Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Nutrición Hospitalaria
versión On-line ISSN 1699-5198versión impresa ISSN 0212-1611
Nutr. Hosp. vol.28 no.5 Madrid sep./oct. 2013
https://dx.doi.org/10.3305/nh.2013.28.5.6725
ORIGINAL / Otros
Diet choice in weight-restored patients with eating disorders; progressive autonomy process by nutritional education
Elección de la dieta en pacientes con trastornos de la conducta alimentaria con peso normalizado; proceso de progresiva autonomía mediante educación nutricional
Inmaculada Ruiz-Prieto1-2, Patricia Bolaños-Ríos1 and Ignacio Jáuregui-Lobera1,3
1Eating Disorders Unit. Behavioral Sciences Institute. Seville. Spain
2Nutritional, Environmental and Genetics Growth and Development Factors Program. Granada University. Granada. Spain
3Nutrition and Bromatology. Pablo de Olavide University. Seville. Spain
The authors thank the Behavioural Science Institute staff for their support.
ABSTRACT
Introduction: Human eating behaviour is regulated by multiple factors. Anorexia nervosa patients show a restrictive eating pattern while bulimia nervosa patients present bingeing-purging episodes. Although treatments are specially successful in the normalization of body composition, maladaptive eating behaviours tend to persist being a risk factor for relapse and recurrence.
Objectives: The aim of this work was to assess the quality of the nutritional choice of eating disorders patients after a year of nutritional education and to assess improvements in choice capacity.
Methods: Thirty-one outpatients of an eating disorders unit planned a menu after body composition normalization and repeated this plan each three months during a one-year programme of nutritional education.
Results: Patients improved the time spent on the assignment (p < 0.01), Body Mass Index (p < 0.01), their body fat mass (p < 0.01) and the content of energy (p < 0.05), carbohydrates (p < 0.01) and polyunsaturated fatty acids (p < 0.05) in their chosen menus. No differences were found on proteins, total fat or fat profile, vitamins or minerals. 12.9% and 3.2% of the patients chose their menu according to the recommendations of caloric and lipid profile, respectively, after a year of nutritional education.
Discussion: Although patients improved energy and carbohydrates content of the menus they tended to reduce caloric and fat food choices, which could lead to relapse and recurrence. Specific nutritional education programmes along with the mandatory psychological and psychiatric treatment may be effective.
Conclusions: One year of nutritional education combined with psychological and psychiatric treatment improved those factors usually involved in relapse and recurrence, thus contributing to a proper outcome.
Key words: Diet choice. Eating disorders. Treatment outcome. Body mass index. Relapse.
RESUMEN
Introducción: El comportamiento alimentario humano está regulado por numerosos factores. Mientras los pacientes con anorexia nerviosa muestran un patrón nutricional restrictivo, los pacientes con bulimia nerviosa presentan episodios de atracón y purgas. Aunque los tratamientos son muy efectivos en la normalización de la composición corporal los comportamientos alimentarios inadecuados tienden a mantenerse constituyendo un factor de riesgo de recaídas y recidivas.
Objetivos: El objetivo de este trabajo fue evaluar la calidad de la elección nutricional de pacientes con trastornos de la conducta alimentaria durante un programa de un año de educación nutricional analizando la mejoría en la capacidad de elección.
Método: Treinta y un pacientes de una unidad de trastornos alimentarios planificaron un menú tras la normalización de la composición corporal, tarea que repitieron cada tres meses durante el año de intervención.
Resultados: Los pacientes mejoraron el tiempo empleado en configurar el menú (p < 0,01), el Índice de Masa Corporal (p < 0,01), la masa grasa corporal (p < 0,01), la energía (p < 0,05), los carbohidratos (p < 0,01) y los ácidos grasos poliinsaturados (p < 0,05) de los menús planificados. No hubo diferencias en cuanto al total de grasas, perfil lipídico, vitaminas y minerales. El 12,9% y 3,2% de los pacientes escogieron sus menús de acuerdo a las recomendaciones de perfil calórico y lipídico, respectivamente, tras el año de tratamiento.
Discusión: Aunque los pacientes mejoraron el contenido energético y los carbohidratos en los menús elegidos, tendieron a reducir el contenido calórico y las grasas en su elección, lo que puede conducir a una peor evolución.
