Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Nutrición Hospitalaria
versión On-line ISSN 1699-5198versión impresa ISSN 0212-1611
Nutr. Hosp. vol.26 no.3 Madrid may./jun. 2011
The use of biochemical and immunological parameters in nutritional screening and assessment
Utilidad de los parámetros bioquímicos e inmunológicos en la evaluación y cribado nutricional
A. González Madroño1, A. Mancha1, F. J. Rodríguez2, J. I. de Ulibarri1 and J. Culebras3
1Sección de Nutrición Clínica y Dietética. Hospital Universitario de La Princesa.
2Instituto de Investigación del Hospital Universitario de La Princesa.
3Servicio de Cirugía. Complejo Asistencial de la Universidad de León. Instituto de Biomedicina (IBIOMED). Universidad de León. España.
VEGENAT, SA. For their continued support for our research in the early detection of hospital malnutrition.
ABSTRACT
Objective: To evaluate the relationship between serum albumin, total cholesterol and total lymphocyte count with two nutritional assessment methods, to verify if their use is justified in nutritional screening tools.
Methods: 101 patients admitted to medical/surgical wards underwent the SGA and the Full Nutritional Assessment (FNA). Blood test which included serum albumin, total cholesterol and total lymphocyte count (TLC), were made. Percentage of weight loss and BMI were calculated. An Anova test was done to measure the differences in the mean levels of the three parameters for the nutritional status evaluated by SGA and FNA. The probability of a patient being malnourished in the four ranges established for each parameter was calculated, as well as the relationship between the ranges and the percentage of weight loss and BMI. Sensitivity and specificity were calculated and the corresponding ROC curves, using SGA as gold standard.
Results: Prevalence of undernutrition is 43.6% and 44.6% for SGA and FNA respectively. Mean levels of the three parameters decrease as the undernutrition degree increases (p < 0.005 for all cases). The probability of a patient being malnourished gets higher as parameter lowers (p = 0.000 for all cases). Total cholesterol shows a relationship with BMI < 18.5 and presence/absence of weight loss (p = 0.074 and p = 0.002 respectively). The area under ROC curves are albumin (0.823), cholesterol (0.790) and TLC (0.758) respectively.
Conclusions: The analytical parameters analyzed show a statistically significant relationship with the nutritional status. Therefore, they are suitable for use in nutritional screening.
Key words: Undernutrition. Malnutrition. Nutritional screening. Serum albumin. Total cholesterol. Total lymphocite count.
RESUMEN
Objetivo: evaluar la relación entre albúmina sérica, colesterol total y linfocitos totales y dos métodos de evaluación nutricional, para verificar si su uso en las herramientas de cribado nutricional está justificado.
Métodos: a 101 pacientes de servicios médicos y quirúrgicos se les realizó el SGA y la Valoración del Estado nutricional Completa (VEN). Se les realizaron análisis de albúmina sérica, colesterol total y linfocitos totales. Se calculó el porcentaje de pérdida de peso y el IMC. Las diferencias entre los niveles medios de los tres parámetros en los distintos niveles nutricionales evaluados por SGA y VEN se hizo mediante el test de ANOVA. Se calculó la probabilidad de estar desnutrido en los cuatros rangos establecidos para cada parámetro, así como la relaciones entre esos rangos y el porcentaje de pérdida de peso y el IMC. Se calculó la sensibilidad y especificidad y sus curvas ROC correspondientes, tomando el SGA como gold standard.
Resultados: La prevalencia de desnutrición es 43,6% (SGA) y 44,6% (VEN). Los valores medios de los tres parámetros disminuyen según aumenta el grado de desnutrición (p < 0,005). La probabilidad de que un paciente esté desnutrido aumenta a medida que disminuyen los niveles de los parámetros (p = 0,000 para los tres). El colesterol total se relaciona con el IMC < 18,5 y con la presencia/ausencia de pérdida de peso (p = 0,790 y p = 0,002 respectivamente).
Conclusiones: Los parámetros analíticos analizados muestran una relación significativa con el estado nutricional y por tanto son válidos para su uso en el cribado de desnutrición.
Palabras clave: Desnutrición. Malnutrición. Cribado nutricional. Albúmina sérica. Colesterol total. Linfocitos totales.
Abbreviations
SGA: Subjective Global Assessment.
FNA: Full Nutritional Assessment.
TLC: Total Lymphocyte Count.
