My SciELO
Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO -
 Access statistics
Access statistics
Related links
-
 Cited by Google
Cited by Google -
 Similars in
SciELO
Similars in
SciELO -
 Similars in Google
Similars in Google
Share
Nutrición Hospitalaria
On-line version ISSN 1699-5198Print version ISSN 0212-1611
Nutr. Hosp. vol.33 suppl.3 Madrid 2016
https://dx.doi.org/10.20960/nh.312
The association between water intake, body composition and cardiometabolic factors among children - The Cuenca study
Marta Milla-Tobarra1,2, Antonio García-Hermoso3, Noelia Lahoz-García2, Blanca Notario-Pacheco2, Lidia Lucas-de la Cruz2, Diana P. Pozuelo-Carrascosa2, María José García-Meseguer4 and Vicente Martínez-Vizcaíno2,5
1Hospital Nuestra Señora del Prado. Talavera de la Reina, Toledo. Spain.
2Health and Social Research Center. Universidad de Castilla-La Mancha. Cuenca, Spain.
3Sports, Physical Activity and Health Science Laboratory. Medical Sciences Faculty. Universidad de Santiago de Chile. Santiago, Chile.
4Faculty of Nursing. Campus de Albacete. Universidad de Castilla-La Mancha. Albacete, Spain.
5Health Sciences Faculty. Universidad Autónoma de Chile. Talca, Chile
ABSTRACT
Introduction: Beverage consumption and its possible association with current obesity epidemic and metabolic syndrome is under investigation in recent years, however water intake is probably the most underestimated of all beverages and could play an important role.
Objective: The aim of this study was to examine the association between water intake, body composition and cardiometabolic factors in a sample of Spanish children.
Methods: A cross-sectional study was conducted in 366 schoolchildren (53.5% girls) aged 9-11 years from the province of Cuenca in Spain. Data of anthropometrics, body composition, cardiometabolic risk factors and cardiorespiratory fitness variables were collected. Beverage consumption was assessed using two non-consecutive 24 h dietary recalls.
Results: We found an inverse association between the consumption of water (ml)/kg per weight with BMI, body fat, fat-free mass, waist circumference, insulin levels, HOMA-IR (p < 0.001), and with arterial pressure parameters, systolic (p < 0.010) and diastolic blood pressure (p < 0.028), and mean arterial pressure (p < 0.012), as well as direct associations with HDL cholesterol (p < 0.001). In ANCOVA analyses, children who drank less water (ml)/kg per weight, had higher levels of LDL cholesterol (p < 0.050) and lower levels of HDL cholesterol (p < 0.042), and overweight-obesity subjects drank less water (ml)/kg per weight than normal peers (p < 0.011). Besides, children with lower levels of HDL cholesterol and higher levels of triglycerides and blood pressure had less water intake as a beverage. Finally, children who drank less water from beverages had high levels of LDL cholesterol.
Conclusions: Higher consumption of water (ml)/kg per weight was negatively associated with BMI, body fat, fat-free mass, waist circumference, insulin levels, HOMA-IR, and positively with HDL cholesterol in children independently of age, sex and cardiorespiratory fitness. In addition, overweight-obese children drank less water (ml)/kg per weight than normoweight ones. Therefore, water consumption is associated with numerous health benefits and its adequate intake could contribute to prevent obesity and metabolic syndrome in childhood.
Key words: Water consumption. Serum lipids. Insulin resistance. Body composition.
Introduction
The majority of the main risk factors associated with cardiovascular disease are preventable and modifiable by lifestyle changes (1). Evidence has shown that overweight, eating behaviors and physical activity affect most cardiometabolic variables associated with cardiovascular risk factors, such as serum lipids, blood pressure, waist circumference and insulin resistance (2).
Regarding these modifiable factors, beverage consumption and their possible association with the current obesity epidemic and metabolic syndrome is under investigation in recent years (3). Most studies have focused on sugar sweetened beverages consumption (4-7), although there are also studies that analyzed diet beverages (8,9). On the other hand, there are studies focused on dairy consumption and its possible positive association with cardiovascular health (10,11), as well as on natural juices intake (12). Preliminary analysis of a recent study has shown that a Healthy Beverage Index, a measure of the overall healthfulness of an individual's beverage intake, was associated with reduced cardiometabolic risk in adults (13). Other authors provide additional evidence suggesting a potential protective effect of higher total water intake (particularly plain water) on kidney but not on cardiovascular risk (14).