Conclusiones: Durante un año de educación nutricio-nal, junto con el correspondiente tratamiento psicológico y psiquiátrico, se observó una mejoría en los factores dietéticos habitualmente implicados en una posible mala evolución.
Palabras clave: Elección de la dieta. Trastornos alimentarios. Resultado del tratamiento. Índice de masa corporal. Recaída.
Abbreviations
AN = Anorexia Nervosa.
BFM = Body Fat Mass.
BMI = Body Mass Index.
BN = Bulimia Nervosa.
CHO = Carbohydrates.
ED = Eating Disorders.
EDNOS = Eating Disorders Not Otherwise Specified.
MUFA = Monounsaturated Fatty Acids.
PRO = Proteins.
PUFA = Polyunsaturated Fatty Acids.
SFA = Saturated Fatty Acids.
SD = Standard Deviation.
Introduction
Human eating behaviour is regulated by multiple reasons such as physiological (like hunger and satiety), emotional (positive or negative mood may influence hunger and satiety sensations), external cues (like the smell of a food), socio-cultural factors (social norms or traditions) and others like political, religious and economic reasons.1
Eating habits and nutritional knowledge also influence the food choice.2,3 Family educational models and family and peers support influence eating habits. It is observed that daughters dieting frequently have mothers with restrictive eating habits. In addition children whose parents cannot control their ingest have the same problem. TV viewing while eating is correlated with eating less fruit and vegetables, and on the other hand with more precooked, processed and fast food and it correlates with the belief that dietary and fat-free products are more nutritive.2,4,5 What is more, eating out correlates with more energetic and fatty food consumption2. Emotional food choice is related with more irrational food beliefs, bulimia and binge eating in women. Health and natural food choice is related to more rational food beliefs and less psychopathology. Weight-control food choice results to be more aesthetic than healthy and is related to restrictive food pattern, drive for thinness and body dissatisfaction.3
Dieting is one of the main factors in the development of an eating disorder (ED) and is related to unhealthy behaviours like vomiting, skipping meals, considering food as forbidden, having a big concern about nutritive characteristics of food and carrying out physical activity to lose weight.6,7 However, it is observed that rigid dieting increases the risk for having inadequate food behaviours more frequently than flexible dieting8 and is more common in women or girls.6,7 Pathological dieters present more magical beliefs about food and health, which is related to ideological food choice. The loss of pleasure associated with food is related to stressed and worrying situations and promotes guiltiness and self-dissatisfaction. In ED the loss of pleasure associated to food may be related to dopaminergic system that acts differently in restrictive and bingeing-purging disorders (while bingeing-purging patients compensate negative emotions with sugar consumption, restrictive ones diminish positive emotions related to food and have positive reinforcement of privation), having both an emotional food choice.7
Anorexia Nervosa (AN) patients usually choose foods with less energy and macronutrient, specially fats, than people without ED and they usually follow a menu deficient in calcium, vitamin A and vitamin D.9,10 However, Mayer et al. found that people with AN used to choose more carbohydrates (CHO) and proteins (PRO) than the control group in a laboratory environment11. In addition, diet variety is usually limited, avoiding food high in palatability such as sauces and condiments, bread and starches, meat, cured meat, fats and oils, sweets and fried, but choosing vegetables more frequently.9,10 Also AN patients use to choose smaller portion sizes.12
Bulimia Nervosa (BN) patients eating behaviour is characterized by binge-purge episodes.13-20 There is no a specific eating pattern described in BN as their behaviour is unpredictable and chaotic. However, BN patients use to choose higher energy foods and higher palatable foods than AN patients.13 During bulimic episodes patients choose foods higher in fat and CHO, specifically refined CHO, and lower in PRO.13-17 They base their food choice in sweets, salty snacks and desserts during the bingeing episode.13-15 Addictive capacity of CHO has been proposed to explain CHO bingeing in obese and bulimic people during distress periods but it is not settled down.15-17
Hunger-satiety sensations are subjective and disturbed in ED patients and influence their food choice. In that way, neither AN nor BN patients show sensory-specific satiety except in case of BN patients and low-caloric food.13,18-20
The purpose of the nutritional treatment in ED aims to restore body composition and physical functioning while normalizing eating patterns, food choice, eating behaviour and food and health cognitions.20-23 Cognitive-behavioural therapy tries to avoid food restrictive patterns and to restore Hunger-satiety sensations.8,20,22 However, the most of the recommendations are based on clinical experience.20
Although treatments are specially successful in the normalization of body composition, maladaptive eating behaviours tend to persist being a risk factor of relapse.12,22 In addition, there have been little advances in treatments during decades so it is necessary new interventions in order to improve eating behaviours as well as to normalize body composition and to give the appropriate psychological treatment during the whole therapeutic proccess.22
Nutritional education (involving health risks of nutritional behaviour typical in ED) is a recent intervention in order to improve food choice and food and health beliefs in ED patients promoting changes in their eating patterns thus leading to body composition normalization.4,6,8,24
The aim of this work was to assess the quality of the nutritional choice of ED patients after a year of nutritional education by a nutritionist and to assess improvements in election capacity to reach a better nutritional choice and a reduction of the time when selecting their menu.
