Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Nutrición Hospitalaria
versión On-line ISSN 1699-5198versión impresa ISSN 0212-1611
Nutr. Hosp. vol.28 supl.5 Madrid sep. 2013
CONSENSUS DOCUMENT AND CONCLUSIONS
Successful intervention models for obesity prevention: The role of healthy life styles
Modelos exitosos de intervención para la prevención de la obesidad: el papel de los estilos de vida saludables
Vicente Martínez Vizcaíno1*, Jorge Cañete García-Prieto1, Blanca Notario-Pacheco1 and Mairena Sánchez-López1,2
1Social and Health Care Research Center. Universidad de Castilla-La Mancha. Cuenca. Spain
2School of Education. Universidad de Castilla-La Mancha. Ciudad Real. Spain
ABSTRACT
Children obesity is considered a serious public health problem around the world. In Spain, the prevalence of overweight/obesity is reaching alarming figures, exceeding 35% of the children. Several hypotheses suggest that the energy balance model does not fit very well when analyzing the causes of the current obesity epidemic and, although genetics seems to explain up to 30% of the likelihood to become obese in infancy, has been suggested that genetics might be influenced by environment factors including vigorous physical activity (PA). Some recent systematic reviews indicate that there is enough evidence about the effectiveness of interventions to prevent obesity in children 6-12 years old; however, the heterogeneity of the effect, and the potential selection, information and publication biases that undermine the validity of these studies, thus their results should be interpreted with caution. In Spain, an extracurricular PA program of leisure-time (MOVI) has evidenced some effectiveness on reducing the adiposity and on improving the lipid profile in schoolchildren. To overcome some weakness of MOVI program, a second edition of this study was designed. The objectives of this review are twofold: 1) to analyze latest data of the obesity epidemic in Spain; and 2) to describe the main features of MOVI-2 program, and overall of the successful interventions to prevent children obesity.
Key words: Obesity. Interventions. Children. School. MOVI program.
RESUMEN
La obesidad infantil continúa siendo un serio problema de salud pública en todo el mundo. Las cifras actuales en España son alarmantes, y se sitúan en torno al 35,4%. Hay varias hipótesis que apuntan a que el modelo de balance energético como causa de la obesidad infantil no se sostiene. Y aunque las razones genéticas parecen explicar hasta el 30% de la probabilidad de llegar a ser obeso, se ha sugerido que esta herencia podría ser influenciable por factores ambientales entre los que se encuentra la actividad física (AF) vigorosa. Aunque las últimas revisiones señalan que existe evidencia suficiente sobre la efectividad de las intervenciones para prevenir la obesidad en niños de 6-12 años, la heterogeneidad del efecto encontrado en los resultados y la posibilidad de sesgos de diseño y de publicación de los estudios hacen que los resultados deban interpretarse con cautela. En España la intervención MOVI, un programa extraescolar de AF de carácter recreativo, ha conseguido disminuir la adiposidad, y mejorar el perfil lipídico. Para superar potenciales limitaciones de la primera intervención, se diseñó una segunda edición. Los objetivos de esta revisión fueron: 1) analizar los últimos datos de la epidemia de la obesidad infantil en España; y 2) describir las principales características del programa MOVI-2, y en general de las intervenciones que han sido efectivas para prevenir la obesidad en niños.
Palabras clave: Obesidad. Intervenciones. Niños. Escuela. Programa MOVI.
Introduction
Children obesity remains a serious public health problem around the world1. In Spain, current prevalence rates range from 35% to 42%.2,3 Although recent studies have shown a leveling-off or even a decline in the prevalence of overweight/obesity in children in different countries of the world,4,5 in the period 2004-2010 prevalence of overweight in boys aged 8-11 years from Cuenca, Spain, increased from 21.6% to 28.0% and the percentage of body fat from 22.6% to 24.0%. In girls, however, the trend seems to have stabilized.2
In parallel to the growing trend in the overweight prevalence, during the last decade of the 20th century underweight prevalence was increasing in Spain, from 2.7% in 1992 to 9.2% in 2004 in children 9-10 years,6 and in other European countries7. Fortunately, latest estimations reported in Spanish children show that from 2004 to 2010 the underweight prevalence has not increased, and stands at around 8.5%.2
Therefore, the population approach for addressing the prevention of overweight, as in other public health problems, we should to be into account the classic good practice Latin axiom primum non nocere, so that it might be that interventions whose effectiveness on reducing overweight is controversial have also an undesirable effect increasing the proportion of underweight children.
