Meu SciELO
Serviços Personalizados
Journal
Artigo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Acessos
Acessos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em
SciELO
Similares em
SciELO -
 Similares em Google
Similares em Google
Compartilhar
Nutrición Hospitalaria
versão On-line ISSN 1699-5198versão impressa ISSN 0212-1611
Nutr. Hosp. vol.34 no.6 Madrid Nov./Dez. 2017
https://dx.doi.org/10.20960/nh.950
The effects of a high-protein, high-calorie, fiber- and fructo-oligosaccharide-enriched enteral formula on nutritional status, bowel habits and tolerance: Safety and Effectiveness of Enteral Nutrition in elderly Spanish patients (SENS Study)
Fórmula enteral hiperproteica e hipercalórica, enriquecida en fibra y en fructooligosacáridos: efecto sobre el estado nutricional, hábitos gastrointestinales y tolerancia en pacientes ancianos españoles (Estudio SENS)
Federico Cuesta-Triana1, Francisco Villazón González2, Alejandro Sanz Paris3, Juan Ignacio Ramos-Clemente Romero4, José Enrique Palacio Abizanda5, Rebeca Sanz Barriuso6; on behalf of the SENS Working Group
1Geriatric Medicine Service. Hospital Clínico San Carlos. Madrid, Spain.
2Endocrinology Service. Hospital Universitario Central de Asturias. Oviedo, Spain.
3Endocrinology and Nutrition Service. Hospital Miguel Servet. Zaragoza, Spain.
4Internal Medicine Service. Hospital Infanta Elena. Huelva, Spain.
5Endocrinology and Nutrition Service. Hospital Universitario Nuestra Señora de Candelaria. Tenerife, Spain. 6Abbott Nutrition. Madrid, Spain
Funding: This study has been supported by Abbott Nutrition.
Conflict of interests: SPA declares that he has been supported by Abbott Nutrition in meetings and conferences. In addition, PAJE declares that he has been supported in research clinical trials by Abbott Nutrition. SBR is an employee of Abbott Nutrition. No other authors declare a conflict of interests.
ABSTRACT
Background: Enteral nutrition (EN) is an effective nutritional intervention for patients at risk of malnutrition or malnourished. However, complications such as gastrointestinal intolerance, hyperglycemia or refeeding syndrome can be triggered by EN.
Aim: To investigate the effects of a tube feeding formula (TFF) on patients' nutritional status, biochemical status, bowel habits and safety.
Methodology: Observational, prospective and multicenter study. Patients ≥ 18 years, undernourished or at nutritional risk, who were prescribed a high-calorie, high-protein, fiber-fortified TFF were included. Patients were evaluated over a period of eight weeks (baseline [V1], four weeks [V2] and eight weeks [V3]).
Results: A statistically significant increase in weight (1.5 kg), body mass index (0.6 kg/m2) and nutritional intake (59.7 kcal/day) was observed between V1 and V2. Between V1 and V3, there was a statistically significant decrease in the percentage of individuals with abnormal biochemical markers for glucose, potassium, total protein and albumin. The number of patients' bowel movements remained stable throughout the study with a mean of 1.1 daily bowel movements.
Conclusion: The TFF was safe and well tolerated, improving patients' nutritional status without altering patients' bowel habits.
Key words: Malnutrition. Enteral nutrition. Safety. Defecation. Nutritional status.
RESUMEN
Introducción: la nutrición enteral es una intervención efectiva para pacientes desnutridos o en riesgo de sufrir desnutrición. Sin embargo, puede desencadenar complicaciones como intolerancia gastrointestinal, hiperglicemia o síndrome de realimentación.
Objetivo: investigar los efectos de una fórmula de nutrición enteral por sonda en el estado nutricional y bioquímico, hábitos gastrointestinales y seguridad de los pacientes.
Metodología: estudio observacional, prospectivo y multicéntrico. Se incluyeron pacientes ≥ 18 años, desnutridos o en riesgo de desnutrición, tributarios de recibir una fórmula de nutrición enteral hipercalórica, hiperproteica, y rica en fibra y fructooligosacáridos. Los pacientes fueron evaluados durante 8 semanas en 3 visitas (V1, inicial; V2, 4 semanas; V3, 8 semanas).