With regard to these hydration habits, one question generally forgotten has been water consumption (15). Regulation of water balance is essential for the maintenance of health and life, and some authors have attempted to elucidate its possible link with obesity (16). Drinking more water has been proposed as a method to reduced weight gain since water consumption could replace other caloric beverages and thereby reduce total calories consumed (16). However, evidence about water intake and its association with cardiovascular health is scarce (17), and in most studies, they are related to water hardness (18). To our knowledge, there is no research focused on children regarding this topic. Therefore, the aim of this study was to examine the association between water intake, body composition and cardiometabolic factors in a sample of Spanish children.
Material and methods
STUDY DESIGN AND PARTICIPANTS
This study was a cross-sectional analysis of baseline measurement data from a cluster-randomized trial aimed to assess the effectiveness of a physical activity program for preventing excess weight in schoolchildren (19). For this report, we used data from a sub-sample of 366 children (196 girls) aged 9 to 11 years, in fifth grade of Primary Education from 20 public primary schools in the Spanish province of Cuenca. The Clinical Research Ethics Committee of the Virgen de la Luz Hospital, in Cuenca, approved the study protocol.
ANTHROPOMETRIC AND BODY COMPOSITION ASSESSMENTS
All measurements were obtained at the schools by trained nurses. Height and weight were measured twice with a five-minute interval between measurements with the children lightly dressed. Weight was measured to the nearest 0.1 kg using a calibrated digital scale (SECA Model 861; Vogel & Halke, Hamburg, Germany). Height was measured to the nearest millimeter using a wall-mounted stadiometer, with the children standing straight against the wall without shoes, to align the spine with the stadiometer. The head was positioned so that the chin was parallel to the floor. The mean of the two weight and height measurements was used to calculate body mass rndex (BMI) as weight in kilograms divided by the square of the body height in meters (kg/m2). Waist circumference (WC) was calculated as the average of two measurements taken with flexible tape at the natural waist (the midpoint between the last rib and the iliac crest). Body fat percentage and fat-free mass percentage were estimated using a BC-418 bioimpedance analysis system (Tanita Corp., Tokyo, Japan). The mean of two readings taken in the morning under controlled temperature and humidity conditions, after urination and a 15-minute rest, with the child being shoeless and fasting was used.
RESTING BLOOD PRESSURE MEASUREMENT
Diastolic and systolic blood pressure (DBP; SBP) were determined as the average of two measurements separated by a five-minute interval, with the child resting for at least five minutes before the first measurement. The child was seated in a quiet, calm environment, with the right arm in a semi-flexed position at the heart level. Blood pressure was measured automatically using the OMRON M5-I monitor (Omron Healthcare Europe BV, Hoofddorp, Netherlands). Mean arterial pressure (MAP) was calculated using the following formula: DBP + (0.333 × [SBP - DBP]).
BIOCHEMICAL ASSESSMENTS
Blood samples were taken in standardized conditions between 8:15 and 9:00 a.m. after at least 12 hours fasting by puncturing the cubital vein. Before the extraction, fasting was confirmed by the child and his parents. The samples were processed using a Roche Diagnostics COBAS C711. The following parameters were determined: triglycerides (GPO-PAP enzymatic method), HDL-cholesterol and LDL-cholesterol (2nd generation method without de-proteinization).
The homeostasis model of assessment (HOMA-IR) was used to determine insulin resistance (IR) and its individual components. Fasting glucose and insulin were determined using standard protocols (chemiluminescent microparticle immunoassay).
CARDIORESPIRATOTY FITNESS
Cardiorespiratory fitness was assessed by the 20-m shuttle run test (20). Participants were required to run between two lines 20 m apart, while keeping pace with audio signals emitted from a pre-recorded compact disc. The running speed started at 8.5 km/h and increased 0.5 km/h each minute. The children were stopped when they could not follow the signal any more. We noted the last half-stage completed as an indicator of their cardiorespiratory fitness (CRF).