Methods
Design
Participants were encouraged to imaging being alone at home during a week so they could plan their diet without their families' food preferences influence. To plan their menu participants were given food options in form of cards distributed in four intakes per day (breakfast, lunch, snack and dinner).
These options included the food elaborations of highest consumption in the study population considering all the food groups (cereals or starches, dairy products, fruits, vegetables, fish, eggs, lean meats, cured meats, oils, fats and sweets). The settings of the menu were carried out every three months.
The menus were evaluated in terms of nutrients (nutritional tracker software designed by Alce Ingeniería, Complutense of Madrid University). To assess caloric and lipid profile it was followed the WHO recommendations.
Body composition was measured by tetrapolar bioelectrical impedance with 50 kHz frequencies and 500 |iA (TANITA TBF-410®) with 0.1 kg precision and capacity from 0-200 kg. Height was measured by 1mm precision scale with capacity of 60-200cm (SECA 220®).
Time spent in the assignment was measured with a watch chronometer (CASIO A178W®) without patient's knowledge.
Participants
The study involved 106 ED outpatients of an ED unit. The inclusion criteria were weight-restored according to the WHO Body Mass Index (BMI) classification criteria and attending treatment weekly or bi-weekly.
The period of study was from December 2010 until January 2013. Seventy-five participants were lost over that period because of discontinuation of treatment, leaving the study or extension of the treatment visiting frequency because of improvements in its outcome.
Procedure
Participants planned the first menu after having restored their weight within the period from December 2010 to January 2012 and repeated it every three months until a year. The menu was performed individually in a room with appropriate conditions and in the presence of a therapist who was able to solve possible doubts. The time spent on the settings of the menu was measured in each of the tests and body composition was measured before starting it.
This work was performed during a year of treatment, which consisted of a multidisciplinary structured behavioural program and nutritional education accomplished by a psychiatrist, a psychologist and a nutritionist. Patients were seen individually and families received support by the entire therapist team weekly or biweekly. Treatment aimed at normalize body composition, eating patterns and psychopathology symptoms. Pharmacology treatment was recommended when needed.
Statistical analysis
Data are presented as means and standard deviation (SD). Friedman test was used to determine differences in macronutrients (CHO, PRO and lipids) and fatty acids content (Monounsaturated Fatty Acids (MUFA), Polyunsaturated Fatty Acids (PUFA) and Saturated Fatty Acids (SFA)). In order to analyse the degree of adequacy with respect to the caloric and lipid profile given by the WHO, the Cochrane test was applied. Differences between ED subtypes were analysed using the Kruskal-Wallis test. In all cases the level of significance was set at p < 0.05.
Ethical
The present work carried out the Ethical Principles for Medical Research Involving Human Subjects in accordance to the Helsinki Declaration and the research protocol was approved by the Direction of the Behavioural Science Institute (Seville, Spain). Participation in the study was voluntary obtaining the informed consent of patients older than 18 years and their parents or tutors for those underage.