Resultados: entre V1 y V2 se observó un incremento estadísticamente significativo en peso (1,5 kg), índice de masa corporal (0,6 kg/m2) e ingesta calórica (59,7 kcal/día). Entre V1 y V3, existió un descenso en el porcentaje de pacientes con valores anormales de glucosa, potasio, proteína total y albúmina. Los hábitos intestinales se mantuvieron estables durante el estudio (1,1 deposiciones diarias de media).
Conclusión: la fórmula fue segura, tolerada, y mejoró el estado nutricional del paciente sin alterar los hábitos intestinales.
Palabras clave: Desnutrición. Nutrición enteral. Seguridad. Hábitos intestinales. Estado nutricional.
INTRODUCTION
Most medical complications tend to involve a decline in nutritional status. Up to 40% of recently hospitalized patients, in particular those with chronic diseases, are at risk of malnutrition (1). Regarding institutionalized patients, 30% are malnourished and 49% are at risk of malnutrition (2). Malnutrition can lead to severe physical and psychological consequences, and delays recovery after surgery and illness; patients' tolerance of treatment and quality of life are reduced, the risk of complications and death rises, length of hospital stay increases, and healthcare costs rise accordingly (3-5). Malnutrition, among other factors, can be the cause and consequence of altered bowel habits, such as diarrhea.
Enteral feeding, alone, or as a supplement to oral feeding, is an effective method for providing nutritional support to individuals who are undernourished or who are at risk of developing malnutrition. Patients who receive enteral nutrition show less weight loss and a lower risk of mortality and complications than patients at risk of malnutrition who receive normal feeding (3), and this type of nutritional intervention is particularly effective if started early (6). Enteral nutrition (EN) has been found to be beneficial in patients with a wide range of conditions, including burns, chronic obstructive pulmonary disease, gastrointestinal surgery or liver diseases (7,8). In addition, it has been shown to be safe and cost-effective and, since its introduction, it has become an established procedure (9).
Side effects of EN may include mechanical complications (e.g., tube obstruction and perforation of the intestinal tract), infectious complications (e.g., aspiration pneumonia and infection at the tube insertion site), gastrointestinal disorders (e.g., diarrhea and constipation) and metabolic complications (e.g., hyperglycemia and refeeding syndrome) (10). Intestinal disorders are one of the most common complications of EN (11), and are reported to affect 30-60% of patients (1,11). Constipation, meanwhile, is very common in patients with reduced mobility (12), and is sometimes even more prevalent than diarrhea in patients receiving enteral feeding alone (13). These complications, aside from the immediate discomfort they cause for patients, can trigger additional problems: adequate nutrition may be limited and electrolyte imbalances may occur, generating additional costs associated with patient care. Fiber-enriched enteral formulas can help improve bowel habits, resolve constipation and reduce the incidence of diarrhea. However, the effects of fiber in nutritional supplements vary according to the different types of fiber and volumes tested (14). Moreover, fiber and fructo-oligosaccharide (FOS)-enriched enteral formulas have been shown to increase patient appetite (15), and they also have a beneficial effect on the gut microbiota (16).
The aim of this study was to evaluate patient nutritional status, effect on bowel habits and the overall safety of a high-calorie, fiber and FOS-enriched enteral formula with a high monounsaturated fatty acid content (Jevity® Plus HP) in clinical practice in Spanish patients.
METHODOLOGY
This was an observational, prospective, multicenter study conducted in the Spanish healthcare setting.
Study population
A total of 102 patients, undernourished or at nutritional risk (Nutritional Risk Scale [NRS] ≥ 3) who were prescribed enteral nutrition in the form of Jevity® Plus HP (Abbott Laboratories S.A.) in routine clinical practice, participated in this study. The duration of daily administration of enteral nutrition was 18-20 hours, gradually increasing between day 1 and day 3 according to patient tolerability.
