Tobacco. | RIESGOS NUTRICIONALES Y CÁNCER COLORRECTAL EN UNA POBLACIÓN PORTUGUESA Resumen Antecedentes: Se sigue debatiendo el que los alimentos y la nutrición sean causas principales en el cáncer colorrectal (CCR). (Nutr Hosp 2005, 20:165-172) Palabras clave: Cáncer colorrectal. Factores de riesgo. Dieta. Nutrientes. Alcohol. Tabaco. |
Correspondence: Paula Ravasco
Unidade de Nutrição e Metabolismo
Instituto de Medicina Molecular
Faculdade de Medicina de Lisboa
Avda. Prof. Egas Moniz
1649-028 Lisboa (Portugal)
E-mail: p.ravasco@fm.ul.pt
Recibido: 21-IX-2004.
Aceptado: 15-XI-2004.
Introduction
Dietary epidemiology worldwide ascribes the incidence of about a third of cancers to nutritional factors1,2; their identification in different geographical areas is a priority since about 50% of cancers are estimated to be preventable by adequate nutrition and body weight, regular physical activity and tobacco abstention1,3. Notwithstanding individual genetics, nutrient-gene interactions and nutrient-modulated gene expression may further explain cancer incidence and progression4-7.
For colorectal cancer (CRC) some nutritional components are putatively accepted as risk factors, e.g. refined carbohydrates8 and lipids9, whereas protein and alcohol are still controversial10-14; conversely, other nutrients are regarded as protectors, e.g. insoluble fiber15,16 and micronutrients17-19.
The increasing incidence of colorectal cancer (CRC) in Portugal calls for objective dietary epidemiological data. Thus, our main purpose was to address this issue and investigate potential indicative patterns with both clinical and Public Health relevance. This study aimed to characterize and identify the prevalence of high-risk life-styles and diet patterns, based on detailed food composition analysis in all classical and recently identified bioactive food constituents, and their associations with colorectal cancer.
Materials and methods
This cross-sectional study approved by the University Hospital Ethics Committee was conducted in accordance with the Helsinki Declaration of 1975 as revised in 1983, and designed to characterize and identify the prevalence of high-risk life-styles and diet patterns and their associations with colorectal cancer. All participants gave their informed consent and individual data were registered in forms preconceived for statistical analysis.
Subjects
Between July 2000 and January 2002, all consecutive ambulatory patients with CRC referred to the Radiotherapy Department (n = 70) were considered eligible. For every patient the clinical and CRC family history, and co-morbidities were registered. Diagnosis was established by histology and imaging methods, according to the TNM classification (American Joint Committee on Cancer)20. The control population was recruited at community health centers or amongst administrative/technical hospital staff, and consisted of 70 randomly selected subjects without any cancer history, matched for sex and age, the latter stratified in 5-year intervals; only subjects with no reported recent weight changes or dietary restrictions were included.
Life-styles and nutritional status
Height was obtained with a stadiometer and weight was determined with a calibrated floor Jofre® scale. Body mass index (BMI) was calculated and categorized as severe malnutrition (≥ 16 kg/m2), malnutrition (> 16-19 kg/m2), adequate (≥ 20-25 kg/m2), overweight (> 25-30 kg/m2), stage 1 obesity (> 30-35 kg/m2), stage 2 obesity (> 35-40 kg/m2) and stage 3 obesity (> 40 kg/m2)21. Jackson's questionnaire categorized physical activity level in a 0 to 7 scale, ranging from "did not perform any regular intense physical exercise or leisure activity" to "did perform regular intense physical exercise"22. According to the previous and present smoking habits, subjects were defined as non-smokers (never or occasional consumption) or smokers (regular consumption >10 years even if not currently consuming); number of packages per day, duration of consumption (years) and the total number of packages per year was calculated.