BMI: Body Mass Index.
ANOVA: Analysis of Variance.
VEN: Valoración del Estado Nutricional.
IMC: Índice de Masa Corporal.
ASPEN: American Society of Parenteral and Enteral Nutrition.
MNA: Mini Nutritonal Assessment.
NRS-2002: Nutritional Risk Index 2002.
MUST: Malnutrition Universal Screening Tool.
BAPEN: British Association of Parenteral and Enteral Nutrition.
ESPEN: European Society of Parenteral and Enteral Nutrition.
NRI: Nutritional Risk Index.
INA: Instant Nutritional Index.
SENPE: Sociedad Española de Nutrición Parenteral y Enteral.
Na: sodio.
K: potasio.
Cl: cloro.
g/dL: gramos/decilitro.
mg/dL: miligramos/decilitro.
Cell/mL: células/mililitro.
SD: Standard Deviation.
AUC: Area Under de Curve.
Alb: Albumin.
Sens: Sensibility.
Specf: Specificity.
LOS: Length of Stay.
UN: Undernutrition.
Introduction
For almost three decades, it has been recognized that hospital patients frequently present undernutrition or have a high probability of developing it due to their underlying disease and/or treatment received. The classic works, published in 1974 and 1976 by Bristian and col., reported that about 50% of patients admitted to a university hospital, in surgical and medical services, presented some degree of undernutrition varying from 45% to 54%.1,2
More recent studies continue to prove that the prevalence of undernutrition upon admission to hospital remains high, although the reported figures are quite variable and generally oscillate between 30% and 60%, depending on the diagnostic criteria employed and the specific population studied.3-9
Clinical undernutrition goes further than hospital undernutrition. It persists after discharge, extends length of stay and convalescence, increases sanitary costs and frequently leads to readmissions.10-16
There are many tools for nutritional screening and assessment. The most commonly used and widely validated are:
Subjective Global Assessment (SGA) suggested by ASPEN for nutritional Assessment,17 the Mini Nutritional Assessment (MNA) developed for elderly patients,18 Nutritional Risk Screening-2002 (NRS-2002),19 and the Malnutrition Universal Screening Tool (MUST) developed by the Malnutrition Advisory Group of BAPEN,20 all three recommended by the ESPEN to detect the prevalence of malnutrition.21 All of them are based on different clinical information such as body mass index (BMI), weight loss, intakes changes, eating difficulties, severity of disease, etc.
In an ideal situation personnel in charge of the patient assess the nutritional risk using one of these screening tools, and when malnourished patients are identified they are referred to the nutritional unit or team, and a nutritional intervention is decided. In practice this is difficult to carry out due to the lack of staff and consciousness of personal in charge of the patient so hospital undernutrition remains under diagnosed and therefore not treated.
In the past, analytical parameters were frequently used in nutritional indexes, combined with other nutritional status parameters, and they proved to be valid and reliable for this purpose. However, in the last years, analytical parameters have not been used for nutritional screening because many authors argue that they reflect severity of desease rather than nutritional status.22 Serum albumin and TLC are the most commonly used; the Nutritional Risk Index (NRI) is based on serum albumin and the ratio of actual to usual weight,23 the equation developed by Elmore includes serum albumin, TLC and % weight loss for nutritional screening,24 the Instant Nutritional Assessment (INA) combines both serum albumin and TLC for the screening.25
The aim of this study was to evaluate the relationship between serum albumin, total cholesterol and total lymphocyte count with different nutritional assessment methods and to verify if they are valid to be used in nutritional screening tools.
Methods
Subjects
The study was carried out in Hospital Universitario de la Princesa, a 500 beds hospital, only for adults, with approximately 17,000 patients admitted per year. Inclusion and exclusion criteria are as follows: 101 patients were randomly selected from all departments except from Psychiatric, Hemodialysis and Intensive Care Units. Patients with no routine analysis done during their first week of hospitalization, those who were admitted for a diagnostic test or a short term stay, or those who didn't sign the inform consent were excluded from the study.
