My SciELO
Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO -
 Access statistics
Access statistics
Related links
-
 Cited by Google
Cited by Google -
 Similars in
SciELO
Similars in
SciELO -
 Similars in Google
Similars in Google
Share
Nutrición Hospitalaria
On-line version ISSN 1699-5198Print version ISSN 0212-1611
Nutr. Hosp. vol.28 n.5 Madrid Sep./Oct. 2013
https://dx.doi.org/10.3305/nh.2013.28.5.6693
ORIGINAL / Otros
Prolonged fasting with fluid therapy is related to poorer outcomes in medical patients
El ayuno prolongado con sueroterapia se asocia con peores resultados clínicos en pacientes médicos
Georgios Kyriakos, Alicia Calleja-Fernández, Dalia Ávila-Turcios, Isidoro Cano-Rodríguez, María D. Ballesteros Pomar and Alfonso Vidal-Casariego
Sección de Endocrinología y Nutrición. Complejo Asistencial Universitario de León
ABSTRACT
Background and objective: An inadequate fluid therapy can worsen the outcomes of surgical patients, but there are no data in medical patients. The aim of this study was to determine the adequacy of fluid therapy in hospitalised patients of medical wards, and its influence on outcomes.
Methods: Cross-sectional study including nil-per-os patients admitted in medical wards of the Complejo Asis-tencial Universitario de León. The administered fluid therapy was compared with the standardised requirements. Nutritional status was evaluated with Subjective Global Assessment. Fasting was considered inappropriate if it lasted > 7 days in well-nourished, and >5 days in malnourished patients if nutritional support had not been provided.
Results: Fluid therapy lasted 4 (IQR = 2) days, and fasting was inadequately maintained in 27% of patients. Fluid requirements were correctly fulfilled, but patients received an excess of sodium (+58.4%) and chloride (+62.2%), and potassium administration was insufficient (-35.1%). Glucose supply was 68.8 (29.2) g/d, and 99% received < 130 g/d. Patients with an inadequate duration of fasting had a longer hospital stay after adjusting for sex, age, nutritional status, infused volume, electrolytes, glucose and diseases. Only malnutrition predicted mortality during hospitalisation (OR 10.5; 95%CI 1.3 to 83.2), when multivariate analysis was performed.
Conclusions: Fasting medical patients receive an inadequate supply of glucose and electrolytes. Prolonged fluid therapy and malnutrition may worsen the outcomes of these patients, independently of other conditions like age or diseases.
Key words: Fluid therapy. Malnutrition. Fasting. Subjective Global Assessment.
RESUMEN
Introducción y objetivo: La sueroterapia inadecuada en pacientes quirúrgicos puede empeorar sus resultados clínicos, pero para pacientes médicos no existen datos publicados. El objetivo de este estudio es determinar la adecuación de la sueroterapia en pacientes médicos hospitalizados y valorar su repercusión en los resultados clínicos.
Métodos: Estudio transversal realizado en pacientes en dieta absoluta de servicios médicos del Complejo Asistencial Universitario de León. Se comparó el aporte de sueros con los requerimientos estandarizados. El estado nutricional se valoró mediante la Valoración Global Subjetiva. Se consideró inadecuado un ayuno con suero como único aporte durante > 7 días en bien nutridos y > 5 días en desnutridos.
Resultados: La duración de la sueroterapia fue 4 (RIQ = 2) días y el 27% de los pacientes permanecieron en dieta absoluta con sueros más tiempo del adecuado. El aporte de líquidos fue correctamente administrado pero los pacientes recibieron un exceso de sodio (+58,4%) y cloro (+62,2%) y una administración insuficiente de potasio (-35,1%). El aporte de glucosa fue de 68,8 (29,2) g/d y el 99,0% de los pacientes recibieron menos de 130 g/día de glucosa. Los pacientes con duración inadecuada del ayuno con sueros tuvieron una estancia hospitalaria más prolongada [22,0 (RIQ = 13,0) vs 13,0 (RIQ = 11,0) días; p = 0,001], una vez ajustado por sexo, edad, estado nutricional y aporte de volumen, iones y glucosa. Al realizar el análisis multivariante solo la malnutrición fue un predictor de mortalidad durante la hospitalización (OR 10,5; 95%CI 1,3 to 83,2).
