Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Nutrición Hospitalaria
versión On-line ISSN 1699-5198versión impresa ISSN 0212-1611
Nutr. Hosp. vol.25 no.6 Madrid nov./dic. 2010
The importance of the coding of hospital malnutrition in the health strategy of the European Union; a Spanish contribution
Importancia de la codificación de la desnutrición hospitalaria en la estrategia de salud de la Unión Europea; una aportación española
J. Álvarez, M. León, M. Planas and A. García de Lorenzo
Members of the Executive Board and Scientific Committee of SENPE (Spanish Society of Parenteral and Enteral Nutrition). Spain
ABSTRACT
Malnutrition related to illness and inadequate nutrition remains a matter of relevant interest in the member countries of the European Union because of its elevated prevalence and high costs. It is estimated to affect 30 million patients and cost 170 billion euros annually. The 2008-2013 strategy "Together for Health" put forward in the European Parliament urges Member States to develop, together with local and regional authorities, initiatives in the field of education of the population, training, investigation and good clinical practices. SENPE (Spanish Society of Parenteral and Enteral Nutrition) collaborates in different areas in the development of this strategy which aim to put malnutrition related to illness in the focus of the health system. One of its contributions has been the preparation of the Document of Consensus on the Coding of Malnutrition SENPE-SEDOM (Spanish Society of Medical Documentation). The agreements adopted have helped normalize the process of coding this pathology with the assignment of specific codes for specifically defined terms. This document has allowed the optimization of information regarding the types and degrees of malnutrition and the procedures employed for its prevention or treatment in the hospital centres of the National Health System.
Key words: Malnutrition. Health strategy. Coding. Consensus SENPE-SEDOM.
RESUMEN
La desnutrición relacionada con la enfermedad y una nutrición inadecuada sigue constituyendo un área sanitaria de interés relevante entre los países miembros de la Unión Europea, por su elevada prevalencia y sus altos costes. Se estima que afecta a 30 millones de pacientes y cuesta 170 billones de euros anuales. La Estrategia 2008-2013 "Together for Health " planteada en el Parlamento Europeo insta a los Estados miembros, a que desarrollen, junto con las autoridades regionales y locales, iniciativas en el ámbito de la educación a la población, la formación específica, la investigación y las buenas prácticas clínicas. La SENPE (Sociedad Española de Nutrición Parenteral y Enteral) colabora en distintas áreas de desarrollo de esta estrategia que pretende situar a la desnutrición relacionada con la enfermedad en el foco de atención del sistema sanitario, como estrategias similares han situado a la obesidad. Una de sus contribuciones ha sido el desarrollo del Documento de Consenso de Codificación de la Desnutrición SENPE-SEDOM (Sociedad Española de Documentación Médica). Los acuerdos adoptados han permitido normalizar el proceso de codificación de esta patología con la asignación de códigos específicos a términos definitorios concretos. Este documento ha permitido optimizar la información sobre la desnutrición tipos y grados, y los procedimientos empleados para prevenirla o tratarla, en los centros hospitalarios de nuestro Sistema Nacional de Salud.
Palabras clave: Desnutrición. Estrategia para la salud. Codificación. Consenso SENPE-SEDOM.
Introduction
Hospital Malnutrition is the focus of attention of a great number of health professionals and managers today. However, it is widely accepted that there is still a lot to be done.