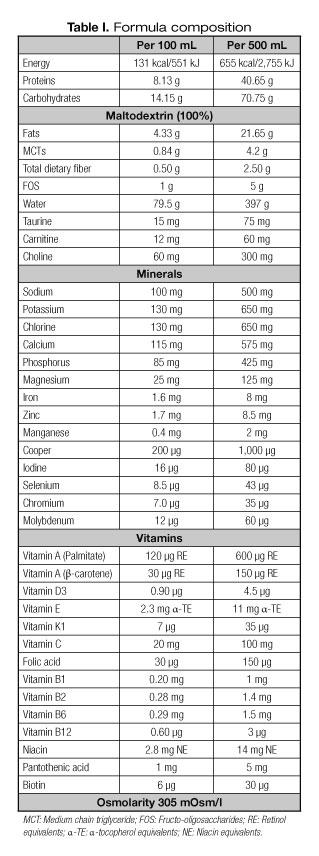
Patients were ≥ 18 years old, admitted in the study sites, who required EN administered via a nasogastric tube. Study exclusion criteria were: patients already receiving EN, and patients with a history of gastrointestinal bleeding, bowel obstruction, or changes in kidney or liver function (defined as serum creatinine > 2.5 mg/dl or serum AST at least three times above the upper limit of normal). Subjects with unstable vital signs for 48 hours or more or with known allergy to any component of Jevity® Plus HP (see composition in table I) were also excluded.
The caloric requirements were calculated per each patient with the Harris-Benedict equation adjusted for stress factor (from 1.1 to 1.3) according to medical judgment. EN was continuously supplied. The rate of infusion was progressively increased to reach the nutritional goal.
Data collection
Patients were evaluated over a period of eight weeks, during which three different visits were performed: baseline (V1), at four weeks (V2) and at eight weeks (V3).
In V1, patient demographic characteristics, informed consent forms, and clinical history were recorded, and the case report forms were provided to the nursing department, to be returned consecutively in V2 and V3. Bowel habits (number of daily bowel movements and stool type) were recorded in these case report forms. Diarrhea was defined as > 3 liquid bowel movements per day and constipation as < 3 weekly bowel movements. Vital signs, hematological parameters and use of laxatives were recorded at the three visits. A physical examination was also performed in V1 and V3.
If the investigator decided to withdraw the patient from the study before completion (eight weeks), the reasons detected during the patient's final evaluation were fully recorded.
An adverse event (AE) was defined as any worsening of a pre-existing disease or condition, whether related or not related with the treatment administered. All AEs were recorded by the physician and classified as mild (transient and easily tolerated by the patient), moderate (defined as significant discomfort affecting the patient's usual activities) or serious (incapacitating or life-threatening). Similarly, the relationship of the AE with study nutrition was classified as probable, possible, unlikely, or unrelated.
Ethical considerations
All patients or legal representatives of patients signed the informed consent form prior to beginning the study. Data of all patients were recorded without including their personal details in order to maintain patient confidentiality. This post-marketing observational study was approved by the Clinical Research Ethics Committee of the Hospital Clínico San Carlos, Madrid.
Statistical analysis
The statistical analysis was performed using the SAS® v9.3 software package. For continuous variables, mean, standard deviation (SD), median, interquartile range (IQR), minimum and maximum values were calculated. The Shapiro-Wilk test was used to determine the normal distribution of the sample. For qualitative variables, absolute or relative frequencies and 95% confidence intervals (CI) were calculated. Missing values were excluded.
Differences in quantitative variables between visits were tested by paired t-test or Wilcoxon matched pairs signed rank test. Comparisons of quantitative variables between groups were performed by t-test (or the non-parametric Wilcoxon rank sum test). In the case of qualitative variables, differences between visits were tested by the McNemar's test and differences between groups, by the Chi-squared test. In all cases, the statistical significance level was 5%.