Results
In the present work 31 outpatients of an ED unit were involved. They were 21.9 ± 7.27 years old (range 14-44) and they had been under treatment for 55.26 ± 96.28 weeks. With respect to the age, there were not statistically significant differences between ED subtypes. 45.16% were AN patients, 29.03% were BN patients and 25.81% were ED not otherwise specified (EDNOS).25
Body composition
The BMI improved from the first measure (20.92 ± 5.85 at the baseline vs. 21.95 ± 4.68 after three months; p < 0.01 and 20.92 ± 5.85 at the baseline vs. 22.10 ± 4.40 after a year; p < 0.01). Data shown in figure 1.
The Body Fat Mass (BFM) improved during the first three months (19.48 ± 10.24% vs. 21.53 ± 7.70%; p < 0.01) and between the last three months (21.72 ± 6.49% vs. 23.12 ± 7.00%; p< 0.01). Differences between the beginning and the final measure were statistically significant (19.48 ± 10.24% vs. 23.12 ± 7.00%; p < 0.01).
Time spent on the assignment
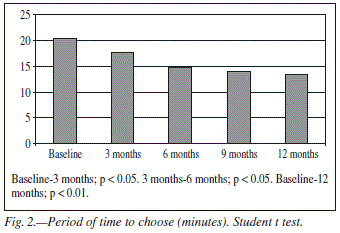
Participants spent a shorter period of time to choose the menu at the end of the study with respect to the beginning of the treatment (20.48 ± 8.19 min vs. 13.48 ± 5.18 min; p < 0.01). There were statistically significant differences between the first and the second time (20.48 ± 8.19 min vs. 17.67 ± 6.22 min; p < 0.05) and between the third and the fourth time (17.67± 6.22 min vs. 14.81 ± 5.29 min; p < 0.05). These data are shown in figure 2.
Energy and macronutrients
Participants improved the total energy content in their menus (1,868.93 ± 448.6 kcal/day at baseline vs. 2,010.22 ± 435.24 kcal/day after a year; p < 0.05). Although after three months the total energy chosen was higher than after a year it was not statistically significant. There were significant differences between the first and the second menu chosen (1,868.93 ± 448.6 kcal/day at baseline vs. 2,062.22 ± 317.37 kcal/day after three months; p < 0.05). These data are shown in figure 3.
The CHO content of the menu was higher after three months (203.7 ± 50.14 g at baseline vs. 224.8 ± 38.02 g after three months; p < 0.05) and it improved again between six and nine months (225.23 ± 37.18 g after six months vs. 237.22 ± 38.41 g after nine months; p < 0.01). After a year participants chose less CHO than after nine months but that difference was not statistically significant (203.7 ± 50.14 g at baseline vs. 225.28 ± 53.58 g after a year; p < 0.01).
The fat content increased during the first three months (77.24 ± 21.37 g at baseline vs. 86.01 ± 14.64 g after three months; p < 0.05) and it decreased during the next three months (86.01 ± 14.64 g after three months vs. 82.44 ± 14.28 g after six months; p < 0.05). There were not significant differences after a year. These data are shown in figure 4.
PRO content did not show statistically significant differences.
During the first nine months menus did not adjust to caloric profile recommended by WHO. After a year 12.9% of patients' chose their menu in accordance to recommended caloric profile.
Fats profile
The total content of MUFA in the menu chosen did not show statistically significant differences after a year. It strongly improved during the first three months (37.75 ± 11.38 g at baseline vs. 43.22 ± 7.58 g after three months; p < 0.01) and significantly decreased between the second and the third menu chosen (43.22 ± 7.58 g after three months vs. 41.01 ± 7.59 g after six months; p < 0.05) and the third and the fourth ones (41.01 ± 7.59 g after six months vs. 38.55 ± 8.42 g after nine months; p < 0.05).
PUFA significantly improved after a year (9.11 ± 2.57 g at baseline vs. 10.15 ± 2.52 g after a year; p < 0.05) with the highest increase between the third and the fourth menu chosen (9.32 ± 1.56 g after six months vs. 10.00 ± 2.28 g after nine months; p < 0.01). Neither PUFA-ω3 nor PUFA-ω6 showed statistically significant differences after a year. PUFA-ω3 improved during the first three months (0.27 ± 0.09 g at baseline vs. 0.31 ± 0.05 g after three months; p < 0.01) but decreased between the third and the fourth menu (0.30 ± 0.06 g after six months vs. 0.25 ± 0.04 g after nine months; p < 0.01). PUFA-ω6 increased during the first three months (2.99 ± 1.11 g at baseline vs. 3.42 ± 0.55 g after three months; p < 0.05) but significantly decreased between the second and the third menu chosen (3.42 ± 0.55g after three months vs. 3.24 ± 0.64 g after six months; p < 0.05) and the third and the fourth ones (3.24 ± 0.64 g after six months vs. 2.68 ± 0.49 g after nine months; p < 0.01). These data are shown in figure 5.
