Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Nutrición Hospitalaria
versión On-line ISSN 1699-5198versión impresa ISSN 0212-1611
Nutr. Hosp. vol.28 no.6 Madrid nov./dic. 2013
https://dx.doi.org/10.3305/nh.2013.28.6.6860
ORIGINAL / Pediatría
Impact of an intervention nutrition program during prenatal on the weight of newborns from teenage mothers
Impacto de un programa de intervención nutricional prenatal en el peso de los recién nacidos de madres adolescentes
Marta Maria Antonieta de Souza Santos1, Denise Cavalcante de Barros1,2, Jamile Lima Nogueira2, Miriam Ribeiro Baião1 and C. Saunders1
1Research Group on Maternal and Child Health (Grupo de Pesquisa em Saúde Materna e Infantil - GPSMI). Instituto de Nutrição Josué de Castro. Universidade Federal do Rio de Janeiro. Brasil.
2Escola Nacional de Saúde Pública Sérgio Arouca. Fundção Oswaldo Cruz. Brasil.
ABSTRACT
Introduction: The nutritional care for teenage mothers had been studied as a factor that influences the course of pregnancy and neonatal outcomes, especially in birth weight.
Objective: Evaluate the effect of a prenatal intervention nutrition program, with early start of the nutritional care and individualized attendance on teenage mother newborns' weight.
Methods: Not randomized study of intervention performed with 746 teenage mothers (14 to 19 years old), subdivided in historic control group (GI; n = 542) and intervention group (GII; n = 204). The dependent variable was the low birth weight (LBW). The independent variables assessed were: sociodemographic (mother age, skin color, instruction level and sanitation conditions), anthropometric (mother's height, pre-gestational nutritional study and adequacy of gestational weight gain), obstetric (gestational age in first prenatal consultation, number of pregnancies, childbirths and abortions, interdelivery and inter-gestational intervals), prenatal attendance (number of prenatal and nutritional attendance consultations) and conditions of the newborn (birth weight and duration of the pregnancy). Data were analyzed by Poisson regression with robust variance.
Results: The average of maternal age at delivery was 17,5 years old (standard deviation 1,59). The percentage of LBW considerably reduced from 11,3% in GI to 2,9% in GII (p < 0,001). We observed in the multivariate model that the teenage mothers who have not received the intervention presented 3,5 more prevalence (GI, RP adjusted 3,5; 95% CI 1,49-8,44) to give birth to a low weight newborn.
Conclusion: The participation of the teenage mother in the prenatal nutrition care program proposed here contributed to the reduction of the low weight of newborns.
Key words: Teenage pregnancy. Low weight newborn. Prenatal nutrition. Prenatal care.
RESUMEN
Introducción: La atención nutricional a la adolescente embarazada se ha estudiado como un factor que influye en la evolución de los resultados del embarazo y neonatales, especialmente en el peso al nacer.
Objetivo: Evaluar el efecto de un programa de intervención nutricional prenatal, con inicio temprano de la asesoría nutricional y seguimiento individualizado, sobre el peso de los recién nacidos de madres adolescentes.
Métodos: Estudio de intervención no aleatorio con 746 adolescentes embarazadas (14 a 19 años), subdivididas entre grupo de control histórico (GI; n = 542) y grupo de intervención (GII; n = 204). La variable dependiente fue el bajo peso al nacer (BPN). Las variables independientes evaluadas fueron: sociodemográfica (edad materna, color de piel, nivel educacional y condiciones de saneamiento), antropométricas (altura, situación nutricional previa a la gestación adecuación incremento de peso en la gestación), obstétricas (edad gestacional en la primera consulta prenatal, número de embarazos, nacimientos y abortos, intervalo entre nacimientos y gestaciones), de la atención prenatal (número de citas médicas prenatales y citas de asistencia nutricional) y las condiciones del recién nacido (peso al nacer y la duración del embarazo). Los datos fueron analizados por regresión de Poisson con varianza robusta.