ASSESSMENT OF WATER AND OTHER BEVERAGE INTAKES
Beverage and water intake of each participant were estimated using a self-administered computerized 24 h dietary recall validated for European adolescents called the Young Adolescents' Nutrition Assessment on Computer (YANA-C) (21). The Spanish YANA-C questionnaire was administered twice in a week: one day asking about a weekday and another one about a weekend day. The YANA-C program was installed in the computer room of each school, where pupils completed the questionnaire in groups. A staff member instructed the children and, then, pupils completed the program autonomously, although two or three staff members were present to provide assistance as required. Interviewers were previously trained.
STATISTICAL ANALYSIS
The distribution of continuous variables was checked for normality before the analysis. Due to their skewed distribution, variables were log-transformed prior to analyses. Continuous variables were expressed as the mean ± SD for normally distributed continuous data. Categorical variables we expressed as n (%). To aid interpretation, data were back-transformed from the log scale for presentation in the results.
Normal weight and overweight-obese were defined according to the BMI cut-offs published for children and adolescents (22).
Categorization of blood pressure (BP) was done using sex, age and height specific cut points informed by the Fourth Report on the Diagnosis, Evaluation and Treatment of High Blood Pressure in Children and Adolescents by the National High Blood Pressure Education Program Working Group on High Blood Pressure in Children and Adolescents (23). High BP (stage 1) was defined as a systolic or diastolic BP at 95th percentile or higher but lower than the 99th percentile; high BP (stage 2) was defined as a systolic or diastolic BP at 99th percentile or higher; and borderline BP was defined as a systolic or diastolic BP at the 90th percentile or higher but lower than the 95th percentile. To obtain more accurate results we simplified the four criteria obtained in two categories, as follows, normotensive (p < 90) and hypertension (stages 1 and 2) (p ≥ 90).
Adverse lipid concentrations were defined as follows: total cholesterol concentrations ≥ 200 mg/dl or higher; HDL < 40 mg/dl; LDL concentrations ≥ 130 mg/dl; and triglycerides concentrations ≥ 130 mg/dl (24). Insulin resistance was defined as follows: fasting glucose concentrations ≥ 126 mg/dl (25); insulin concentrations > 15.05 µU/ml (25); and HOMA-IR > 3.43 (26).
Multiple linear regression analyses were made to explore possible relationships between water intake, body composition and cardiometabolic factors adjusted by age, sex, and cardiorespiratory fitness. ANCOVA models were estimated to test the differences in water intake variables by categories of BMI (normoweight vs overweight-obese children) and cardiometabolic risk (non-risk vs at risk children).
Results
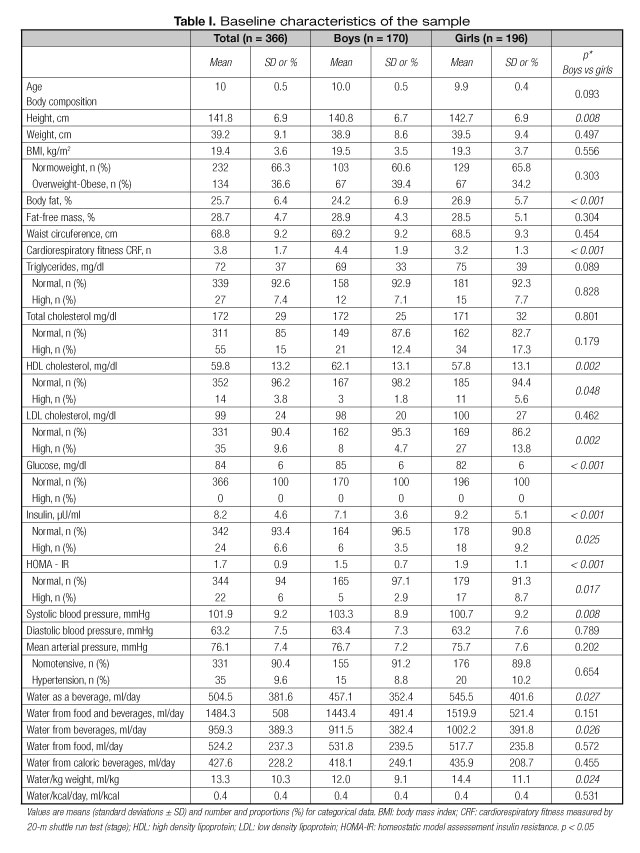
The sample characteristics are presented in table I. There were statistically significant gender differences in the mean of height (higher in girls, p = 0.008), body fat percentage (higher in girls, p < 0.001), and CRF (higher in boys (p < 0.001), but not for BMI. The prevalence of overweight-obesity was 36.6% for the total sample. Regarding cardiometabolic factors, boys had higher levels of HDL cholesterol (p = 0.002), fasting plasma glucose (p < 0.001) and SBP (p = 0.008) than girls. Girls had higher insulin levels (p < 0.001) and HOMA-IR (p < 0.001) than boys. Concerning lipids parameters, 7.4% of children had higher levels of triglycerides, 15% total cholesterol elevated, 3.8% HDL cholesterol low, and 9.6% had adverse LDL cholesterol. All children had normal amounts of fasting plasma glucose (≥ 126 mg/dl). Finally, we found a 9.6% of children with hypertension. Concerning water intake, for most of water variables, except for water from food variable, girls took more quantities than boys, although the differences were non-significant.