Neither SFA nor cholesterol was significantly different after a year.
About lipid profile after nine months of nutritional education 12.9% of the patients' choice were maid based on WHO recommendations and after a year only 3.2% did. During the first nine months any choice was maid in accordance to the recommendations.
Vitamins and minerals
Any statistically significant differences were found in the amount of vitamin B12, vitamin D, folic acid, calcium or iron.
Differences in ED subtypes' choice
Energy choice was higher in AN patients menus after six months (p < 0.05) and after a year (p < 0.05). In addition, they chose menus with much more content of PRO (p < 0.05), fats (p < 0.05), SFA (p < 0.05), vitamin B12 (p < 0.01), vitamin D (p < 0.05), calcium (p < 0.05) and iron (p < 0.05) after a year. AN patients chose menus with higher content of MUFA after six months (p < 0.05). With respect to cholesterol, the content in the menus chosen by AN patients was higher at the beginning (p < 0.05) and after nine months (p < 0.01). No differences were found considering CHO, fibre, PUFA or folic acid menus content in comparison with other ED diagnosis subtypes.
Discussion
The major of evidences published on the topic of nutritional choice in ED patients are conducted in AN or overweight/obese cravers. Little is known about what is the food pattern that characterized BN patients.9-12,15-17 However, bulimic eating habits are based on restriction episodes followed by bingeing/purging or vice versa.13-20 In this study, all subtypes of ED were included. Moreover, most of studies are transversal while this is a year follow-up study in ED patients' diet choice.
The period of time spent in the menu setting improved after a year, this indicates that during nutritional education patients improve their knowledge about healthy food thus leading them to choose faster. Although brain feeding regulation is unclear, thus medial prefrontal and obifrontal regions showed abnormal activation patterns in ED patients these patterns improving with body composition normalization17. It might indicate a better diet choice ability.
Clinical outcome in ED patients indicates the effectiveness of treatment in normalizing body composition and improving some psychopathological symptoms although some relevant clinical symptomatology tend to maintain over time.1 Relapse and recurrence are estimated to be between 30 and 60 percent of the cases.1,10-12,19 ED patients' food pattern tends to persist over time based on restrictive food choice and altered sensations.13-18,20 Moreover, AN patients tend to restrict energy and fat density foods while BN patients tend to maintain CHO craving with a low sensory-specific satiety in both subtypes. In AN, patients tend to classify some foods as "safe foods" (those which do not make them grow fat) and in BN patients maintain a strong desire of hypercaloric and palatable foods.9,11,13,18,20,26
The present work showed that ED patients improved the energy content of the menus chosen during a year of nutritional education. Although it was not statistically significant, they chose a higher energy density menu after the first three months and tend to reduce it over the next months until a year. This is in accordance with other results that affirm an improvement in energy content diet choice in AN patients while they tend to decrease over time.11-12,22,26 However, in this work energy content of diet choice was lower than in other works, which may be explained because differences on treatment environment (most of studies were conducted during hospitalization), socio-cultural or because this is a choice record instead of real ingest one.10,11,12,22
Opposite to other works, in this study ED patients increased CHO diet choice content significantly but they maintained fat and PRO choice.10-12,22,27 Fat avoidance is related to poorer outcome.9,10 Micronutrient choice is under needs coinciding with another recent work.9 PUFA choice increased in the present work but it is not included in other studies.
In accordance to other studies, AN patients tend to chose menus with higher content of PRO9-11 but, different to other evidences, in this work AN patients chose more fats than other ED patients,9-17 which might be understood as the effectiveness of the nutritional education in combination to the psychological and psychiatric treatments. The CHO choices were not significantly different among ED subtypes, this being contrary to the Mayer et al. findings.12 Major of evidences show that BN patients tend to choose higher CHO and fats food content during bulimic episodes13-17 but the present work aimed to analyse the patients' choices in a normal situation, which could explain the absence of differences in the menus CHO content among different ED.
