Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Nutrición Hospitalaria
versión On-line ISSN 1699-5198versión impresa ISSN 0212-1611
Nutr. Hosp. vol.29 no.3 Madrid mar. 2014
https://dx.doi.org/10.3305/NH.2014.29.3.7150
ORIGINAL / Nutrición enteral
A safe "cut, tie and thread-pull" method for percutaneous endoscopic gastrostomy tube removal in children with congenital craniofacial anomalies and pharyngeal stenosis
Un método seguro para "cortar, atar y tirar del hilo" para retirada de sonda mediante gastrostomía endoscópica percutánea en niños con anomalías craneofaciales y estenosis faríngea congénitas
Adam Hermanowicz1, Ewa Matuszczak1, Katarzyna Kondej-Muszynska2, Marta Komarowska1, Wojciech Debek1 and Stanislaw Klek3
1Pediatric Surgery Department. Medical University of Bialystok. Poland
2Pediatric Gastroenterology Department. Medical University of Bialystok. Poland
3General and Oncology Surgery Unit. Stanley Dudrick Memorial Hospital. Skawina. Poland
ABSTRACT
Percutaneous endoscopic gastrostomy (PEG) is a widely used method for tube feeding with enteral nutrition. Both PEG´s insertion and PEG´s removal are usually easy and uncomplicated. The latter can be, however, of substantial difficulty in children with distorted anatomy, such as pharyngeal stenosis or endured craniofacial trauma, when regular endoscopy is contraindicated. The aim of the study was to assess the very simple, but rarely used method for percutaneous removal of the tube by pulling the thread. Four children (4 males, mean age 4.1 year) were analyzed. In all of them the procedure was successful, quick and uncomplicated. To conclude, the thread method should be recommend in case the endoscopic removal is impossible.
Key words: PEG. Pull technique. Craniofacial anomalies.
RESUMEN
La gastrostomía endoscópica percutánea (GEP) es un método muy utilizado para alimentación por sonda con nutrición enteral. Habitualmente tanto la inserción como la retirada de la sonda mediante GEP es fácil y sin complicaciones. Sin embargo, la segunda puede ser sustancialmente difícil en niños con una anatomía alterada como la estenosis faríngea o que haya sufrido un traumatismo craneofacial, en donde la endoscopia rutinaria está contraindicada. El propósito de este estudio fue evaluar un método muy sencillo pero rara vez usado como es la retirada percutánea de la sonda con el hilo. Se analizaron 4 niños (4 varones, edad media 4,1 años). En todos ellos el procedimiento fue exitoso, rápido y sin complicaciones. Para concluir, el método del hilo debería recomendarse en el caso de que la retirada endoscópica no sea posible.
Palabras clave: GEP. Técnica de tirar. Anomalías craneofaciales.
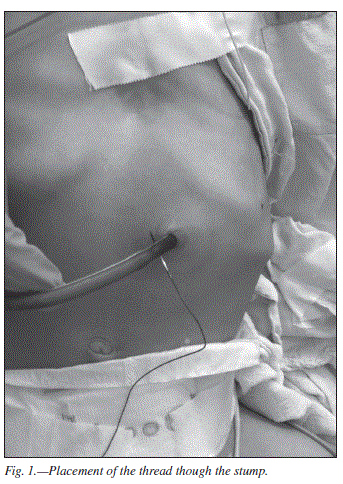
Introduction Percutaneous endoscopic gastrostomy (PEG) is a widely used method for insertion of a gastrostomy tube in patients who are unable to swallow and who require the administration of enteral nutrition.1 The procedure is safe, the incidence of complications related to PEG and further enteral nutrition is low, while the surgical gastrostomy is usually associated with a higher rate of complications.1,2 The PEG´s removal represent rarely discussed procedure as it poses no difficulties in most of patients. It can be, however, of substantial difficulty in children with distorted anatomy, such as pharyngeal stenosis or endured craniofacial trauma, when regular endoscopy is contraindicated. In those patients, the surgical procedure under general anesthesia is usually required, which increases the risk and number of possible complications. It would be useful to develop a new method, less invasive and safer. The aim of the study was to assess the very simple, but rarely used method, which was the percutaneous removal with the thread. Method Four children (4 males, mean age 4.1 year) were analyzed. The indication was the tube blockage and unsuccessful provision of nutrients. The underlying diseases were as follow: Pierre-Robin syndrome in