My SciELO
Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO -
 Access statistics
Access statistics
Related links
-
 Cited by Google
Cited by Google -
 Similars in
SciELO
Similars in
SciELO -
 Similars in Google
Similars in Google
Share
Nutrición Hospitalaria
On-line version ISSN 1699-5198Print version ISSN 0212-1611
Nutr. Hosp. vol.33 n.6 Madrid Nov./Dec. 2016
https://dx.doi.org/10.20960/nh.770
TRABAJO ORIGINAL / Paciente crítico
Phase Angle and Onodera's Prognostic Nutritional Index in critically ill patients
Ángulo de fase e índice de Onodera en pacientes críticamente enfermos
Karina Marques Vermeulen1, Leilane Lilian Araújo Leal1, Mariana Câmara Martins Bezerra Furtado2, Sancha Helena de Lima Vale3 and Lúcia Leite Lais3
1Multidisciplinary Residency Training Program and 2Section of Nutrition. Onofre Lopes University Hospital. Federal University of Rio Grande do Norte. Natal, Brazil.
3Department of Nutrition. Federal University of Rio Grande do Norte. Natal, Brazil
ABSTRACT
Introduction: Assessing severity and nutritional prognosis in critical patients has become increasingly important in recent years, since these parameters are related to morbidity/mortality and used to guide therapeutic options.
Objective: Determine nutritional prognosis through the Phase Angle (PA) and Onodera's Prognostic Nutritional Index (OPNI) and its relationship with severity, hospitalization time and mortality of critically ill patients.
Methods: Descriptive cross-sectional study, involving adult patients hospitalized in an Intensive Care Unit (ICU). Data were collected from the patients' medical records to calculate severity indicators (APACHE II, SOFA and SAPS 3) and determine the length of hospitalization and outcome. Bioimpedance was conducted to calculate the PA, using resistance and reactance data.
Results: A total of 35 patients (26% men and 74% women), with mean age of 55.5 ± 16.7 years, were included. The mortality rate (17%) was similar to that expected by APACHE II and SOFA, but higher than that predicted by SAPS 3. The mean values for the PA (4.2 ± 1.0) and OPNI (38.7 ± 8.3) were lower than the reference values adopted. Individuals with PA < 5.1 exhibited significantly lower reactance and albumin and higher APACHE II and SOFA values, in addition to longer hospitalization time and higher mortality. The PA was inversely correlated with all the severity indicators under study (APACHE II, SOFA and SAPS 3), and the length of hospitalization. By contrast, there was no correlation between OPNI and these parameters, or between PA and OPNI.
Conclusion: The PA proved to be a good tool in assessing nutritional prognosis in critically ill patients. By contrast, more studies using the OPNI with this type of patients are needed.
Key words: Intensive care. Critical illness. Nutrition. Prognosis.
RESUMEN
Introducción: en los últimos años se ha valorado la evaluación de la gravedad y del pronóstico nutricional en pacientes críticos, por ser parámetros relacionados a la morbimortalidad y porteadores de conductas terapéuticas.
Objetivo: verificar el pronóstico nutricional mediante el Ángulo de Fase (AF) y el Índice de Pronóstico Nutricional de Onodera (OPNI) y su relación con la gravedad, con el tiempo de internación y con la mortalidad de pacientes críticos.
Métodos: estudio transversal descriptivo, incluyendo pacientes adultos, internados en Unidad de Terapia Intensiva (UTI). Fueron recabados datos en la historia clínica de los pacientes para cálculo de los indicadores de gravedad (APACHE II, SOFA y SAPS 3), y verificación del tiempo de internación y desenlace. Fue realizada la bioimpedancia para cálculo del AF, mediante datos de resistencia y reactancia.
Resultados: se incluyeron 35 pacientes, con edad promedio de 55,5 ± 16,7 años, siendo 26% del sexo masculino y 74% del femenino. La tasa de mortalidad encontrada en el estudio (17%) fue semejante a aquella esperada por los indicadores de gravedad APACHE II y SOFA, pero superior a aquella esperada por el SAPS 3. Los valores promedios encontrados para el AF (4,2 ± 1,0) y el OPNI (38,7 ± 8,3) fueron inferiores a los valores de referencia adoptados. Aquellos con AF < 5,1 presentaron significativamente menores valores de reactancia y albumina, mayores valores del APACHE II y del SOFA, y tuvieron mayor tiempo de internación y mortalidad. El AF se correlacionó inversamente con todos los indicadores de gravedad, pero lo contrario fue observado con el OPNI, no habiendo correlación entre estos dos indicadores de pronóstico nutricional.