In spite of important scientific and technical advances, malnutrition related to illness and inadequate nutrition continue to be of relevant interest due to its elevated prevalence and high cost, it is estimated to affect 30 million patients and cost 170 billion euros annually1
The European Parliament, in plenary sessions held on the 25th of September and the 9th of October 2008 approved two resolutions which urge the European Commission to "take a more holistic approach to nutrition and make malnutrition, alongside obesity, a key priority in the field of health, incorporating it wherever possible into Community-funded research, education and health promotion initiatives and EU-level partnerships" and that the "Member States, along with regional and local authorities, to use the cooperation mechanism to improve the exchange of best practice". For this reason they asked the Commission "to be proactive in producing guidelines and recommendations based on such good practice". These resolutions are encompassed within the Strategy "Together for Health: A Strategic Approach for the EU 2008-2013".2,3
On the 11th of June 2009, representatives from the Ministries of Health of the Member States of the EU, the Czech presidency of the EU, medical experts, representatives of the health administrations and health insurance groups, ESPEN (European Society for Clinical Nutrition and Metabolism), and ENHA (European Nutritional Health Alliance) signed the Prague Declaration and arrived at the unanimous conclusion that malnutrition, including malnutrition related to illness is an urgent public health problem in Europe. They also stressed that appropriate actions must be taken to prevent malnutrition because of its relationship with an increase in morbidity and mortality, as well as deterioration in the quality of life of patients.4
The Spanish Society of Parenteral and Enteral Nutrition (SENPE), as an active member of ESPEN participates in the strategy "Together for Health", in the fight against malnutrition related to illness. In this context they have acquired the commitment to implement activities integrated in a nutritional care plan (specific training in health collectives, good clinical practice guides, etc).
One of these activities is designed for the management of hospital malnutrition information. The Documentation Work Group created the document SENPESEDOM Coding of Hospital Malnutrition. The interest of this document lies in the identification and unification of the defining concepts of malnutrition together with its types and degrees in the hospital environment. After several months of work, members of SENPE and SEDOM, made their conclusions public in a consensus document which was distributed by the media organizations of both scientific societies,5,6,7 and adopted as the instructional baseline document in the coding of hospital malnutrition by the Technical Office of the ICD-9 of the Ministry of Health and Consumption (MHC).8 Among the most important functions of the Technical Unit of the ICD-9 of the National Health System (NHS) is the unification of diagnostic and procedural coding at the national level and to define the coding regulations for the NHS.9
This is an important contribution in the normalization of information regarding hospital malnutrition, but we are aware of the difficulties that doctors may have with the comprehension of some of the concepts related with the coding methodology employed in the document. For this reason, with this article we are trying to facilitate the understanding of the normal process of coding hospital malnutrition in light of the SENPE-SEDOM agreements.
Coding
Knowledge of our health reality will always help us to analyze the situation prior to making a decision. The importance of a record of activities in this regard is well known to everyone. All this information is important from an epidemiological and economic management point of view.
Coding is one way of indexing clinical information that contains clinical histories in order to facilitate its storage and recovery. In the middle of the 20th century the ICD-9, International Statistical Classification of Diseases and Related Health Problems was developed in the United States, as an adaptation of the International Classification of Diseases Adopted for use in the United States (ICDA-8) and the ICDA Adaptation for Hospitals (H-ICDA). The intention of this initiative was that it would serve as a basis both for mortality and morbidity data collected for statistical purposes as well as information regarding illnesses and operations present in clinical histories, with the object of facilitating the storage and recovery of said data.10
Several versions of this document have existed which have updated the information contained in it. The latest version in use in all spanish hospitals is called the ICD 9 CM. It is a clinical modification of the International Classification of Diseases 9th Revision (ICD 9) of the World Health Organization.11
The term "clinical" is used to emphasize the purpose of the amendment: which is to serve not only for health statistics, but as a useful tool in the classification of morbidity data for the management of clinical histories, revisions of medical treatments, outpatient care programs and other types of medical care. Obviously to describe the clinical picture the codes must be more precise than those needed for statistical groupings and the analysis of trends.
The coding of diseases follows a system of numerical categories which have been assigned to diseases in accordance with previously established criteria. A classification of diseases must meet a series of conditions such as:
- Have a restricted number of categories in which all diseases must be grouped.
- Any disease can only be classified in one category, since the categories are exclusive among themselves.
The ICD 9 CM complies with these requisites and although, as we will see further on, it is not perfect, it has the advantage that it is being used in hospitals all over the world to code discharges and it is updated annually.12
Thus, the ICD 9 CM has established itself as a useful tool for the management of clinical information and constitutes an information baseline for the health financing systems in the United States of America and a great number of European countries.