one, malformation syndrome in three of them. PEG removal´s necessity was due to the inability to infuse feeding solution through the tube-blockage (n = 2) and peritubular leakage (n = 2). In one patient in addition to aforementioned symptoms inability to push in and rotate the tube was noticed - the buried bumper syndrome was diagnosed. Mean time before tube removal was 8 months (range 5-21 months). PEG devices were 10 Ch to 16 Ch. In all cases it was impossible to insert a regular endoscope with a channel for the loop, it was only possible to insert an infant tool with a probe channel. Mean number of preceding endoscopic attempts was 2/child. Informed consent was obtained in all patients. The method was approved by a local ethical committee. The PEG removal procedure was performed under general anesthesia. The prophylactic antibiotic shot was administered. At first the cutting needle was passed through the external end of the PEG tube, and the integrity of the tube was checked with a traction. The PEG tube was cut approximately 2,5 cm above skin level, and a needle was passed 1 cm over the skin through the PEG tube and tied afterwards (figs. 1, 2). The distal end of the thick, nonabsorbable suture was inserted into the stomach along with the shortened PEG stump (fig. 3). The thread was then grabbed with an endoscopic forceps inside the stomach after lubrication with gel (fig. 4). The thread and the endoscope was brought out through the mouth. The surgeon was able to remove shortened PEG stump orally by pulling the thread (figs. 5, 6). In one case PEG stump was blocked in the proximal pharynx, and Magill´s forceps were used to extract it. Results In all of four patients the procedure was successful. There were not any postoperative complications. Mean duration of the procedure was 6.6 minutes (range: 4.5-11.2 min.) After the removal, the enteral feeding via nasogastric tube was performed for 4-5 weeks and another PEG was reinserted subsequently. Discussion Several methods of PEG removal are described in the literature, e.g. the "cut-and-push" technique for PEG removal was described in 1991. The "cut-and-push" technique is cutting the tube at the skin level and allowing the tube and internal flange to pass spon-taneously.9 This technique is used in patients who are thought to have no risk of distal adhesions or strictures - so patients with previous abdominal surgery should be excluded for this type of PEG removal.9,10 Still the remnant can become blocked in the bowel, and result in perforation and even a death of the patient.9,10,11 The PEG flange may be retrieved endoscopically but this may become technically challenging in children with pharyngeal stenosis, for example with Pierre-Robin Syndrome, with innate craniofacial anomalies, gothic palate or acquired pharyngeal stenosis e.g. after trauma, as was the case in our patients. External traction causes tissue disruption, the patients do not tolerate the procedure well, and retrieval of the PEG is often unsuccessful. The grasp with endoscopic forceps is often not so assured and the cut PEG fragment can be blocked in the esophagus. In case the infusion of feeding solution via the tube due to its blockage and peritubular leakage, there are indications for the PEG removal. When aforementioned symptoms are accompanied by the inability to push in and out and to rotate the tube and abdominal pain - buried bumper syndrome should be considered.5 Klein et al first described the latter in 1990.12 Usually patient is referred for emergency endoscopy or surgical removal of the bumper. In some cases removing the PEG tube is achievable by external traction, without an abdominal incision, especially in cases in whom retrieval-type PEG tubes have been used.13 The only migrated bumper we had was removed using an open surgical technique (minilaparotomy) after the endoscopic attempt of the retrieval failed, and a new tube was placed. Although some authors advocate leaving the