Assessments of nutritional state
Selected patients underwent two different nutritional assessments methods during their first week of hospitalization:
Subjective Global Assessment (SGA), is made by a nutritionist of the Dietetic Unit. The SGA assesses nutritional status based on clinical history and physical examination. The history records data related to weight changes in the last six months, modification on diet intakes, presence of gastrointestinal symptoms and functional capacity. The physical examination includes: presence of loss of subcutaneous fat, muscle wasting, ankle oedema and ascites. The exam classifies patients as well nourished, moderately or suspected of being undernourished and severely malnourished.17
Full Nutritional Assessment (FNA), is made by a physician of the Dietetic Unit. It is based on the SENPE (Sociedad Española de Nutrición Enteral y Parenteral) protocol for Nutritional Assessment. It includes:
Anamnesis: principal diagnose, admission's reason, food allergies and/or intolerances, metabolic disorders, presence of gastrointestinal symptoms, changes on diet intakes, digestive loss, personal records, previous surgeries, treatment.
Physical examination: general look/aspect, loss of subcutaneous fat, muscle wasting, oedema, ascites, mucocutaneous lesions and changes in skin appendages.
Anthropometrics: Patients were weighed, whenever clinically possible, using the scale available, they were asked about their height and an estimated weight six months prior to admission. Percentage of weight loss was calculated, as well as body mass index (BMI).
This assessment classifies patients as well nourished, moderately or suspected of being malnourished and severely malnourished.
Blood test: includes serum determinations of albumin, total cholesterol, total lyphocyte count, hemogram, pre-albumin, transferrin, iron, lipids profile, serum and urine ions (Na, K, Cl) and hepatic, renal and endocrine-metabolic function.
Analytical variables and ranges
The three parameters analyzed (serum albumin, total cholesterol and total lymphocyte count) are classified according to their normality or deficiency levels in four categories as shown in table I. Serum albumin (g/dL) is used as an indicator of protein reserves,26-28 total cholesterol (mg/dL) is used as a caloric depletion parameter,29-30 and finally, total lymphocyte (Cell/mL) count is used as an indicator of loss of immune defences caused by undernutrition.31-33 Serum albumin and total cholesterol were analyzed by a "Roche Modular Analyzer", and total lymphocyte count was analyzed by a "Roche SYSMES Hematological".
Statistical analysis
Categorical variables were described as the number of cases and percentages and age with the mean ± standard deviation (SD). The association level between the results of the SGA and the FNA was measured using the X2 Test, and the agreement degree was measured by contingency tables using the kappa index.34
The relationship between the three parameters and the nutritional status was measured as follows:
First, an ANOVA test was carried out to test the significance of the difference in the mean levels of albumin, cholesterol and lymphocytes for the three nutritional status evaluated by SGA and FNA.
Second, the probability of a patient being malnourished in the four ranges established for each parameter was calculated using contingency tables. For this analysis, patients were classified as malnourished (if moderately or severely undernorished) or not malnourished (if well nourished).
Third, the relationship between the three parameters and BMI and weight loss was tested by an ANOVA test. BMI was classified into two categories: BMI > or < than 18.5 as these ranges/limits are considered as an indicators of malnutrition, and weight loss was categorized in presence or absence.
Fourth, to compare the malnutrition diagnostic efficacy of the biochemical and immunological parameters studied, different efficacy rates were calculated (sensitivity, specificity, and their corresponding confidence intervals) for the different cut points and the corresponding ROC curves and Kruskall-Wallis tests). SGA was used as the gold standard.
The level of significance was established for a probability of 0.05. All tests were performed using SPSS package vs. 13.0.
Results
Subject
101 patients were studied, most of them hospitalized in medical wards (79.21%). Sample description is shown in table II. Of these patients 5 (4.9%) had no information about BMI, and 14 (13.9%) had none about weight loss. From those with data available, only 18.8% had a BMI lower than 20, and 53.4% had lost weight, and almost 18% had a weight loss greater than 10%.
Nutritional status evaluated by SGA and FNA is shown in table III. Note that the prevalence of undernutrition (moderate and severe) is close to 45% of the patients for both methods. SGA and FNA present a high concordance degree when evaluating undernutrition, as shown by kappa index = 0.787.
Mean levels of the three parameters for the nutritional status evaluated by SGA is shown in table IV. Notice that a decreased trend can be observed for the three of them as the undernutrition degree gets higher, and that this trend is statistically significant in all cases.
The probability of a patient being malnourished gets higher the lower the range for each parameter (table V), and this trend is statistically significant for the three parameters.
When analyzing the relationship of the parameters with BMI and weight loss (table VI), we can observe that some kind of relation exist for the three of them, so that the mean levels of albumin, cholesterol, and TLC are higher for individuals with a BMI > 18.5 or with no weight loss than for those with BMI < 18.5 and some weight loss, but these differences get significant levels only in the case of serum cholesterol.