The exercise of coding
The ICD 9 CM and its latest version the ICD 10 CM, are published in three volumes:13
- Volume 1 Illnesses: Tabular List.
- Volume 2 Illnesses: Alphabetic Index.
- Volume 3 Procedures: Tabular List and Alphabetic Index.
In the ICD 9 CM each chapter is divided into categories or sections to which a 3 digit code is always assigned. Within each category there are different subcategories which add a fourth digit to the code and sometimes the subcategory is divided into sub classifications which will add a 5th digit to the code. In order to classify and code correctly, the greatest number of digits possible must be reached. Very few diseases exist which can be classified with only 3 digits.
To guide the coder in his activity, at the beginning of each chapter, section, subcategory or sub classification of the tabular list of diseases appears a series of orders such as: Includes; Excludes; Note; Code addition or Use additional code if desired. Some abbreviations are also used, for example NOS which means Not Otherwise Specificied, and signs which indicate whether it is necessary to add a complementary code. Also, the classification of diseases has been increased to include physical states related with health and to provide greater specificity to the level of the fifth digit. Said fifth digits are not optional; they were designed for use in the recording of targeted information data (from the information collected) in the clinical history.
It is difficult for us doctors to understand the coding work that our documentalist colleagues do. It is clear that the exercise of coding requires rigorous method which is faithfully followed through ad hoc training.
The procedure of coding for each care episode is rigorously established. This must begin with the indexing which consists of identifying the principal diagnosis, secondary diagnosis and procedures.14
The preferred primary document for the indexing of the clinical history for the MBDS (Minimum Basic Data Set) is the discharge report, provided that both (discharge report and clinical history) are consistent. When it is deemed that the discharge report is incomplete, subsequently, the following clinical history documents will be taken into account in order of priority:
- Anamnesis page(s).
- Operative page(s).
- Anatomic pathologic report.
- Urgent care report.
- Nurse´s observations.
- Other documents.
The coder must extract, from the discharge reports, the significant elements:
- Principal diagnosis.
- Secondary diagnosis.
- Surgical procedures.
- Non-surgical procedures.
It is understood from the principal diagnosis of the condition what, after the necessary study and the criteria of the doctor responsible for the patient, was the cause of their admission to hospital, even though major complications appeared or even other independent conditions which are entered as secondary diagnoses. Those being the diagnoses other than the principal, which coexist with it at the time of admission, or that develop during the hospital stay and influence the duration of the same or the treatment administered. Surgical procedures are those which are performed in the operating room or maternity ward and non-surgical procedures are considered to be the tests performed on a patient for the purpose of therapeutic diagnosis.
Hospital malnutrition, in the majority of cases, is a secondary diagnosis of great interest, as we have already stated, because of its influence in the evolution of the original disease and the treatment it implies. Moreover, the specialized nutritional support measures are not surgical procedures. The record sheets of the Nutrition Units, which form a part of the clinical history, are relevant information for consultation in those cases in which the discharge report does not reflect the diagnosis of malnutrition. In the case of electronic histories, some system of universal record keeping should be taken into consideration which allows the nutritional state of the patients to be known, and being capable of incorporating the data into the final discharge report through an automatic connection.
After the indexing is identified, in each of the distinctive elements, the key element which allows its coding. The key term for a diagnostic expression will be the one word which serves to access the alphabetic index. Correspondence of a key term with a principal term in the alphabetical index will be sought, selecting those with the following priorities:
- Pathology or process.
- Adjective.
- Name or eponym.
The anatomical location is not used as a principal term.
After identifying the key element, it must be located in the index, paying close attention to all the instructions. Subsequently going to the tabular list and selecting the code which best defines the diagnosis or procedure. When there are several possible diagnoses which could justify admission, the decision will be made by the doctor responsible as to which is the principal, taking into account which of the diagnoses uses the most resources and above all which requires a surgical procedure. The acute processes always take preference over chronic processes when determining a principal diagnosis. In the case of chronic diseases, always make reference to the aggravations, complications or consequences which justify the care.
