Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Nutrición Hospitalaria
versión On-line ISSN 1699-5198versión impresa ISSN 0212-1611
Nutr. Hosp. vol.26 no.1 Madrid ene./feb. 2011
Adherence of pregnant women to dietary counseling and adequacy of total gestational weight gain
Adhesión de gestantes a los consejos dietéticos y adecuación del aumento de peso en toda la gestación
B. Della Líbera1, M. Ribeiro Baião2, M. M.a A. de Souza Santos2, P. Padilha1, P. Dutra Alves1 and C. Saunders1
1Departamento de Nutrição e Dietética. Instituto de Nutrição Josué de Castro. Centro de Ciências da Saúde. Universidade Federal do Rio de Janeiro. Ilha do Fundão. Rio de Janeiro. RJ. Brasil.
2Departamento de Nutrição e Social e Aplicada. Instituto de Nutrição Josué de Castro. Centro de Ciências da Saúde. Universidade Federal do Rio de Janeiro. Ilha do Fundão. Rio de Janeiro. RJ. Brasil.
Financial support: Conselho Nacional de Desenvolvimento Científico e Tecnológico/CNPq (Support to Research), Fundação Carlos Chagas Filho de Amparo à Pesquisa do Estado do Rio de Janeiro/FAPERJ (Grants of Scientific Initiation), Programa Institucional de Bolsas de Iniciação Científica - Universidade Federal do Rio de Janeiro - Conselho Nacional de Desenvolvimento Científico e Tecnológico/PIBIC/UFRJ/CNPq (Grants of Scientific Initiation).
ABSTRACT
Introduction: in scientific literature there are not published researches which have used a validated assessment method of adherence to dietary counseling capable of being reproduced.
Objective: to evaluate the adherence of pregnant women to dietary counseling during the prenatal period using a validated instrument according to the outcome of total gestational weight gain.
Methods: two hundred and eight adult pregnant women participated in the research. The instrument for adherence classification to dietary counseling was elaborated according to four evaluation criteria: food quantity and quality, meal pattern and adjustment to weekly weight gain. We classified as poor adherence when zero-one criterion was observed, good adherence when 2-3 aspects were observed and excellent when the amount was 4 aspects.
Results: Pregnant women with good or excellent adherence had a higher adjustment proportion of the total gestational weight gain in comparison to those who presented poor adherence in the second and fourth visits, respectively (p < 0.006; p < 0.007). Women with poor adherence to dietary counseling in the second visit presented about three times more chances of having poor adherence in the fourth visit (OR = 3.11; CI = 1.46-6.36).
Conclusion: Adherence of pregnant women to dietary counseling had a positive association with the adjustment of total gestational weight gain.
Key words: Pregnant women. Counseling. Weight gain. Pregnancy nutrition.
RESUMEN
Introducción: en la literatura científica no se han publicado investigaciones que han utilizado un método validado de avaluación de la adhesión de gestantes a los consejos dietéticos.
Objetivo: avaluar la adhesión de gestantes a los consejos dietéticos, durante periodo prenatal, mediante un instrumento válido según los resultados del aumento de peso en toda la gestación.
Métodos: participaron de la encuesta 208 gestantes adultas en el período entre 2005 y 2006. El instrumento para la clasificación de la adhesión fue elaborado partiendo de 4 criterios de evaluación: cantidad, calidad alimentar, padrón de comidas, la adecuación de ganancia de peso semanal. Se clasificó como baja adhesión cuando se observó entre 0 y 1 criterios, como buena adhesión, entre 2 y 3 criterios, y óptima con 4 criterios.
Resultados: las gestantes con buena u óptima adhesión tuvieron una mayor proporción de adaptación del aumento de peso total durante la gestación, comparándose con las que presentaron baja adhesión (p < 0,006; p < 0,007). Las mujeres con baja adhesión en la segunda consulta presentaron 3 veces más probabilidad de tener baja adhesión en la cuarta consulta (OR = 3,11; IC = 1,46-6,36).
Conclusiones: la adhesión de las gestantes tuvo asociación positiva con la adaptación precoz al aumento de peso total durante la gestación, demostrando la importancia del cuidado alimentar precoz, fundamento de la advertencia dietética.
Palabras clave: Gestantes. Consejería. Aumento de peso. Alimentación prenatal.