Sensibility and specificity obtained for the three variables are shown in table VII.
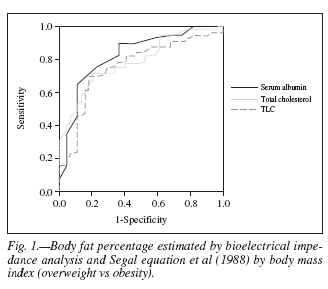
The ROC curve of the albumin shows an area under the curve (AUC) of 0.823 (95% CI 0.740-0.907), the AUC for total cholesterol is 0.790 (95% CI 0.703-0.876) and for TLC is 0.758 (95% CI 0.661-0.855) (fig. 1).
Discussion
From the first studies published about the so called hospital undernutrition1-3 to the more recent ones,6-8 undernutrition prevalence rates have maintained a considerably high rate. There are multiple causes for that malnutrition, as the illness process itself, the hospitalization, the diagnostic and therapeutical procedures, which very often include fasting and the lack of interest about a patient's nutritional status from the sanitary staff. Prevalence of malnutrition in our hospital is very high according to the SGA and FNA (43.6% and 44.6% respectively), and these results are consistent with other literature reports.35,36
Another reason for the continuation of these high undernutrition rates might be the lack of quick and cheap nutritional screening tools, applicable periodically to all inpatient populations, to alert about this serious sanitary issue. The aim of a nutritional screening is to identify malnourished patients, or those at risk of malnutrition, who will need a further and more complete nutritional assessment, in order to start a nutritional support as soon as possible, if needed. This screening should be simple and applicable to all inpatients until the clinic process has finished/ is over (illness, hospitalization, therapy and complications).
The usefulness of the analytical parameters for nutritional screening has been widely discussed. In the past, they were commonly used for this purpose, combined with other analytical information (IRN, IPN, etc.). In the last years they have been replace by nutritional screening tools based only on clinical information such as the SGA (recommended by the ASPEN), the NRS-2002 (recommended by ESPEN) and the MUST (BAPEN). Nevertheless, all of these tools must be done through a direct interview and examination of the patient; therefore, they can hardly be applied to all inpatients and repeated during the hospital stay, so that this aspiration of the Council of Europe37 and the ESPEN21 considerably elevates staff numbers and time requirements.
The main reason for not using the analytical parameters in nutritional screening is that some authors made objections to these parameters as indicators of nutritional status when present in illness or aggressive treatment. For this reason, we wanted to study the behavior of the analytical parameters, specifically in these situations.
The three analytical parameters analyzed in this study have been selected among those more frequently used in clinical practice, to indicative the patient's nutritional balance. The three of them show a good association with the nutritional status assessed by the SGA and FNA, so that as the levels of each one of the parameters get lower the patient's undernutrition degree gets higher, as can be observed in tables IV and V.
The dynamics of the cut points adjust to what would be expected (table VII). The three parameters show a considerably high sensitivity in the first cut point, and it is the albumin that, at this point, shows the maximum specificity (Alb > 3,5, sens = 0.89, spcf = 0.65). Total cholesterol and total lymphocyte count present, at that point, a much lower specificity value (0.46 in both cases). As it would be expected sensibility lowers for the three variables as the cut points go to lower values, and specificity increases to 1 in the case of albumin > 2.5 mg/dL. The choice of any of the cut points will depend upon how these parameters will be used.
As it can be observed in figure 2, the three parameters show a wide area under the curve (AUC), which indicates that their precision in detection of undernutrition is good.
Many authors reject albumin as an indicator of nutritional status, due to its long midlife (20 days). In clinical practice that midlife shortens immediately depending upon the seriousness of the clinical process. A hemorrhage or lymphorrhage can cause a dramatical decrease in minutes of the albumin level, as it falls in hours in a surgery or a chemotherapy or steroid treatment. Another reason to reject the use of albumin, is that serum albumin levels can be affected by many factors other than malnutrition such as inflammation, some drugs (corticosteroids, insulin, thyroid hormone, etc.) renal and liver disease, all of which result in a low sensitivity and specificity to changes on nutritional intake.38 Many studies have demonstrated the predictive value of hypoalbuminemia for morbidity, mortality, increase of LOS (length of stay) and costs.26-28 Therefore, hipoalbuminemia is often considered as an indicator of the illness severity rather than the nutritional status. However, there is an indirect relationship between inflammation (and the consequent hypoalbu-minemia) with nutritional status. Inflammation contributes to an increase in net protein loss caused by catabolism, and also induces anorexia, reducing the probability that a patient will get an adequate intake to his requirements, thus accelerating the undernutrition process.39 In the present study, we have found a direct and significant relationship between serum albumin and nutritional status, which agrees with other literature reports.40-42 For this reason, even though serum albumin can be affected by many others non nutritional factors (illness, hospitalization or therapeutical treatments) it presents a strong relationship with nutritional status, and therefore it can not be ruled out for use in nutritional screening.