Determinants of the obesity epidemic in Spanish children
At the individual level, body fat accumulation results from an imbalance between energy intake and energy expenditure. If intake exceeds expenditure the excess of energy will be stored as fat. On the other hand, it has been estimated that genetics susceptibility explains about the 30% of the likelihood of child will develop obesity,8 although this is a polygenic inheritance strongly influenced by the interaction genes, environment and lifestyle.9
However, at the population level non-genetic factors are the responsible for the frequency of obesity, including epigenetic,10 eating behavior patterns at an early age, activity/inactivity patterns, and other psychological, social and environmental factors.9 Nowadays, the relative importance of energy expenditure and intake in the development of the current obesity epidemic is a debatable issue. A recent review of studies addressing this question in different regions of the world11 concluded that in view of the great variability in the study designs, in the exposure and outcome measures used, and the wide population range in which the studies were based, the estimation of the importance of each one of these two factors, intake and energy expenditure, was not possible in children and teens.
In Spanish children, however, there are some considerations that worth to examine, and that leading us to suspect a greater importance of the decreasing of energy expenditure as determinant of the current obesity epidemic. First, data from both the AVENA study12 and the enKid study13 support the association between overweight and TV hours in Spanish children and adolescents. Furthermore, baseline measurement of an intervention study not yet published by our group,14 show that children who are overweight or obese consume on average less calories/day than children with normal weight, and these normal weight children less than thinness children. After a first view of these data might be argued that children with overweight/ obesity do less daily physical activity than less normal weigh children, but when we controlled in multivariate models for cardiorespiratory fitness levels, a variable closely related to physical activity levels, these differences in energy intake by weight categories remain unchanged. These results are in accordance with that reported from other studies,15,16 and support the new hypothesis proposed by Gutin suggesting that vigorous physical activity at early ages would have a pivotal role in the of stem cells differentiation in bone and muscle tissues through stimulation by mechanical influences such as physical activity17. If this theory were consolidated would have important implications in determine which is the best age range for implement preventive interventions, and which is the most appropriate type of activity for it.
There are several hypotheses that do not support the energy balance model for explaining the childhood obesity epidemic, and even though no one doubt of the importance of genetics on predicting obesity, it has been suggested that genetics could be very strongly influenced by environmental factors including vigorous physical activity.18,19
Efectividad de las intervenciones preventivas sobre obesidad infantil
A Cochrane systematic review aimed to evaluate the effectiveness of interventions for preventing obesity in children and adolescent concluded that there is enough evidence on the effectiveness of interventions to prevent obesity in children aged 6-12 years, although should be considered that the heterogeneity of the effect found in the studies, as well as the risk of design and publication biases, and therefore this results should be interpreted with caution. Furthermore this review concludes by recommending for future studies: 1) analyze the long-term results, 2) assess how those interventions that are effective can be maintained over time in a sustainable manner, 3) include economic evaluations, 4) potential damage reporting (i.e. eight reduction in thinner children, reduction of essential nutrients, etc.), 5) subgroup analysis by gender, location, race or socioeconomic status, 6) describe in detail the activities carried out in the intervention (to facilitate their applicability and transferability to other populations), and finally, 7) to focus on children 0-5 years.20
A recent meta-analysis whose objective was to assess the efficacy of intervention programs on the body mass index (bMi) of children and adolescents, as well as explore the possible differences between the school and after-school intervention programs showed school or after school interventions had a similar effect.21 Considering that in Spanish context seems very complicated to propose legislative changes aimed to include interventions to tackle children obesity in the schools curricula, the implementation of interventions at recess or after school seems to be more feasible.