Conclusiones: El paciente en dieta absoluta recibe un aporte inadecuado de iones y glucosa. La sueroterapia prolongada y la malnutrición pueden empeorar los resultados clínicos de estos pacientes de manera independiente de otras condiciones como la edad o enfermedad.
Palabras clave: Sueroterapia. Malnutrición. Ayuno. Valoración Global Subjetiva.
Abbreviations
NCEPOD: National Confidential Enquiry into Perioperative Deaths.
MDRD: Modification of Diet in Renal Disease.
SGA: Subjective Global Assessment.
Introduction
Intravenous fluid therapy has been used for almost 200 years and still remains as an essential part of patient care during hospitalisation, deserving the title of the quintessential cross-disciplinary subject of Medicine.1,2 The clinical situations in which intravenous fluids are used are myriad as a result of altered intake, extra losses and dynamic shifts within the body. The main aims of intravenous fluid therapy include the replacement of fluid and electrolyte losses, providing fluid resuscitation to correct the effects of underlying diseases, maintaining cardiac output, blood pressure, tissue metabolism and waste removal, ensuring a stable intra and extra cellular milieu, preserving the membrane potential and transport mechanisms, and providing the required minimum amount of glucose to meet the energy requirements of the brain.3 An adequate intravenous fluid therapy avoids the development of oedema and other therapy-related adverse effects.
The assessment of fluid balance and subsequent prescription of fluid therapy is a complex task.4 It is usually based on patient's underlying illness, fluid input (resuscitation fluids, food or artificial nutrition) and output (urine, gastrointestinal loss, drainages), noninvasive monitoring of vital signs, skin and mucous membrane properties, and measurement of serum and urinary electrolytes and urea.5 However, errors during the administrations of intravenous fluid therapy are common. Such errors include incorrect selection of intravenous fluid type, volume, concentration and rate of fluid and electrolyte administration6. Clinical complications such as pulmonary oedema, heart failure and volume depletion have been reported following these errors.7 Volume and sodium overload is commonly seen in surgical patients and is associated with significant morbidity, mortality and increased length of stay with consequent increases in patient and health care system costs.8 The extent of the problem was highlighted by the 1999 UK National Confidential Enquiry into Perioperative Deaths (NCEPOD), which recommended a multidisciplinary approach to fluid therapy, the accurate recording of fluid intake and output, and the development of local good practice guidelines.9
Almost a decade on from the NCEPOD enquiry, only a few studies have been published that have evaluated the appropriateness of fluid therapy in the hospitalised patients of medical wards, and there is not yet any consensus statement about fluid therapy. This study aimed to assess whether the intravenous fluid therapy used for maintenance of the nil-per-os patient admitted to medical wards of the Complejo Asistencial Universitario de León adequately covers the daily requirements of water, glucose and electrolytes, to identify the number of patients remaining with intravenous therapy as the only nutritional support during an excessive time, and if this practice is associated with increased hospital stay and mortality.
Methods
Study design
This descriptive cross sectional study was conducted on patients admitted in medical wards of the Complejo Asistencial Universitario de León from September 2011 to February 2012. A sample size of 100 patients was calculated according to previous studies in order to detect a difference of 4 days in hospital stay based on the adequacy of fluid therapy with a potency of 20%.10,11. All procedures were approved by the local Research Ethics Committee, and informed consent was obtained from each patient.
Patient selection
Adult patients admitted to medical wards in nil-per-os status were included, excluding those < 18 yr, terminally-ill patients, patients treated surgically or awaiting surgery, those fasting for medical explorations, and patients receiving oral diet or any type of nutritional support such as oral supplements, enteral or parenteral nutrition. For the identification of cases, the diet prescription form was revised.
Methods
Once detected, patients were included in the study if they stayed longer than 24 hours fasting with intravenous fluids as the sole support. From each recruited patient the following data were obtained: medical history and reason for admission, physical examination (including usual and current weight, height -estimated from the ulna length if it could not be measured-, presence of oedema, diuresis, and temperature), biochemical parameters (serum urea, creatinine, glomerular filtration rate -which was estimated using the Modification of Diet in Renal Disease (MDRD) formula-, sodium, potassium, chloride), and administered fluid therapy (indication, start and suspension date, types of fluid, total volume and the amounts of sodium, potassium, chloride and glucose provided, intravenous medication). Nutritional status was evaluated using the Subjective Global Assessment (SGA).