Table II shows the ANCOVA analysis. We found that children who drank fewer water as a beverage had higher values of triglycerides (p = 0.009), worst levels of HDL cholesterol (p < 0.001) and hypertension (p = 0.023). On the other hand, children who drank less water from all beverages had adverse levels of LDL cholesterol (p = 0.022). Moreover, those who ingested less water (ml)/kg per weight, had lower levels of HDL cholesterol (p = 0.042) and higher levels of LDL cholesterol (p = 0.050). Finally, overweight-obese children drank less water (ml)/kg per weight than normal peers did (p = 0.011) and had more consumption of water/kcal day (p = 0.023).
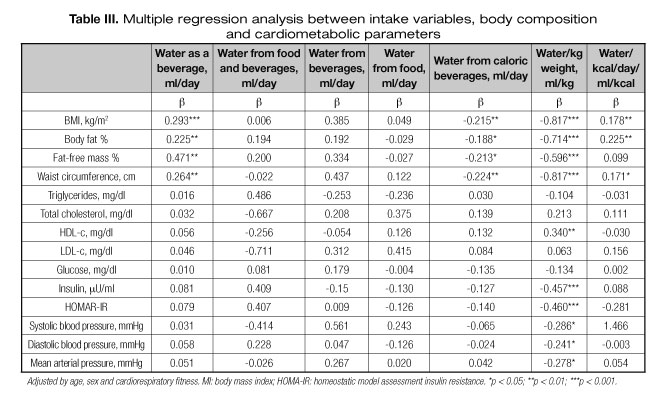
Table III presents the relationship between water intake variables, BMI and cardiometabolic risk factors adjusted by age, sex and cardiorespiratory fitness. We found a positive association between water as a beverage with BMI (p < 0.001), body fat (p < 0.004), fat free mass (p < 0.001) and waist circumference (p < 0.001). A positive association also appears between water/kcal day and BMI (p = 0.009), body fat (p < 0.001) and waist circumference (p = 0.011). On the other hand, there was a negative association between water from caloric beverages with BMI (p = 0.005), body fat (p = 0.010), fat free mass (p = 0.010) and waist circumference (p = 0.003). Regarding water (ml)/kg per weight, we showed an inverse relationship with BMI, body fat, fat free mass, waist circumference, insulin levels, HOMA-IR (p < 0.001), and arterial pressure parameters (SBP, p = 0.010; DBP, p = 0.028; and mean arterial pressure, p = 0.012). Finally, we found direct associations between water (ml)/kg per weight and HDL cholesterol (p = 0.001).
Discussion
The aim of the study was to examine the association between water intake, body composition and cardiometabolic risk factors in a sample of Spanish children. Overall, our results showed an inverse association between water (ml)/kg per weight and several body composition variables, lipid profile and insulin resistance parameters, independently of age, sex and cardiorespiratory fitness.