The conclusions of a review that examines the systematic reviews and meta-analysis aimed to evaluate the effectiveness of programs addressing the prevention and control of childhood obesity indicates that information about the barriers and challenges encountered when designing and implementing interventions in real life situations will provide important information on feasibility and sustainability, and identify if failure or modest success of the intervention was due to a problem with the intervention's development, content or implementation.22
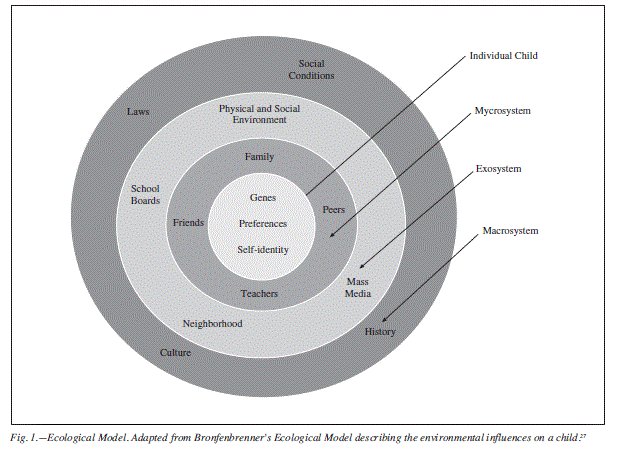
Most of the systematic reviews emphasize on the importance of taking into account the theoretical models of behavior's changes in which the intervention is based.23 The usefulness of these models in in the development of intervention strategies that affect multiple areas has been proven in several studies.24,25 One of the most commonly used is the socio-ecological model.26,27 This model distinguishes several levels on influence on behavior usually depicted as a graph with concentric circles (fig. 1). At the central level are represented the biological/genetic, physiological and sociocultural influences that make-up the individual's identity. In the second circle are placed personal relationships, the environment close to the children; this micro-system consisted of relationships with parents, teachers, sibling, and friends. A third level of influence it's known as exo-system, and includes physical and social environments that influence children's behavior, but without interacting (neighborhood and its built environment, media, location of the school, working conditions of parents, etc.). Finally, the macro-system (fourth level) influences the child's behavior; this macro-system includes traditions, social, culture, laws, history, etc., of the country where the child growths.
This paper review the characteristics of the most promising interventions.
Results
Table I shows characteristics of 12 effective school-based interventions on prevention obesity in children (6-12 years). All studies were randomized controlled trials, implemented in school area, and included as outcome BMI or prevalence of overweigh/obesity.
Six studies were conducted in the United States, one in South America, one in Australia and four in different countries of the European Union (Spain, Switzerland, Germany and Sweden). Most of the studies were done in school (with modifications into curriculum),28-36 two studies were done in after school schedule (FitKid and MOVI),37-40 and one was done jointly in school and after school (STOPP).41 The duration of follow-up ranged from 3 months to four years; of these 12 studies, 2 studies had a follow-up period of 3 months, 5 studies between 8 months and one and a half year, and 6 studies more than one and a half year (two, three o four years). Seven of the interventions included increase in physical activity levels or reduce sedentary time, and the rest combined increase in physical activity levels or reduce sedentary time and diet. It is noteworthy that none study exclusively focused on diet was identified. Five of them were designed from the perspective of theoretical models of behavior change (FitKid, Switch-play, PAAC, KISS and Planet Health).
Participants' characteristics
One study included girls only (Dance for Health) and the rest included both girls and boys, although only two of these reported sex specific results (MOVI and Planet Health). The mean age at baseline varied from 6 to 12 years (median 9.5 years). One study involved a participants group with overweight/obese (KOPS), and the rest involved children recruited from all body mass index categories.