Abbreviatures
BMI: Body Mass Index.
CI: Confidence Interval.
GD: Gestational Diabetes.
HSP: Hypertensive Syndromes of Pregnancy.
IUT: Infection of Urinary Tract.
OD: Odds Ratio.
SGA: Small for Gestational Age.
SD: Standard Deviation.
VAD: Vitamin A Deficiency.
Introduction
Some of the goals of larger global concerns in the areas of health and reproductive rights are to improve maternal health and to prevent avoidable deaths. In view of the actual world panorama where nearly 585,000 women die annually on account of pregnancy, childbirth and postnatal complications —99% of these deaths occur in developing countries, including Brazil— the necessary and effective strategies to decrease and prevent maternal deaths1 have been more and more discussed
Literature is consensual in recognizing the protective effect of prenatal care for maternal and neonatal health, which comprehends a set of actions addressed to risk reduction and severity of morbidity and mortality for the mother-child relationship.2-4 The efficacy of nutritional assistance during the prenatal period has already been suggested by a rising number of works which attest the benefits of adequate nutrition to pregnancy outcome.5-7
In the area of nutritional assistance, dietary counseling may be understood as discussed and negotiated guidelines of food and nutrition which aim the making of autonomous decisions related to behavior and food practices. Besides the more objective and quantified issues which embody the nutrition conduct itself, in prenatal context, the dietitian acting as a counselor may create a welcoming environment to allow the discussion of subjective issues inherent to the act of eating during the gestational period, hence contributing with a large adherence of pregnant women to nutrition guidelines.8,9
Up to the present moment, published researches which propose methods of adherence assessment related to any type of nutrition intervention are still scarce mainly when this intervention concerns the gestational period. Adherence assessment is an extremely relevant study area. In scientific literature, some assessment studies addressed to pregnant women were developed using different methods which took into account the need of elaboration, implementation and validation of actions which promote the effective incorporation of healthier food practices.10-12
In scientific literature there are not published researches which have used a validated assessment method of adherence to dietary counseling capable of being reproduced. Taking this into consideration, the aim of the study was to evaluate the adherence of pregnant women to dietary counseling through the elaboration of an instrument to be validated according to the total gestational weight gain outcome.
Materials and methods
This is a cross-sectional study conducted with 208 adult pregnant women attended in a public maternity hospital in the municipality of Rio de Janeiro in the period of 2005-2006 who participated in the research entitled "Impact assessment of prenatal nutritional assistance on obstetric outcomes".13 Inclusion criteria were: adult women (> 20 years old) without chronic diseases, with the beginning of prenatal assistance before 16 weeks of gestation and one fetus pregnancy.
This study was approved by the Ethics Committee of the Instituto de Puericultura e Pediatria Martagão Gesteira at the Universidade Federal do Rio de Janeiro/UFRJ and all participants signed the Free and Informed Term of Consent.14
Data collection was conducted by trained and supervised researchers. Data concerning socio-demographic and obstetric characteristics of the newborn and of nutritional and prenatal assistance were collected at the time of the visits to the dietitian through interviews and assessment of the subjects´ records.
As regards socio-demographic characteristics the following variables were considered: marital status, schooling degree, skin color, per capita family income, use of cigarette, alcohol and illicit drugs during pregnancy. Basic sanitation condition was considered adequate when the pregnant woman reported access to potable water, public sewage system, and waste collection.
The variables related to the current pregnancy, to the newborn, to obstetric and prenatal assistance characteristics were pre-gestational BMI, total gestational weight gain, birthweight, birthweight adequacy, gestational age at delivery, digestive symptomatology, gestational intercurrence according to the criteria of the Ministry of Health[3], number of pregnancies and number of prenatal visits to the doctor and to the dietitian. For anemia diagnosis the hemoglobin values of < 11.0 g/dl3 were considered, and the standardized interview for gestational night blindness was applied13 for identification of vitamin A deficiency (VAD).
To the purpose of developing prenatal dietary counseling, some principles were applied by the research team, such as to know the life history of the pregnant woman; to know how to listen; to show interest; to create and maintain a bond; to make dialogue possible; to communicate using an accessible language; to encourage; to pay compliments; and to suggest instead of imposing.8,9 Such principles were included in the individual visits to the dietitian, and a minimum amount of four visits along pregnancy was established and they should begin at the same time of prenatal care at the unit.