In this study, we suggest total cholesterol as an indicator of the patient's energetic reserves,29,30 as the illness and therapeutical procedures frequently compromise the patient's caloric balance. When the patient presents a caloric malnutrition, a weight loss and a drop in the BMI are observed. In our clinic experience we have observed how serum cholesterol lowers at caloric depletion, even before a weight loss or other anthropometrical changes can be observed. We have found a relationship between total cholesterol and BMI and the percentage of weight loss (table VI), which would confirm its usefulness as an indicator of the patient's caloric reserves.
Undernutrition induces immunological changes, such as a drop in total lymphocyte count, which increases frequency and severity of infection. This accounts for much of the morbidity and mortality associated with malnutrition. Total lymphocyte count has been suggested as a useful indicator of the nutritional status and outcomes, and it is quickly done and appropriate for all age groups.31-33
BMI is frequently used as an indicator of a patient's nutritional status, considering lack of undernutrition if BMI > 20. We think that BMI itself is not a good indicator of nutritional status. When analyzing the results obtained in the present study, it can be observed that 80.2% of patients have a BMI > 20, and only 10,4% have a BMI < 18, while the prevalence of undernutrition found by SGA is 44%. Results concerning percentage of weight loss are closer to the prevalence of undernutrition in our study, since 46% of the patients referred lost weight. Therefore, SGA is more useful than BMI to detect undernutrition, These results are in agreement with other studies.43
Apart from their sensibility and specificity rates, a remarkable advantage of the analytical parameters for nutritional screening is that they are already available in every patient's clinical file, this information is obtained at admission, during the hospital stay and during treatment. When planning the use of nutritional screening parameters, one must go to the clinical data bases to retrieve the information. Specific software could be utilized by clinicians to obtain nutritional risk measurements. The need for further nutritional assessment and/or needed intervention would be immediately determine. Depending on the result of the screening's result, further nutritional assessment and early and adequate nutritional intervention can be done.
Conclusions
Analytical parameters analyzed in this study show a statistically significant relationship with the nutritional status evaluated by SGA and FNA. Total cholesterol correlates with BMI and percentage of weight loss, and therefore it can be consider as an indicator of caloric undernutrition. The results obtained in the present study support the use of the analytical parameters in computer screening tools for the early detection of undernutrition.
For these reasons, we propose bringing back the use of analytical parameters along with computer tools for automatic screening of patient undernutrition. With the computer tools it is possible to reach a larger number of patients during their entire clinical process. The tools permit quick and easy detection of variations during treatment as well as patient complications. What we propose would result in saving of money, personnel, and time for the hospital. In addition to its efficiency, this approach would be more patient friendly.
Acknowledgments
Our acknowledgments to:
Ana Diaz, Clinical Analysis Section Chief and Central Clinical Laboratory and Informatics Coordinator, for her invaluable help facilitating the availability of analytical data necessary for the study.
Guillermo Fernandez. Medical expert systems, always attentive to improving the care quality for our patients.