The administered fluid therapy (including intravenous medications) was compared with the standardised requirements: water 35 mL/kg plus losses from fever or drainages, potassium 1 mmol/kg plus losses, sodium 2 mmol/kg plus losses, chloride 2 mmol/kg plus losses.12 For this purpose the mean administration of glucose, electrolytes and water was calculated. A minimum daily supply of 130 g of glucose, which has been defined by the National Academy of Science of the United States to meet the requirements of the brain in more than 98% of individuals in the healthy population, was considered correct.13 Electrolytic disturbances were defined as follows: hyponatraemia, plasma sodium < 135 mmol/L; hypernatraemia, plasma sodium > 145 mmol/L; hypokalaemia, plasma potassium < 3.5 mmol/L; hyper-cloraemia, plasma chloride > 110 mmol/L. Fasting was classified as inadequate if intravenous fluid therapy was the only nutritional supply for more than 7 days in well-nourished patients, and over 5 days in malnourished.14
Statistical analysis
The normality of the quantitative data was confirmed with the Kolmogorov-Smirnov test. If the data adjusted to a normal distribution, they were presented like mean (standard deviation, SD) and compared with Student's t test. In other case, they were presented as medians (interquartile range, IQR), and compared with the Mann-Whitney U test. Categorical data are summarised with percentages. Multivariate analysis was performed using linear and logistic regression. The strength of the linear relationship between the values was estimated using Pearson's correlation coefficient. The level of statistical significance was set at p < 0.05.
Results
The sample included 100 patients, of whom 51% were male, with mean age 76.6 (13.3) years. Most of them were recruited from the Department of Internal Medicine (71%), followed by Oncology (20%), Gastroenterology (8%) and Neurology (1%). According SGA, 67% of patients were classified as malnourished. Both the most frequent reasons for hospital admission and the indication of fasting with fluid therapy were related to gastrointestinal diseases and food intolerance, respectively (figs. 1 and 2). The duration of fluid therapy was 4 (IQR = 2) days, and 27% of the patients remained in inadequate fasting.
The most common type of fluid prescribed was glucose-saline at different concentrations: glucosaline 3%-0.3% (pre-charged with potassium chloride) in 69% of the cases, or glucosaline 5%-0.3% (without potassium) in 42%. It should be noted that the prescription of these intravenous fluids could change during hospitalisation. The intravenous medication in nearly all cases was administered with 0.9% saline.
Volume requirement [2,299.6 (355.4) ml] was correctly fulfilled as patients received 2,295.7 (683.4) ml of intravenous water. Data on the requirements in electrolytes are presented in figure 3, where it can be seen that the patients received an excess of sodium and chloride of 32.9% and 56.2%, respectively, and a deficit of potassium of 54.0%. Glucose administration was 68.8 (29.2) grams per day and 99% of patients received less than 130 grams per day.