Resultados: La edad materna promedio al nacer fue de 17,5 años (desviación estándar 1.59). El porcentaje de BPN sufrió una reducción significativa de 11,3% en GI a 2,9% en GII (p < 0,001). El modelo multivariado mostró que las adolescentes embarazadas que no recibieron la intervención mostraron 3,5 veces más alta prevalencia (GI RP ajustada 3,5; IC 95% 1,49-8,44) de dar a luz a un recién nacido de bajo peso.
Conclusión: La investigación concluye que la participación de adolescentes embarazadas en un programa de atención nutricional prenatal contribuye a la reducción del bajo peso al nacer en sus descendientes.
Palabras clave: Embarazo adolescente. Recién nacido de bajo peso. Nutrición prenatal. Atención prenatal.
Abbreviations
LBW: low birth weight.
PN: prenatal.
GI: historic control group.
GII: intervention group.
WHO: World Health Organization.
BMI: body mass index.
TGWG: total gestational weight gain.
RP: prevalence ratio.
CI: Confidence interval.
LMP: Last menstrual period.
SD: Standard deviation.
Introduction
The discussion about teenage pregnancy falls undoubtedly into many and important areas of knowledge. Under biologic approach, authors1-3 state that, especially in less than 15 years old teenagers, the pregnancy is biologically considered a high risk pregnancy, due to higher incidence of obstetric and perinatal complications, such as low weight at birth (LBW), small to gestational age, preterm delivery, premature amniorrhexis, anemia, hypertensive disorders of pregnancy and gestational diabetes.
Throughout the years, scientifically endorsed procedures have been incorporated to the prenatal program (PN). Scientific evidences4-7 have been shown that this improvement allowed the expansion of universal access, early and adequate attendance of the mother, as well as safe delivery offer and post-delivery attendance. However, in spite of the gains, the maternal and perinatal morbimortality markers remain unsatisfactory in all Brazilian regions, even disregarding the differences.
The challenge of implementing a great combination of interventions that reduces the prevalence of LBW remains, and thus may contribute to the prevention of type 2 diabetes, hypertension and cardiovascular disease in fetuses in adult life8. Recent studies have been shown that interventions aiming the dietary counseling with appreciation of the mother's sociocultural component contribute for a healthy pregnancy and with satisfactory perinatal results8-10.
Accordingly, it is notoriously important that the interventions must be identified and evaluated regarding type, intensity and effectiveness which present a better association with positive obstetric and perinatal outcomes in teenage mothers10-14.
The objective of the study is to evaluate the effect of a prenatal nutrition care program for teenage mothers on the birth weight.
Methods
It is a non-randomized intervention study with historic control group15, performed with 746 teenage mothers (14-19 years old) in public healthcare in Rio de Janeiro, Brazil.
Two reasons led to this choice: a) ethical grounds of the research16, especially regarding the principle of beneficence, which states that the actions of the researchers must aim at the best for the subject, from the ethical and technical care point of view17 and; b) because of the difficulty to control the influence of real conditions in which the health programs and actions are performed.
The control group (GI) contains all the teenagers (n = 542) whose deliveries occurred between july 2004 and january 2006 (before the intervention). The criteria of inclusion in this group were: less than 20 years old pregnant at the delivery, with no pre-existing chronic diseases and single fetus pregnancy. Data were collected from the records, using the instruments tested before in pilot study.
The prenatal nutrition care program for teenage mothers (intervention) consisted in the nutrition attendance of a prospective cohort of 227 teenage mothers (GII), from the first PN consultation to the immediate post-delivery, between November 2007 and February 2010. The criteria for inclusion in the cohort were: maximum age of 19 years old when registering the PN, nutrition care start simultaneous to the first PN consultation, single fetus pregnancy and no pre-existing chronic diseases.
For the calculation of the sample size, the significance level established was 5%, the power of the study in 90% to detect minimum difference of 15% between two proportions. The loss standard was evaluated considering the distribution of the follow-up final rate.