Concept of malnutrition in ICD-9 CM
One of the objectives of the SENPE-SEDOM coding work group was to meticulously analyze the concepts established as definitive for malnutrition in the ICD 9 CM. In the concrete case of malnutrition, it has added the principal malnutrition codes for protein malnutrition (Kwashiorkor), caloric (Marasmus) or mixed with the definition criteria for malnutrition which have historically been defined in the paediatric age group in less developed countries. Therefore, it does not specifically consider the case of hospital malnutrition in adults.
This is limiting in terms of achieving truthful information, a reflection of the care reality in hospital centres, given that our sick adults or children in the western world, who present with malnutrition as a secondary diagnosis in its different degrees of severity should receive some of these codes are not in line with clinical reality. For example, a previously healthy individual who after a severe event develops severe protein malnutrition should be coded as such. According to the ICD 9 he would be assigned the code 260 or probably better 262, but, with the definition given by the ICD 9, in the view of the doctor, neither of the two adjusts to this clinical manifestation in a way that could be considered adequate (table I).
A universally accepted definition of malnutrition does not exist. In addition, in recent years new clinicalpathological terms related to malnutrition are emerging, such as sarcopenia, cachexia and pre-cachexia which have been the subject of consensus documents among international Scientific Societies.15 Probably all this has contributed to maintaining certain difficulties in the interpretation of the codes, but an agreement has repeatedly been called for on the definitions and terms underpinning these codes (16). For this reason, the conclusions of the SENPE-SEDOM Coding group include definitions and codes agreed upon for the different types and degrees of hospital malnutrition which we diagnose daily in our patients5 (table II y III).
Recently a group of experts from ESPEN and ASPEN have agreed on a proposed definition for malnutrition in adults, linking it directly with the "etiological diagnosis".17,18 This definition highlights the importance of malnutrition related to the primary illness of the patient. This consensus describes three types of malnutrition:
- When there is chronic emaciation without inflammation, the experts propose the term "emaciation related with malnutrition". Examples of this clinical situation would be situations similar to those we see in a patient with anorexia nervosa.
- When there is chronic emaciation with chronic inflammation, of mild or moderate degree, they propose the term "malnutrition related with chronic illness". An example of this type would be patients who present criteria of organ failure, pancreatic cancer, rheumatoid arthritis or obesity with sarcopenia
- When there is chronic emaciation with inflammation acute and of severe degree, the proposal of the experts is to term it "malnutrition related with acute illness or state of aggression", accompanied by an acute inflammatory response. Some examples would be the malnutrition presented by patients with severe infections, burns, multiple injuries or cranial trauma.
It is obvious that this work group does not have the capacity to modify a universal norm, but to adapt, in a practical and rigorous way, the definitions, categorizations and coding of malnutrition in the ICD 9 CM, with the intention of facilitating the work of the coders and the better understanding of the doctors.
We have in our hands, validated methods of screening and nutritional diagnosis,19-24 which permit us to establish a diagnosis on the discharge of a patient to identify malnutrition as a primary or secondary diagnosis, as a determining pathology, the type according to the deficiency, caloric and/or protein and the severity. All this data contributes to the enrichment of our information systems, the MBDS of our hospital, and if we accept the coding agreements we could have an information management and resource consumption tool which permits us to make comparisons with ourselves in distinct periods of time and with hospitals of similar characteristics (benchmarking).
How to code malnutrition and the related procedures
As we have already said, malnutrition usually forms a part of the list of secondary diagnoses in a discharge report. Its recording is fundamental because of its clinical implications and because the consumption of resources associated with a malnourished person, by the illness itself or the diagnostic and therapeutic procedures used to prevent or reverse it is high and must always be taken into account.
The criteria for coding in the matter of malnutrition demand:
1. Documentation confirmation. For the assignation of a malnutrition code a diagnosis of the same is necessary with the corresponding documentation which reflects it.
2. Documentation sources. The preferred documentation source is the Discharge report, the decision of the doctor responsible or the Nutritional Support Team also being valid, the diagnosis of malnutrition in the clinical history, regardless of the support for the same, as we have previously said.