Conclusión: el AF es una herramienta confiable para evaluación del pronóstico nutricional en pacientes críticos. Por el contrario, se necesitan más estudios utilizando el OPNI con este tipo de pacientes.
Palabras clave: Cuidados intensivos. Enfermedad crítica. Nutrición. Pronóstico.
Introduction
The Intensive Care Unit (ICU) is an area reserved for critically ill patients that require continuous specialized attention, and the specific materials and technologies needed for diagnosis, monitoring and treatment (1). Critically ill patients generally suffer from catabolic stress resulting from a pre-existing systemic inflammatory state, correlated with higher morbidity, mortality, multiple organ dysfunction, use of mechanical ventilation and prolonged hospitalization (2).
Recent years have seen an attempt to improve the classification of these patients as to severity, since this knowledge helps to determine criteria for patient admission, treatment and discharge, in addition to enabling assessment of the costs and benefits of the ICU (3). Among the tools used to classify severity are Acute Physiology and Chronic Health Evaluation II (APACHE II), Sequential Organ Failure Assessment (SOFA) and Simplified Acute Physiology Score 3 (SAPS 3). These indicators estimate severity and the risk of morbidity and mortality, with high values directly related to worse outcome (4).
In critically ill patients, the metabolic response to stress promotes intense protein catabolism to repair damaged tissue and supply energy, compromising immunological response, interfering in organ function, changing body composition, and making nutritional depletion a frequent condition. In this respect, nutritional status is also a factor capable of directly influencing a patient's prognosis, morbidity and mortality (5).
Assessment of nutritional status in critically ill patients is hindered by interference from the acute disease and the therapeutic measures applied, which changes body composition and affects result interpretation (6). In this regard, establishing an early nutritional prognosis is important to monitor the nutritional progress of the patient and identify patients at risk of complications who may benefit from a specific nutritional intervention (7). Moreover, poor nutritional prognosis is associated with greater likelihood of morbidity and mortality (6). Among the nutritional prognosis methods are the Phase Angle (PA) and Onodera's Prognostic Nutritional Index (OPNI).
The PA, calculated from measures of resistance (R) and reactance (Xc) collected during bioimpedance (BIA), is used as an indicator of body cell mass (8). Low PA values are associated with morbidity and mortality in critically ill patients (9). OPNI, in turn, originally developed to predict prognosis in surgical patients, is a simple tool using measures of serum albumin and total lymphocyte Count (TLC) that can be rapidly applied in a large number of patients (10).
Accordingly, the present study aimed to determine nutritional prognosis using the PA and OPNI and its relationship with severity, length of hospitalization and mortality of critical patients.
Methodology
This cross-sectional descriptive study was reviewed and approved by the Research Ethics Committee of the Onofre Lopes University Hospital (HUOL) (CAAE: 40580114.1.0000.5292). All participants or legal guardians provided written, informed consent before enrollment.
The convenience sample consisted of patients of both sexes, aged 21 years or older and hospitalized at HUOL, in Natal, Brazil, between March and November, 2015. Patients with less than 24 hours in the ICU and those not indicated for BIA (pregnant women, amputees and pacemaker users) were excluded.
Sociodemographic (sex and age), clinical (diagnosis, routes of feeding and biochemical examinations), length of hospitalization and outcome data were collected. Patients were classified as to clinical or surgery profile according to the reason for hospitalization. All patients were monitored from admission to the ICU until discharge or death, with length of hospitalization considered both in the ICU and the hospital. The parameters under study were collected in the first 24 hours' stay in the ICU.
The APACHE II (11), SOFA (12) and SAPS 3 (13) indicators were used to analyze patient severity. The data required to make the respective calculations were collected from patients' medical records and the results were classified according to the literature (11-13). Patients with sepsis were identified according to the third international consensus for sepsis (Sepsis-3) (14).
To obtain the PA, BIA was applied using a Quantum II® analyzer (RJL Systems, Clinton Township, MI, USA), promoting the passage of a safe and painless low-frequency, current (50 kHz, 800 microA), following the method described by Lukaski et al. (15). Next, the PA was calculated by the formula: PA = arc-tangent (Xc/R) x 180/π. PA cutoff point of 5.1 was adopted in accordance with the literature (16). OPNI was calculated from the formula (17) where OPNI is equal to 10 x Albumin (g/100 mL) + 0.005 x TLC (mm³), with a reference value ≤ 40 (18).