Patient percentage with biochemical parameters between the standards was based on: glucose, 70-110 mg/dl; sodium, 135-145 mEQ/l; potassium, 3.5-5.3 mEq/l; chlorine, 96-106 mEq/l; gamma-glutamyl transferase (GGT), 6-50 U/l; total protein, 6-8.3 g/dl; albumin, 34-54 g/l and pre-albumin, 10-40 mg/dl.
RESULTS
Patient characteristics
From the total (n = 102), the more common indication for EN were cancer (29.4%), neurodegenerative diseases (22.5%) and cardiovascular events (10.8%). Among them, 43.1% were hospitalized and 56.9% were outpatients.
In total, 81.4% (n = 83) of the patients included in the study completed the eight-week follow-up. The most common causes of early withdrawal from the study (excluding missing data from the calculations) were adverse events (7.8%; n = 8), of which only one was probably due to EN, and death (4.9%; n = 5), unrelated to the intervention. At baseline, no significant differences were found in age, weight and biochemical markers levels between patients who completed the eight-week follow-up and those who were prematurely withdrawn.
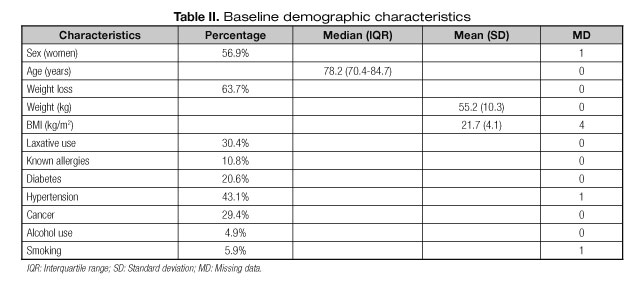
Of all the participants, 56.9% were women, and median age was 78.2 years (IQR 70.4 - 84.7). Anthropometric measurements showed the mean weight of patients at the beginning of the study was 55.2 (SD: 10.3) kg. Mean body mass index (BMI) was 21.7 (4.05) kg/m2 (Table II). At the beginning of the study, 30.4% of patients needed laxatives throughout the study. Regarding their medical history, 10.8% of patients had medication allergies, 29.4% had cancer, and up to 43.1% had arterial hypertension.
Effect of nutritional formula on the patient's nutritional status
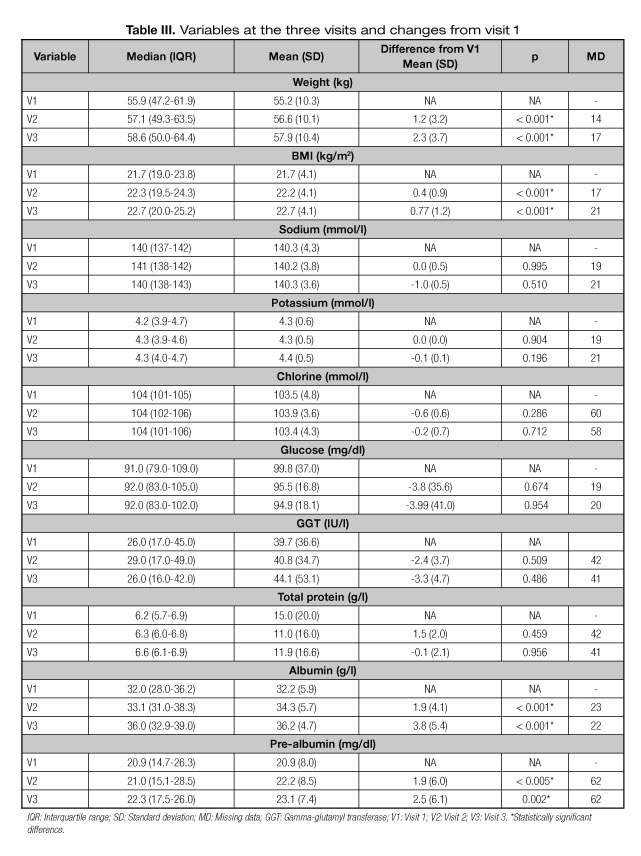
At the start of the study, 63.7% (n = 65) of patients had experienced unintentional weight loss. The proportion of patients who showed an increase in weight from baseline was 72.3% in V2, and 75.3% in V3. Median weight increased significantly by 1 kg (IQR 0-2; p < 0.001) between V1 and V2, while between V1 and V3, weight increased by 1.5 kg (IQR 0.2-4.0; p < 0.001). Differences in weight between V2 and V3 were also