3. Different state. When a patient passes through different degrees of malnutrition in the same episode, the most severe that he has suffered will be recorded.
4. Procedures of artificial nutritional support. The performance of a nutritional procedure does not constitute the presumption of a diagnosis. In the presence of nutritional support without a diagnosis, the existence of the same must be confirmed and if it does not exist, only procedural codes will be recorded. The nutritional support must be greater than 1,000 kcal/day for it to be taken into consideration when it comes to coding.
5. Guidelines to follow in coding. If we take into consideration the general guidelines of coding previously described, after identifying the key term of the secondary diagnosis (malnutrition) we locate it in the alphabetic index and look to the tabular list to select the code which best defines the diagnosis, taking into account the categories and subcategories. In this way we would find it in the ICD 9 CM:
Malnutrition (caloric) 263.9
- abandonment................
..............
- degree
- - severe 261
- - - protein-calorie 262
- - mild 263.1
- - moderate 263.0
- - first 263.1
- - second 263.0
- - third 262
- severe 261
- - protein-calorie NCOC (Not codable under another concept) 262
- mild 263.1
- malignant 260
- moderate 263.0
- protein 260
- protein-calorie 263.9
- - severe 262
- - specified type NCOC 263.8
The SENPE-SEDOM agreements have permitted the identification, categorization and coding of the distinct types and degrees of malnutrition, facilitating the assigning of codes by the coder to the definitions of malnutrition, types and degrees, accepted by consensus by the doctors and documentalists. The allocation of the consensually proposed codes is the following:
Calorie Malnutrition:
Mild: 263.1
Moderate: 263.0
Severe: 261
Unspecified degree: 263.9Protein Malnutrition:
In any degree: 260Mixed or Protein-calorie Malnutrition:
Mild: 263.8
Moderate: 263.8
Severe: 262
Unspecified degree: 263.9Unspecified Malnutrition:
Mild: 263.1.
Moderate: 263.0.
Severe: 261.
Unspecified degree: 263.9
6. Coding of nutritional support procedures: Parenteral Nutrition: 99.15. The corresponding catheter insertion must be coded, provided that it takes place during admitting.
Enteral Nutrition: 96.6 reflecting support greater than 1000 Kcal/day.
In this difficult framework, the reader could be surprised by the allocation of the same code to identify various diagnoses, like for example those of mixed malnutrition of unspecified degree and unspecified malnutrition of unspecified degree, or those of caloric malnutrition mild or moderate and unspecified malnutrition in mild or moderate degree. These codes were agreed upon by doctors and documentalists to facilitate the classification of processes which until that time were assigned according to the subjective criteria of the coder. On occasions the lack of information supplied in the discharge report did not allow for the allocation of the proper code with the consequences that this could have on the estimates of the consumption of resources.
We also want to point out that according to the definitions established in the ICD 9 CM for the nutritional support procedures, both dietary counselling and nutritional supplements are not covered and therefore are not considered in the classification and allocation of codes. In the field of clinical nutrition, this is one of the criticisms that the ICD 9 CM receives, as it leaves out the classification of aspects of diagnostic or procedural interest. However, to understand this absence it is important to remember two fundamental aspects. The first is the conceptual origin of the ICD 9 CM which we have commented on throughout the text. The second is that it deals with a general norm, internationally and universally accepted, in that no country has the ability to unilaterally modify it. It is for this reason that the adaptations suggested in the SENPE-SEDOM consensus document must be understood to act as an interpretation guide for our use in our clinical practice, so that everyone is able to collect the recorded information regarding hospital malnutrition using a common language.
Since the dissemination of this information among the coders in all Spanish national territory and the official publication of the SENPE -SEDOM Consensus Document, in the June 2008 Bulletin by the Technical Office of the ICD 9 -CM of the MHC,8 the recording of codes has followed the agreed upon guidelines which have clearly facilitated the exercise of coding.