It is well-known that AN patients tend to overestimate energy and fat content of the food they eat, which possibly explains that they do not reach energy needs.9,11,19 Moreover, the media positively influences altered food behaviours maintenance. This is based on the promotion of personal transformation by means of weight loss and dieting, food restriction to promote physical, emotional and psychological healthy state and beauty, and maintenance of thinness obsession.7,28-30 In addition, food information, magazine pictures, family and peers reinforce may lead to preservation of unhealthy eating behaviours.28
It is observed that in ED patients maladaptive eating behaviours persist focused on anticipatory anxiety related to meals because of irrational and magical food beliefs; fears related to food with avoidance of high fat or energy density foods; high concern about the content of the food they eat; effect of food on their shape and weight; tendency to restrictive food behaviour; abnormal Hunger-satiety sensations after weight normalization; and altered weight changes perception.7,10,11,19,20,22,31 AN patients avoid energy-density, high fat and high palatable foods and maintain high satiety sensation 14 minutes after the meal is over, which may influence diet choice. After discharge they tend to reduce serving portions and more caloric content foods to maintain skipping meals and to control weight behaviours.12,19,20,26 Bn patients maintain restrictive behaviours and taboos about food, avoidance of fat-density foods and inclusion of more artificial sweetened unhealthy beverages when reducing purging behaviours. Being so meals satiety sensation disappear about 14 minutes after the meal, which increases the risk of bingeing.20,32,33 Food inhibition and "prohibited" foods lead to anxiety and eating in secret which is accompanied with shame and culpability. CHO consumption may improve mood through serotoninergic system, thus preventing CHO craving and bingeing while distress mood.13,15,16
BMI normalization is similar to that found in other works but in AN there is a tendency to reduce their BMI after discharge.6,26 BFM proportion also predicts the pathology course with a lower percent of BFM related to poorer clinical outcome.34 In this work although BFM significantly improved during a year, the percentage is similar to the lower one in the Bodell et al. study.34
Unhealthy eating behaviours precede weight loss and malnutrition is related to complications and mortality.9,10 A healthy varied and balanced diet is essential to a proper recovery of an ED.9,12,23
Nutritional education effectiveness on ED patients is unclear but evidences indicate that food choice based on healthy topics improve food choice and eating behaviour.3,5,24,27,28,35 Specific programs based on variety and quality of the diet and concrete food are more effective than those based on energy even while diet variety related to clinical outcome remains controversial.12,24,26 Cognitive-behavioural treatment and nutritional education including eating sociability, exposure response preventing therapy, weight-changes experience, nutritional risks for abnormal eating behaviours and healthy food choice are effective in clinical evolution.1,8,20,22-24,31 In the present work 12.9% of ED patients chose menus based on WHO caloric profile recommendations and 3.2% did in accordance to lipid profile recommendations.
Limitations
The sample size was relatively small as it may influence the results obtained. Moreover, different subtypes on ED respond differently to nutritional education and they present different eating patterns4 so more researches are needed to clarify these differences.
While in the nutritional treatment of ED outpatients five intakes per day were recommended (3 major meals and 2 snacks) this work only had options for four intakes per day because this style is more frequent among Spanish population.
Giving patients cards with food options may influence their food choice so it would be preferable working freely without cards to be able to assess patients menu planning capacity.
Body composition measures were not carried out in a standard protocol as neither menstruation period nor food and beverages intake were took into account because it was measured during treatment visiting before starting the assignment.
Results show a weekly menu food choice so it could not be considered as a real food menu. Even food choice highly determines what patients will eat, it is not what they really had eaten. Self-report menu may have been under-reporting or over-reporting while patients may had been choosing their menu in accordance to what they thought their therapists wanted them to choose.
Conclusion
ED patients present a maladaptive eating behaviour that tends to maintain after body composition normalization. Healthy food choice, diet variety, energy-density, high fat and high palatable food consumption, proper Hunger-satiety sensations, adequate weight-changes perception, BMI maintenance in accordance to peers without ED symptomatology and BFM proportions are related to a better outcome and a lower relapse prevalence. Different studies support that nutritional interventions along with psychological and psychiatric treatments are effective to improve eating behaviours and to normalize BMI and body composition. In addition, these interventions contribute to improve the food choice ability when diet planning.