During the visits, nutritional assessment was conducted providing elements to an individual dietary guideline which consisted in a food bulletin based on the measurement of the total energetic value,15,16 the need of macro and micronutrients and the pregnant woman habits and food preferences, besides her economic, social and cultural possibilities. Recommendations for digestive symptoms, gestational intercurrences, nutrition deficiencies or any other aspect related to the nutritional area were also carried out.13
Adherence assessment was performed through an interview with pregnant women. In this interview the habitual feeding related to the period that was between the last visit and the subsequent one was questioned, and the information reported by the client was compared to the contents of the nutritional orientation bulletin. Assessed criteria were quantity (of the used food servings), quality (intake frequency of the food groups), meal patterns (considering the number and hours of the meals, their composition and food substitution by items belonging to the same group) and adequacy of weekly weight gain in comparison to the weekly weight gain measured in the previous visit. We consider as adequate the weekly weight gain up to 20% above or below the planned gain, and inadequate when this condition was not met.
After the individual analysis of each of the four items described previously, adherence was classified as poor (0 to one observed criterion), good (two-three criteria) or excellent (four criteria).
Adequacy of weekly and total gestational weight gain was conducted based on the proposition of the Ministry of Health3 for each range of pre-gestational body mass index (BMI).17,18 The cutoff points according the BMI categories were < 18,5 kg/m2 - underweight; 18,5-24,9 kg/m2 - normal; 25-29,9 kg/m2 - overweight and > 30,0 kg/m2 - obese, and the range of weight gain for each category were 12,5-18 kg, 11,5-16 kg, 7-11,5 kg, and 7 kg, respectively.
For the validation study of the adherence of pregnant women to nutritional guidelines, the association between adherence and the adequacy of total gestational weight gain outcome was verified.10-12,19 For the purpose of statistical measures, the good and excellent categories were grouped into a single category (good).
The instrument of data collection was pre-tested in the pilot study in a sample of 26 women with characteristics similar to those of the studied population. Data collected in this stage were not incorporated in the final sample of the study.
In the exploratory data analysis, the measures of central tendency and dispersion (mean and standard deviation - SD) for numerical variables and frequency distribution for the categorical variables were calculated. The Chi-square test was applied and the odds ratio (OR) and the 95% confidence interval (CI) were measured measured in order to verify the association among categorical variables. A 5% significance level was considered in the overall analyses. Analyses were carried out in the SPSS software program for Windows v.13.
Results
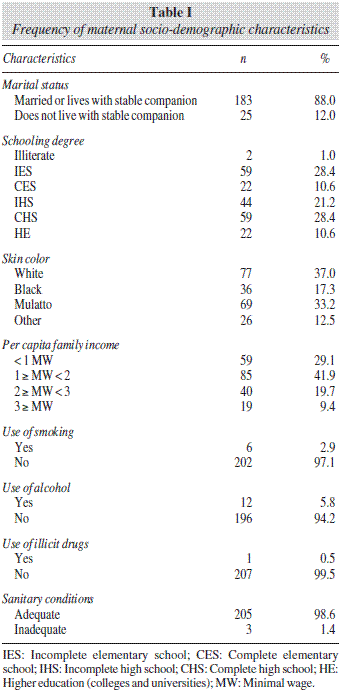
The pregnant women who participated in this study presented mean age of 27.3 years (SD = 4.8), most of them were not white (62.8%), the mean per capita family income was 1.88 minimal wages (SD = 4.65), and 88% were married or lived with a companion. Maternal socio-demographic characteristics are shown in table I.
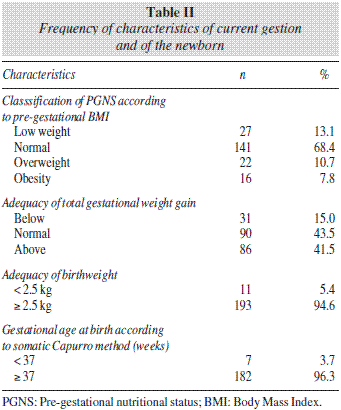
43.5% of women had an adequate total gestational weight gain (table II). The mean of visits to prenatal assistance was 9.02 (SD = 1.74) and to prenatal nutritional assistance, 4.12 (SD = 1.67).