References
1. Bristian BR, Blackburn GL, Hallowell E, Heddle R. Protein status on general surgical patients. JAMA 1974; 230: 858-860. [ Links ]
2. Bristian BR, Blackburn GL, Vitale J, Cochran D, Naylor J. Prevalence of malnutrition in general medical patients. JAMA 1976; 235: 1567-1570. [ Links ]
3. Kamath SK, Lawer M, Smith AE, Kalat T, Smith AR. Hospital malnutrition: a 33-hospital screening study. J Am Diet Assoc 1986; 86: 203-6. [ Links ]
4. McWhirter JP, Pennington CR. Incidence and recognition of malnutrition in hospital. BMJ 1994; 308: 945-8. [ Links ]
5. Corish CA, Kennedy NP. Protein-energy undernutrition in hospital in-patients. Br J Nutr 2000; 83: 575-91. [ Links ]
6. Waitzberg DL, Caiaffa WT, Correira MI. Hospital malnutrition: the Brazilian national survey (IBRANUTRI): a study of 4000 patients. Nutrition 2001; 17: 573-80. [ Links ]
7. Fettes SB, Davison HI, Richardson RA, Pennington CR. Nutritional status os elective gastrointestinal surgery patients pre-and post-operatively. Clin Nutr 2002; 21: 249-254. [ Links ]
8. Lamb CA, Parr J, Lamb EI, Warren MD. Adult malnutrition screening, prevalence and management in a United Kingdom hospital: cross-sectional study. Br J Nutr 2009; 102 (4): 571-5. [ Links ]
9. Coelho AK, Rocha FL, Fausto MA. Prevalence of undernutrition in elderly patients hospitalized in a geriatric unit in Belo Horizonte, MG, Brazil. Nutrition 2006; 22 (10): 1005-11. [ Links ]
10. Anderson CF, Moxness K, Meisser J, Burrit MF. The sensitivity and specificity of nutrititon-related variables in relationship to the duration of hospital stay and the rate of complications. Mayo Clin Proc 1984; 59: 477-83. [ Links ]
11. Tucker HN, Miguel SG. Cost containment through nutrition intervention. Nutr Rev 1996; 54: 477-83. [ Links ]
12. Chima CS, Barco K, Dewitt ML, Maeda M, Teran JC, Mullen KD. Relationship of nutritional status to length of stay, hospitals costs, and discharge status of patiens hospitalized in the medicine service. J Am Diet Assoc 1997; 97: 975-8. [ Links ]
13. Norman K, Pichard C, Lochs H, Pirlich M. Prognostic impact of disease-related malnutrition. Clin Nutr 2008; 27 (1): 5-15. [ Links ]
14. Green CJ: Existence, causes and consequences of disease-related malnutrition in the hospitals and the community, and clinical and financial benefits from nutritional intervention. Clin Nutr 1999; 18 (Suppl.): 3-28. [ Links ]
15. Amaral TF, Matos LC, Tavares MM, Subtil A, Martins R, Nazare M, Sousa Pereira N. The economic impact of disease-related malnutrition at hospital admission. Clin Nutr 2007; 26 (6): 778-84. [ Links ]
16. Goiburu ME, Goiburu MM, Bianco H, Diaz JR, Alderete F, Palacios MC et al. The impact of malnutrition on morbidity, mortality and length of stay in trauma patients. Nutr Hosp 2006; 21 (5): 604-10. [ Links ]
17. Detsky AS, Smalley PS, Chang J. The rational clinical examination. Is this patient malnourished? JAMA 1994; 271: 54-8. [ Links ]
18. Vellas B, Guigoz Y, Garry PJ, Nourhasemi F, Bennahum D, Lauque S et al. The Mini Nutricional Assessment (MNA) and its use in grading the nutricional state of elderly patiens. Nutrition 1999; 15 (2): 116-22. [ Links ]
19. Kondrup J, Rasmussen HH, Hamberg O, Stanga Z. Nutritional risk screenig (NRS 2002): a new method based on an analysis of controlled clinical trials. Clin Nutr 2003; 22: 321-336. [ Links ]
20. Sttratton RJ, Hackston A, Longmore D y cols. Malnutrition in hospital outpatients and inpatients: prevalence, concurrent validity and ease of use of the "malnutrition universal screening tool" (MUST) for adults. Br J Nutr 2004; 92: 799-808. [ Links ]
21. Kondrup J, Allison SP, Elia M, Vellas B, Plauth M. ESPEN Gudelines for Nutrition Screening 2002. Clin Nutr 2003; 22 (4): 415-421. [ Links ]
22. Furhman MP, The Albumin-Nutrition Connection: Separating Myth from Fact. Nutrition 2002; 18: 199-200. [ Links ]