The intervention
The main feature was the nutrition care with early beginning and individualized and detailed nutritional evaluation of the teenage mother, performed in a minimum of 4 consultations throughout the PN and with the development of surveillance actions, prevention and recovery of clinical and nutritional (inadequacy on the pregnant weight gain, anemia, hypertensive disorders of pregnancy, gestational diabetes, digestive symptomatology, and others). The patients received a diet calculated to estimated weight gain until delivery, a list of food substitutions and guidelines for intercurrences. The teenages also participated at least in three group consultations with the multiprofessional team, when they received more information about nutrition during pregnancy and their doubts were clarified.
Dependent and independent variables
The dependent variable was the low birth weight (LBW), defined by World Health Organization (WHO)18 as less than 2,500 g. The independent variables included in the analysis were: (1) sociodemographic: maternal age at delivery, skin color (self-rated as white, brown or black), marital status (single, married or living with the partner), education level (incomplete basic education; complete basic education, incomplete high school, complete high school or more) and sanitation conditions at home (adequate -piped and treated water, sewage system and regular garbage collection; inadequate -in the absence of one of these services); (2) anthropometric: stature (< 1.45 m; 1.45 or more), pre-gestational nutrition status (low weight, adequate, overweight, obesity) and classification of the adequacy of total gestational weight gain (insufficient; adequate; excessive); (3) obstetric: gestational age when starting the PN (according to last menstrual period-LMP), number of pregnancies, deliveries and abortions, interdelivery and intergestational interval; (4) PN attendance: number of PN consultations (1 to 5; 6 or more) and PN nutrition attendance (1 to 3; 4 or more); (5) newborn: birth weight (< 2,500 g; 2,500 g or more) and gestational age at birth, according to LMP (< 37 weeks; 37 weeks or more).
Among the various cut off points, the pre-gestational body mass index-BMI [weight (kg)/stature (m2)] - was used to evaluate the nutrition status up to two months before the gestation. The cut off points recommended by the Ministry of Health19 and adapted by Saunders et al20 were used, considering the age of the teenagers in years and months according to proposition of WHO21: low weight (BMI/age < 5-percentile), eutrophic (BMI/age > 5-percentile to < 85-percentile), overweight (BMI/age > 85-percentile to < 95-percentile) and obesity (BMI/age > 95-percentile).
For the calculation of total gestational gain (TGWG), the pre-gestational weight was subtracted from the pre-delivery weight or from the weight registered at the last PN consultation. The adequacy of TGWG was evaluated based on the table of ranges of weight gain according to the pre-gestational nutrition status, recommended by Ministry of Health22, from the publication of pre-gestational BMI.
Statistical Analyses
In the data analysis, we used the t-Student test for averages, chi-squared test for frequencies and bivariate analysis to identify the variables associated to the outcome (LBW), based on the prevalence ratios (RP) and withdrawal periods of 95%, according to the groups of study. The multivariate analysis was performed for estimation of RP adjusted, using Poisson regression with robust variance, being the groups of study the main independent variable. We have also tested other variables which have shown differences between the groups, or association with outcome, in the bivariate analysis, accepting the value of p < 0.05 for this choice for statistical significance. All analyses were performed in the statistical package SPSS for windows version 17.0.
The study was planned respecting the ethical aspects provided in resolution 196/96 of National Council of Health-CNS17 and approved by the Ethical Committee in Research of Maternity School of Federal University of Rio de Janeiro.
Results
The average age of the teenagers mothers at delivery was 17.5 years old (standard deviation - SD 1.59), 17.3 years old in GI and 17.9 years old in GII.
The loss of follow-up in GII was 10.13% (n = 23) having as main motivation the occurrence of the delivery in other maternity, with the loss of the records and lack of information about the newborn. In all the variables studied, there were no differences between the teenagers whose records had information about the birth weight and those who had not.