Dietary pattern
The diet history method (including alcohol consumption) comprising a 24-hour recall food questionnaire, a food frequency questionnaire and a 72-hours diet diary (2 week days and 1 weekend day)23,24 was always used; the same registered research dietician (PR) interviewed all subjects who were also questioned on the use of dietary supplements. The software DIETPLAN version 5 for Windows (Forestfield software Ltd 2002, Horsham, UK) was used to analyze nutrient contents of foodstuffs and meals. In what concerns alcohol consumption, the duration (years), type of alcoholic beverages and intake frequency were registered, the usual intake amounts were quantified by using photographic models25, and the total alcohol intake was calculated (expressed in grams per day). Total nutrient and alcohol intake were compared with the Dietary Recommended Intake (DRI)26,27; for flavonoids or isoflavones, lacking established DRI, comparisons were based on median intakes and the average content of rich dietary sources. Nutritional intake analysis comprised the foods/nutrients classically associated with CRC and "new" components, whose relevance has been recently suggested in vitro.
Statistical Analysis
Statistical analysis was conducted using SPSS 10.0 (SPSS Inc, Chicago, USA) and EPI-Info 2000 (CDC, Atlanta, USA). Parametrical (Students't) and non-parametrical (Wilcoxon) tests determined differences in nutritional status and life-style variables between cases and controls. Correlations were assessed by Spearman rank method. For both food and total nutrient intake, subjects were categorized according to quartiles of intake. We used relative risk as a measure of association, defined as the incidence of CRC in each food intake quartile, divided by the corresponding rate among the subjects on the lowest quartile. Age-adjusted relative risks were calculated after stratification according to 5-year categories. Proportional hazards models were used to adjust for multiple risk factors simultaneously (age, BMI, CRC family history, tobacco, physical activity, co-morbidities). In addition stratified analyses were conducted to determine whether the influence of nutritional intake was modified by other risk factors for CRC. All P values are two-sided. To evaluate the influence of measurement error on our findings, we used a correction procedure that adjusts the relative risks and confidence intervals to account for errors in assessing nutritional intake28. For all statistics, significance was accepted at the 5% probability level.
Results
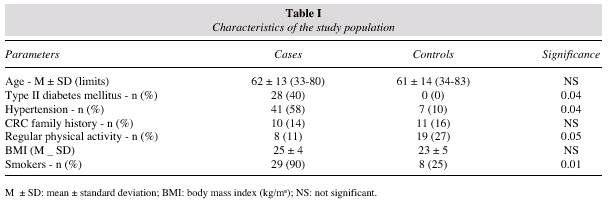
Characteristics of the study population are shown in table I; subjects with type II diabetes mellitus and/or hypertension were just treated with drug therapy and did not follow any specific diet. There was an overall trend associating a lower BMI to higher level of physical activity (p = 0.09) though the latter was unrelated to CRC risk. In what concerns smoking there were 29 current smokers amongst CRC patients and 8 amongst controls, all female patients and controls were non-smokers; there was a smoking-associated relative risk of 1.90 (1.86-1.97). None of the participants was taking nutritional supplements.