Water consumption is probably the most underestimated of all beverages intakes (15). Water is essential for life and plain water, instead of other caloric beverages, is one approached for decreasing energy intake (27), and therefore may play an important role to fight against obesity and metabolic syndrome. However, the mechanism remains unclear. Some studies have suggested that water intake elicited acute changes in human physiology because it provides a sympathetic stimulus, increasing the metabolic rate, which in turn augments the daily energy expenditure (28,29). Other authors reported that water drinking activates the autonomic nervous system and induces acute hemodynamic changes (30). The actual stimulus for these effects is undetermined but might be related to either gastric distension or osmotic factors (30). In our sample, water (ml)/kg per weight was inversely associated with BMI, body fat, fat free mass and waist circumference, as well as, overweight-obesity children drank less water(ml)/kg per weight than normal weight peers.
Healthy eating is one of the keys for obesity prevention (31) and knowledge of the energy contribution from beverages is particularly important, since consumption of healthy fluids is part of a balanced diet (32). Drinking plain water instead of caloric beverages may reduce dietary energy density and help in body weight management (33). Among children, several surveys have checked that promotion and provision of drinking water could effectively reduce the risk of overweight (34) and that an increase of water intake has been associated as well with weight loss in overweight children (35). However, in adults, some review studies showed that whereas encouraging water consumption may facilitate weight management, the evidence was very limited (16,36,37). Moreover, we found an inverse relationship between water from caloric beverages (sugar sweetened beverages, dairy consumption and fruit juices) with BMI, body fat, fat free mass, and waist circumference. This is controversial because most reviews link sugar sweetened beverages consumption with greater risk of obesity and metabolic syndrome (6,38). In this sense, it is important to say that, in our study, water from all types of liquids that provide calories, including dairy products and fruit juices, were the drinks most consumed by our children (39), which could justify our results, as some authors present a possible positive relationship with body composition and cardiovascular health (12,40).
Otherwise, there is little evidence about beverage consumption and its association with blood lipids. We observed that children who drank less plain water had higher blood triglycerides values and lower HDL cholesterol values. Consistent with this, children who drank less water (ml)/kg per weight had lower HDL cholesterol levels and higher LDL cholesterol levels. Finally, we have shown a direct association between HDL cholesterol values and water(ml)/kg per weight. These two categories refer to plain water intake and plain water intake per kg of weight. In this sense, a review reports that drinking water results in greater rates of fat oxidation because fat oxidation is maximal when blood insulin levels are low (41). The reason for this is that insulin inhibits or decreases the ability of rate limiting enzymes that breakdown triglyceride fats into free fatty acids (41). Since water does not contain calories or carbohydrates like other beverages, it does not trigger an insulin response (41). Moreover, one study in women showed that drinking one liter or more water per day was associated with decreases in triglycerides, total cholesterol and LDL cholesterol over 12 months (42).
Besides, we have observed an inverse relationship between water (ml)/kg per weight and fasting insulin and HOMA-IR. There is limited evidence regarding this issue. Some authors had drawn attention to a low water intake as a possible new risk factor for impaired glycemia, suggesting that an increase in water intake (an easy and costless intervention) could prevent or delay the onset of hyperglycemia and subsequent diabetes (43). In addition, the same study in women reported that a higher consumption of water per day was associated with significant decreases in fasting insulin and HOMA-IR (42).
Lastly, information about the relationship between blood pressure and water intake is scarce. There is some evidence for the relationship between drinking water content of magnesium and calcium and the risk for cardiovascular disease, because these captions regulate muscular contractility, and a lack of magnesium leads to an increase in vascular tension and a lower muscular contraction threshold (18). A recent case-control study in children and adolescents has shown that the magnesium and calcium levels content of drinking water may have a protective role against early stages of atherosclerosis (44). In adults, a randomized controlled trial reported an improvement in SBP replacing caloric beverages with non-caloric alternatives as water (45). In addition, another study showed a significant decrease in blood pressure in women that drunk one liter or more of water per day (42). Our findings showed a negative association between the consumption of water (ml)/kg per weight and SBP, DBP and mean arterial pressure, and in accordance with this, children who drank less plain water had more prevalence of hypertension (p ≥ 90) (23). We could speculate that water content in minerals could be the reason of these relationships; however, we have not quantified the amount of sodium and potassium content in our drinking water.