For statistical analysis, the variables were initially analyzed using Microsoft Office Excel 2011® and later by GraphPad Prism 6.0a (Stata Corp., College Station, TX, USA, 2012). Statistical analysis was based on data distribution on a Gaussian curve, using the Shapiro-Wilk test. The quantitative variables of normal distribution were expressed as means and standard deviations. Those with non-normal distribution were presented as median, with interquartile range. The difference between groups with PA < 5.1 and PA ≥ 5.1 was assessed using the unpaired t-test and Mann-Whitney test for variables with and without normal distribution, respectively. Furthermore, the variables were correlated applying Pearson's and Spearman's correlations for those with and without normal distribution, respectively. The significance level was set at p < 0.05.
Results
A total of 35 patients, 26% men and 74% women, mean age of 55.5 ± 16.7 years, were included in the study. Most of the patients had undergone surgery (60%) and fasted in the first 24 hours (54%). With respect to nutritional prognosis indices, mean PA and OPNI were below the cutoff point. The general characteristics are shown in table I.
Analysis of the patients in relation to PA showed that those with PA < 5.1 exhibited significantly lower reactance and albumin and higher APACHE II and SOFA values (Table I). Moreover, the group with low PA exhibited longer ICU stays and greater mortality rates.
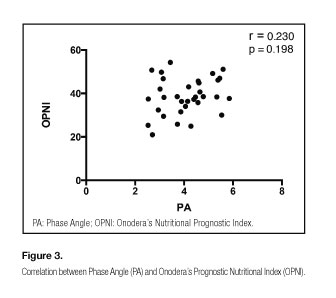
The PA was inversely correlated with all the severity indicators under study (APACHE II, SOFA and SAPS 3) (Fig. 1), length of stay in the ICU and the hospital (Fig. 2). By contrast, there was no correlation between OPNI and these parameters (Figs. 1 and 2), or between PA and OPNI (Fig. 3). In addition, sepsis was observed in 46% of patients (Table I) and there was no difference in PA and OPNI means between patients with or without sepsis (Fig. 4). The correlation between prognosis indices and severity indicators studied were not influenced by sepsis condition (Tables II and III).
Discussion
In the population under study, there was a wide range of diagnoses, divided into clinical and surgical, with a higher prevalence of surgical patients. In relation to the route of feeding, most of the patients (54%) fasted for the first 24 hours, followed by either an oral diet (37%) or enteral nutrition (9%) (Table I). According to recommendations, feeding should be initiated within 24 to 48 hours, if the digestive tube is viable and the patient is hemodynamically stable (19-21). This early feeding contributes to reducing the risk of complications and length of hospital stay, in addition to improving the patient's clinical prognosis (20-22). Thus, the patients under study were within the acceptable range, without exceeding the recommended fasting time.
Severity indicators quantify acute and chronic physiological changes during admission, estimating mortality in order to correct errors and improve ICU performance (23). High values are proportionally associated with greater risk of morbidity, mortality and length of hospitalization (4,16). The mean values found for APACHE II, SOFA and SAPS 3 in the present study, when classified according to the literature (11-13), indicated an expected mortality rate of 15%, 18.6% and < 10%, respectively. The mortality observed in our study was 17% (Table I), similar to values expected by APACHE II and SOFA. However, the ICU mortality rate can vary between 25 and 30% (24) or be even higher, depending on the characteristics of each sector (25). The large number of elective surgeries in the unit studied prevented a higher mortality rate (26). This finding corroborated the study by Mayr et al. (2006) (27), where the mortality rate in 3700 critically ill patients was low (9.5%), because nearly half of them had undergone elective cardiac surgery with good prognosis.
Identifying prognosis indices for critically ill patients is important in the clinical management of their disease. Among these, the PA assesses prognosis based on cell membrane integrity, and can be used under different clinical conditions (28-30). In our study population, the mean PA was lower than the cutoff point (PA = 5.1) adopted for healthy patients (16) (Table I).
The PA has been used as an indicator of nutritional status and survival predictor for a number of diseases, such as acquired immunodeficiency syndrome, as well as oncological, nephropathic and septic disorders (4,16,28). It may also be positively associated with a number of serious diseases, suggesting it is an important instrument in assessing the muscularity, nutritional prognosis and clinical outcome of critically ill patients (4,31-33).