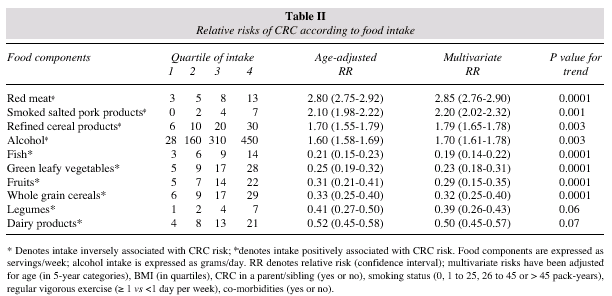
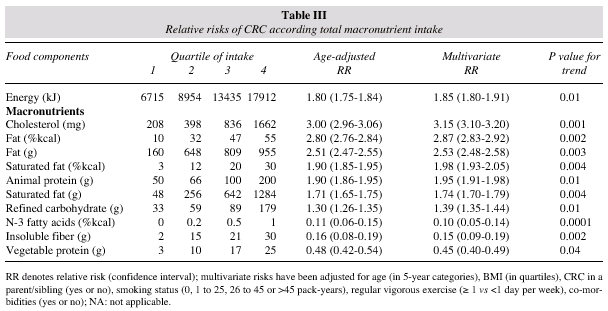
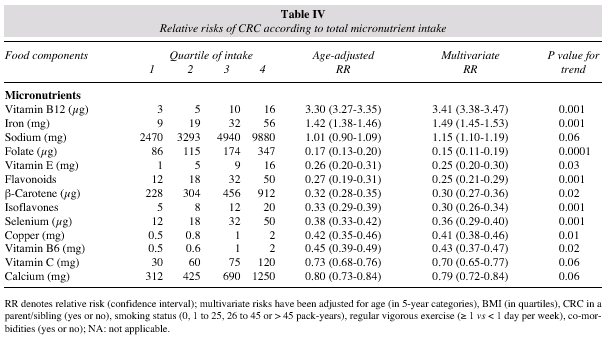
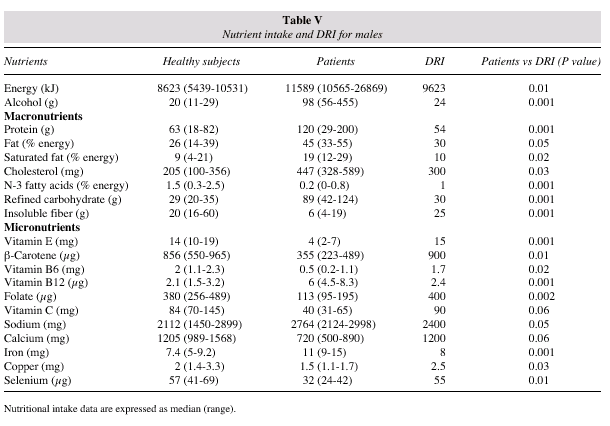
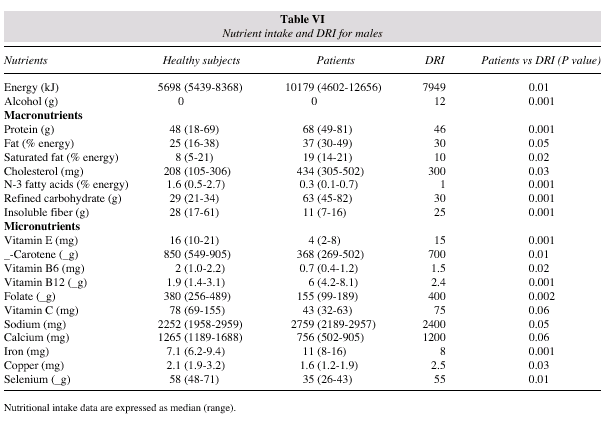
Age-adjusted and multivariate analyses showed that both the diet pattern and the intake of specific nutrients were strongly associated with the incidence of CRC, in the highest as compared with the lowest quartile, tables II, III and IV. In multivariate analyses, each increment of 4 servings per week of red meat, smoked salted pork products and 100g of alcohol corresponded to an increased relative risk of 1.29 (95% CI: 1.21-1.34). In what concerns nutrients, each increment of at least 50% in the weekly intake of protein, total fat, saturated fat, cholesterol, refined carbohydrates, iron, vitamin B12,sodium and alcohol corresponded to an increased relative risk of 1.53 (95% CI: 1.47-1.59). Conversely, the increment of 4 servings per day of green leafy vegetables, fruits and fish corresponded to a decreased relative risk of 0.35 (95% CI: 0.29-0.41). Each increment of at least 50% in the weekly intake of n-3 fatty acids, insoluble fibber, vitamin E, flavonoids, isoflavones, ß-carotene, folate and selenium corresponded to a decreased relative risk of 0.31 (95% CI: 0.26-0.37). Further nutrient analysis in patients identified several differences between current intake and the DRI, tables V and VI. The median intake of flavonoids and isoflavones was also significantly lower (p = 0.001) than the comparison value.