However, more researches are needed to clarify food choices differences among different ED and long-term nutritional intervention treatment effectiveness.
References
1. Renner B, Sproesser G, Stronhbach S, Schupp HT. Why we eat what we eat. The Eating Motivation Survey (TEMS). Appetite 2012; 59: 117-28. [ Links ]
2. Patrick H, Nicklas TA. A review of family and social determinants of children's eating patterns and diet quality. J Am Coll Nutr 2005; 24 (2): 83-92. [ Links ]
3. Jáuregui-Lobera I, Bolaños-Ríos P. What motivates the consumer's food choice? Nutr Hosp 2011; 26 (6): 1313-21. [ Links ]
4. Jacquier C, Bonthoux F, Baciu M, Ruffieux B. Improving the effectiveness of nutritional information policies: assessment of unconscious pleasure mechanisms involved in food-choice decisions. Nutrition Reviews 2012; 70 (2): 118-31. [ Links ]
5. Bannon K, Schwartz MB. Impact of nutrition messages on children's food choice: Pilot study. Appetite 2006; 46: 124-9. [ Links ]
6. Quiles-Marcos Y, Balaguer-Solá I, Pamies-Aubalat L, Quiles-Sebastián MJ, Marzo-Campos J, Rodríguez-Marín J. Eating habits, physical activity, consumption of substances and eating disorders in adolescents. Spanish J Psychol 2011; 14 (2): 712-23. [ Links ]
7. Lindeman M, Stark K. Loss of pleasure, ideological food choice reasons and eating pathology. Appetite 2000; 35: 263-8. [ Links ]
8. Korinth A, Schiess S, Westenhoefer J. Eating behaviour and eating disorders in students of nutrition sciences. Public Health Nutrition 2009; 13 (1): 32-7. [ Links ]
9. Jáuregui-Lobera I, Bolaños-Ríos P. Choice of diet in patients with anorexia nervosa. Nutr Hosp 2009; 24 (6): 682-7. [ Links ]
10. Schebendach J, Mayer LE, Devlin MJ, Attia E, Contento IR, Wolf RL, Walsh BT. Food choice and diet variety in weight-restored patients with anorexia nervosa. J Am Diet Assoc 2011; 111 (5): 732-6. [ Links ]
11. Mayer LES, Schebendach J, Bodell LP, Shingleton RM, Walsh BT. Eating behaviour in Anorexia Nervosa: Before and after treatment. Int J Eat Disord 2011; 45 (2): 290-3. [ Links ]
12. Schebendach JE, Mayer LES, Devlin MJ, Attia E, Contento IR, Wolf RL, Walsh BT. Dietary energy density and diet variety as predictors of outcome in anorexia nervosa. Am J Clin Nutr 2008; 87: 810-6. [ Links ]
13. Hetherington MM, Altemus M, Nelson ML, Bernat AS, Gold PW. Eating behaviour in bulimia nervosa: multiple meal analyses. Am J Clin Nutr 1994; 60: 864-73. [ Links ]
14. Theim KR, Tanofsky-Kraff M, Salaita CG, Haynos AF, Mirch MC, Ranzenhofer LM et al. Children's descriptions of the foods consumed during loss of control eating episodes. Eat Behav 2007; 8 (2): 258-65. [ Links ]
15. Spring B, Schneider K, Smith M, Kendzor D, Appelhans B, Hadeker D, Pagoto S. Abuse potential of carbohydrates for overweight carbohydrate cravers. Psychopharmacology (Berl) 2008; 197 (4): 637-47. [ Links ]
16. Corsica JA, Spring B. Carbohydrate craving: A double-blind, placebo controlled test of the self-medication hypothesis. Eat Behav 2008; 9 (4): 447-54. [ Links ]
17. Mena JD, Sadeghian K, Baldo BA. Induction of hyperphagia and carbohydrate intake by mu-opioid receptor stimulation in circumscribed regions of frontal cortex. J Neurosci 2011; 31 (9): 3249-60. [ Links ]
18. Rolls BJ, Andersen AE, Moran TH, McNeils AL, Baier HC, Fedoroff IC. Food intake, hunger and satiety after preloads in women with eating disorders. Am J Clin Nutr 1992; 55: 1093-103. [ Links ]