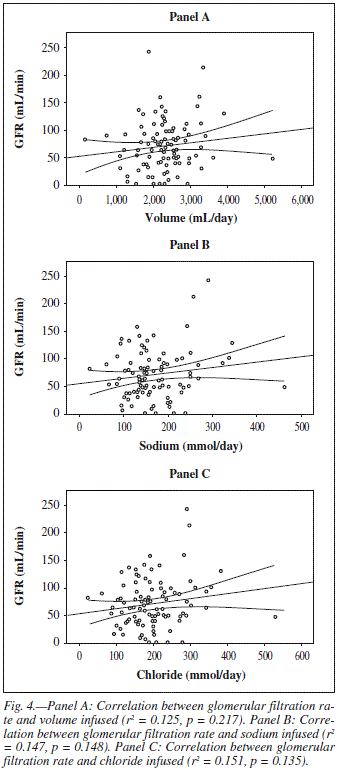
Patients with pathological conditions, like heart failure and hypertension that can alter the amount of volume and electrolytes required in order to avoid cardiovascular deterioration and oedema, were compared with those free of those conditions. Patients with heart failure received less volume (1,789 vs. 2,390 ml, p = 0.001) and sodium (120 vs. 177 mEq/L, p = 0.001) than those without this cardiologic condition. Patients with hypertension received a similar volume (2,211 vs. 2,458 ml) and a smaller amount of sodium (157 vs. 190 mEq/L), and the latter was statistically significant (p = 0.018). The prevalence of electrolytic disturbances was relatively low: hypernatraemia 13%, hyponatraemia 18%, hypokalaemia 13% and hypercloraemia 8%. Those patients with hypokalaemia received a significantly lower supply of potassium (27.3 mmol/d vs. 42.3 mmol/d, p = 0.018), but there were not differences in electrolyte and volume administration, or in the duration of fluid therapy according the presence of electrolytic disturbances. There were not differences in mortality or length of hospital stay when electrolytic alterations were present. The relation between volume and electrolytes administered and renal function can be seen in figure 4.
Analysing the data in order to detect possible effects of the administered intravenous fluid therapy on patients outcomes, it was observed that patients with an inadequately prolonged fasting receiving only fluid therapy had a longer hospital stay [22.0 (IQR = 13.0) vs. 13.0 (IQR = 11.0) days, p = 0.001]. This difference remained significant after adjusting for sex, age, nutritional status, volume, electrolytes and glucose supply, and underlying diseases. There was also a higher percentage of mortality among malnourished patients compared to well nourished (25.4% vs. 3.0%, p = 0.06). After adjusting for the factors previously mentioned only malnutrition was a factor predictive of mortality during hospitalisation, with an odds ratio of 10.5 (95% CI 1.3 to 83.2).
Discussion
This cross-sectional study was conducted in order to know the management of intravenous fluid therapy in nil-per-os patients in medical wards of a tertiary hospital. To our knowledge, this is the first study to evaluate the implications of this practice in the outcomes of medical patients. Comparing the daily electrolyte requirements with the administered by intravenous fluid, we observed that patients receive an excessive amount of sodium and chloride and an insufficient amount of potassium. The results on the supply of glucose are discouraging with 99% of patients receiving less than the minimum required amount to prevent ketosis and meet the energy requirements of the brain.
Although not directly assessed, these data may lead to the conclusion that there is an inadequate knowledge and a subsequently suboptimal prescribing of fluid therapy by medical staff, and can be attributed to the lack of graduate and postgraduate training of physicians, and the lack of widely accepted consensus or guidelines. One study into 2 major medical universities in the United Kingdom showed that students received less than 3 hours of education on fluid therapy during their 6-year career. Only 58.9% and 19.8% of sixth graders could recognise the composition of 0.9% saline and Ringer lactate, respectively. Regarding 24h electrolyte needs, it was correctly estimated only by 32% for sodium, 34% for chloride and 55% for potassium.15 Another study in 25 British hospitals showed that in surgical wards the prescribing of fluid therapy was performed in 89% by preregistration house officers, and less than a half of them knew the sodium content of 0.9% saline. The majority acknowledged that they had not been given any formal or informal guidelines on fluid and electrolyte prescribing while on the surgical firm.16 Based on these results, it has been evaluated whether the implementation of structured workshops can help to fill this lack of training, demonstrating that it can be a successful way of acquiring knowledge and gaining clinical skills.17 Since 1999, the NCEPOD has emphasised the need for training of medical personnel in the physiology of fluids and electrolytes in order to increase knowledge and to disseminate good practice.9
In this study, the majority of patients were given glucosaline and the medication was administered by 0.9% saline, explaining the excess of sodium and chloride received. In a previous study on surgical patients of another Spanish hospital, the type of fluids more commonly used were dextrose 5% and saline 0.9%.10 The local fluid therapy policy encourages the use of pre-charged fluids to reduce the manipulation in wards, but these results demonstrate that the use of all-in-one fluids can result in an inadequate glucose and electrolyte supply. In spite of this, electrolytic disturbances were infrequently found, and they were not related to adverse outcomes. The former can be explained by the short duration of fluid therapy (4 days), and the latter by a small sample size. It is important to reflect that chloride, an anion which is not taken into account many times during the prescription of fluid therapy, was administered in an excess of more than 50%.