The table I consolidates the sociodemographic data and the data of pre-gestational nutrition status of the studied mothers. The groups are similar regarding the sanitation conditions at home, with higher proportion of mothers who lived in a place with adequate conditions for both (p= 0.942). Concerning alcohol use, there is also no difference between the groups, with 8,5% of the teenagers in GI and 8.8% in GII presenting this behavior during the pregnancy (p = 0.919). Otherwise, the instruction level was different between the groups, with the number of mothers with incomplete and complete basic education increasing from 17.1% (GI) to 57.6% (GII) (p < 0.001), and the proportion of married teenagers or living with the partner increasing too (GI = 10.0%, GII = 41.6%; p < 0.001). There was also a difference concerning smoking during the pregnancy, with a significant reduction of smokers in GII (7.5%) in relation to GI (14.0%; p < 0.001). The skin color presented differences too, with 51.6% of the teenagers in GI and 70.6% in GII self-rated brown or black (p < 0.001). The distribution of the teenagers according to pre-gestational BMI presented considerable difference between the groups: 87.5% of the teenagers in GI and 77.6% in GII were eutrophic; the proportion of teenagers with overweight and obesity was higher in GII (20.1%) in relation to GI (11.4%) (p = 0.041).
Still on table I, there is the frequency of the adequacy of the birth weight according to the groups of study. The percentage of LBW reduced from 11.3% in GI to 2.9% in GII (p < 0.001). The average weight at birth was 3,032 g (SD 602) for GI and 3,207 g (SD 449) for GII (data not presented in table).
The comparison of the averages of the maternal variables and prenatal assistance by groups of study (GI and GII) can be observed in table II. There is a considerable difference between the groups for almost every variable, except pre-gestational BMI, gestational weight gain and number of PN consultations PN (p > 0.05), with unfavorable values always in GI.
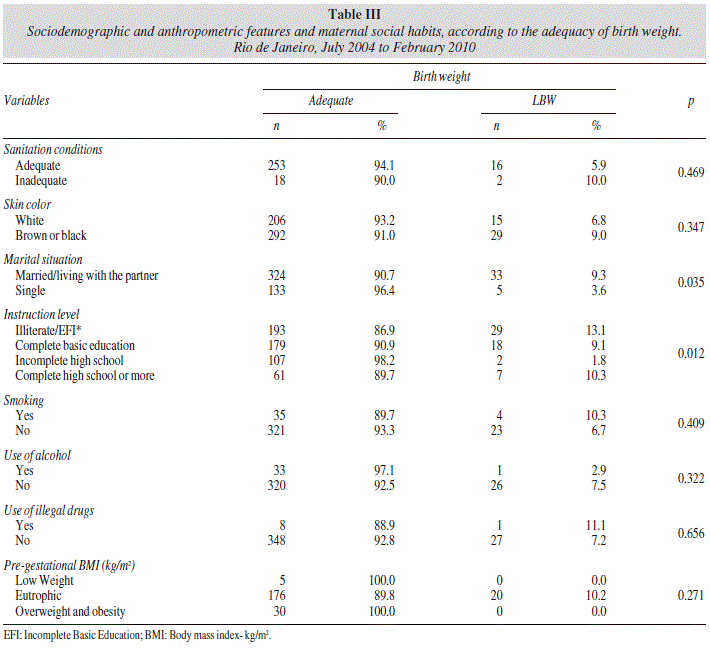
In table III, we can observe that the prevalence of LBW was higher among the married teenagers or who lived with the partner, compared to the single ones (9.3% and 3.6%, p = 0.035) and to the lower instruction level (p = 0.012). The other variables, including pre-gestational BMI, have not presented association with the birth weight (p > 0.05).