statistically significant (p < 0.001). Similarly, an increase in BMI values was recorded in 65.9% of patients in V2 and in 71.6% of patients in V3. Median increase was 0.4 kg/m2 (IQR 0.0-0.7; p < 0.001) in V2, and 0.6 kg/m2 (IQR 0.0-1.5; p < 0.001) in V3 (Table III). The differences between V2 and V3 were also statistically significant (p = 0.019). Mean caloric requirements increased significantly throughout the study, from 1,568 (SD, 298) kcal/day (n = 102) at the beginning of the study, 1,610 (SD, 321) kcal/day (n = 90) in V2 (p = 0.011) and 1,628 (SD, 328) kcal/day (n = 84) in V3 (p = 0.034). On average, mean caloric intake exceeded the caloric requirements in 99 kcal/day during the first four weeks (1,709 [SD, 331] kcal/day [n = 102]) and in 151 kcal/day during the last four weeks (1,779 [SD, 335] kcal/day [n = 89]).
In general, no significant changes were found in biochemical variables between the three study visits, with the exception of two parameters: albumin and pre-albumin. Albumin rose by 1.9 g/l (SD, 4.1; p < 0.001) between V1 and V2 and by 3.8 g/l (SD, 5.4; p < 0.001) between V1 and V3. Changes were also observed in pre-albumin: compared to values recorded in V1, levels rose in V2 and V3 by 1.9 mg/dl (SD 6.0; p < 0.001) and by 2.5 mg/dl (SD 6.1; p = 0.002), respectively (Table III). Mean albumin values were below normal limits at baseline and recovered in V2, while the other biochemical parameters analyzed, including glucose, remained within normal limits throughout the study.
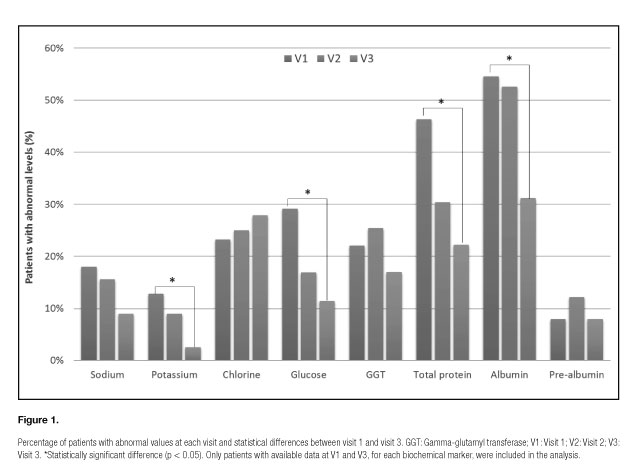
In general terms, the percentage of individuals with abnormal biochemical markers fell throughout the study (Fig. 1). These differences were significant between V1 and V3 in patients with altered glucose (V1: 29.1% - V3: 11.4% [n = 79]; p = 0.003), potassium (V1: 12.8% - V3: 2.6% [n = 78]; p = 0.020), total protein (V1: 46.3% - V3 22.2% [n = 54]; p = 0.009) and albumin (V1: 54.6% - V3: 31.2% [n = 77]; p < 0.001). Moreover, a fall in numbers of patients with abnormal sodium levels was observed, but this difference was not significant (V1: 17.9% - V2: 8.9% [n = 78]; p = 0.126).