Some studies have found lower PA values among the females (4,16) as expected, since PA increases according to the amount of muscle mass and body cell mass (34). However, in our study, no difference was found in PA between males (4.3 ± 1.0) and females (4.1 ± 1.1), (p = 0.659) (data not shown).
In the present study, there was a strong correlation between PA and severity indicators (Fig. 2), in line with literature findings (15), which also demonstrated an association between low PA and mortality. Furthermore, other studies (4,28,29) suggest that low PA values in critically ill patients are related to decreased cell integrity, decline in lean mass, poor prognosis and higher mortality.
Silva et al. (16) (2015) found prevalence of sepsis in 47% of patients and observed a significant negative correlation between PA and APACHE II (r = -0.506; p < 0.001) just in patients without sepsis. In our study, sepsis was observed in 46% of patients, according to the clinical criteria (Singer et al., 2016). However there was no difference in PA (p = 0.179) and OPNI (p = 0.272) means between patients with or without sepsis (p = 0.179) (Fig. 4), demonstrating that the presence or absence of sepsis did not influence the correlation between prognosis indices and severity indicators studied (Tables II and III).
As expected, no significant correlation was found between PA and SOFA in patients with or without sepsis because SOFA is part of clinical criteria to identify patients with sepsis (14). Also, there was no correlation between OPNI and the severity indicators, independent of sepsis condition (Table III). Thus, our results demonstrate that PA is a useful prognostic indicator in critically ill patients with or without sepsis. Nevertheless, the same cannot be assured with the OPNI.
When differences in severity indicators were compared between groups with lower and higher PA (Table I), a significant difference was found between APACHE II and SOFA, with higher severity values for patients with lower PA, indicating poor nutritional prognosis. Interestingly, SAPS 3 values were not significantly different between the groups, perhaps due to the small sample size.
In this study, the length of stay in the ICU and the hospital was significantly different between the groups with higher and lower PA (Table I). Moreover, PA was negatively correlated with length of ICU and hospital stay (Fig. 2). Kyle et al. (2013) (35) also found a significant association between low PA values and longer hospital stays, and mortality.
The mean OPNI found in the study was lower than the reference value (18), but not correlated with severity indicators (Fig. 1) or length of ICU and hospital stay (Fig. 2). This finding can be explained by the fact that this index considers biological levels of albumin and TLC in its calculation. TLC measures momentary immunological reserves, associated with undernourished individuals. However, it is important to underscore that in critically ill patients this parameter can be changed by clinical status or the use of medication. Thus, OPNI seems to be better employed in patients receiving peritoneal dialysis, and those with terminal liver disease and active tuberculosis (10).
Despite the limitation of albumin as an indicator of nutritional status, a number of studies (6,26) have correlated its decline with the increased incidence of clinical complications, morbidity and mortality. In the present study, the patients with a lower PA exhibited lower serum albumin (Table I). Lima and Silva et al. (2015) (26) also obtained low PA in critically ill patients with hypoalbuminemia.
The prognosis indices under study did not correlate between each other (Fig. 3). Although both assessed nutritional prognosis, they are based on completely different parameters and were developed for different groups of patients. While the PA uses tissue resistance to an electric current, OPNI uses biochemical levels that may be altered in a critically ill patient.
Among the limitations found in the study are the small sample size, primarily in patients with PA > 5.1, and the lack of studies applying OPNI in critically ill patients.
Conclusion
The mean PA of the study population was lower than the reference value adopted and was inversely correlated with severity indicators and length of stay in the ICU and the hospital. Thus, the PA was shown to be a good tool in assessing nutritional prognosis in critically ill patients, identifying patients at risk of complications who could benefit from a more specific nutritional therapy. The mean OPNI found was also lower than the cutoff point, but not correlated with the other variables, showing the need for more studies, involving patients with different clinical profiles, including those in critical illness.