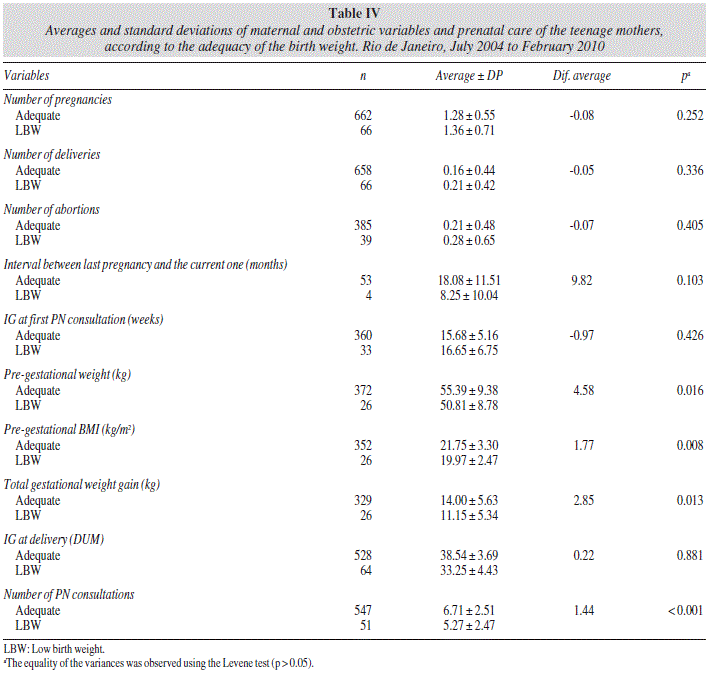
Otherwise, data of table IV show an association between LBW and the average of the variables: pre-gestational weight (p = 0.016), pre-gestational BMI (p = 0.008), total gestational weight gain (p = 0.013) and number of PN consultations (p < 0.001), with the unfavorable results remaining in the pre-intervention group (GI).
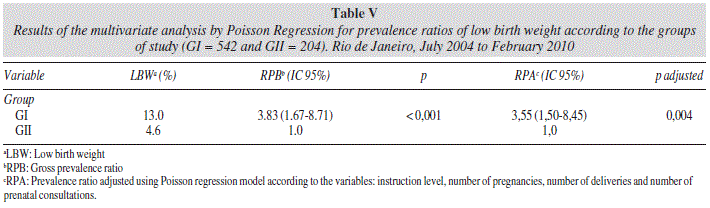
In the multivariate analysis (table V), we observe that the occurrence of LBW was kept highly determined by the group of study to which the teenage belonged. In other words, among the teenage mothers of the pre-intervention group (GI), we observe a prevalence adjusted 3.5 higher (RP adjusted 3.5; 95% CI 1.50-8.45) of LBW, compared to those which formed the GII, showing the protective effect of the nutrition care, even after the adjustment for the confounding variables (instruction level, number of pregnancies, deliveries and prenatal consultations).
Discussion
Initially, some considerations must be made regarding the design of this study. It is notorious that the standards for the evaluation of interventions are the randomized, double-blind and controlled studies. However, these strategies of investigation are limited against the compromise with the ethical questions of the research, particularly regarding the choice of a control group. Aiming to remedy this limitation, we chose using the comparison pre and post intervention by historic control, whose plausibility is shown by the reduction of the risk factors associated, as well as by the reduction of the problem itself- LBW.
Concerning the general development of the nutrition care program, the results showed a satisfactory accessibility, with a low proportion of loss of follow-up.
Despite of the result on the study of significant contribution of nutritional monitoring, initiated early and maintained throughout the prenatal, the adequacy of the birth weight of children of teenage mothers. In comparison between groups was possible to observe the contribution of nutritional care in reducing the prevalence of LBW, which occurred in 11.3% of GI went to 2.9% in GII (p < 0.001).
LBW was chosen as dependent variable for it recognized by WHO23 since the beginning of the eighties as the most important single factor for child's survival, growing and development. More recently, LBW has been related to the occurrence of chronic diseases in adult life such as obesity, type 2 diabetes and hypertension24,25. Because of its multicausal nature, LBW evolves a combination of risk factors, especially the unfavorable sociodemographic conditions, reproductive history, maternal nutrition status before and after the pregnancy, smoking and quality and access of prenatal care26.
The analysis had included maternal age as a risk factor for the LBW associated with biological immaturity of teenagers, the groups are similar, since the average age in both groups was 17.5 years and the literature suggests increased risks of adverse perinatal outcomes for teenage mothers under 15 years old26,27.