23. Perioperative total perenteral nutrition in surgical patients. The Veterans Affairs Total Parenteral Nutrition Group. N Engl J Med 1991; 325: 525-532. [ Links ]
24. Elmore MF, Wanger DR, Knoll DM, Eizember L, Oswalt MA, Glowinsky FA et al. Developing an effective adult nutrition screening tool for a community hospital. J Am Diet Assoc 1994; 94: 113-118, 1121. [ Links ]
25. Seltzer MH, Bastidas JA, Cooper DM, Engler P, Slocum B, Fletcher HS. Instant nutritional assessment. JPEN 1979; 3 (3): 157-9. [ Links ]
26. Gibbs J, Cull W, Henderson W, Daley J, Hur K, Khuri SF. Preoperative serum albumin level as a predictor of operative mortality and morbidity: results from the National VA Surgical Risk Study. Arch Surg 1999; 134: 36-42. [ Links ]
27. Harvey KB, Moldawer LL, Bristian BR, Blacburn GL. Biological maesures for the formulations of a prognostic index. Am J Clin Nutr 1981; 34: 2013-2022. [ Links ]
28. Sullivan DH, Walls RC, Bopp MM. Protein-energy undernutrtion and the risk of mortality within one year of hospital discharge: a follow up study. J Am Geriatr Soc 1995; 43: 507-12. [ Links ]
29. López-Martínez J, Sanchez-Castilla M, García-de-Lorenzo A. Hypocholesterolemia in critically ill patients. Intensive Care Med 2000; 26: 259-60. [ Links ]
30. Reuben DB, Ix JH, Grendale GA et al. The predictive value of combined Hypoalbuminemia and hypocholesterolemia in high functioning community-dwelling older persons: Mac Arthur Studies of succesful aging. J Am Geriatr Soc 1999; 47: 402-406. [ Links ]
31. Shronts EP. Basic concepts of inmunology and its aplication to clinical nutrition. Nutr Clin Pract 1993; 8: 177-83. [ Links ]
32. Casey J, Flinn WR, Yao JS et al. Correlation of inmune and nutritional status with wound complications in patients undergoing vascular operations. Surgery 1983; 93: 822-7. [ Links ]
33. Omran ML, Morley JE, Assessment of protein energy malnutrition in older persons, part II: Laboratory evaluation. Nutrition 2000; 16: 131-140. [ Links ]
34. Fleiss JL. Statistical methods for rates and proportions (2nd ed.) New York: Wiley, 1981, pp. 217-234. [ Links ]
35. Vidal A, Iglesias MJ, Pertega S, Ayúcar A, Vidal O. Prevalence of malnutrition in medical and surgical wards of a university hospital. Nutr Hosp 2008; 23 (3): 267-7. [ Links ]
36. Lamb CA, Parr J, Lamb EI, Warren MD Adult malnutrition screening, prevalence and management in a United Kingdom hospital: cross-sectional study. Br J Nutr 2009: 102 (4): 571-5. [ Links ]
37. Council of Europe. Committee of Experts on Nutrition, Food Safety and Consumer Protection. Food and Nutritional Care in Hospitals: How to Prevent Undernutrition. Report ans recommendations. Strasbourg: Council of Europe Publisshin; 2002. ISBN: 92-871-5053-2. [ Links ]
38. Furhman MP, The Albumin-Nutrition Connection: Separating Myth from Fact. Nutrition 2002; 18: 199-200. [ Links ]
39. Fuhrman MP, Charney P, Mueller CM. Hepatic Proteins and Nutrition Assessment. J Am Diet Assoc 2004; 104: 1258-1264. [ Links ]
40. Brugler L, Stankovic AK, Schlefer M, Bernstein L . A simplified nutrition screen for hospitalized patients using readily available laboratory and patient information. Nutrition 2005; 21: 650-658. [ Links ]
41. Serum albumin concentration and clinical assessements of nutritional status in hospitalized older people: different sides of different coins? J Am Geriatr Soc 2002; 50: 631. [ Links ]
42. Sungurtekin H, Sungurtekin U, Hanci V, Erdem E. Comparison of two nutrition assessment techniques in hospitalized petients. Nutrition 2004; 20; 428-432. [ Links ]
43. Baccaro F, Sánchez A. Comparison between subjective global assessment and body mass index in the evaluation of hospital hyponutrition. Nutr Hosp 2008; 23 (6): 628-9. [ Links ]
![]() Correspondence:
Correspondence:
A. González Madroño.
Hospital Universitario de La Princesa.
Sección de Nutrición Clínica y Dietética.
C/ Diego de León, 62.
28006 Madrid.
E-mail: ana_madrono@yahoo.com
Recibido: 7-II-2011.
Aceptado: 9-II-2011.