As regards digestive symptoms, the most commonly reported were nauseas (66.6%), pyrosis (57.9%) and constipation (55.2%).
Concerning gestational intercurrences, anemia was the most prevalent one and was diagnosed in 16.8% of the pregnant women along pregnancy, followed by infection of the urinary tract (IUT: 6.8%); hypertensive syndromes of pregnancy (HSP: 5.8%); and gestational diabetes (GD: 1.8%). Moreover, a percentage of 6.2% of gestational night blindness was verified.
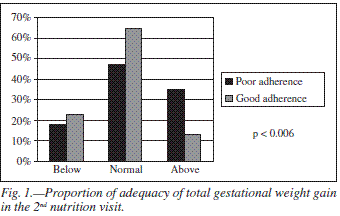
Figures 1 and 2 show the adequacy frequency of total gestational weight gain according to adherence in the second and fourth visits. We observed that in both visits the pregnant women who presented an adherence classified as good or excellent, as regards the nutritional follow-up, showed a higher proportion of adequacy of total gestational weight gain in comparison to those who presented a poor adherence.
It was not observed association between adherence to dietary counseling in 2nd or 4th visits with the nutritionist and socio-demographic characteristics, respectively. It implies that adherence was independent of marital status (p = 0.201; p = 0.730), schooling degree (p = 0.690; p = 0.076), skin color (p = 0.388; p = 0.466), per capita family income (p = 0.269; p = 0.438), use of cigarette (p = 0.07; p = 0.070), alcohol (p = 0.267; p = 0.629) and illicit drugs (p = 0.477; p = 0.299) and basic sanitation condition (p = 0.215; p = 0.960) during pregnancy.
In table III is shown the association between adherence in the second and fourth visits to the dietitian. It is shown that women who presented poor adherence in the second visit had about three times more chances of presenting poor adherence in the fourth visit.
Discussion
Literature is consensual in demonstrating the protective effect of nutritional status adequacy on the motherchild health.19,20
Regarding the care towards pregnant women, the main objective of nutritional assistance addresses the maintenance and recovery of their nutritional status, as well as prevention of intercurrences and promotion of a favorable obstetric outcome.21 In this way, this study aimed to verify to what extent pregnant women followed their personalized dietary planning, organized in a harmonio us and balanced way in every meal and distributed in different timetables along the day.
In this study, a statistically significant increase (p = 0.000) was observed between the mean number of visits to the dietitian during the prenatal period (4.12; SD = 1.67) when compared to the mean obtained in a research conducted in the previously cited maternity hospital between 1999 and 2001 (0.56; SD = 1.35),22 a period where the concept of dietary counseling had not yet been incorporated by the research team. In the same way, the number of visits in the prenatal care assistance also differed, and the mean number of visits was higher (9.03; SD = 1.74) when compared to what had been previously observed (7.52; SD = 2.79).22
Women who presented poor adherence in the second visit showed more chances of presenting poor adherence in the fourth visit, hence reinforcing the importance of an early beginning of the prenatal nutritional assistance helped by dietary counseling. This concept has been implemented since researches have demonstrated the advantages of the adequacy of maternal weight gain still in the first trimester of pregnancy.18,23,24
Besides the importance of total gestational weight gain, prevention of intercurrences in pregnancy also constitutes an important factor in nutritional care. Thus, anemia and HSP, considered as main causes of direct obstetric death,25 as well vitamin A deficiency (VAD), are challenges for the health team, especially for professional dietitians in their control through dietary counseling.
Anemia is related to low birthweight, prematurity, abortion and maternal-child mortality and it is associated with a reduction of 30-45% in favorable obstetric outcome. Moreover, 40% of perinatal maternal deaths are related to this intercurrence.26
As regards HSP, scientific studies address them as potential risk factors for prematurity, low birthweight, Small for Gestational Age newborns (SGA), need of mechanic ventilation, low Apgar in the first and fifth minutes, and perinatal morbidity and mortality.27-30
On the other hand, VAD is also associated with prematurity, low birthweight, to anemia itself and to child morbidity and mortality.31-33
In this study, prevalences of anemia, HSP and VAD were 16.8%, 5.8%, and 6.2%, respectively. Such rates stood out as considerably lower when compared to the values found in other researches in the same maternity hospital: 28.4% of anemia, 18.7% of VAD22 and 10.26% of HSP.28
When analyzing the effect of intervention on the adequacy of total weight gain, it was verified that the percentage of adequacy increased to 43.5% in comparison comparison to findings of the previous study which showed that just 20.4% of pregnant women presented adequate weight at pregnancy term.22 Such result reflects the adequacy of intervention measures applied in the study in order to improve adequacy of weight gain, including detailed nutritional assessment and personalized nutritional counseling.