19. Sysko R, Walsh BT, Schebendach J, Wilson T. Eating behaviour among women with anorexia nervosa. Am J Clin Nutr 2005; 82: 296-301. [ Links ]
20. Sunday SR, Halmi KA. Eating behaviour and eating disorders: the interface between clinical research and clinical practice. Phychofarmacology Bulletin 1997; 33 (3): 373-9. [ Links ]
21. Sandy KJ, Chernecki LL, Leichner PP. Eating disorders patient's opinions of the cafeteria-style vs. hospital-style presentation of meals. J Am Diet Assoc 2007; 107 (3): 376-8. [ Links ]
22. Steinglass J, Albano AM, Simpson HB, Schebendach J, Attia E. Fear of food as a treatment target: exposure and response prevention for anorexia nervosa in an open series. Int J Eat Disord 2012; 45: 615-21. [ Links ]
23. Bolaños Ríos P. Nutritional treatment in eating disorders. In: Jáuregui Lobera I editor. Relevant topics in eating disorders. Croatia: Intech; 2012, pp. 357-82. [ Links ]
24. Loria V, Gómez C, Lourenço T, Pérez A, Castillo R, Villarino M et al. Evaluación de la utilidad de un programa de educación nutricional en trastornos de la conducta alimentaria. Nutr Hosp 2009; 24 (5): 558-67. [ Links ]
25. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders: DSM IV-RT. Washington DC: American Psychiatric Association; 2000. [ Links ]
26. Schebendach J, Mayer LES, Devlin MJ, Attia E, Walsh BT. Dietary Energy Density and Diet Variety as Risk Factors for Relapse in Anorexia Nervosa: A Replication. Int J Eat Disord 2012; 45: 79-84. [ Links ]
27. Devalla JE, Hamer RM, Kanodia A, Reyes-Rodríguez ML, Bulik CM. Diet and Physical Activity in Women Recovered from Anorexia Nervosa: A Pilot Study. Int J Eat Disord 2011; 44 (4): 376-82. [ Links ]
28. Hill AJ. Motivation for eating behaviour in adolescent girls: the body beautiful. Proceedings of the Nutrition Society 2006; 65: 376-84. [ Links ]
29. Woolhouse M, Day K, Rickett B, Milnes K. Cos girls aren's supposed to eat like pigs are they? Young women negotiating gendered discursive constructions of food and eating. J Health Psychol 2012; 17 (1): 46-56. [ Links ]
30. Burgic-Radmanovic M, Gavric Z, Strkic D. Eating behaviour disorders of female adolescents. Psychiatria Danubina 2009; 21 (3): 297-301. [ Links ]
31. Farrow CV, Tarrant M. Weight-based discrimination, body dissatisfaction and emotional eating: The role of perceived social consensus. Psychology and Health 2009; 24 (9): 1021-34. [ Links ]
32. Hawks SR, Madanat HN, Merrill RM, Goudy MB, Miyagawa T. A cross-cultural analysis of motivation for eating as a potential factor in the emergence of global obesity: Japan and the United States. Health Promotion International 2003; 18 (2): 153-62. [ Links ]
33. Siega-Riz A, Haugen M, Meltzer HM, Von Holle A, Hamer R, Torgersen L et al. Nutrient and food group intakes of women with and without Bulimia Nervosa and Binge Eating Disorder during pregnancy. Am J Clin Nutr 2008; 87 (5): 1346-55. [ Links ]
34. Bodell LP, Mayer LE. Percent body fat is a risk factor for relapse in anorexia nervosa: a replication study. Int J Eat Disord 2011; 44 (2):118-23. [ Links ]
35. Sandy KJ, Chernecki LL, Leichner PP. Eating Disorder Patient's Opinion of Cafeteria-Style vs. Hospital-Style Presentation of Meals. J Am Diet Assoc 2007; 107 (3): 376-8. [ Links ]
![]() Correspondence:
Correspondence:
Inmaculada Ruiz-Prieto
Behavioral Sciences Institute
C/ Fernando IV, 24-26
41011 Seville. Spain
E-mail: inma.irp@gmail.com
Recibido: 20-V-2013
Aceptado: 29-V-2013