Types of outcome measures
Five studies reported BMI or prevalence of over-weigh/obesity and seven studies reported furthermore BMI or prevalence of overweigh/obesity of at least one measure of adiposity. Three of them measured cardiovascular risk factors (FitKid, MOVI and KISS); four, objectively physical activity (KISS, Switch-play, PAAC and STOPP); four, fitness (FitKid, KISS, Healthy school, El Paso Catch); three, physical activity related behaviours (Dance for Health, Planet Health, KOPS) and three, diet-related behaviours (Planet Health, KOPS, STOPP). Only one study included results on quality of life (KISS).
Effectiveness of the interventions in Spanish settings
The MOVI interventions in schoolchildren
Two interventions focused on the promotion of physical activity in the school setting have been tested in the last years by our group. The distinguishing characteristics of MOVI interventions are the following: 1) in children in 4th and 5th of Primary School (age ranged 9-11 years); 2) recreational, non-competitive, leisure time physical activity; 3) open to all the children, and suitable for everyone, regardless of their body composition or motor skills; and 4) takes place outside school hours but in the school sports facilities (www.movidavida.org).
This intervention, in its first edition (three sessions per week, each one of 90 minutes of moderate and vigorous intensity physical activity, lasting two school years) showed moderate effect in reducing adiposity and improving the lipid profile, but did not significantly improve overall cardiometabolic risk because of did not reduce insulin levels.39,40 Our working hypothesis was that another intervention increasing the intensity of the program, putting more emphasis on the development of muscle strength, and including a weekend session on Saturday morning because we suspected that in the first edition compensating behaviors during weekend might be responsible of mitigate the effects of the intervention; therefore we implemented a 2nd edition of MOVI including two after school 90 minute sessions on school days and a 150-minute session on Saturday morning, during a school year) hypothesizing that this new intervention could be more effective on reducing obesity, but also remain acceptable to parents and school authorities. In addition, the MOVI-2 intervention,14 included as objectives to produce behavioral changes in children and parents similarly to other effective previous interventions (CATCH, M-SPAM).
The main objective of MOVI-2 was to evaluate the effectiveness of an intervention that essentially consisted of implementing a standardized leisure time physical activity program aimed to reduce overweight/obesity and other cardiovascular risk factors, and lasting one academic year. As secondary objectives we plan to evaluate the impact of MOVI-2 on other health-related variables: physical fitness, duration and quality of sleep, health-related quality of life, and academic performance. Among the most notable results of this cluster randomized clinical trial, in preliminary analysis, worth noting a decrease in body fat, an increase in lean mass, and a decreased in insulin levels.
The experience of these two consecutive interventions makes us feel able to provide some recommendations for future interventions to tackle against childhood obesity in the Spanish context:
1) Because of the magnitude and consequences of childhood obesity not only at this moment but also in the future, it is a priority testing the effectiveness of interventions for controlling this epidemic in Spain; otherwise we would expect an increase in morbidity/ mortality and other cardiovascular diseases in the coming years.
2) The most appropriate interventions in Spanish children to prevent obesity should be based on the promotion of physical activity so that: a) it has been repeatedly reported low levels of physical fitness in Spanish schoolchildren, particularly from data of the AVENA study;12 b) unpublished data from our group indicate that the caloric intake of overweight children is not greater than in normal weight or underweight children; c) a exclusively diet based intervention may not be free of risk for thinness children; and d) an intervention to promote physical activity based on playground games could improve other health-related aspects such as quality of life, academic performance, time and quality of sleep, etc.