In view of those findings, we can suggest that the practice of dietary counseling could have enhanced the adherence of pregnant women to the visit schedule as it may have provided higher adherence of the patient to the guidelines and, consequently, to a better adequacy of weight gain. In both cases, it is suggested that counseling may have been associated with a higher satisfaction and motivation of the users as regards the assistance model proposed, which is evidenced by a satisfactory total gestational weight gain and reduction of gestational intercurrences.
Therefore we assume that such aspects have been triggered by the personalized care offered to pregnant women such as the bond created between the woman and the professional. It is this bond that makes dialogue possible entailing the negotiation of the necessary food adjustments to her biological condition comprehending her psychological and sociocultural contexts.
It is assumed that this type of intervention may have contributed to a better understanding of practices peculiar to the food behavior of pregnant women, providing them with reflection on their acts and the willingness to search strategies for changes in their daily lives, modifying their lifestyle and the quality of their food, thus favoring the obstetric outcome.19,20
The adequacy of prenatal nutritional assistance, both from a quantitative and quantitative point of view, presupposes the performance of a professional prepared to identify pregnant women in nutritional risk through an early assessment of their nutritional status as well the conduction of a personalized nutritional guideline. In the same way it is necessary to provide a continuous and frequent assessment of adherence of these women to the proposed planning. Such procedure aims the possibility of readjusting food planning when necessary in order to achieve the optimization of the mother-to-be nutritional status, the improvement of her conditions for delivery and the adequacy of the newborn weight.19,20
Besides being able to translating the practices related to the frequency and composition of the women´s meals as well their weekly weight gain, the proposed instrument, validated according to the outcome of the total gestational weight gain, may be considered an important guide to the dietitian´s behavior.
Current researches have evidenced the association between the anthropometric markers, mainly the total gestational weight gain, and the obstetric outcomes reflecting upon the intercurrences in pregnancy, delivery, breastfeeding and conditions at birth such as birthweight and prematurity.19,20 In view of those findings, the use of such instrument, as early as possible, is of fundamental importance due to the possibility of identifying pregnant women with higher risk of inadequate weight gain at pregnancy term.
Because this way of measuring adherence is an important method to assess the pregnant woman response to dietary counseling, associated with the lack of a criterion which could address this need, the creation of an instrument capable of satisfying such demand is of extreme importance in the area of prenatal nutritional assistance as it can generate an improvement in its quality and functionality.
Taking into account the positive association between adherence to dietary counseling and total gestational weight gain found in the present study, it is assumed that the set of factors embodied by dietary counseling, since the time of the diet guidelines up to more subjective aspects related to the eating act, differently from the conventional medical, hospital centered and technocratic model,34 is of vital importance. It is the nutritional care to pregnant women which will provide a differential component as regards the quality and success of prenatal nutritional assistance and the expected positive obstetric outcome.
Conclusion
The implementation of dietary counseling as a way of approaching pregnant women led them to a higher adherence to nutritional care. The proposition of an instrument capable of assessing the adherence of pregnant women which might be incorporated in the clinical practice of prenatal nutritional assistance showed a positive association with the adequacy of total gestational weight gain, evidencing the importance of prenatal nutritional care based on the principles of counseling during pregnancy.
Acknowledgments
There were no conflicts of interest in this manuscript. All authors participated in all the stages of the elaboration of this paper.