References
1. Oliveira NS, Caruso L, Bergamaschi DP, Cartolano FC, Soriano FG. Impacto da adequação da oferta energética sobre a mortalidade em pacientes de UTI recebendo nutrição enteral. Rev Bras Ter Intensiva 2011;23(2):183-9. [ Links ]
2. Ribeiro LMK, Filho RSO, Caruso L, Lima PA, Damasceno NRT, Soriano FG. Adequação dos balanços energético e proteico na nutrição por via enteral em terapia intensiva: quais são os fatores limitantes? Rev Bras Ter Intensiva 2014;26(2):155-62. [ Links ]
3. Tranquitelli AM, Padilha KG. Sistemas de classificação de pacientes como instrumentos de gestão em Unidades de Terapia Intensiva. Rev Esc Enferm USP 2007;4(1):141-6. [ Links ]
4. Berbigier MC, Pasinato VF, Rubin BA, Moraes RB, Perry ID. Bioelectrical impedance phase angle in septic patients admitted to intensive care units. Rev Bras Ter Intensiva 2013;25(1):25-31. [ Links ]
5. Lucas MCS, Fayh APT. Estado nutricional, hiperglicemia, nutrição precoce e mortalidade de pacientes internados em uma unidade de terapia intensiva. Rev Bras Ter Intensiva 2012;24(2):157-61. [ Links ]
6. Maicá AO, Schweigert ID. Avaliação nutricional em pacientes graves. Rev Bras Ter Intensiva 2008;20(3):286-95. [ Links ]
7. Freitas BJSA, Mesquita LC, Teive NJV, Souza SR. Antropometria Clássica e Músculo Adutor do Polegar na Determinação do Prognóstico Nutricional em Pacientes Oncológicos. Rev Bras de Cancerologia 2010;5(4):415-42. [ Links ]
8. Oliveira CMC, Kubrusly M, Mota RS, Silva CAB, Oliveira VN. A Desnutrição na insuficiência renal crônica: qual o melhor método diagnóstico na prática clínica? J Bras Nefrol 2010;32(1):57-70. [ Links ]
9. Gunn SN, Halbert JA, Giles LC, Stepien JM, Miller MD, Crotty M. Bioelectrical phase angle values in a clinical sample of ambulatory rehabilitation patients. Dynamic Medicine 2008;7(14). [ Links ]
10. Kang SH, Cho KH, Park JW, Yoon KW, Do JY. Onodera's Prognostic Nutritional Index as a Risk Factor for Mortality in Peritoneal Dialysis Patients. J Korean Med Sci 2012;27(11):1354-8. [ Links ]
11. Knaus WA, Draper EA, Wagner DP, Zimmerman JE. APACHE II: a severity of disease classification system. Crit Care Med 1985;13(10):818-29. [ Links ]
12. Moreno R, Vincent JL, Matos R, Mendonça A, Cantraine F, Thijs L, et al. The use of maximum SOFA score to quantify organ dysfunction/failure in intensive care. Results of a prospective, multicentre study. Intensive Care Med 1999;25:686-96. [ Links ]
13. Moreno RP, Metnitz PGH. Almeida E, Jordan B, Bauer P, Abizanda R, et al. SAPS 3-From evaluation of the patient to evaluation of the intensive care unit. Part 2: Development of a prognostic model for hospital mortality at ICU admission. Intensive Care Med 2005;31(10):1345-55. [ Links ]
14. Singer M, Deutschman CS, Seymour CW, Shankar-Hari M, Annane D, Bauer M, et al. The Third International Consensus Definitions for Sepsis and Septic Shock (Sepsis-3). JAMA 2016;315(8):801-10. [ Links ]
15. Lukaski HC, Bolonchuk WW, Hall CB, Siders WA. Validation of tetrapolar bioelectrical impedance method to assess human body composition. J Appl Physiol 1986;60:1327-32. [ Links ]
16. da Silva TK, Berbigier MC, Rubin BA, Moraes RB, Corrêa Souza G, Schweigert Perry ID. Phase Angle as a Prognostic Marker in Patients With Critical Illness. Nutr Clin Pract 2015;30(2):261-5. [ Links ]
17. Onodera T, Goseki N, Kosaki G. Prognostic nutritional index in gastrointestinal surgery of malnourished cancer patients. Nihon Geka Gakkai Zasshi 1984;85(9):100-5. [ Links ]
18. Nozoe T, Ninomiya M, Maeda T, Matsukuma A, Nakashima H, Ezaki T. Prognostic Nutritional Index: A tool to predict the biological aggressiveness of gastric carcinoma. Surg Today 2010;40:440-3. [ Links ]
19. Associação de Medicina Intensiva Brasileira; Sociedade Brasileira de Infectologia; Sociedade Brasileira de Nutrição Parenteral e Enteral. Diretrizes da Saúde suplementar. Sepse e Nutrição; 2009. [ Links ]