This study is not without limitations. First, our study was a cross-sectional design, thus observational findings do not allow us to evaluate whether water intake has a possible causal relationship with body composition and cardiometabolic factors over time. Additionally, we have found little evidence between these associations, and most of them are in adults, although, in general, the physiological differences between children and adolescents compared to adults are related to water content in the body, insensible water loss, sweating and index of renal function in the case of children aged less than two years. In spite of physiological differences, thermoregulatory capacity of children and adolescents is comparable to that of adults (46). Moreover, the assessment of diet in children, either directly or by adult proxy, has some methodological challenges. It has been suggested that 10-year-old children are not able to give valid responses to food frequency questionnaires covering periods longer than one day. In our study, the use of pictures in the YANA-C software helped children to remember not only the food eaten during the last 24 hours, but also the portion size. Finally, we have not been able to quantify the mineral content in children's water intake, so results cannot be easily compared to some literature reports.
Conclusions
In conclusion, our data show an inverse association between water (ml)/kg per weight and BMI, body fat, fat free mass, waist circumference, fasting insulin, HOMA-IR, and blood pressure parameters in children. We observed as well that children who drink less plain water and less quantity of plain water/kg per weight had higher levels of triglycerides and LDL cholesterol, and lower values of HDL cholesterol. Finally, overweight-obese children's intake of plain water/kg per weight is lower than that of normal counterparts. Hopefully, our study could serve as a benchmark to design appropriate randomized clinical trials testing the efficacy of water intake, instead of other beverages, to prevent obesity and cardiometabolic diseases in children.
References
1. Weintraub WS, Daniels SR, Burke LE, Franklin BA, Goff DC, Hayman LL, et al. Value of primordial and primary prevention for cardiovascular disease: A policy statement from the American Heart Association. Circulation 2011;124(8):967-90. [ Links ]
2. Daubenmier JJ, Weidner G, Sumner MD, Mendell N, Merritt-Worden T, Studley J, et al. The contribution of changes in diet, exercise, and stress management to changes in coronary risk in women and men in the multisite cardiac lifestyle intervention program. Ann Behav Med 2007;33(1):57-68. [ Links ]
3. Duffey KJ, Gordon-Larsen P, Steffen LM, Jacobs DR, Popkin BM. Drinking caloric beverages increases the risk of adverse cardiometabolic outcomes in the Coronary Artery Risk Development in Young Adults (CARDIA) Study. Am J Clin Nutr 2010;92(4):954-9. [ Links ]
4. Chan TF, Lin WT, Huang HL, Lee CY, Wu PW, Chiu YW, et al. Consumption of sugar-sweetened beverages is associated with components of the metabolic syndrome in adolescents. Nutrients 2014;6(5):2088-103. [ Links ]
5. Barrio-López MT, Martínez-González MA, Fernández-Montero A, Beunza JJ, Zazpe I, Bes-Rastrollo M. Prospective study of changes in sugar-sweetened beverage consumption and the incidence of the metabolic syndrome and its components: The SUN cohort. Br J Nutr 2013;110(9):1722-31. [ Links ]
6. Richelsen B. Sugar-sweetened beverages and cardio-metabolic disease risks. Curr Opin Clin Nutr Metab Care 2013;16(4):478-84. [ Links ]
7. Xi B, Huang Y, Reilly KH, Li S, Zheng R, Barrio-López MT, et al. Sugar-sweetened beverages and risk of hypertension and CVD: A dose-response meta-analysis. Br J Nutr 2015;113(5):709-17. [ Links ]
8. Nettleton JA, Lutsey PL, Wang YF, Lima JA, Michos ED, Jacob DR. Diet soda intake and risk of incident metabolic syndrome and type 2 diabetes in the Multi-Ethnic Study of Atherosclerosis (MESA). Diabetes Care 2009;32(4):688-94. [ Links ]