internal bumper in situ as a relatively safe treatment option,14 it is in our opinion risky, because it may result in serious complications including gastrointestinal bleeding, perforation of the stomach, peritonitis and death.15 To conclude, it should be emphasized that the cut, tie and pull method is safe and quick and not technically challenging in children with congenital or acquired pharyngeal stenosis. It can reduce the mean time of the PEG tube removal and moreover can be performed by a single endoscopist. Statement of authorship All authors state that they have made substantial contributions to the study and that they give their approval to the final version of the manuscript. Acknowledgements Adam Hermanowicz was a main researcher and the coordinator of the study. He was responsible for the conception and contributed to the experimental design, data interpretation and writing of the manuscript. All authors contributed to the data collection and writing of the manuscript. Stanislaw Klek critically revised the intellectual content of the study and contributed to its creation. References 1. Vanis N, Saray A, Gornjakovic S, Mesihovic R. Percutaneous endoscopic gastrostomy (PEG): retrospective analysis of a 7-year clinical experience. Acta Inform Med 2012; 20: 235-7. [ Links ] 2. Grant JP. Comparison of percutaneous endoscopic gastrostomy with Stamm gastrostomy. Ann Surg 1988; 207: 598-603. [ Links ] 3. Gauderer MW, Ponsky JL, Izant RJ Jr. Gastrotomy without laparotomy: a percutaneous endoscopic technique. J Pediatr Surg 1980; 15: 872-5. [ Links ] 4. Disario J. Endoscopic approaches to enteral nutritional support. Best Pract Res Clin Gastroenterol 2006; 20: 605-30. [ Links ] 5. Erdil A, Genc H, Uygun A, Ilica AT, Dagalp K. The buried bumper syndrome: the usefulness of retrieval PEG tubes in its management. Turk J Gastroenterol 2008; 19: 45-8. [ Links ] 6. Vu CK. Buried bumper syndrome: old problem, new tricks. J Gastroenterol Hepatol 2002; 17: 1125-8. [ Links ] 7. Gencosmanoglu R, Koc D, Tozun N. The buried bumper syndrome: migration of internal bumper of percutaneous endoscopic gastrostomy tube into the abdominal wall. J Gastroenterol 2003; 38: 1077-80. [ Links ] 8. Ma MM, Semlacher EA, Fedorak RN, et al. The buried gastrostomy bumper syndrome: prevention and endoscopic approaches to removal. Gastrointest Endosc 1995; 41: 505-8. [ Links ] 9. Peacock O, Singh R, Cole A, Speake W: The "cut and push" technique: is it really safe? BMJ Case Rep 2012; 27: doi:10.1136/ bcr-2012-006607 [ Links ] 10. Harrison E, Dillon J, Leslie FC. Complications of the cut-and-push technique for percutaneous endoscopic gastrostomy tube removal. Nutr Clin Pract 2011; 26: 230-1. [ Links ] 11. Agha A, AlSaudi D, Furnari M, Abdulhadi Ali MM, Morched Chakik R, Alsaudi I, Savarino V, Giannini EG. Feasibility of the cut-and-push method for removing large-caliber soft percutaneous endoscopic gastrostomy devices. Nutr Clin Pract 2013; 28: 490-2. [ Links ] 12. Klein S, Heare BR, Soloway RD. The "buried bumper syndrome": a complication of percutaneous endoscopic gastrostomy. Am J Gastroenterol 1990; 5: 448-51. [ Links ] 13. Erkan G, Coban M, Kaan Atac G, Caliskan A, Degertekin B. The advantage of retrieval PEG tubes in patients with buried bumper syndrome - A case report. Turk J Gastroenterol 2012; 23: 773-5. [ Links ] 14. Kejariwal D, Aravinthan A, Bromley D, Miao Y. Buried bumper syndrome: cut and leave it alone! Nutr Clin Pract 2008; 23: 322-4. [ Links ] 15. Anagnostopoulos GK, Kostopoulos P, Arvanitidis DM. Buried bumper syndrome with a fatal outcome, presenting early as gastrointestinal bleeding after percutaneous endoscopic gastrostomy placement. J Postgrad Med 2003; 49: 325-7. [ Links ] Recibido: 17-XI-2013 ![]() Correspondence:
Correspondence:
Stanislaw Klek
Assoc. Prof. Stanley Dudrick´s Memorial Hospital
General and Oncology Surgery Unit
32-050 Skawina, 15 Tyniecka Street, Poland
E-mail: klek@poczta.onet.pl
Aceptado: 1-XII-2013