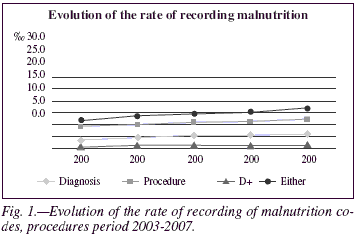
It is clear that the interest of both doctors as well as coders has increased, to obtain this information and significantly increase the records of malnutrition and coded procedures (fig. 1), as well as the assignation of more specific numerical codes. The recorded rate of any code corresponding to any type of malnutrition in 2003 was 3,3 for every 1000 hospital discharges, while in 2007, after the implementation of the hospital malnutrition coding document, the rate was 5,93 for every 1000 discharges. In the case of procedures, during the same period, the records increased from 9,14 to 12,24 for every 1,000 discharges25 (tables IV, V and VI).
Final considerations
The coding process demands specific training and the knowledge of a laborious methodology. The stringency in coding allows us to obtain information of great relevance in the field of epidemiology, of economic management and the quality of care.
Malnutrition related to illness and especially hospital malnutrition constitutes a clinical entity of great significance in public health care systems around the world because of its high socio-health and economic costs.
The implementation of measures to optimize the information is a commitment from SENPE. That is why the development of a tool along these lines, like the SENPE-SEDOM Consensus document for the Coding of Malnutrition, has been an object of great interest among the members of both scientific societies, because it allows us to seek more rigorous information in our national care panorama in this area.
We believe that this document could be of assistance to all those members of other scientific societies similar to SENPE, federated in ESPEN, standardizing the definition and coding of malnutrition, types and degrees. A common language in a global health strategy.
Acknowledgements
Our appreciation to Dr J de Rio Mata, member of SEDOM, for his collaboration with the SENPESEDOM consensus document for the coding of Hospital, as well as, the analysis of malnutrition coding data from Spanish hospitals.
References
1. http://www.espen.org/fam.html [ Links ]
2. http://ec.europa.eu/health/ph_overview/Documents/strategy_wp_en.pdf [ Links ]
3. Clavete Oliva A. Estrategia de salud de la Unión Europea: salud pública para las personas europeas. Rev Esp Salud Pública 2008; 82: 271-281. [ Links ]
4. The Prague declaration: stop disease-related malnutrition. En: http://www.espen.org/wp/wordpress/?p=157 [ Links ]
5. Documento SENPE-SEDOM sobre la codificación de la Desnutrición Hospitalaria. En: http://www.sedom.es/99_pdf/senpe-sedom.pdf. [ Links ]
6. Álvarez J, García de Lorenzo A. Codificación de la desnutrición hospitalaria, la vigencia de una frase. Nutr Hosp 2008; 23: 529-530. [ Links ]
7. Álvarez J, Del Río J, Planas M, García Peris P, Gracía de Lorenzo A, Calvo V, Olveira G, Irles JA, Piñeiro G, Grupo de Trabajo de Documentación de SENPE. Nutr Hosp 2008; 23: 526-540. [ Links ]
8. Codificación de la Desnutrición Hospitalaria. En: Codificación Clínica con la CIE-9-MC. Unidad Técnica de la CIE-9-MC para el Sistema Nacional de Salud. Boletín no29, año XII, junio 2008. Ministerio de Sanidad y Política Social. Pp. 47-58. [ Links ]
9. Normativa. Manual de Usuarios de la CIE 9 MC. http://www.msc.es/estadEstudios/estadisticas/normalizacion/clasifEnferm/instrucNorma.htm [ Links ]
10. L J Lizarraga. Fichas Guía de Codificación Clínica. Ministerio de Sanidad y Consumo. Unidad de Técnica de la CIE-9-MC para el Sistema Nacionald e Salud. 3a ed. CIE-9-MC, 1997. [ Links ]