3) Although it is generally accepted that BMI is the most useful and practicable indicator of excess of adiposity on clinical and population based studies, it should taken into account that BMI does not distinguish between fat and lean body mass. Therefore, it seems advisable include in population interventions focused on promoting physical activity in children as the main outcome, in addition to BMI, an indicator of body fat such as skin-fold thickness or body fat measured by bioimpedance,22 so that physical activity might reduce fat while increasing muscle mass, and as consequence the weight/height ratio would remain unchanged.17,39
4) Early infancy is probably the best opportunity to intervene, so that is considered the best age to establish perdurable healthy behaviors. Furthermore, it is known that the risk of obesity in adulthood is much higher when early adiposity rebound occurs.42
5) Consistent evidence indicate that genes explain up to 30% of the likelihood of becoming obese; however epigenetic hypothesis support that genetic expression could be influenced by environmental factors, and vigorous physical activity is one of the most influential factor.18,19
6) The school environment is considered the most suitable setting for carrying out physical activity interventions on children because of: it is possible targeting to large segments of the youth population, students spend a considerable amount of day in school, most of schools provide health education (physical activity and nutritional habits) and, finally, the school environment provides a powerful social network of teacher and peers.22
7) The design of the interventions should be based on theoretical models of behavior change. A main limitation for most of obesity interventions in children is that the lack of theoretical underpinning on behavioral change models threats the perdurability over time of the effect.
References
1. Lobstein T, Baur L et al. Obesity in children and young people: a crisis in public health. Obes Rev 2004; 5 (Suppl 1): 4-104. [ Links ]
2. Martínez-Vizcaíno V, Solera Martínez M, Notario Pacheco B, Sánchez López M, García-Prieto JC, Torrijos Niño C, et al. Trends in excess of weight, underweight and adiposity among Spanish children from 2004 to 2010: the Cuenca Study. Public Health Nutr 2012; 15 (12): 2170-4. [ Links ]
3. Álvarez Caro F, Díaz Martín JJ, Riano Galán I, Pérez Solis D, Venta Obaya R, Málaga Guerrero S. Classic and emergent cardiovascular risk factors in schoolchildren in Asturias. An Pediatr (Barc) 2011; 74 (6): 388-95. [ Links ]
4. Olds T, Maher C, Zumin S, Peneau S, Lioret S, Castetbon K, et al. Evidence that the prevalence of childhood overweight is plateauing: data from nine countries. Int J Pediatr Obes 2011; 6 (5-6): 342-60. [ Links ]
5. Rokholm B, Baker JL, Sorensen TI. The levelling off of the obesity epidemic since the year 1999-a review of evidence and perspectives. Obes Rev 2010; 11 (12): 835-46. [ Links ]
6. Martínez-Vizcaíno V et al. Trends in excess weight and thinness among Spanish schoolchildren in the period 1992-2004: the Cuenca study. Public Health Nutr 2009; 12: 1015-8. [ Links ]
7. Kolle E, et al. Secular trends in adiposity in Norwegian 9-year-olds from 1999-2000 to 2005. BMC Public Health 2009; 9: 389. [ Links ]
8. Beyerlein A, von Kries R, Ness AR, Ong KK. Genetic Markers of Obesity Risk: Stronger Associations with Body Composition in Overweight Compared to Normal-Weight Children. PLoS One 2011; 6 (4): el9057. [ Links ]
9. Moreno LA, et al. Childhood obesity: etiology-synthesis part II. En: Springer, ed. Epidemiology of obesity in children and adolescents. Prevalence and etiology. London; 2011. [ Links ]