20. Kreymann KG, Bergerb MM, Deutzc NEP, Hiesmayrd M, Jolliete P, Kazandjievf G, et al. ESPEN Guidelines on Enteral Nutrition: Intensive care. Clin Nutr 2006;25(2):210-23. [ Links ]
21. McClave AS, Martindale RG, Vanek VW, McCarthy M, Roberts P, Taylor B, et al. Guidelines for the Provision and Assessment of Nutrition Support Therapy in the Adult Critically Ill Patient: Society of Critical Care Medicine (SCCM) and American Society for Parenteral and Enteral Nutrition (A.S.P.E.N.). JPEN J Parenter Enteral Nutr 2009;33(3):277-316. [ Links ]
22. Pasinato VF, Berbigier MC, Rubin BA, Castro K, Moraes RB, Dalira I, et al. Terapia nutricional enteral em pacientes sépticos na unidade de terapia intensiva: adequação às diretrizes nutricionais para pacientes críticos. Rev Bras Ter Intensiva 2013;25(1):17-24. [ Links ]
23. Silva Junior JM, Malbouisson LMS, Nuevo HL, Barbosa LGT, Marubayashi LY, Teixeira IC, et al. Aplicabilidade do Escore Fisiológico Agudo Simplificado (SAPS 3) em Hospitais Brasileiros. Rev Bras Anestesiol 2010;60(1):20-31. [ Links ]
24. Bastos PG, Sun X, Wagner DP, Wu AW, Knaus WA. Glasgow Coma Scale score in the evaluation of outcome in the intensive care unit: findings from the Acute Physiology and Chronic Health Evaluation III study. Crit Care Med 1993;21(10):1459-65. [ Links ]
25. Freitas ERSF. Perfil e gravidade dos pacientes das unidades de terapia intensiva: aplicação prospectiva do escore APACHE II. Rev Latino-Am Enfermagem 2010;18(3):7. [ Links ]
26. Lima e Silva RR, Pinho CPS, Rodrigues IG, Monteiro Júnior JGM. Ángulo de fase como indicador del estado nutricional y pronóstico em pacientes críticos. Nutr Hosp 2015;31(3):1278-85. [ Links ]
27. Mayr VD Dünser MW, Greil V, Jochberger S, Luckner G, Ulmer H, et al. Causes of death and determinants of outcome in critically ill patients. Crit Care 2006;10(6):R154. [ Links ]
28. Silva LM, Caruso L, Martini LA. Aplicação do ângulo de fase em situações clínicas. Rev Bras Nutr Clin 2007;22(4):317-21. [ Links ]
29. Norman K, Stobäus N, Pirlich M, Bosy-Westphal A. Bioelectrical phase angle and impedance vector analysis--clinical relevance and applicability of impedance parameters. Clin Nutr 2012;31(6):854-61. [ Links ]
30. Selberg O, Selberg D. Norms and correlates of bioimpedance phase angle in healthy human subjects, hospitalized patients, and patients with liver cirrhosis. Eur J Appl Physiol 2002;86(6):509-16. [ Links ]
31. Azevedo ZMA, Silva DR, Dutra MVP, Elsas MICG, Barbosa-Silva MCG, Fonseca VM. Associação entre ângulo de fase, PRISM I e gravidade da sepse. Rev Bras Ter Intensiva 2007;19(3):297-303. [ Links ]
32. Lee Y, Kwon O, Shin CS, Lee SM. Use of bioelectrical impedance analysis for the assessment of nutritional status in critically ill patients. Clin Nutr Res 2015;4(1):32-40. [ Links ]
33. Kuchnia A, Earthman C, Teigen L, Cole A, Mourtzakis M, Paris M, et al. Evaluation of Bioelectrical Impedance Analysis in Critically Ill Patients: Results of a Multicenter Prospective Study. JPEN J Parenter Enteral Nutr 2016 May 24. pii: 0148607116651063. (Epub ahead of print). [ Links ]
34. Barbosa-Silva MCG, Barros AJD, Wang J, Heymsfield SB, Pierson RN. Bioelectrical impedance analysis: population reference values for phase angle by age and sex. Am J Clin Nutr 2005;82(1):49-52. [ Links ]
35. Kyle UG, Genton L, Pichard C. Low phase angle determined by bioelectrical impedance analysis is associated with malnutrition and nutritional risk at hospital admission. Clin Nutr 2013;32(2):294-9. [ Links ]
![]() Correspondence:
Correspondence:
Lúcia Leite Lais.
Departamento de Nutrição.
Campus Universitario.
Lagoa Nova, 59078-900.
Natal-RN, Brasil
e-mail: ludl10@hotmail.com
Received: 19/02/2016
Accepted: 07/07/2016