Effect of nutritional formula on patients' bowel habits
The percentage of patients with diarrhea, according to clinical criteria, was 4.3% (n = 4, three of them receiving several drugs that may cause diarrhea) during the first four weeks (weeks 1-4) and 1.1% (n = 1, who received medications that may cause diarrhea) during the last four weeks (weeks 5-8) (torasemide, clorazepam, amoxicillin, tobramicina, bicalutamide, dexamethasone, granisetron, levodopa and carbidopa). This difference was not statistically significant. According to data recorded in the patient diary, during the first four weeks 13.1% (n = 13) of patients had diarrhea during a median of two days (IQR 1-2), whereas during the last four weeks, 11.6% (n = 10) of patients had diarrhea, with a median duration of one day (IQR, 0-2). In both cases, nine of those patients were receiving concomitant treatments that may cause diarrhea. None of these differences were statistically significant. Mean daily number of bowel movements was 1.1 (SD, 0.2) (n = 101) during the first four weeks and 1.1 (SD, 0.4) (n = 89) during the following four weeks. This difference was not significant (p = 0.548).
Product safety
In total, 11.8% (n = 12) of patients reported AEs (a total of 20 AEs were reported including fever [n = 3], infections [n = 6], respiratory failure [n = 3], emergency tracheotomy [n = 1], drug interaction [n = 1], acute diarrhea [n = 1], death [n = 1] and others [n = 4]). Only one (0.9%) of the cases was probably related to the EN (drug interaction in a patient with diabetes mellitus and chronic anemia). Another patient (0.9%) had acute diarrhea, possibly, but not probably, related to EN. One AE reported was a case of hyperglycemia, with no proven relationship with the enteral formula.
DISCUSSION
Malnutrition is associated with chronic diseases and other complications, including comorbidities and death (17-19). Enteral nutrition is a safe and cost-effective intervention to feed patients who cannot cover all requirements from food or oral nutritional supplements, or who cannot swallow safely (9).
The main aim of using high-calorie and high-protein enteral tube feeds containing fiber is to provide appropriate nutritional support, and to prevent weight loss, or even achieve weight gain. Jevity® Plus HP has been shown to be effective in this setting, as most of patients (75.3%) gained weight both in the first four weeks after starting the study, and at the end of the study.
Despite the benefits of enteral feeding, one of the reported problems is an increase in episodes of diarrhea and constipation (10). However, the diarrhea suffered by patients on EN is often due to medication use, infections, problems caused by their underlying disease, or the feeding method, rather than by the enteral formula as such (20,21). The use of fiber-enriched formulas helps to regulate bowel function, reducing the incidence of diarrhea (14,22) and constipation (increasing bowel movements, if baseline frequency is low, and reducing them, if baseline frequency is high) (22). The data from this study concur with these findings in that the percentage of patients with diarrhea, despite enteral feeding (and concomitant treatments which could cause diarrhea), was very low. According to clinical criteria, only four (4.3%) patients had diarrhea in the first four weeks, and in the last four weeks the incidence fell to 1.1% (n = 1). This incidence of diarrhea in patients on EN is lower than the rates of 15-20% reported in other studies conducted in Spain (23,24). These reported studies were focused on ICU and critical ill patients, in contrast to our study, which was targeted to general population receiving EN. This fact could explain the observed discrepancy. In addition, there are differences in diarrhea criteria between studies (e.g., three vs five liquid bowel movements per day). Other complications of enteral feeding include the risk of hyperglycemia and refeeding syndrome (25,26). Blood tests were performed at all visits to analyze the risk of complications. No significant differences were found for most biochemical variables between the three visits, with the exception of two parameters, albumin and pre-albumin, which increased. Mean albumin levels were below normal values at the beginning of the study, and reached normal levels at visit 2 (four weeks), while pre-albumin was within normal levels at the three visits. Other biochemical parameters, including blood glucose, remained stable and within normal ranges. With regard to patients whose biochemical parameters were outside normal ranges, a general improvement was found over the course of the three visits, being statistically significant for those with altered glucose, potassium, total protein and albumin levels in blood. Thus, a normalization of electrolyte balance and glucose levels was observed. It should be noted that biochemical basal values could be affected for all different factors related with the patient's clinical background.