Otherwise, other authors1,2,28-30 have been shown that the maternal age itself is not a good predictive factor on the determination of the birth weight and must be considered together with the insertion of the teenage in social contexts characterized by poverty, low instruction level, black ethnicity, unstable marital situation or absence of partner, maternal nutrition status and prenatal care. In this study, although we have found sociodemographic differences between pre and post intervention groups, they are not capable to be kept as explanatory variable to define the birth weight.
Drug's use during pregnancy represents important risk factor for LBW; however, amongst all the drugs consumed by the mothers, smoking is undoubtedly the most common, and it can cause intrauterine hypoxia, leading to fetal malnutrition31. In this study, we found that this practice does not present association with LBW and its frequency was less expressive among the mothers who participated in the intervention group (GII). These results are similar to what Freire et al.32 found. They indicate the nutrition care as a protective factor against smoking during pregnancy, once the mothers who had no nutrition care presented three times more chance of smoking during pregnancy compared to the ones who had professional attendance.
Comparing the average of the variables number of pregnancies, deliveries and abortions between GI and GII, we verified that, in spite of the differences identified with statistical importance, they do not denote clinical significance because the values are low too, once in both groups most of the teenagers were primiparous.
The final analysis of this study identified statistical association between the frequency of the teenager to 6 or more PN consultations and her participation in the nutrition care program with lower occurrence of LBW. It is well documented and recognized the efficiency of the early and adequate nutritional counseling and prenatal care over the weight and age of teenage the mothers at delivery,6,28,33. According to Orstead et al.34, since the sixties the efficiency of prenatal nutritional counseling has been registered by North American scholars.
These authors34 also evaluated the efficiency of the prenatal nutrition care on the mother weight gain, the birth weight and the cost-effectiveness of PN. The results showed that the mothers who received the intensive nutrition care together with each PN consultation gained an average of 2.5 kg more and had a newborn 0.1 kg heavier, compared to the mothers who frequented only one 30 minutes nutrition care together with others, offered in the PN first consultation. The nutritional counseling tested in this study34 was applied in group consultations, there was also the development of individualized diet for pregnant women by nutritionist, and the obstetrician reinforced the guidelines given by nutritionist.
The evaluation of the cost-benefit showed in the study mentioned above34 pointed to a lower investment for the offer of intensive nutritional counseling (time, nutritionist and direct costs for visits to the clinic) than the one for single nutrition attendance. LBW was higher in the group of mothers who received the single attendance, causing an increase of expenses with special care neonatal units and, therefore, the intensive nutrition care program is most cost-effective.
In conclusion, the results found here reinforce that the PN care considerably contributes for the pregnant and the newborn's health, but it shows that it can be better though. The health system is responsible to provide the necessary assistance to improve the efficiency and effectiveness of PN health actions and the health professional must support the expansion of the nutrition counseling programs with universal access, early beginning and individual and customized attendance throughout the
Intervention nutrition during prenatal from teenage mothers pregnancy, in order to considerably reduce the occurrence of low weight at birth among the newborns, especially the ones from teenagers mothers.
Acknowledgments
The authors would like to thank the partnership with Centro Colaborador de Alimentação e Nutrição-Região Sudeste. Escola Nacional de Saúde Pública/ FIOCRUZ.