10. Lillycrop KA, Burdge GC. Epigenetic changes in early life and future risk of obesity. Int J Obes (Lond) 2011; 35 (1): 72-83. [ Links ]
11. Bleich SN, Ku R, Wang YC. Relative contribution of energy intake and energy expenditure to childhood obesity: a review of the literature and directions for future research. Int J Obes (Lond) 2011; 35 (1): 1-15. [ Links ]
12. Vicente-Rodríguez G, Rey-López JP, Martín-Matillas M, Moreno LA, Wärnberg J, Redondo C, et al. Television watching, videogames, and excess of body fat in Spanish adolescents: The AVENA study. Nutrition 2008; 24 (7-8): 654-62. [ Links ]
13. Aranceta J, Pérez Rodrigo C, Ribas L, Serra-Majem L. Sociodemographic and lifestyle determinants of food patterns in Spanish children and adolescents: the enKid study. Eur J Clin Nutr 2003; 57 (S1): S40-4. [ Links ]
14. Martínez-Vizcaíno V, Sánchez-López M, Salcedo-Aguilar F, Notario-Pacheco B, Solera-Martínez M, Moya-Martínez P et al; MOVI-2 group. Protocol of a randomized cluster trial to assess the effectiveness of the MOVI-2 program on overweight prevention in schoolchildren. Rev Esp Cardiol (Engl Ed) 2012; 65 (5): 427-33. [ Links ]
15. Yin Z, Moore JB, Johnson MH, Barbeau P, Cavnar M, Thornburg J, et al. The Medical College of Georgia Fitkid project: the relations between program attendance and changes in outcomes in year 1. Int J Obes (Lond) 2005; 29 (Suppl 2):S40-5. [ Links ]
16. Stallmann-Jorgensen IS, Gutin B, Hatfield-Laube JL, Humphries MC, Johnson MH, Barbeau P. General and visceral adiposity in black and white adolescents and their relation with reported physical activity and diet. Int J Obes (Lond) 2007; 31 (4): 622-9. [ Links ]
17. Gutin B. Diet vs exercise for the prevention of pediatric obesity: the role of exercise. Int J Obes (Lond) 2011; 35: 29-32. [ Links ]
18. Levin BE. Epigenetic influences on food intake and physical activity level: review of animal studies. Obesity (Silver Spring) 2008; 16 (Suppl 3): S51-4. [ Links ]
19. Kilpeläinen TO, Qi L, Brage S, Sharp SJ, Sonestedt E, Demerath E, et al. Physical activity attenuates the influence of FTO variants on obesity risk: a meta-analysis of 218,166 adults and 19,268 children. PLoS Med 2011; 8 (11): e1001116. [ Links ]
20. Waters E, de Silva-Sanigorski A, Hall BJ, Brown T, Campbell KJ, Gao Y, et al. Interventions for preventing obesity in children. Cochrane Database Syst Rev 2011; 12: CD001871. [ Links ]
21. Khambalia AZ, Dickinson S, Hardy LL, Gill T, Baur LA. A synthesis of existing systematic reviews and meta-analyses of school-based behavioural interventions for controlling and preventing obesity. Obes Rev 2012; 13 (3): 214-33. [ Links ]
22. Vasques C, Magalhães P, Cortinhas A, Mota P, Leitão J, Lopes VP. Effects of Intervention Programs on Child and Adolescent BMI: A Meta-Analysis Study. J Phys Act Health 2013 Jan 30. (Epub ahead of print). [ Links ]
23. Glanz K, Rimer BK, Viswanath K. Health Behavior and Health Education: Theory, Reserach, and Practice. San Francisco: Jossey, Bass; 2008. [ Links ]
24. Niederer I, Kriemler S, Zahner L, Bürgi F, Ebenegger V, Hartmann T, et al. Influence of a lifestyle intervention in preschool children on physiological and psychological parameters (Ballabeina): study design of a cluster randomized controlled trial. BMC Public Health 2009; 9: 94. [ Links ]
25. Eisenmann JC, Gentile DA, Welk GJ, Callahan R, Strickland S, Walsh M et al. SWITCH: rationale, design, and implementation of a community, school, and family-based intervention to modify behaviors related to childhood obesity. BMC Public Health 2008; 8: 223. [ Links ]
26. Sallis JF, Cervero RB, Ascher W, Henderson KA, Kraft MK, Kerr J. An ecological approach to creating active living communities. Annu Rev Public Health 2006; 27: 297-322. [ Links ]