Lastly, the enteral formula was well tolerated and highly accepted. Only one patient (0.9%) had a gastrointestinal complication (acute diarrhea), possibly related to the administration of the EN formula. Another patient (0.9%) had an adverse event (drug interaction with raised GGT), probably related to the administration of EN. Only one hyperglycemic event, not related to enteral feeding, was recorded, despite 20.6% of the patients being diabetics. No cases of refeeding syndrome were reported.
This study is limited by the fact that there was no control group in the study and the intervention group had a wide range of diseases. In addition, population was not uniform. Outpatients and hospitalized patients were included. Studies performed in the future in homogeneous patient groups with specific diseases may provide a more precise overview of the benefits and tolerability of the product. Moreover, the lack of available data on bowel movements previous to TFF administration limits the interpretation of TFF effects on bowel habits. Given that 20% of patients were diabetic, another limitation is the lack of exhaustive records about glycosylated hemoglobin A1c, type of diabetes and its treatment.
In conclusion, during the course of the study, most patients showed a significant increase in weight, BMI, pre-albumin and albumin levels, while blood glucose levels and other biochemical parameters remained stable. In addition, patients' stool patterns were kept stable within normal limits throughout the study. The high-calorie, high-protein enteral formula, enriched with fiber, FOS, and monounsaturated fatty acids (Jevity® Plus HP) was found to be well tolerated by patients and was beneficial in the management of patients who were malnourished or at risk of malnutrition.
ACKNOWLEDGMENTS
The SENS Working Group is integrated by Aguirre Palacios, Delgado Cárdenas, Megías Baeza, Da Silva Gonzalez, Ruiz Moreno, Rodríguez Náñez, Rodríguez Méndez, Rodríguez Aizcorbe, González Gil, Penacho Lázaro, Lample Lacasa, Hernández Barrera, Rius Payá, Avellana Zaragoza, Rodríguez Hernández, García Sánchez, García Moreno, de Castro Ojeda, Valverde Moyar, Aullo Chaves, Vitales Farrero, Ruiz Nava, Zumeta Fustero, Pereyra-García Castro, Palma Milla, Turro Ribalta, Galvis Vargas. In addition, the authors express thanks to the "Matia Foundation" for its contribution in the study.
REFERENCES
1. Stroud M, Duncan H, Nightingale J. Guidelines for enteral feeding in adult hospital patients. Gut 2003;52(Suppl 7):vii1-vii12.
2. Bermejo RV, Garcí IA, Galera DM, De las Heras Rodríguez M, Torramadé JP. Prevalencia de desnutrición en personas mayores institucionalizadas en España: un análisis multicéntrico nacional. Nutr Hosp 2015;31(3):1205-16.
3. Stratton RJ, Elia M. Who benefits from nutritional support: What is the evidence? Eur J Gastroenterol Hepatol 2007;19:353-8.
4. Álvarez J, Monereo S, Ortiz P, Salido C. Gestión en nutrición clínica. Nutr Hosp 2004;19(3):125-34.
5. Isabel TD, Correia M. The impact of malnutrition on morbidity, mortality, length of hospital stay and costs evaluated through a multivariate model analysis. Clin Nutr 2003;22(3):235-9.
6. Amparo N, Giraldo G, Velásquez JV, Andrea P, Cano R, Astudillo CO, et al. Cost-effectiveness of early nutritional therapy in malnourished adult patients in a high complexity hospital. Nutr Hosp 2015;32(65):2938-47.
7. Woestenenk JW, Castelijns SJAM, Van der Ent CK, Houwen RHJ. Nutritional intervention in patients with cystic fibrosis: A systematic review. J Cyst Fibros 2013;12(2):102-15.
8. Mueller C. Disease-related malnutrition: An evidence-based approach to treatment. Nutr Clin Pract 2003;18(6):527-8.
9. Majka AJ, Wang Z, Schmitz KR, Niesen CR, Larsen RA, Kinsey GC, et al. Care coordination to enhance management of long-term enteral tube feeding: A systematic review and meta-analysis. J Parenter Enter Nutr 2014;38(1): 40-52.