9. Gardener H, Rundek T, Markert M, Wright CB, Elkind MS, Sacco RL. Diet soft drink consumption is associated with an increased risk of vascular events in the Northern Manhattan Study. J Gen Intern Med 2012;27(9):1120-6. [ Links ]
10. Bel-Serrat S, Mouratidou T, Jiménez-Pavon D, Huybrechts I, Cuenca-García M, Mistura L, et al. Is dairy consumption associated with low cardiovascular disease risk in European adolescents? Results from the HELENA Study. Pediatr Obes 2014;9(5):401-10. [ Links ]
11. Crichton GE, Bryan J, Buckley J, Murphy KJ. Dairy consumption and metabolic syndrome: A systematic review of findings and methodological issues. Obes Rev 2011;12(5):e190-201. [ Links ]
12. Ruxton CH, Gardner EJ, Walker D. Can pure fruit and vegetable juices protect against cancer and cardiovascular disease too? A review of the evidence. Int J Food Sci Nutr 2006;57(3-4):249-72. [ Links ]
13. Duffey KJ, Davy BM. The healthy beverage index is associated with reduced cardiometabolic risk in US adults: A preliminary analysis. J Acad Nutr Diet 2015;115(10):1682-9.e2. [ Links ]
14. Sontrop JM, Dixon SN, Garg AX, Buendía-Jiménez I, Dohein O, Huang S-HS, et al. Association between water intake, chronic kidney disease, and cardiovascular disease: A cross-sectional analysis of NHANES data. Am J Nephrol 2013;37(5):434-42. [ Links ]
15. Popkin BM, D'Anci KE, Rosenberg IH. Water, hydration, and health. Nutrition Reviews 2010;68(8). [ Links ]
16. Daniels MC, Popkin BM. Impact of water intake on energy intake and weight status: A systematic review. Nutr Rev 2010;68(9):505-21. [ Links ]
17. Chan J, Knutsen SF, Blix GG, Lee JW, Fraser GE. Water, other fluids, and fatal coronary heart disease: The Adventist Health Study. Am J Epidemiol 2002;155(9):827-33. [ Links ]
18. Rylander R. Drinking water constituents and disease. J Nutr 2008;138(2):423S-5S. [ Links ]
19. Martínez-Vizcaíno V, Sánchez-López M, Salcedo-Aguilar F, Notario-Pacheco B, Solera-Martínez M, Moya-Martínez P, et al. Protocol of a randomized cluster trial to assess the effectiveness of the MOVI-2 program on overweight prevention in schoolchildren. Rev Esp Cardiol (Engl Ed.) 2012;65(5):427-33. [ Links ]
20. Leger LA, Mercier D, Gadoury C, Lambert J. The multistage 20 metre shuttle run test for aerobic fitness. J Sports Sci 1988;6(2):93-101. [ Links ]
21. Vereecken CA, Covents M, Sichert-Hellert W, Alvira JMF, Le Donne C, De Henauw S, et al. Development and evaluation of a self-administered computerized 24-h dietary recall method for adolescents in Europe. Int J Obes 2008;32(Suppl. 5):S26-34. [ Links ]
22. Cole TJ, Flegal KM, Nicholls D, Jackson AA. Body mass index cut offs to define thinness in children and adolescents: International survey. Br Med J 2007;335(7612):194-7. [ Links ]
23. National High Blood Pressure Education Program Working Group on High Blood Pressure in Children. The fourth report on the diagnosis, evaluation, and treatment of high blood pressure in children and adolescents. Pediatrics 2004;114(2 Suppl. 4th report):555-76. [ Links ]
24. Expert Panel on Integrated Guidelines for Cardiovascular Health and Risk Reduction in Children and Adolescents. National Heart, Lung, and Blood Institute. Expert panel on integrated guidelines for cardiovascular health and risk reduction in children and adolescents: Summary report. Pediatrics 2011;128(Suppl 5):S213-56. [ Links ]
25. Classification and diagnosis of diabetes mellitus and other categories of glucose intolerance. National Diabetes Data Group. Diabetes 1979;28(12):1039-57. [ Links ]
26. Cuartero BG, Lacalle CG, Lobo CJ, Vergaz AG, Rey CC, Villar MA, et al. Índice HOMA y QUICKI, insulina y péptido C en niños sanos. Puntos de corte de riesgo cardiovascular. An de Pediatr2007;66(5):481-90. [ Links ]