References
1. Chen CW, Tsai CY, Sung FC, Lee YY, Lu TH, Li CY, Ko MC. Adverse birth outcomes among pregnancies of teen mothers: age-specific analysis of national data in Taiwan. Child Care Health Dev 2010 Mar; 36 (2): 232-40. [ Links ]
2. Chen XK, Wen SW, Fleming N; Demissie K, Rhoads GG, Walker M. Teenage pregnancy and adverse birth outcomes: a large population based retrospective cohort study. Int J Epidemiol 2007; 36: 368-73. [ Links ]
3. Conde-Agudelo A, Belizan JM, Lammers C. Maternal-perinatal morbidity and mortality associated with adolescent pregnancy in Latin America: cross-sectional study. Am J Obstet Gynecol 2005; 192 (2): 342-9. [ Links ]
4. Goldenberg P, Figueiredo MCT, Souza e Silva R. Gravidez na adolescência, pré-natal e resultados perinatais em Montes Claros, Minas Gerais, Brasil. Cad. Saúde Pública 2005; 21 (4): 1077-86. [ Links ]
5. Gama SGN, Szwarcwald CL, Sabroza AR, Branco VC, Leal MC. Fatores associados à assistência pré-natal precária em uma amostra de puérperas adolescentes em maternidades do Município do Rio de Janeiro, 1999-2000. Cad. Saúde Pública 2004; 20, Suppl 1:101-11. [ Links ]
6. Young J, Trotman H, Thame M. The impact of antenatal care on pregnancy performance between adolescent girls and older women. West Indian Med J 2007; 56 (5): 414-20. [ Links ]
7. Calderon IMP, Cecatti JG, Vega CEP. Intervenções benéficas no pré-natal para prevenção da mortalidade materna. Rev Bras Ginecol Obstet 2006; 28 (5): 310-15. [ Links ]
8. Alam DS. Prevention of Low Birthweight. In: Kalhan SC, Prentice AM, Yajnik CS (eds). Emerging Societies - Coexistence of Childhood Malnutrition and Obesity. Nestlé Nutr Inst Workshop Ser Pediatr Program 2009; 63: 209-25. [ Links ]
9. Mersal FA, Esmat OM, Khalil GM. Effect of prenatal counselling on compliance and outcomes of teenage pregnancy. East Mediterr Health J 2013 Jan; 19 (1): 10-7. [ Links ]
10. Guerra AFFS, Heyde MED, Mulinari RA. Impacto do estado nutricional no peso ao nascer de recém nascidos de gestantes adolescentes. Rev Bras Ginecol Obstet 2007; 29 (3): 126-33. [ Links ]
11. Santos GHN, Martins MG, Sousa MS. Gravidez na adolescência e fatores associados com baixo peso ao nascer. Rev Bras Ginecol Obstet 2008; 30 (5): 224-31. [ Links ]
12. Carvalho DS e Novaes HMD. Avaliação da implantação de programa de atenção pré-natal no Município de Curitiba, Paraná, Brasil: estudo em coorte de primigestas. Cad Saúde Pública 2004; 20, suppl. 2: S220-30. [ Links ]
13. Costa MCO, O Neto AF. Abordagem nutricional de gestantes e nutrizes adolescentes: estratégia básica na prevenção de riscos. J Pediatr 1999; 75 (3): 161-6. [ Links ]
14. Brown JE. Caveat emptor to Ellison's "Prenatal nutrition counseling: Two caveats." Journal of the American Dietetic Associa tion (Letter) 1996; 96: 449-50. [ Links ]
15. Rothman KJ, Greenland S, Lash TL. Tipos de estudos epidemiológicos. In: Epidemiologia Moderna. Porto Alegre: ARTMED, 2011: 107-122. [ Links ]
16. Brasil. Comissão Nacional de Ética em Pesquisa. Cadernos de Ética em Pesquisa. CONEP. ANO I, número 1, julho de 1998. Brasil: CONEP. [ Links ]
17. Brasil - Ministério da Saúde. Diretrizes e normas regulamentadoras de pesquisas envolvendo seres humanos. Resolução 196/96 do Conselho Nacional de Saúde. Rio de Janeiro: Fundação Oswaldo Cruz, 1998. [ Links ]
18. Organização Mundial da Saúde. CID-10. Classificação estatistica internacional de doenças e problemas relacionados à saúde. 10a Revisão. São Paulo: EDUSP. 1998. p. 1184. [ Links ]