11. Manual de la Clasificación Internacional de Enfermedades, Heridas y Causas de Muerte. Organización Mundial de la Salud. Ginebra, Suiza, 1977. [ Links ]
12. Clasificación Internacional de Enfermedades 9a revisión Modificación Clínica (CIE 9-MC). En: http://www.msc.es/estadEstudios/estadisticas/normalizacion/clasifEnferm/home.htm [ Links ]
13. Organización Mundial de la Salud. Clasificación estadística internacional de enfermedades y problemas relacionados con la salud. - 10a. revisión. v. 3. Lista tabular. Washington, D.C.: OPS; 1995. [ Links ]
14. CIE 9 MC. 7a edición. Ministerio de Sanidad y Consumo. Enero 2010. [ Links ]
15. Muscaritoli M, Ander SD, Argilés J, Aversa Z, Bauer JM, Biolo G, Boire Y, Basaeus I et al. Consensus definition of sarcopena, cachexia and pre-cachexia: Joint document elaborated by Special Interest Groups (SIG) "cachexia-anorexia in chronic wasting disease" and nutrition in geriatrics". Clin Nutr 2010; doi: 10.1016/j.clinu.2009.12.004. [ Links ]
16. Swails WS, Samour PT, Babineau TJ, Bristian BR. A Proponed revision of current ICD-9-CM malnutrition code definitions. J Am Diet Assoc 1996; 96: 370-373. [ Links ]
17. Jensen GL, Mirtillo J, Compher C, Dhaliwal R, Forbes A, Figueredo Grijalba R, Ardí G, Kondrup J, Labadarios D, Nyulasi I, Castillo Pineda JC, Waitzberg D. Adult Starvation and Disease-Related Malnutrition: A Proposal for Etiology - Based Diagnosis in the Clinical Practice Setting From the International Consensus Guidelines Committee. JPEN 2010; 34: 156-159. [ Links ]
18. Jensen GL, Mirtillo J, Compher C, Dhaliwal R, Forbes A, Figueredo Grijalba R, Ardí G, Kondrup J, Labadarios D, Nyulasi I, Castillo Pineda JC, Waitzberg D. Adult Starvation and Disease-Related Malnutrition: A Proposal for Etiology - Based Diagnosis in the Clinical Practice Setting From the International Consensus Guidelines Committee. Clin Nut 2010; doi:10.1016/j.clnu.2009.11.010 [ Links ]
19. García Luna PP, Romero Ramos H. Desnutrición hospitalaria en pacientes adultos en España. En: Libro Blanco de la desnutrición clñínica en España. Coordinador JI Ulibarri. Editores: A García de Lorenzo, PP García Luna, P Marsé, M Planas. Acción Médica . Madrid 2004. Pp. 61-70. [ Links ]
20. Willett WC, Dietz WH, Colditz GA. Guidelines for healthy weight. N Engl J Med 1999; 341: 427-434. [ Links ]
21. Russell MK, Mueller C. Cribado y Valoración Nutriconal. En: Core Currículo en Apoyo Nutricional. Una aproximación basada en casos clínicos. Paciente adulto. Unidad 2. MM Gotteschkich ed. ASPEN versión española. Drug Farama SL. 2008. Pp. 1-24. [ Links ]
22. Kondrup J, Allison S, Elia M, Vellas B, Plauth M. ESPEN Guidelines for Nutrition Screening 2002. Clin Nutr 2003; 22: 415-421. [ Links ]
23. Stratton RJ, Green CJ, Elia M. Scientific criteria for defining malnutrition. In: Disease related malnutrition: an Evidence-Based approach to treatment. CABI Publishing UK, 2003. Pp. 1-34. [ Links ]
24. Lochs H, Allison SP, Meier R, Pirlich M, Kondrup J, Schneider St, van den Berghe G, Pichard C. Introductory to the ESPEN Guidelines on Enteral Nutrition: Terminology, Definitions and General Topics. Clin Nutr 2006; 25: 180-186. [ Links ]
25. Del Río Mata J, Bernal Losada O, Conejo Gómez C, Martínez Reina A, Geribés Hernandis MT, Fernandez Morales E. Registro de Desnutrición em el Conjunto Mínimo de Base de Datos del Sistema Nacional de Salud (2003-2007). En: http://www.juntadeandalucia.es/ [ Links ]
![]() Correspondence:
Correspondence:
Julia Álvarez.
E-mail: julia.alvarez@telefonica.net
Recibido: 3-X-2010.
Aceptado: 4-X-2010.