Discussion
Nutrition is a putative though controversial risk factor for CRC. This prospective study thoroughly investigated epidemiological data previously unknown in Portugal. The diet of "healthy subjects" was indeed similar to the Mediterranean pattern1,29, 30, unlike CRC patients' monotonous and unbalanced diet, characterized by high risk nutritional deficits and surpluses. Patients' diet was characterized by frequent and excessive consumption of red meat and processed meat products resulting in excessive intake of animal protein, saturated fat, cholesterol, vitamin B12 and haem iron; likewise, refined carbohydrates and alcohol consumption was overabundant. Conversely, the intake of fruits and vegetables was lower than the recommended 5-9 daily portions31 with subsequent deficits of insoluble fiber, vitamins, minerals and other protective compounds, e.g. flavonoids29,32 and isoflavones33; the intake of fish and n-3 fatty acids was also very low. This diet pattern was associated with smoking habits in 45% of patients and with low physical activity in 77%, though the latter was unrelated to CRC risk unlike previously suggested34,35. Among life-style risk factors, several case-control studies demonstrated a consistent association between tobacco consumption and CRC35-37; our results are only concordant in men since women were non-smokers. CRC risk associated with alcohol abuse is controversial14,38, 39, potentially enhanced by concurrent vita-min deficits; in this study women were teetotal, thus alcohol was a risk factor just for men whose diets were also markedly deficient in various vitamins, similarly to what we have previously shown40,41.
Epidemiological data concerning energy intake and CRC have been inconsistent, excessive energy intake and increased risk42 versus no risk43. In our study, high energy intake represented an 85% increase of CRC risk, and energy sources, e.g. total fat and refined carbohydrates, which independently represented 187% and 79% increased risk, respectively; this association is consistent with their pro-carcinogenic effect on colorectal cell lines9,44. The association between excessive protein intake and CRC has been inconsistent, no risk11,12 versus increased risk10, the latter was corroborated by our study; the citotoxicity of protein metabolism end products may act as a carcinogenesis promoter45.
A marked reduction of CRC risk associated with frequent fish consumption and n-3 fatty acids was a major novelty of this study; its relevance may bear to their anti-inflammatory effects46 and potential pro-apoptotic properties47.
A high intake of insoluble fiber is consistently recommended given its ascribed direct48-50 and indirect protective roles8,51. CRC patients' diet was markedly deficient in insoluble fiber that whenever consumed according to recommendations31 is expected to result in an 85% risk reduction.
Deficits of antioxidants are likely to promote oxidative stress and carcinogenesis52. Patients' diet contained a marked surplus of haem iron associated with free radicals production53, while the concurrent vitamin E deficit forbear their protective effects54-56. Epidemiology also reports an association between low blood α-tocopherol concentrations and increased CRC risk57, our study is however the first to show that an adequate intake of vitamin E is associated with 75% reduced risk. Selenium, seldom evaluated58, now revealed a protective effect. Flavonoids are a hot research topic due to their antioxidant59, pro-apoptotic properties60, and cell proliferation inhibitory effect61; this study first shows epidemiological data on their protective effect with 75% risk reduction. Fruits and vegetables, main sources of vitamin C and ß-carotene, are rich in numerous beneficial compounds62-64; indeed a significant protective effect higher than 60% was attributed to an adequate intake of green leafy vegetables, fruits and legumes.
In spite of the potential physiological properties of isoflavones33,65, exclusively conveyed by vegetables, our study is so far the first to have identified a significant protective effect against CRC.