19. Brasil. Ministério da Saúde. SISVAN. Protocolos do Sistema de Vigilância Alimentar e Nutricional-SISVAN na assistência à saúde. Brasília: Ministério da Saúde. 2008. [ Links ]
20. Saunders C, Accioly E, Costa RSS, Lacerda EMA, Santos MMAS. Gestante Adolescente. In: Accioly E, Saunders C, Lacerda EMA. Nutrição em Obstetricia e Pediatria. Rio de Janeiro: Cultura Médica. 2012: 151-175. [ Links ]
21. World Health Organization - WHO. WHO reference 2007: growth reference data for 5-19 years. http://www.who.int/growthref/en/ (acessado em 10 de abril 2013). [ Links ]
22. Brasil. Ministério da Saúde. Secretaria de Atenção à Saúde. Departamento de Ações Programáticas Estratégicas. Área Técnica de Saúde da Mulher. Pré-Natal e Puerpério: atenção qualificada e humanizada - Manual Técnico. Brasilia: DF, MS, 3a ed. revisada, 2006. [ Links ]
23. World Health Organization - WHO. The incidence of low birth weight: a critical review of available information, Wld Hlth Statist. Quart 1980; 33: 197-224. [ Links ]
24. Bismarck-Nasr EM, Frutuoso MFPetroli, Gamabardella AMD. Efeitos tardios do baixo peso ao nascer. Rev Bras Crescimento Desenvolv Hum 2008; 18 (1): 98-103. [ Links ]
25. Horta BL, Barros FC, Victora CG, Cole TJ. Early and late growth and blood pressure in adolescence. J Epidemiol Community Health 2003; 57 (3): 226-30. [ Links ]
26. Keskinoglu P, Bilgic N, Picakciefe M, Giray H, Karakus N, Gunay T. Outcomes and Risk Factors of Adolescent Mothers. J Pediatr Adolesc Gynecol 2007; 20: 19-24. [ Links ]
27. Fraser AM, Brockert JE, Ward RH. Association of young maternal age with adverse reproductive outcomes. N Engl J Med 1995; 332: 1113-7. [ Links ]
28. Gama SGN, Szwarcwaldb MCL, Theme Filha MM. Gravidez na adolescência como fator de risco para o baixo peso ao nascer no Municipio de Rio de Janeiro, 1996 a 1998. Rev Saúde Pública 2001; 35 (1): 74-80. [ Links ]
29. Mariotoni GGB e Barros Filho AA. A gravidez na adolescência é fator de risco para o baixo peso ao nascer? Jornal de Pediatria 1998; 74 (72): 107-13. [ Links ]
30. Kassar SB, Gurgel RQ, Albuquerque MFM, Barbieri MA, Lima MC. Peso ao nascer de recém-nascidos de mães adolescentes comparados com o de puérperas adultas jovens. Rev Bras Saude Mater Infant 2005; 5 (3): 293-9. [ Links ]
31. Leopércio W, Gigliotti A. Tabagismo e suas peculiaridades durante a gestação: uma revisão critica. J Bras Pneumol 2004; 30 (2): 176-85. [ Links ]
32. Freire K, Padilha PC, Saunders C. Fatores associados ao uso de álcool e cigarro na gestação. Rev Bras Ginecol Obstet 2009; 31 (7): 335-41. [ Links ]
33. Felice ME, Granados JL, Ances IG, Hebel R, Roeder LM, Heald FP. The young pregnant teenager. Impact of comprehensive prenatal care. J Adolesc Health Care 1981; 1: 193-7. [ Links ]
34. Orstead C, Arrington D, Kamath SK, Olson R, Kohrs MB. Efficacy of prenatal nutrition counseling: weight gain, infant birth weight, and cost-effectiveness. J Am Diet Assoc 1985; 85: 40-5. [ Links ]
![]() Correspondence:
Correspondence:
Claudia Saunders.
Instituto de Nutrição Josué de Castro.
Centro de Ciências da Saúde. Universidade Federal do Rio de Janeiro.
Av. Carlos Chagas Filho, 373, bl J. 2.o andar, sala 26. Cidade Universitaria.
21941-590 Rio de Janeiro. Brasil.
E-mail: claudiasaunders@nutricao.ufrj.br
Recibido: 22-V-2013.
1.a Revisión: 23-VII-2013.
Aceptado: 30-VII-2013.