The increased plasma chloride results in hyperchloraemic acidosis, especially harmful in elderly patients. This acidosis may reduce blood flow and decrease gastric intramucosal pH, and can affect gastric motility. Hypercloraemia may also produce renal vasoconstriction and reductions glomerular filtration, contributing to high salt retention. Too much sodium, on the other hand, produces fluid retention and oedema, peripheral and splanchnic, resulting in increased abdominal pressure, ascites and even abdominal compartment syndrome. This in turn can lead to decreased mesenteric artery blood flow causing ileus, intestinal failure and, in surgical patients, anastomosis dehiscence.18 In our cohort, patients with hypertension and heart failure received a volume and amount of electrolytes adjusted to their underlying condition in order to avoid complications from volume and sodium overload. Furthermore, we did not find any renal side effects in terms of altered glomerular filtration rate in relation with the amount of volume and electrolytes infused.
An interesting finding of the study is that although 67% of patients were malnourished according to SGA, they only received a median of 68.8 g glucose and 27% remained in an inadequate fasting status, these facts probably further worsening their nutritional status. Malnutrition is common in the hospital setting, with 20-50% of patients identified as malnourished on admission.19,20,21 Malnutrition has been negatively associated with a variety of clinical, functional and economic outcomes.22 On a physical level, malnutrition can cause a loss of muscle and fat mass, reduced respiratory muscle and cardiac function, and atrophy of visceral organs. On a cellular level, malnutrition impairs the body's ability to mount an effective immune response in the face of infection, often making infection harder to detect and treat. It also increases the risk of pressure ulcers, delays wound healing, increases infection risk, decreases nutrient intestinal absorption, alters thermoregulation and compromises renal function.23 Malnourished patients have been shown to have a length of hospital stay from 1.5 to 1.7 times longer than the well-nourished patients.24 It has also been shown to have a three-fold increase in mortality for a period of 12 months after discharge and more likely to be readmitted within 15 days.25 In a recent study on the actual cost of hospitalisation, the average cost for malnourished patients is greater than for well-nourished patients (p = 0.014), with malnutrition being a significant predictor of mortality.26 Similar results were obtained in our study where malnutrition was the only predictor of mortality adjusted for factors such as age or underlying disease.
There are few studies that evaluate fluid therapy in medical patients. A study in an infectious diseases ward of a teaching hospital found frequent mistakes in the rate of fluid administration (29.8%), in volume calculation (26.5%) and in fluid selection (24.6%).27 There are more data on the surgical patient. A review from two American university teaching hospitals, which attempted to estimate the burden of morbidity and mortality from pulmonary oedema in patients following major surgery, estimated that there could be 213,200 cases of postoperative pulmonary oedema annually in the United States, accounting for 8,315 deaths during the 30 days following surgery, in which no cause apart from excessive fluid administration could be inferred.28 The same year, the report of the NCEPOD indicated that 20% of patients have a poor record of fluid balance or have a water imbalance untreated or unrecognised that could contribute to severe postoperative morbidity and mortality.9 During the next decade, several studies have assessed the consequences of different attitudes in the management of fluid therapy before, during and after surgery, and a meta-analysis by Varadhan and Lobo in 2010 showed that patients who received balanced fluid therapy had statistically significant fewer complications and a shorter length of stay.8 Regarding medical patients, our study found that inadequate fasting with fluid therapy as the sole nutritional support was independently associated with a longer hospital stay.
Several measures have been proposed to improve the use of fluid therapy.2 First, a specific training for medical students in aspects of electrolyte balance. Second, a multidisciplinary approach from various specialties to the contribution of developing clinical guidelines based on evidence.29 A first attempt was the British Consensus Guidelines on Intravenous Fluid Therapy for Adult Surgical Patients Guidelines (GIFTASUP).30 The guidelines from the National Institute for Health and Clinical Excellence (NICE) that will help standardise the management and prescription of fluids are also pending publication.31 Third, the formation of a collaboration of clinical biochemists that may be responsible for reviewing patients who remain nil-per-os with fluid therapy has been proposed, as nutrition services do to patients with parenteral nutrition or pharmacists who review medications routinely patterned by doctors.2
The main limitation of the study was that the information of fluid therapy was collected from the medical records of patients, with difficulties collecting the amount of intravenous medication that is not always correctly reflected. Moreover, in many cases the water balance chart was not fully complemented, as urine output was not always properly collected. One more limitation is the small number of the sample with the wide confidence intervals.