Epidemiological evidence associates folate deficiencies to CRC incidence, since chronically deficient diets determine DNA hypomethylation and chromosomic alterations (66, 67). Two studies showed a modest risk increase associated with prolonged deficits of vitamin B6, methionine, folate and vitamin B1268,69. Notwithstanding the lack of data related to excessive intake, vitamin B12 in excess may compete with folate on the remethylation cycle and determine DNA hypomethylation19. In CRC patients' diet, vitamin B6 and folate was >3 times below the DRI whereas vitamin B12 in-take was 3 times higher the DRI; both deficit and surplus were associated with >70% increased risk.
Despite the study's limitations related to its sample size, data were adjusted for all recognized confounding variables and still pinpointed nutrients identified worldwide since 1982 as risk factors for CRC27 and reinforced the protective of others, whilst disclosing emerging protective nutrients33,59, 60. Given the worldwide high and increasing incidence of CRC, investigations of nutrient-carcinogenesis interactions are warranted to further stress the relevance of preventive nutrition.
ACNOWLEDGEMENTS
We are indebted to the medical, nursing and technical staff of the Radiotherapy Department of the Hospital of Santa Maria.
REFERENCES
1. World Cancer Research Fund: American Institute of Cancer Research. Food, nutrition and the prevention of cancer: a global perspective. In: American Institute for Cancer Research, 1997. [ Links ]
2. Working Group on Diet and Cancer of the Committee on Medical Aspects on Food and Nutrition Policy: Nutritional aspects of the development of cancer. London: Dep. Health Rep. Health Social Subjects 48 (The Stationery Office), 1998. [ Links ]
3. World Health Organization: Prevention of cancer. Geneva: WHO, 1964. Report No.: WHO Tech. Rep. 276. [ Links ]
4. Palli D, Vineis P, Russo A et al: Diet, metabolic plolymorphisms and DNA adducts: the EPIC-Italy cross-sectional study. Int J Cancer 2000, 87:444-451. [ Links ]
5. Slattery M, Andersen K, Curtin K, Ma K-N, Schaffer D, Samowitz W: Dietary intake and microsatellite instability in colon tumors. Int J Cancer 2001, 93:601-607. [ Links ]
6. Hill M: Mechanisms of diet and colon carcinogenesis. Eur J Cancer Prev 1999, 8:S95-S98. [ Links ]
7. Rock C, Lampe J, Patterson R: Nutrition, genetics and risks of cancer. Annu Rev Public Health 2000, 21:47-64. [ Links ]
8. Franceschi S, dal Maso L, Augustin L et al: Dietary glycemic load and colorectal cancer risk. Ann Oncol 2001, 12:173-178. [ Links ]
9. Hill M, Aries V: Faecal steroid composition and its relationship to cancer of the large bowel. J Pathol 1971, 104:129-139. [ Links ]
10. Meyer F, White E: Alcohol and nutrients in relation to colon cancer in middle-aged adults. Am J Epidemiol 1993, 138:225-236. [ Links ]
11. Macquart-Moulin G, Riboli E, Cornee J, Charnay B, Berthezene P, Day N: Case-control study on colorectal cancer and diet in Marseilles. Int J Cancer 1986, 38:183-191. [ Links ]
12. Benito E, Stiggelbout A, Bosch F et al: Nutritional factors in colorectal cancer risk: a case-control study in Majorca. Int J Cancer 1991, 49:161-167. [ Links ] 13. Breuer-Katschinski B, Nemes K, Marr A et al: Alcohol and cigarette smoking and the risk of colorectal adenomas. Dig Dis Sci 2000, 45:487-493. [ Links ]