References
1. WHO (World Health Organization). Making a difference in countries - Strategic Approach to Improving Maternal and Newborn Survival and Health. Geneva: WHO; 2006. [ Links ]
2. Berg CJ. Prenatal care in developing countries: the World Health Organization Technical Working Group on antenatal care. JAMWA 1995; 50 (5): 182-186. [ Links ]
3. MS (Ministério da Saúde). Secretaria de Atenção à Saúde. Departamento de Ações Programáticas Estratégicas. Área Técnica de Saúde da Mulher. Pré-natal e Puerpério: atenção qualificada e humanizada - manual técnico/Ministério da Saúde, Secretaria de Atenção à Saúde, Departamento de Ações Programáticas Estratégicas - Brasília: Ministério da Saúde, 163 p., 2005. [ Links ]
4. Chen XK, Wen SW, Yang Q, Walker MM. Adequacy of prenatal care and neonatal mortality in infants born to mothers with and without antenatal high-risk conditions. Aust N Z J Obstet Gynaecol 2007; 47 (2): 122-7. [ Links ]
5. Aguayo VM, Roley JA, Malanzele J, Meershoek SP. Opportunities for improving the quality of nutritional services in the national health system in Mozambique: findings from Manica Province. J Trop Pediatrics 2004; 50 (5): 314-318. [ Links ]
6. Boyd NR, Windsor RA. A formative evaluation in maternal and child health practice: the Partners for Life Nutrition Education Program for pregnant women. Matern Child Health J 2003; 7 (2): 137-43. [ Links ]
7. Villar J, Merialdi M, Gülmezoglu AM, Abalos E, Carroli G, Kulier R, Oni M. Nutritional interventions during pregnancy for the prevention or treatment of maternal morbidity and preterm delivery: an overview of randomized controlled trials. J Nutr 2003; 133: 1606S-1625S. [ Links ]
8. Rodrigues EM, Soares FPTP, Boog MCF. Resgate do conceito de aconselhamento no contexto do atendimento nutricional. Rev Nutr 2005; 18 (1): 119-128. [ Links ]
9. Bueno LGS, Teruya KM. Aconselhamento em amamentação e sua prática. J Pediatr 2004; 80 (5): S126-S130. [ Links ]
10. Kafatos AG, Vlachonikolis IG, Codrington CA. Nutrition during pregnancy: the effects of an educational intervention program in Greece. Am J Clin Nutr 1989; 50: 970-979. [ Links ]
11. Olson CM, Strawderman MS, Reed RG. Efficacy of an intervention to prevent excessive gestational weight gain. Am J Obstet Gynecol 2004; 191: 530-536. [ Links ]
12. Reader D, Splett P, Gunderson EP. Diabetes Care and Education Dietetic Practice Group. Impact of gestational diabetes mellitus nutrition practice guidelines implemented by registered dietitians on pregnancy outcomes. J Am Diet Assoc 2006; 106 (9): 1426-33 [ Links ]
13. Saunders C. Avaliação do impacto da assistência nutricional no resultado obstétrico, 2005. Research registered on Sigma/UFRJ, number 12127. [ Links ]
14. MS (Ministério da Saúde), 1998. Diretrizes e normas regulamentadoras de pesquisas envolvendo seres humanos. Resolução 196/96 do Conselho Nacional de Saúde. Rio de Janeiro: Fundação Oswaldo Cruz. [ Links ]
15. ANVISA. Agência Nacional de Vigilância Sanitária. RDC n. 269, de 22 setembro de 2005. Aprova o regulamento técnico sobre a Ingestão Diária Recomendada (IDR) de proteína, vitaminas e minerais. http://e-legis.anvisa.gov.br/leisref/public/showAct.php (Accessed October 2007). [ Links ]
16. FAO. Food and Agriculture Organization of the United Nations. Human energy requirements. Report of a Joint FAO/WHO/UNU Expert Consultation. FAO Food and Nutrition Technical Report Series 1. Rome, 2004. [ Links ]
17. WHO (World Health Organization). Physical status: the use and interpretation of report anthropometry: report of a WHO Expert Committee. Geneva: WHO; 1995. [ Links ]
18. Padilha PC. Validação de metodologia de avaliação antropométrica de gestantes. (Dissertation) Rio de Janeiro: Instituto de Nutrição Josué de Castro, Universidade Federal do Rio de Janeiro; 2006. [ Links ]