Conclusion
Our results showed that the nil-per-os medical patients receive an inadequate supply of electrolytes and glucose, and that a considerable percentage remains in inadequate prolonged fasting despite malnutrition being very common. Inappropriately prolonged fluid therapy and malnutrition are associated with worse outcomes in these patients independently of other conditions such as age or underlying diseases. Further prospective studies are needed to confirm these results.
References
1. Awad S, Allison SP, Lobo DN. The history of 0.9% saline. Clin Nutr 2008; 27 (2): 179-88. [ Links ]
2. Smellie WS. Intravenous fluid therapy - an under-recognized patient safety opportunity. Ann Clin Biochem 2009; 46 (Pt 6): 438-40. [ Links ]
3. Leach R. Fluid management on hospital medical wards. Clin Med 2010; 10 (6): 611-5. [ Links ]
4. Shafiee MA, Bohn D, Hoorn EJ, Halperin ML. How to select optimal maintenance intravenous fluid therapy. QJM 2003; 96 (8): 601-10. [ Links ]
5. Rhoda KM, Porter MJ, Quintini C. Fluid and electrolyte management: putting a plan in motion. JPEN J Parenter EnteralNutr 2011; 35 (6): 675-85. [ Links ]
6. Hilton AK, Pellegrino VA, Scheinkestel CD. Avoiding common problems associated with intravenous fluid therapy. Med J Aust 2008; 189 (9): 509-13. [ Links ]
7. Walsh SR, Walsh CJ. Intravenous fluid-associated morbidity in postoperative patients. Ann R Coll Surg Engl 2005; 87 (2): 126-30. [ Links ]
8. Varadhan KK, Lobo DN. A meta-analysis of randomised controlled trials of intravenous fluid therapy in major elective open abdominal surgery: getting the balance right. Proc Nutr Soc 2010; 69 (04): 488-98. [ Links ]
9. Callum KG, National Confidential Enquiry into Perioperative Deaths. Extremes of age: the 1999 report of the National Confidential Enquiry into Perioperative Deaths: data collection period 1 April 1997 to 31 March 1998. London: National Confidential Enquiry into Perioperative Deaths; 1999. [ Links ]
10. Campo Angora M, García Rodríguez P, Martínez Díaz C, Serrano Garrote O, Herreros de Tejada y Lopez Coterilla A. (Use of maintenance fluid therapy in surgery). Farm Hosp 2004; 28 (2): 84-9. [ Links ]
11. Lobo DN, Bostock KA, Neal KR, Perkins AC, Rowlands BJ, Allison SP. Effect of salt and water balance on recovery of gastrointestinal function after elective colonic resection: a randomised controlled trial. Lancet 2002; 359 (9320):1812-8. [ Links ]
12. Lobo DN, Lewington AJ, Allison SP. Basic Concepts of Fluid and Electrolyte Therapy. 1st ed. Melsungen: Bibliomed - Medizinische Verlagsgesellschaft mbH; 2013, 136 p. [ Links ]
13. National Research Council (U.S.). Subcommittee on the Tenth Edition of the RDAs., National Institutes of Health (U.S.), National Research Council (U.S.). Committee on Dietary Allowances. Recommended dietary allowances. 10th ed. Washington, D.C.: National Academy Press; 1989. [ Links ]
14. White JV, Guenter P, Jensen G, Malone A, Schofield M. Consensus statement: Academy of Nutrition and Dietetics and American Society for Parenteral and Enteral Nutrition: characteristics recommended for the identification and documentation of adult malnutrition (undernutrition). JPEN J Parenter Enteral Nutr 2012; 36 (3): 275-83. [ Links ]