14. Kearney J, Giovannucci E, Rimm E et al: Diet, alcohol, and smoking and the occurrence of hyperplastic polyps of the colon and rectum (United States). Cancer Causes Control 1995, 6:45-56. [ Links ]
15. Reddy B, Engle A, Katsifis S, et al: Biochemical epidemiology of colon cancer: effect of types of dietary fiber on fecal mutagens, acid, and neutral sterols in healthy subjects. Cancer Res 1989, 49:4629-35. [ Links ]
16. Harris P, Ferguson L: Dietary fibers may protect or enhance carcinogenesis. Mutas Res 1999, 443:95-110. [ Links ]
17. El-Bayoumy K; The protective role of selenium on genetic damage and on cancer. Mutas Res 2001, 475:123-139. [ Links ]
18. Claycombe K, Meydani S: Vitamin E and genome stability. Mutas Res 2001, 475:37-44. [ Links ]
19. Ames B: DNA damage from micronutrient deficiencies is likely to be a major cause of cancer has a modest but potentially important protective effect against colorectal cancer. Mutat Res 2001, 475:7-20. [ Links ]
20. Sobin L, Ch W: UICC TNM Classification of malignant tumors. New York: John Willey & Sons, Inc., 1997. [ Links ]
21. Garrow JS: Treat obesity seriously. Edinburgh: Churchil Livingstone, 1981. [ Links ]
22. Arroll B, Jackson R, Beaglehole R: Validation of a three-month physical activity recall questionnaire with a seven-day food intake and physical activity diary. Epidemiology 1991, 2:296-299. [ Links ]
23. Burke B: The diet history as a tool in research. J Am Diet Assoc 1947, 23:1041-1046. [ Links ]
24. Ocké M, Kaaks R: Biochemical markers as additional measurements in dietary validity studies: application of the methods of triads with examples from the European Prospective Investigation into Cancer and Nutrition. A J Clin Nutr 1997, 65 (Supl. 4):1240S-1245S. [ Links ]
25. Marques M, Pinho O, Vaz de Almeida M: Manual de quantificação de alimentos. 1ª ed. Porto: Rocha Artes Gráficas, Lda, 1996. [ Links ]
26. Food and Nutrition Information Center: Dietary Reference In-takes (DRI) and Recommended Dietary Allowances (RDA). Beltsville, Maryland: National Agricultural Library (NAL) and U.S. Department of Agriculture (USDA), 2001. [ Links ]
27. WHO SG: Diet, nutrition and the prevention of chronic diseases. Geneva: WHO, 1990. Report No.: Technical report series no 797. [ Links ]
28. Rosner B, Spiegelman D, Willet W: Correction of logistic regression relative risk estimates and confidence intervals for measurement error: the case of multiple covariates measured with error. Am J Epidemiol 1990, 132:734-745. [ Links ]
29. Panagiotakos D, Chrysohoou C, Pitsavos C et al: The association of Mediterranean diet with lower risk of acute coronary syndromes in hypertensive subjects. Int J Cardiol 2002, 82:141-147. [ Links ]
30. La Vecchia C AA, Tavani A: Vegetables, fruit, antioxidants and cancer: a review of Italian studies. Eur J Nutr 2001, 40:261-267. [ Links ]
31. National Cancer Institute and the Produce for Better Health Foundation: 5 a day for better health: National Cancer Institute and the Produce for Better Health Foundation, 2001. [ Links ]
32. Perez-Jimenez F, Lopez-Miranda J, Pinillos M et al: A Mediterranean and a high-carbohydrate diet improve glucose metabolism in healthy young persons. Diabetologia 2001, 44:2038-43. [ Links ]
33. Nagel S, vom Saal F, Welshons W: The effective free fraction of estradiol and xenoestrogens in human serum measured by whole cell uptake assays: physiology of delivery modifies estrogenic activity. Proc Soc Exp Biol Med 1998, 217:300-309. [ Links ]