27. Bronfenbrenner U. Ecological systems theory. Annals Child Dev 1989; 6: 187-249. [ Links ]
28. Flores R. Dance for health: improving fitness in African American and Hispanic adolescents. Public Health Rep 1995; 110: 189-93. [ Links ]
29. Robinson TN. Reducing children's television viewing to prevent obesity: A randomised controlled trial. JAMA 1999; 282: 1561-7. [ Links ]
30. Salmon J, Ball K, Hume C, Booth M, Crawford D. Outcomes of a group-randomized trial to prevent excess weight gain, reduce screen behaviours and promote physical activity in 10-year-old children: switch-play. Int J Obes (Lond) 2008; 32: 601-12. [ Links ]
31. Donnelly JE, Greene JL, Gibson CA, Smith BK, Washburn RA, Sullivan DK et al. Physical Activity Across the Curriculum (PAAC): a randomized controlled trial to promote physical activity and diminish overweight and obesity in elementary school children. Prev Med 2009; 49: 336-41. [ Links ]
32. Kriemler S, Zahner L, Schindler C, Meyer U, Hartmann T, Hebestreit H et al. Effect of school based physical activity programme (KISS) on fitness and adiposity in primary schoolchildren: cluster randomised controlled trial. BMJ 2010; 340: c785 [ Links ]
33. Gortmaker SL, Peterson K, Wiecha J, Sobal AM, Dixit S, Fox MK et al. Reducing obesity via a school-based interdisciplinary intervention among youth. Arch Pediat Adol Med 1999; 153: 409-18. [ Links ]
34. Müller MJ, Asbeck I, Mast M, Lagnaese L, Grund A. Prevention of Obesity-more than an intention. Concept and first results of the Kiel Obesity Prevention Study (KOPS). Int J Obes (Lond) 2001; 25 (Suppl 1): S66-74. [ Links ]
35. Kain J, Uauy R, Albala, Vio F, Cerda R, Leyton B. Schoolbased obesity prevention in Chilean primary school children: methodology and evaluation of a controlled study. Int J Obes (Lond) 2004; 28: 483-93. [ Links ]
36. Coleman KJ, Tiller CL, Sánchez J, Heath EM, Sy O, Milliken G, et al. Prevention of the epidemic increase in child risk of overweight in low-income schools. Arch Pediat Adol Med 2005; 159: 217-24. [ Links ]
37. Yin Z, Gutin B, Johnson MH, Hanes Jr. J, Moore JB, Cavnar M et al. An environmental approach to obesity prevention in children: Medical College of Georgia FitKid Project year 1 results. Obes Res 2005; 13: 2153-61. [ Links ]
38. Gutin B, Yin Z, Johnson M, Barbeau P. Preliminary findings of the effect of a 3-year after-school physical activity intervention on fitness and body fat: the Medical College of Georgia Fitkid Project. Int J Pediatr Obes 2008; 3: 3-9. [ Links ]
39. Martínez Vizcaíno V, Salcedo Aguilar F, Franquelo Gutiérrez R, Solera Martínez M, Sánchez López M, Serrano Martínez S et al. Assessment of an after-school physical activity program to prevent obesity among 9- to 10-year-old children: a cluster randomized trial. Int J Obes (Lond) 2008; 32 (1): 12-22. [ Links ]
40. Salcedo Aguilar F, Martínez-Vizcaíno V, Sánchez López M, Solera Martínez M, Franquelo Gutiérrez R, Serrano Martínez S, et al. Impact of an after-school physical activity program on obesity in children. J Pediatr 2010; 157 (1): 36-42 e3. [ Links ]
41. Marcus C, Nyberg G, Nordenfelt A, Karpmyr M, Kowalski J, Ekelund U. A 4-year, cluster-randomized, controlled childhood obesity prevention study: STOPP. Int J Obes (Lond) 2009; 33: 408-17. [ Links ]
42. Whitaker RC et al. Early adiposity rebound and the risk of adult obesity. Pediatrics 1998; 101 (3): E5. [ Links ]
![]() Correspondence:
Correspondence:
Vicente Martínez Vizcaíno
Centro de Estudios Sociosanitarios
Universidad de Castilla-La Mancha
Santa Teresa Jornet, s/n
16071 Cuenca
E-mail: Vicente.Martinez@uclm.es