15. Chari A, Cooke JS, Singh S, Findlay JM. Peri-operative fluid and electrolyte management: Undergraduate preparation and awareness. e-SPEN, the European e-Journal of Clinical Nutrition and Metabolism. 2011;6(4):e207-e10. DOI: 10.1016/j.eclnm.2011.06.002. [ Links ]
16. Lobo D. Problems with solutions: drowning in the brine of an inadequate knowledge base. Clin Nutr 2001; 20 (2): 125-30. [ Links ]
17. Awad S, Allison S, Lobo D. Fluid and electrolyte balance: The impact of goal directed teaching. Clin Nutr 2008; 27 (3): 473-8. [ Links ]
18. Allison SP, Lobo DN. Fluid and electrolytes in the elderly. Curr Opin Clin Nutr Metab Care 2004; 7 (1): 27-33. [ Links ]
19. Vidal A, Iglesias MJ, Pertega S, Ayucar A, Vidal O. Prevalence of malnutrition in medical and surgical wards of a university hospital. Nutr Hosp 2008; 23 (3): 263-7. [ Links ]
20. Norman K, Pichard C, Lochs H, Pirlich M. Prognostic impact of disease-related malnutrition. Clin Nutr 2008; 27 (1): 5-15. [ Links ]
21. Sarto B, Elío I, Planas M, Forga M, Cantón A, Trallero R, Muñoz MJ, Pérez D, Bonada A, Saló E, Lecha M, Enrich G, Salas-Salvadó J. Prevalence of malnutrition and its etiological factors in hospitals. Nutr Hosp 2012; 27 (2): 469-76. [ Links ]
22. Waitzberg DL, Ravacci GR, Raslan M. Hospital hyponutrition. Nutr Hosp 2011; 26 (2): 254-64. [ Links ]
23. Barker LA, Gout BS, Crowe TC. Hospital malnutrition: prevalence, identification and impact on patients and the healthcare system. Int J Environ Res Public Health 2011; 8 (2): 514-27. [ Links ]
24. Correia MI, Waitzberg DL. The impact of malnutrition on morbidity, mortality, length of hospital stay and costs evaluated through a multivariate model analysis. Clin Nutr 2003; 22 (3): 235-9. [ Links ]
25. Middleton MH, Nazarenko G, Nivison-Smith I, Smerdely P. Prevalence of malnutrition and 12-month incidence of mortality in two Sydney teaching hospitals. Intern Med J 2001; 31 (8): 455-61. [ Links ]
26. Lim SL, Ong KC, Chan YH, Loke WC, Ferguson M, Daniels L. Malnutrition and its impact on cost of hospitalization, length of stay, readmission and 3-year mortality. Clin Nutr 2012; 31 (3): 345-50. [ Links ]
27. Mousavi M, Khalili H, Dashti-Khavidaki S. Errors in fluid therapy in medical wards. Int J Clin Pharm 2012; 34 (2): 374-81. [ Links ]
28. Arieff AI. Fatal postoperative pulmonary edema: pathogenesis and literature review. Chest 1999; 115 (5): 1371-7. [ Links ]
29. Cordero Cruz AM, Moreno Villares JM, Gomis Muñoz P, Valero Zanuy MÁ, Calleja Hernández MÁ. Pilot study of intravenous fluid therapy management in adult patients at a tertiary care hospital. Nutr Hosp 2012; 27 (3): 943-7. [ Links ]
30. Powell-Tuck J GP, Lobo DN, Allison SP, Carlson GL, Gore M. British consensus guidelines on intravenous fluid therapy for adult surgical patients. London: Association of Surgeons of Great Britain and Ireland; 2008. (Last accessed August 28, 2012, at http://www.bapen.org.uk/pdfs/bapen_pubs/giftasup.pdf). [ Links ]
31. Pearse RM, Ackland GL. Perioperative fluid therapy. BMJ 2012; 344: e2865. [ Links ]
![]() Correspondence:
Correspondence:
Georgios Kyriakos
Sección de Endocrinología y Nutrición
Complejo Asistencial Universitario de León
C/ Altos de Nava, s/n
24008 León. Spain
E-mail: giorgos6@yahoo.com
Recibido: 1-IV-2013
1.a Revisión: 13-V-2013
Aceptado: 15-V-2013