10. Blumenstein I, Shastri YM, Stein J. Gastroenteric tube feeding: Techniques, problems and solutions. World J Gastroenterol 2014;20(26):8505-24.
11. Scott R, Bowling T. Enteral tube feeding in adults. J R Coll Physicians Edinb 2015;45(1):49-54.
12. Orejana Martín M, Torrente Vela S, Murillo Pérez MA, García Iglesias M, Cornejo Bauer C, Morales Sánchez C, et al. Análisis del estreñimiento en pacientes con traumatismo grave. Enferm Intensiva 2014;25(2):46-51.
13. Bittencourt AF, Martins JR, Logullo L, Shiroma G, Horie L, Ortolani MC, et al. Constipation is more frequent than diarrhea in patients fed exclusively by enteral nutrition: Results of an observational study. Nutr Clin Pr 2012;27(4):533-9.
14. Del Olmo D, López Del Val T, Martínez De Icaya P, De Juana P, Alcázar V, Koning A, et al. La fibra en nutrición enteral: revisión sistemática de la literatura. Nutr Hosp 2004;19:167-74.
15. Whelan K, Efthymiou L, Judd PA, Preedy VR, Taylor MA. Appetite during consumption of enteral formula as a sole source of nutrition: The effect of supplementing pea-fibre and fructo-oligosaccharides. Br J Nutr 2007; 96(2):350.
16. Wierdsma NJ, Van Bodegraven AA, Uitdehaag BMJ, Arjaans W, Savelkoul PHM, Kruizenga HM, et al. Fructo-oligosaccharides and fibre in enteral nutrition has a beneficial influence on microbiota and gastrointestinal quality of life. Scand J Gastroenterol 2009;44:804-12.
17. Saka B, Kaya O, Ozturk GB, Erten N, Karan MA. Malnutrition in the elderly and its relationship with other geriatric syndromes. Clin Nutr 2010;29(6):745-8.
18. Freijer K, Lenoir-Wijnkoop I, Russell C, Koopmanschap M, Kruizenga H, Lhachimi S, et al. The view of European experts regarding health economics for medical nutrition in disease-related malnutrition. Eur J Clin Nutr 2015;69280:539-45.
19. Barker L, Gout B, Crowe T. Hospital malnutrition: Prevalence, identification and impact on patients and the healthcare system. Int J Environ Res Public Health 2011;8(12):514-27.
20. Eisenberg PG. Causes of diarrhea in tube-fed patients: A comprehensive approach to diagnosis and management. Nutr Clin Pract 1993;8(3): 119-23.
21. Chang S-J, Huang H-H. Diarrhea in enterally fed patients: Blame the diet? Curr Opin Clin Nutr Metab Care 2013;16(5):588-94.
22. Elia M, Engfer MB, Green CJ, Silk DBA. Systematic review and meta-analysis: The clinical and physiological effects of fibre-containing enteral formulae. Aliment Pharmacol Ther 2008;27(2):120-45.
23. Velázquez Núñez JM, Mayoll Carbonell MD. Incidencia de las complicaciones gastrointestinales en la nutrición enteral. Resultados de un protocolo. Enferm Intensiva 1998;9(3):109-14.
24. Montejo González JC, Estébanez Montiel B. Gastrointestinal complications in critically ill patients. Nutr Hosp 2007;22(Suppl 2):56-62.
25. Mehanna H, Moledina J, Travis J. Refeeding syndrome: What it is, and how to prevent and treat it. BMJ 2008;336(7659):1495-8.
26. Kosiborod M, Inzucchi SE, Spertus JA, Wang Y, Masoudi FA, Havranek EP, et al. Elevated admission glucose and mortality in elderly patients hospitalized with heart failure. Circulation 2009;119(14):1899-907.
 Correspondence:
Correspondence:
Federico Miguel Cuesta-Triana.
Geriatric Medicine Service.
Hospital Clínico San Carlos.
C/ del Profesor Martín Lagos, s/n.
28040 Madrid, Spain
e-mail: federicomiguel.cuesta@salud.madrid.org
Received: 19/02/2017
Accepted: 28/06/2017