34. Giovannucci E, Ascherio A, Rimm E, Colditz G, Stampfer M, Willett W: Physical activity, obesity, and risk for colon cancer and adenoma in men. Ann Intern Med 1995, 122:327-34. [ Links ]
35. Terry P, Ekbom A, Lichtenstein P, Feychting M, Wolk A: Long-term tobacco smoking and colorectal cancer in a prospective cohort study. Int J Cancer 2001, 91:585-7. [ Links ]
36. Slattery M, Potter J, Friedman G, Ma K, Edwards S: Tobacco use and colon cancer. Int J Cancer 1997, 70:259-264. [ Links ]
37. Heineman E, Zahm S, McLaughlin J, Vaught J: Increased risk of colorectal cancer among smokers: results of a 26-year follow-up of US veterans and a review. Int J Cancer 1994, 59:728-738. [ Links ]
38. Bardou M, Montembault S, Giraud V et al: Excessive alcohol consumption favours high risk polyp or colorectal cancer occurrence among patients with adenomas: a case control study. Gut 2002, 50:38-42. [ Links ]
39. Jedrychowski W, Steindorf K, Popiela T et al: Risk of colorectal cancer from alcohol consumption at lower vitamin intakes. A hospital-based case-control study in Poland. Rev Environ Health 2001, 16:213-222. [ Links ]
40. Cravo M, Glória ML, Camilo ME, Neves Cardoso J, Nobre Leitao C, Mira F: Deficiências vitamínicas nos alcoólicos crónicos: consequências metabólicas e implicações clínicas. Jornal Português de Gastrenterologia 1995, 2:74-79. [ Links ]
41. Glória ML, Cravo M, Camilo ME et al: Nutritional deficiencies in chronic alcoholics: relation to dietary intake and alcohol consumption. Am J Gastroenterology 1997, 92:485-489. [ Links ]
42. Lyon J, Mahoney A, West D et al: Energy intake: its relationship to colon cancer risk. J Natl Cancer Inst 1987, 78:853-861. [ Links ]
43. Bostick R, Potter J, Kushi L et al: Sugar, meat, and fat intake, and non-dietary risk factors for colon cancer incidence in Iowa women (United States). Cancer Causes Control 1994, 5:31-52. [ Links ]
44. Young G, McIntyre A, Albert V, Folino M, Muir J, Gibson P: Wheat bran suppresses potato starch-potentiated colorectal tumorigenesis at the aberrant crypt stage in a rat model. Gastroenterology 1996, 110:508-514. [ Links ]
45. Cummings J, Macfarlane G: The control and consequences of bacterial fermentation in the human colon. J Appl Bacteriol 1991, 70:443-459. [ Links ]
46. Latham P, Lund E, Johnson I: Dietary n-3 PUFA increases the apoptotic response to 1,2-dimethylhydrazine, reduces mitosis and suppresses the induction of carcinogenesis in the rat colon. Carcinogenesis 1999, 20:645-650. [ Links ]
47. Chen Z, Istfan N: Docosahexaenoic acid is a potent inducer of apoptosis in HT-29 colon cancer cells. Prostaglandins Leukot Essent Fatty Acids 2000, 63:301-308. [ Links ]
48. van Munster I, Tangerman A, Nagengast F: Effect of resistant starch on colonic fermentation, bile acid metabolism, and mucosal proliferation. Dig Dis Sci 1994, 39:834-42. [ Links ]
49. Jenkins D, Kendall C, Popovich D et al: Effect of a very-high-fiber vegetable, fruit, and nut diet on serum lipids and colonic function. Metabolism 2001, 50:494-503. [ Links ]
50. Wang J, Friedman E: Short-chain fatty acids induce cell cycle inhibitors in colonocytes. Gastroenterology 1998, 114:940-946. [ Links ]
51. Bruce W, Wolever T, Giacca A: Mechanisms linking diet and colorectal cancer: the possible role of insulin resistance. Nutr Cancer 2000, 37:19-26. [ Links ]