27. Lee H-S, Park S, Kim M-H. Factors associated with low water intake among South Korean adolescents-Korea National Health and Nutrition Examination Survey, 2007-2010. Nutr Res Pract 2014;8(1):74-80. [ Links ]
28. Vij VA, Joshi AS. Effect of "water induced thermogenesis" on body weight, body mass index and body composition of overweight subjects. J Clin Diag Res 2013;7(9):1894-6. [ Links ]
29. Boschmann M, Steiniger J, Franke G, Birkenfeld AL, Luft FC, Jordan J. Water drinking induces thermogenesis through osmosensitive mechanisms. J Clin Endocrinol Metab 2007;92(8):3334-7. [ Links ]
30. Brown CM, Barberini L, Dulloo AG, Montani JP. Cardiovascular responses to water drinking: Does osmolality play a role? Am J Physiol Regul Integr Comp Physiol 2005;289(6):R1687-92. [ Links ]
31. Hesketh K, Waters E, Green J, Salmon L, Williams J. Healthy eating, activity and obesity prevention: A qualitative study of parent and child perceptions in Australia. Health Promot Int 2005;20(1):19-26. [ Links ]
32. Benelam B, Wyness L. Hydration and health: A review. Nutr Bull 2010;35(1):3-25. [ Links ]
33. Drewnowski A, Rehm C, Constant F. Water and beverage consumption among children age 4-13y in the United States: Analyses of 2005-2010 NHANES data. Nutr J 2013;12:85. [ Links ]
34. Muckelbauer R, Libuda L, Clausen K, Toschke AM, Reinehr T, Kersting M. Promotion and provision of drinking water in schools for overweight prevention: Randomized, controlled cluster trial. Pediatrics 2009;123(4): e661-7. [ Links ]
35. Dubnov-Raz G, Constantini NW, Yariv H, Nice S, Shapira N. Influence of water drinking on resting energy expenditure in overweight children. Int J Obes 2011;35(10):1295-300. [ Links ]
36. Dennis EA, Flack KD, Davy BM. Beverage consumption and adult weight management: A review. Eat Behav 2009;10(4):237-46. [ Links ]
37. Muckelbauer R, Sarganas G, Grüneis A, Müller-Nordhorn J. Association between water consumption and body weight outcomes: A systematic review. Am J Clin Nutr 2013;98(2):282-99. [ Links ]
38. Malik VS, Pan A, Willett WC, Hu FB. Sugar-sweetened beverages and weight gain in children and adults: A systematic review and meta-analysis. Am J Clin Nutr 2013;98:1084-102. [ Links ]
39. Tobarra MM, Martínez-Vizcaíno V, García NL, García-Prieto JC, Arias-Palencia NM, García-Hermoso A. The relationship between beverage intake and weight status in children: The Cuenca study. Nutr Hosp 2014;30(4):818-24. [ Links ]
40. Kratz M, Baars T, Guyenet S. The relationship between high-fat dairy consumption and obesity, cardiovascular, and metabolic disease. Eur J Nutr 2013;52(1):1-24. [ Links ]
41. Stookey JD. Drinking water and weight management. Nutr Today 2010; 45(6):S7-12. [ Links ]
42. Stookey J, Gardner C, Popkin B. Increased water intake reduces metabolic syndrome over 12 mo in overweight dieting women, independent of diet composition, activity and weight loss. Faseb J 2008;22:295-304. [ Links ]
43. Roussel R, Fezeu L, Bouby N, Balkau B, Lantieri O, Alhenc-Gelas F, et al. Low water intake and risk for new-onset hyperglycemia. Diabetes Care 2011;34(12):2551-4. [ Links ]
44. Poursafa P, Kelishadi R, Amin MM, Hashemi M, Amin M. First report on the association of drinking water hardness and endothelial function in children and adolescents. Arch Med Sci 2014;10(4):746-51. [ Links ]
45. Tate DF, Turner-McGrievy G, Lyons E, Stevens J, Erickson K, Polzien K, et al. Replacing caloric beverages with water or diet beverages for weight loss in adults: Main results of the Choose Healthy Options Consciously Everyday (CHOICE) randomized clinical trial. Am J Clin Nutr 2012;95(3):555-63. [ Links ]
46. Rowland T. Thermoregulation during exercise in the heat in children: Old concepts revisited. J Appl Physiol (1985) 2008;105(2):718-24. [ Links ]
![]() Correspondence:
Correspondence:
Marta Milla-Tobarra.
Hospital Nuestra Señora del Prado.
Ctra. de Madrid, km. 114.
45600 Talavera de la Reina, Toledo.
Spain
e-mail: mmillatobarra@gmail.com