19. Thorsdottir I, Thorsdottir JE, Birgisdottir BE, Geirsson RT. Weight gain in women of normal weight before pregnancy: complications in pregnancy or delivery and birth outcome. Obstet Gynecol 2002; 799-806. [ Links ]
20. Nielsen JN, Gittelsohn J, Anliker J, O´Brien K. Interventions to improve diet and weight gain among pregnant adolescents and recommendations for future research. J Am Diet Assoc 2006; 106 (11): 1825-1840. [ Links ]
21. Rouse, DJ. Potential cost-effectiveness of nutrition interventions to prevent adverse pregnancy outcomes in the developing world. J Nutr 2003; 133 (5 Suppl. 2): 1640S-1644S. [ Links ]
22. Saunders, C. Final report of the research "Avaliação do impacto da assistência pré-natal no resultado obstétrico", Edital 51/2005. CNPq, march/2008. Research registered on Sigma/UFRJ, number 12127. [ Links ]
23. Neufeld LM, Haas JD, Grajéda R, Martorell R. Changes in maternal weight from the first to second trimester of pregnancy are associated with fetal growth and infant length at birth. Am J Clin Nutr 2004; (4): 646-52. [ Links ]
24. Brown JE, Murtaugh MA, Jacobs DRJR, Margellos HC. Variation in newborn size according to pregnancy weight change by trimester. Am J Clin Nutr 2002; 76 (1): 205-9. [ Links ]
25. MS (Ministério da Saúde). Secretaria de Atenção à Saúde. Departamento de Ações Programáticas Estratégicas. Manual dos comitês de mortalidade materna/Ministério da Saúde, Secretaria de Atenção à Saúde, Departamento de Ações Programáticas Estratégicas. - 3. ed. - Brasília: Editora do Ministério da Saúde, 104 p. (Série A. Normas e Manuais Técnicos), 2007. [ Links ]
26. WHO (World Health Organization). Iron deficiency anaemia: assessment, prevention, and control: a guide for programme managers. Geneva: WHO; 2001. [ Links ]
27. Ray JG, Burrows RF, Burrows EA, Vermeulen MJ. MOS HIP: McMaster outcome study of hypertension in pregnancy. Early Hum Dev 2001; 64 (2): 129-143. [ Links ]
28. Oliveira CA, Lins CP, Sá RAM, Netto HC, Bornia RG, Silva NR, Amim Junior J. Síndromes hipertensivas da gestação e repercussões perinatais. Rev Bras Saúde Matern Infant 2006; 6 (1): 93-98. [ Links ]
29. Habli M, Levine RJ, Qian C, Sibai B. Neonatal outcomes in pregnancies with preeclampsia or gestational hypertension and in normotensive pregnancies that delivered at 35, 36, or 37 weeks of gestation. Am J Obstet Gynecol 2007; 197 (4): 406.e1-406.e7. [ Links ]
30. Savona-Ventura C, Buttigieg GG, Grima S. Outcomes of hypertensive obstetric patients in the Maltese Islands. Int J Gynaecol Obstet 2008; 101 (2): 189-191. [ Links ]
31. Radhiha MS, Bhaskaram P, Balakrishna N, Ramalakshmi BA, Devi S, Kumar BS. Effects of vitamin A deficiency during pregnancy on maternal and child health. Int J Gynaecol Obstet 2002; 109 (6): 689-693. [ Links ]
32. Tielsch JM, Rahmathullah L, Katz J, Thulasiraj RD, Coles C, Sheeladevi S, Prakash K. Maternal night blindness during pregnancy is associated with low birthweight, morbidity, and poor growth in South India. J Nutr 2008; 138: 787-792. [ Links ]
33. Christian P, West Jr KP, Khatry SK, Leclerq C, Kimbrough-Pradhan E, Katz J, Shrestha SR. Maternal night blindness increases risk of mortality in the first 6 months of life among infants in Nepal. J Nutr 2001; 131 (5): 1510-1512. [ Links ]
34. Serruya SJ, Cecatti JG, Lago TG. O Programa de Humanização no Pré-natal e Nascimento do Ministério da Saúde no Brasil: resultados iniciais. Cad Saúde Pública 2004; 20 (5): 1281-1289. [ Links ]
![]() Correspondence:
Correspondence:
Beatriz Della Libera.
Departamento de Nutrição e Dietética.
Instituto de Nutrição Josué de Castro.
Centro de Ciências da Saude.
Universidade Federal do Rio de Janeiro.
Rua Maestro Arturo Toscanini, 145/201.
CEP 21910-260 Tauá , Rio de Janeiro, RJ, Brasil.
E-mail: bdellalibera@hotmail.com
Recibido: 13-XII-2009.
1a Revisión: 29-XII-2009.
Aceptado: 6-I-2010.