52. Bruce W, Giacca A, Medline A: Possible mechanisms relating diet and risk of colon cancer. Cancer Epidemiol Biomarkers Prev 2000, 9:1271-1279. [ Links ]
53. Babbs C: Free radicals and the etiology of colon cancer. Free Radic Biol Med 1990, 8:191-200. [ Links ]
54. Chinery R, Brockman J, Peeler M, Shyr Y, Beauchamp R, Coffey R: Antioxidants enhance the citotoxicity of chemotherapeutic agents in colorectal cancer: a p53-independent function of p21WAF1/CIP1 via c/EBP beta. Nat Med 1997, 3:1233-1240. [ Links ]
55. Dubois R, Radhika A, Reddy B, Entingh A: Incrased COX-2 levels in carcinogen-induced rat colonic tumours. Gastroenterology 1996, 110:1259-1264. [ Links ]
56. Eberhart C, Coffey R, Radhika A, Giardello F, Ferrenbach S, Dubois R: Up-regulation of COX-2 gene expression in human colorectal adenomas and adenocarcinomas. Gastroenterology 1994, 107:1183-1188. [ Links ]
57. Longnecker M, Martin-Moreno J, Knekt P et al: Serum alpha-tocopherol concentration in relation to subsequent colorectal cancer: pooled data from five cohorts. J Natl Cancer Inst 1992, 84:430-435. [ Links ]
58. Clark L, Cantor K, Allaway W: Selenium in forage crops and cancer mortality in U.S. counties. Arch Environ Health 1991, 46:37-42. [ Links ]
59. Owen R, Giacosa A, Hull W, Haubner R, Spiegelhalder B, Bartsch H: The antioxidant/anticancer potential of phenolic compounds isolated from olive oil. Eur J Cancer 2000, 36:1235-1247. [ Links ]
60. Wenzel U, Kuntz S, Brendel M, Daniel H: Dietary flavone is a potent apoptosis inducer in human colon carcinoma cells. Cancer Res 2000, 60:3823-3831. [ Links ]
61. Kuntz S, Wenzel U, Daniel H: Comparative analysis of the effects of flavonoids on proliferation, cytotoxicity, and apoptosis in human colon cancer cell lines. Eur J Nutr 1999, 38:133-142. [ Links ]
62. Cook N, Le I, Manson J, Buring J, Hennekens C: Effects of beta-carotene supplementation on cancer incidence by baseline characteristics in the Physicians' Health Study (United States). Cancer Causes Control 2000, 11:617-626. [ Links ]
63. Palozza P, Calviello G, Serini S et al: beta-carotene at high concentrations induces apoptosis by enhancing oxy-radical production in human adenocarcinoma cells. Free Radic Biol Med 2001, 30:1000-1007. [ Links ]
64. Palozza P, Calviello, G, Maggiano N, Lanza P, Ranelletti F, Bartoli G: Beta-carotene antagonizes the effects of eicosapentaenoic acid on cell growth and lipid peroxidation in WiDr adenocarcinoma cells. Free Radic Biol Med 2000, 28:228-234. [ Links ]
65. Frentzel-Beyme R, Chang-Claude J: Vegetarian diets and colon cancer: the German experience. Am J Clin Nutr 1994, 59 (5 Supl.): 1143S-1152S. [ Links ]
66. Pufulete M, Al-Ghnaniem R, Leather A et al: Folate status, genomic DNA hypomethylation, and risk of colorectal adenoma and cancer: a case control study. Gastroenterology 2003, 124:1240-1248. [ Links ]
67. Konings E, Goldbohm R, Brants H, Saris W, van den Brandt P: Intake of dietary folate vitamers and risk of colorectal carcinoma: results from The Netherlands Cohort Study. Cancer 2002, 95:1421-1433. [ Links ]
68. Harnack L, Jacobs DJ, Nicodemus K, Lazovich D, Anderson K, Folsom A: Relationship of folate, vitamin B-6, vitamin B-12, and methionine intake to incidence of colorectal cancers. Nutr Cancer 2003, 43:152-158. [ Links ]
69. Slattery M, Schaffer D, Edwards S, Ma K, Potter J: Are dietary factors involved in DNA methylation associated with colon cancer? Nutr Cancer 1997, 28:52-62. [ Links ]